Abstract
Purpose
The anatomical position of the lingula is clinically very important to prevent injuries during sagittal split ramus osteotomy. Our study aims to evaluate the localisation of the lingula by cone beam computed tomography (CBCT) and to compare the localisation of the lingula between malocclusion, gender, and lingula types.
Methods
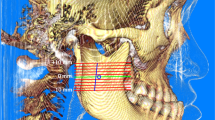
A retrospective study was conducted to evaluate the shape and location of the lingula using CBCT. A total of 250 CBCT images were included in this study. The lingula was classified as nodular, assimilated, truncated, or triangular type. Six defined distances from the top of the lingula were measured: anterior border of the ramus (L-A), posterior border of the ramus (L-P), internal oblique ridge (L-IOR), mandibular notch (L-N), and distal surface of the mandibular second molar (L-M2) and occlusal plane (L-OP). The measured distances were compared between gender, malocclusion, and lingula types.
Results
The most common type of lingula was nodular (32.4%). The L-N, L-P, L-M2, and L-OP distances between genders were statistically higher in male patients than in female patients. The L-IOR, L-M2, and L-OP distances exhibited statistically significant differences found between malocclusions. No statistically significant difference was found when the distances of the lingula to the anatomical points were compared between the lingula types.
Conclusion
These variations in positioning of the lingula depending on the dysmorphoses are developing towards a systematic 3D examination before any mandibular osteotomy to precisely visualize the position and shape of the lingula.



Similar content being viewed by others
Data availability
Data available upon request.
References
Acebal-Bianco F, Vuylsteke PL, Mommaerts MY, De Clercq CA (2007) Perioperative complications in corrective facial orthopedic surgery: a 5-year retrospective study. J Oral Maxillofac Surg 58:754–760. https://doi.org/10.1053/joms.2000.7874
Akcay H, Kalabalık F, Tatar B, Ulu M (2019) Location of the mandibular lingula: comparison of skeletal Class I and Class III patients in relation to ramus osteotomy using cone-beam computed tomography. J Stomatol Oral Maxillofac Surg 120:504–508. https://doi.org/10.1016/j.jormas.2019.07.013
Angelopoulos C, Thomas SL, Hechler S, Parissis N, Hlavacek M (2008) Comparison between digital panoramic radiography and cone-beam computed tomography for the identification of the mandibular canal as part of presurgical dental implant assessment. J Oral Maxillofac Surg 66:2130–2135. https://doi.org/10.1016/j.joms.2008.06.021
De Vos W, Casselman J, Swennen GR (2009) Cone-beam computerized tomography (CBCT) imaging of the oral and maxillofacial region: a systematic review of the literature. Int J Oral Maxillofac Surg 38:609–625. https://doi.org/10.1016/j.ijom.2009.02.028
Falter B, Schepers S, Vrielinck L, Lambrichts I, Thijs H, Politis C (2010) Occurrence of bad splits during sagittal split osteotomy. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 110:430–435. https://doi.org/10.1016/j.tripleo.2010.02.003
Fernandes AC, Cardoso PM, Fernandes IS, Moraes M (2013) Anatomic study for the horizontal cut of the sagittal split ramus osteotomy. J Oral Maxillofac Surg 71:1239–1244. https://doi.org/10.1016/j.joms.2013.01.013
Freire-Maia B, Machado VD, Valerio CS, Custódio AL, Manzi FR, Junqueira JL (2017) Evaluation of the accuracy of linear measurements on multi-slice and cone beam computed tomography scans to detect the mandibular canal during bilateral sagittal split osteotomy of the mandible. Int J Oral Maxillofac Surg 46:296–302. https://doi.org/10.1016/j.ijom.2016.11.007
Hsu KJ, Tseng YC, Liang SW, Hsiao SY, Chen CM (2020) Dimension and location of the mandibular lingula: comparisons of gender and skeletal patterns using cone-beam computed tomography. Biomed Res Int 2020:2571534. https://doi.org/10.1155/2020/2571534
Jang HY, Han SJ (2019) Measurement of mandibular lingula location using cone-beam computed tomography and internal oblique ridge-guided inferior alveolar nerve block. J Korean Assoc Oral Maxillofac Surg 45:158–166. https://doi.org/10.5125/jkaoms.2019.45.3.158
Jansisyanont P, Apinhasmit W, Chompoopong S (2009) Shape, height, and location of the lingula for sagittal ramus osteotomy in Thais. Clin Anat 22:787–793. https://doi.org/10.1002/ca.20849
Kositbowornchai S, Siritapetawee M, Damrongrungruang T, Khongkankong W, Chatrchaiwiwatana S, Khamanarong K, Chanthaooplee T (2007) Shape of the lingula and its localization by panoramic radiograph versus dry mandibular measurement. Surg Radiol Anat 29:689–694. https://doi.org/10.1007/s00276-007-0270-9
