Abstract
Purpose
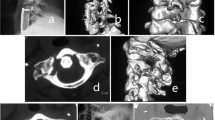
To investigate the prevalence and morphological characteristics of ponticulus posticus (PP) and ponticulus lateralis (PL) using computed tomography (CT) images on a large study sample of the Anatolian population. The presence of the PP and PL bridges can limit gap available for placement procedure through the bony elements of C1. Routine screw techniques are contraindicated because of high risk of fatal bleeding of vertebral artery (VA).
Methods
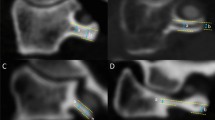
The CT images of 1000 subjects (500 males, 500 females) were examined for the morphological characteristics and presence of PP and PL. The anteroposterior diameter, superoposterior (transverse) diameter, surface area, and central thickness of the bony bridge of the PP, PL, and transverse foramina (TF).
Results
The prevalence of PP was 14.8%, and bilateral complete PP was the most common PP type at 6.8%. The prevalence of PL was 4.1% and left-side complete PL was the most common PL type at 1.2%. The prevalence of both PP and PL was more common in males and bilateral complete PP were more predominant in males (p = 0.004, p = 0.038, and p = 0.010, respectively). The surface area of PP and PL were determined to be smaller than the surface area of the ipsilateral TF (p < 0.001 and p = 0.042, respectively).
Conclusion
PP is not an uncommon anatomic anomaly and PL is even less frequently encountered. The prevalence of PP and PL was more common in males and bilateral complete PP was more predominant in males. Detailed information about the prevalence and morphometry of the PP and PL obtained in the present study could guide the clinicians dealing with neurosurgery, physical medicine and rehabilitation, and radiology in their practice.




Similar content being viewed by others
References
Ahn J, Duran M, Syldort S, Rizvi A, D’Antoni AV, Johal J, Iwanaga J, Oskouian RJ, Tubbs RS (2018) Arcuate foramen: anatomy, embryology, nomenclature, pathology, and surgical considerations. World Neurosurg 118:197–202. https://doi.org/10.1016/j.wneu.2018.07.038
Arslan D, Ozer MA, Govsa F, Kıtıs O (2018) The ponticulus posticus as risk factor for screw insertion into the first cervical lateral mass. World Neurosurg 113:e579–e585. https://doi.org/10.1016/j.wneu.2018.02.100
Bodon G, Grimm A, Hirt B, Seifarth H, Barsa P (2016) Applied anatomy of screw placement via the posterior arch of the atlas and anatomy-based refinements of the technique. Eur J Orthop Surg Traumatol 26:793–803. https://doi.org/10.1007/s00590-016-1771-1
Cirpan S, Yonguc GN, Edizer M, Mas NG, Magden AO (2017) Foramen arcuale: a rare morphological variation located in atlas vertebrae. Surg Radiol Anat 39:877–884. https://doi.org/10.1007/s00276-016-1808-5
Elgafy H, Pompo F, Vela R, Elsamaloty HM (2014) Ipsilateral arcuate foramen and high-riding vertebral artery: implication on C1–C2 instrumentation. Spine J 14:1351–1355. https://doi.org/10.1016/j.spinee.2014.01.054
Elliott RE, Tanweer O (2014) The prevalence of the ponticulus posticus (arcuate foramen) and its importance in the Goel-Harms procedure: meta-analysis and review of the literature. World Neurosurg 82:e335-343. https://doi.org/10.1016/j.wneu.2013.09.014
Geist JR, Geist SM, Lin LM (2014) A cone beam CT investigation of ponticulus posticus and lateralis in children and adolescents. Dentomaxillofac Radiol 43:20130451. https://doi.org/10.1259/dmfr.20130451
Karau PB, Ogengo JA, Hassanali J, Odula P (2010) Anatomy and prevalence of atlas vertebrae bridges in a Kenyan population: an osteological study. Clin Anat 23:649–653. https://doi.org/10.1002/ca.21010
Kim C, Lee SH, Park SS, Kim BJ, Ryu WS, Kim CK, Oh MY, Chung JW, Yoon BW (2012) A quantitative comparison of the vertebral artery and transverse foramen using CT angiography. J Clin Neurol 8:259–264. https://doi.org/10.3988/jcn.2012.8.4.259
Kim KH, Park KW, Manh TH, Yeom JS, Chang BS, Lee CK (2007) Prevalence and morphologic features of ponticulus posticus in Koreans: analysis of 312 radiographs and 225 three-dimensional CT scans. Asian Spine J 1:27–31. https://doi.org/10.4184/asj.2007.1.1.27
Kotil K, Kilincer C (2014) Sizes of the transverse foramina correlate with blood flow and dominance of vertebral arteries. Spine J 14:933–937. https://doi.org/10.1016/j.spinee.2013.07.447
Paraskevas G, Papaziogas B, Tsonidis C, Kapetanos G (2005) Gross morphology of the bridges over the vertebral artery groove on the atlas. Surg Radiol Anat 27:129–136. https://doi.org/10.1007/s00276-004-0300-9
Pękala PA, Henry BM, Pękala JR, Hsieh WC, Vikse J, Sanna B, Walocha JA, Tubbs RS, Tomaszewski KA (2017) Prevalence of foramen arcuale and its clinical significance: a meta-analysis of 55,985 subjects. J Neurosurg Spine 27:276–290. https://doi.org/10.3171/2017.1.Spine161092
