Abstract
Purpose
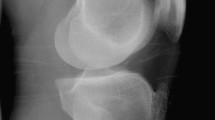
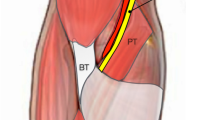
The cubital tunnel is limited anteriorly by the medial epicondyle (ME), laterally by the medial collateral ligament, and superiorly by Osborne’s fascia and the cubital tunnel retinaculum. Previous studies were mostly dedicated to the roof of the cubital tunnel, in the way that the study of the groove for ulnar nerve and ME anatomy is relatively scarce in the literature. We sought to describe the radiological anatomy of the groove for ulnar nerve and ME in healthy volunteers with multiplanar computed tomography (CT).
Methods
We analyzed 3D CT images of 30 healthy volunteers (mean age 39 years, range 18–66 years). Nine variables were measured from the right elbow, including sizes, areas and angles in two different planes (coronal and axial).
Results
Mean ME width and length were 17.3 ± 3.5 mm and 31.7 ± 4.5 mm, respectively. According to categorical correlation studies, ME width (X) was deemed the most representative morphological characteristic because of the positive correlation to five other different anatomical measurements. A three-tiered anatomical classification was proposed based on data distribution.
Conclusion
Large individual variation is found in the shape of ME, both in coronal and axial planes. The knowledge of individual osseous morphology is of great value potentially contributing to the surgical decision-making in patients affected by cubital tunnel syndrome.



Similar content being viewed by others
References
Amadio PC, Beckenbaugh RD (1986) Entrapment of the ulnar nerve by the deep flexor–pronator aponeurosis. J Hand Surg Am 11:83–87. https://doi.org/10.1016/s0363-5023(86)80110-1
Apfelberg DB, Larson SJ (1973) Dynamic anatomy of the ulnar nerve at the elbow. Plast Reconstr Surg 51:76–81
Bartels RH (2001) History of the surgical treatment of ulnar nerve compression at the elbow. Neurosurgery 49:391–400. https://doi.org/10.1097/00006123-200108000-00023
Caliandro P, La Torre G, Padua R, Giannini F, Padua L (2016) Treatment for ulnar neuropathy at the elbow. Cochrane Database Syst Rev 11:CD006839. https://doi.org/10.1002/14651858.CD006839.pub4
Feindel W, Stratford J (1958) Cubital tunnel compression in tardy ulnar palsy. Can Med Assoc J 78:351–353
Feindel W, Stratford J (1958) The role of the cubital tunnel in tardy ulnar palsy. Can J Surg 1:287–300
Gonzalez MH, Lotfi P, Bendre A, Mandelbroyt Y, Lieska N (2001) The ulnar nerve at the elbow and its local branching: an anatomic study. J Hand Surg Br 26:142–144. https://doi.org/10.1054/jhsb.2000.0532
Granger A, Sardi JP, Iwanaga J et al (2017) Osborne’s ligament: a review of its history, anatomy, and surgical importance. Cureus 9:e1080. https://doi.org/10.7759/cureus.1080
Huang JH, Samadani U, Zager EL (2004) Ulnar nerve entrapment neuropathy at the elbow: simple decompression. Neurosurgery 55:1150–1153. https://doi.org/10.1227/01.neu.0000140841.28007.f2
Imamura K, Beppu M, Shimizu H, Aoki H (1996) An anatomical study of the medial epicondyle of the humerus. J Jpn Soc Hand Surg 12:977–981 (Japanese)
Imamura K, Shimizu H, Beppu M, Aoki H (2000) Anatomical study of ulnar nerve groove of the medial humeral epicondyle. J Jpn Soc Hand Surg 17:264–268
Inserra S, Spinner M (1986) An anatomic factor significant in transposition of the ulnar nerve. J Hand Surg Am 11:80–82. https://doi.org/10.1016/s0363-5023(86)80109-5
James J, Sutton LG, Werner FW, Basu N, Allison MA, Palmer AK (2011) Morphology of the cubital tunnel: an anatomical and biomechanical study with implications for treatment of ulnar nerve compression. J Hand Surg Am 36:1988–1995. https://doi.org/10.1016/j.jhsa.2011.09.014
Karatas A, Apaydin N, Uz A, Tubbs R, Loukas M, Gezen F (2009) Regional anatomic structures of the elbow that may potentially compress the ulnar nerve. J Shoulder Elbow Surg 18:627–631. https://doi.org/10.1016/j.jse.2009.03.004
Khoo D, Carmichael SW, Spinner RJ (1996) Ulnar nerve anatomy and compression. Orthop Clin N Am 27:317–338
Kim DH, Han K, Tiel RL, Murovic JA, Kline DG (2003) Surgical outcomes of 654 ulnar nerve lesions. J Neurosurg 98:993–1004. https://doi.org/10.3171/jns.2003.98.5.0993
Kleinman WB (1999) Cubital tunnel syndrome: anterior transposition as a logical approach to complete nerve decompression. J Hand Surg Am 24:886–997. https://doi.org/10.1053/jhsu.1999.0886
Macchi V, Tiengo C, Porzionato A et al (2014) The cubital tunnel: a radiologic and histotopographic study. J Anat 225:262–269. https://doi.org/10.1111/joa.12206
Mahan MA, Gasco J, Mokhtee DB, Brown JM (2015) Anatomical considerations of fascial release in ulnar nerve transposition: a concept revisited. J Neurosurg 123:1216–1222. https://doi.org/10.3171/2014.10.JNS141379
Makhni EC, Khanna K, Simpson MT et al (2014) Medial epicondyle morphology in elite overhead athletes: a closer look using 3-dimensional computer simulation. Orthop J Sports Med 2:2325967113517211. https://doi.org/10.1177/2325967113517211
O’Driscoll SW, Horii E, Carmichael SW, Morrey BF (1991) The cubital tunnel and ulnar neuropathy. J Bone Jt Surg Br 73:613–617
Osborne G (1959) Ulnar neuritis. Postgrad Med J 35:392–396
Acknowledgements
We are grateful to Prof. Gabriel de Araújo Serrão, MD, MSc for the thoughtful comments.
Funding
The authors have no funding to declare.
Author information
Authors and Affiliations
Contributions
LQC: protocol development, data collection, data analysis and manuscript writing/editing. GVSF: protocol development, data analysis. FHPS: protocol development, data analysis. MAA: protocol development, data collection, data analysis and manuscript writing/editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
Marcílio Dias Naval Hospital Ethical Committee—study number 58174616.5.0000.5256/2016.
Data availability and material
Material available.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chaves, L.d., Fonseca, G.V.d., da Silva, F.H.P. et al. Osseous morphology of the medial epicondyle: an anatomoradiological study with potential clinical implications. Surg Radiol Anat 43, 713–720 (2021). https://doi.org/10.1007/s00276-020-02669-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-020-02669-3