Lima FJ, Oliveira Neto OB, Barbosa FT, Sousa-Rodrigues CF (2016) Location, shape and anatomic relations of the mandibular foramen and the mandibular lingula: a contribution to surgical procedures in the ramus of the mandible. Oral Maxillofac Surg 20:177–182. https://doi.org/10.1007/s10006-016-0547-4
Mommaerts MY (1992) Two similar “bad splits” and how they were treated. Report of two cases. Int J Oral Maxillofac Surg 21:331–332. https://doi.org/10.1016/s0901-5027(05)80754-4
Muto T, Takahashi M, Akizuki K (2012) Evaluation of the mandibular ramus fracture line after sagittal split ramus osteotomy using 3-dimensional computed tomography. J Oral Maxillofac Surg 70:648–652. https://doi.org/10.1016/j.joms.2012.07.048
Park JH, Jung HD, Kim HJ, Jung YS (2018) Anatomical study of the location of the antilingula, lingula, and mandibular foramen for vertical ramus osteotomy. Maxillofac Plast Reconstr Surg 40:15. https://doi.org/10.1186/s40902-018-0155-3
Park KR, Kim SY, Kim GJ, Park HS, Jung YS (2014) Anatomic study to determine a safe surgical reference point for mandibular ramus osteotomy. J Craniomaxillofac Surg 42:22–27. https://doi.org/10.1016/j.jcms.2013.01.041
Plooij JM, Naphausen MT, Maal TJ, Xi T, Rangel FA, Swennnen G, Koning M, Borstlap WA, Bergé SJ (2009) 3D evaluation of the lingual fracture line after a bilateral sagittal split osteotomy of the mandible. Int J Oral Maxillofac Surg 38:1244–1249. https://doi.org/10.1016/j.ijom.2009.07.013
Pogrel MA, Schmidt BL, Ammar A (1995) The presence of the antilingula and its relationship to the true lingula. Br J Oral Maxillofac Surg 33:235–238. https://doi.org/10.1016/0266-4356(95)90007-1
Reyneke JP, Ferretti C (2016) The bilateral sagittal split mandibular ramus osteotomy. Atlas Oral Maxillofac Surg Clin North Am 24:27–36. https://doi.org/10.1016/j.cxom.2015.10.005
Sekerci AE, Cantekin K, Aydinbelge M (2013) Cone beam computed tomographic analysis of the shape, height, and location of the mandibular lingula in a population of children. Biomed Res Int 2013:825453. https://doi.org/10.1155/2013/825453
Sekerci AE, Sisman Y (2014) Cone-beam computed tomography analysis of the shape, height, and location of the mandibular lingula. Surg Radiol Anat 36:155–162. https://doi.org/10.1007/s00276-013-1150-0
Sinanoglu A, Seki U, Tokuc B (2022) A detailed radiomorphometric analysis of the mandibular foramen, lingula and anti-lingula with a special emphasis on mandibular prognathism. J Stomatol Oral Maxillofac Surg 124:101260. https://doi.org/10.1016/j.jormas.2022.08.003
Sindel M, Salim H, Sarıkaya DM, Ozturk S, Goztepe MB, Bilgin B, Calguner E, Sindel A (2019) Surgical morphological evaluation of the anatomical position of lingula mandibulae. Anatomy 13:105–106
Smith BR, Rajchel JL, Waite DE, Read L (1991) Mandibular ramus anatomy as it relates to the medial osteotomy of the sagittal split ramus osteotomy. J Oral Maxillofac Surg 49:112–116. https://doi.org/10.1016/0278-2391(91)90095-4
Steenen SA, Becking AG (2016) Bad splits in bilateral sagittal split osteotomy: systematic review of fracture patterns. Int J Oral Maxillofac Surg 45:887–897. https://doi.org/10.1016/j.ijom.2016.02.001
Tengku Shaeran TA, Shaari R, Abdul Rahman S, Alam MK, Muhamad Husin A (2017) Morphometric analysis of prognathic and non-prognathic mandibles in relation to BSSO sites using CBCT. J Oral Biol Craniofac Res 7:7–12. https://doi.org/10.1016/j.jobcr.2016.10.007
Trost O, Salignon V, Cheynel N, Malka G, Trouilloud P (2010) A simple method to locate mandibular foramen: preliminary radiological study. Surg Radiol Anat 32:927–931. https://doi.org/10.1007/s00276-010-0645-1
Tuli A, Choudhry R, Choudhry S, Raheja S, Agarwal S (2000) Variation in shape of the lingula in the adult human mandible. J Anat 197:313–317. https://doi.org/10.1046/j.1469-7580.2000.19720313.x
Werther J, Hall H (2000) Vertical ramus osteotomy and the inverted-L osteotomy. Oral and Maxillofac Surg 2:311–323
Funding
None.
Author information
Authors and Affiliations
Contributions
All the authors have made substantial contributions to the study. GT and NSK: research development and data analysis. MU: tomographic analysis. GT, YCK, GG, GC, NSK, and OD: manuscript writing and editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. The study procedure was approved by the Osmangazi University Ethics Committee, Eskişehir, Turkey (Approval No. 2020/18).
Informed consent
Informed consent was obtained from the patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tekin, G., Kose, N.S., Ugurlu, M. et al. Determining the safety margin of mandibular lingula in sagittal split ramus osteotomy. Surg Radiol Anat 46, 159–166 (2024). https://doi.org/10.1007/s00276-023-03291-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-023-03291-9