Pękala PA, Henry BM, Phan K, Pękala JR, Taterra D, Walocha JA, Tubbs RS, Tomaszewski KA (2018) Presence of a foramen arcuale as a possible cause for headaches and migraine: systematic review and meta-analysis. J Clin Neurosci 54:113–118. https://doi.org/10.1016/j.jocn.2018.05.008
Saleh A, Gruber J, Bakhsh W, Rubery PT, Mesfin A (2018) How common is the ponticulus posticus?: a computed tomography based analysis of 2917 patients. Spine Phila Pa 1976 43:E436–e441. https://doi.org/10.1097/brs.0000000000002400
Sanchis-Gimeno JA, Llido S, Perez-Bermejo M, Nalla S (2018) Prevalence of anatomic variations of the atlas vertebra. Spine J 18:2102–2111. https://doi.org/10.1016/j.spinee.2018.06.352
Tambawala SS, Karjodkar FR, Sansare K, Motghare D, Mishra I, Gaikwad S, Dora AC (2017) Prevalence of ponticulus posticus on lateral cephalometric radiographs, its association with cervicogenic headache and a review of literature. World Neurosurg 103:566–575. https://doi.org/10.1016/j.wneu.2017.04.030
Travan L, Saccheri P, Gregoraci G, Mardegan C, Crivellato E (2015) Normal anatomy and anatomic variants of vascular foramens in the cervical vertebrae: a paleo-osteological study and review of the literature. Anat Sci Int 90:308–323. https://doi.org/10.1007/s12565-014-0270-x
Tubbs RS, Johnson PC, Shoja MM, Loukas M, Oakes WJ (2007) Foramen arcuale: anatomical study and review of the literature. J Neurosurg Spine 6:31–34. https://doi.org/10.3171/spi.2007.6.1.6
Tubbs RS, Shoja MM, Shokouhi G, Farahani RM, Loukas M, Oakes WJ (2007) Simultaneous lateral and posterior ponticles resulting in the formation of a vertebral artery tunnel of the atlas: case report and review of the literature. Folia Neuropathol 45:43–46
Vaněk P, Bradáč O, de Lacy P, Konopková R, Lacman J, Beneš V (2017) Vertebral artery and osseous anomalies characteristic at the craniocervical junction diagnosed by CT and 3D CT angiography in normal Czech population: analysis of 511 consecutive patients. Neurosurg Rev 40:369–376. https://doi.org/10.1007/s10143-016-0784-x
Wakao N, Takeuchi M, Nishimura M, Riew KD, Kamiya M, Hirasawa A, Kawanami K, Imagama S, Sato K, Takayasu M (2014) Vertebral artery variations and osseous anomaly at the C1–2 level diagnosed by 3D CT angiography in normal subjects. Neuroradiology 56:843–849. https://doi.org/10.1007/s00234-014-1399-y
Yamazaki M, Okawa A, Furuya T, Sakuma T, Takahashi H, Kato K, Fujiyoshi T, Mannoji C, Takahashi K, Koda M (2012) Anomalous vertebral arteries in the extra- and intraosseous regions of the craniovertebral junction visualized by 3-dimensional computed tomographic angiography: analysis of 100 consecutive surgical cases and review of the literature. Spine Phila Pa 1976 37:E1389–1397. https://doi.org/10.1097/BRS.0b013e31826a0c9f
Yeom JS, Buchowski JM, Kim HJ, Chang BS, Lee CK, Riew KD (2013) Risk of vertebral artery injury: comparison between C1–C2 transarticular and C2 pedicle screws. Spine J 13:775–785. https://doi.org/10.1016/j.spinee.2013.04.005
Yeom JS, Kafle D, Nguyen NQ, Noh W, Park KW, Chang BS, Lee CK, Riew KD (2012) Routine insertion of the lateral mass screw via the posterior arch for C1 fixation: feasibility and related complications. Spine J 12:476–483. https://doi.org/10.1016/j.spinee.2012.06.010
Funding
None.
Author information
Authors and Affiliations
Contributions
MG: Project administration, Conceptualization, Visualization, Writing Original Draft. EK: Project development, Data collection. HS: Data analysis, Visualization. FG: Supervision, Writing Review and Editing. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
No financial conflict of interest exists with any commercial entity whose products are described, reviewed, evaluated or compared in the manuscript. None of the authors has a financial interest in any of the product, devices or drugs mentioned in this article. This article has not been submitted or published elsewhere in part or in whole and that it is original work.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study was approved by the suitably constituted Ethical Committee at the Researches Department of University, within which the work was undertaken, and the study conforms to the Declaration of Helsinki.
Consent for publication
Informed consent Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Golpinar, M., Komut, E., Salim, H. et al. The computed tomographic evaluation of bony bridge of C1 as bleeding risk factor at the screw placement. Surg Radiol Anat 44, 585–593 (2022). https://doi.org/10.1007/s00276-022-02919-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-022-02919-6