Abstract
Purpose
The gluteal region is a key element of beauty balance and sexual appearance. However, there is no clear anatomical description of the infragluteal fold, nor any classification exists allowing standardizing treatment of this area in case of jeopardisation. The purpose of this study was to perform an anatomical description of the infragluteal fold (IGF) matching radiological and anatomical findings in describing specifically raise of the fibrous component at the bone level.
Methods
Six volunteers (three males and three females) underwent an MRI scan (Siemens Aera® 1.5 T) of the pelvic region. T1 Vibe Morpho T2, Sag Space 3D, and Millimetric slices were performed in order to obtain a more detailed selection of the gluteal landmark. Trabecular connective tissue of the region was analyzed using Horos® ROI (region of interest) segmentation function. Four fresh cadavers (two males, two females, accounting for 8 hemipelvis) were dissected in order to compare the radiological findings.
Results
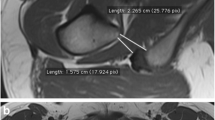
The infragluteal fold is a connectival fibrous band extending from the ramus of the ischium (but not involving the ischial tuberosity, for a length of 21 mm ± 2 and 21 mm ± 3), the apex of the sacrum (for a length of 13 ± 2 and 11 mm ± 2), and the coccyx (for a length of 19 mm ± 2 and 20 mm ± 2, all measures referring to volunteers and cadavers, respectively) reaching superficially the dermis of the medial one-third of the cutaneous fold. No significant difference was found between volunteer and cadaver group in MRI measurement of bony origins, or between MRI and cadaveric dissection measurements.
Conclusion
Knowledge of this structure will define novel surgical techniques in infragluteal fold restoration.







Similar content being viewed by others
References
Babuccu O, Barut C, Zeyrek T et al (2008) Infragluteal sulcus: a combined histologic and anatomic reappraisal. Aesthet Plast Surg 32(3):496–502. https://doi.org/10.1007/s00266-008-9127-9
Babuccu O, Kargı E, Hosnuter M et al (2004) Morphology of the gluteal region in the female population 5 to 83 years of age. Aesthet Plast Surg 28(6):405–411. https://doi.org/10.1007/s00266-004-4010-9
Cartmill M, Hylander WL, Shafland J (1988) Human structure. Harvard University Press, Cambridge, Mass
Centeno RF, Young VL (2006) Clinical anatomy in aesthetic gluteal body contouring surgery. Clin Plast Surg 33(3):347–358. https://doi.org/10.1016/j.cps.2006.05.005
Coban YK, Uzel M, Celik M (2004) Correction of buttock ptosis with anchoring deepithelialized skin flaps. Aesthet Plast Surg 28(2):116–119. https://doi.org/10.1007/s00266-004-3109-3
Cuenca-Guerra R, Lugo-Beltran I (2006) Beautiful buttocks: characteristics and surgical techniques. Clin Plast Surg 33(3):321–332. https://doi.org/10.1016/j.cps.2006.04.002
Da Rocha RP (2001) Surgical anatomy of the gluteal region’s subcutaneous screen and its use in plastic surgery. Aesthetic Plast Surg 25(2):140–144. https://doi.org/10.1007/s002660010111
Gonzalez R (2005) Treating the banana fold with the dermotuberal anchorage technique: case report. Aesthet Plast Surg 29(4):300–303. https://doi.org/10.1007/s00266-004-0133-2
Gonzalez R (2006) Etiology, definition, and classification of gluteal ptosis. Aesthet Plast Surg 30(3):320–326. https://doi.org/10.1007/s00266-005-0051-y
Hoenig JF, Swetje K (2013) Age-related ptosis of the buttock: an anthropometric gender-specific analysis. Aesthet Plast Surg 37(6):1090–1099. https://doi.org/10.1007/s00266-013-0205-2
Huemer GM, Dunst KM, Schoeller T (2005) Restoration of the gluteal fold by a deepithelialized skin flap: preliminary observations. Aesthet Plast Surg 29(1):13–17. https://doi.org/10.1007/s00266-004-0006-8
Illouz Y-G (1989) Surgical implications of “fixed points”: a new concept in plastic surgery. Aesthet Plast Surg 13(3):137–144. https://doi.org/10.1007/BF01570210
Kirwan L (2004) Anchor thighplasty Aesthet Surg J 24(1):61–64. https://doi.org/10.1016/j.asj.2003.10.003
Lockwood TE (1991) Superficial fascial system (SFS) of the trunk and extremities: a new concept. Plast Reconstr Surg 87(6):1009–1018. https://doi.org/10.1097/00006534-199106000-00001
Moore KL, Daley AF (2006). Clinically Oriented Anatomy. 5th ed. Lippincott Williams and Wilkins, Philadelphia, p. 589. https://doi.org/https://doi.org/10.1111/j.1469-7580.2006.00537.x
Nteli Chatzioglou G, Bagheri H et al (2018) Anatomical topography of the inferior lumbar triangle for transversus abdominis block. Surg Radiol Anat 40(1):99–107. https://doi.org/10.1007/s00276-017-1912-1
Schlesinger SL (1991) Two arcane areas in liposuction: the banana and the sensuous triangle. Aesthet Plast Surg 15(2):175–180. https://doi.org/10.1007/BF02273852
Sönmez Ergün S, Gayretli Ö, Kılıçarslan R, Bilgiç B (2013) The infragluteal sulcus: a histologic and ultrasonographic study. Aesthet Plast Surg 37(6):1209–1213. https://doi.org/10.1007/s00266-013-0228-8
Wong WW, Motakef S, Lin Y, Gupta SC (2016) Redefining the ideal buttocks: a population analysis. Plast Reconstr Surg 137(6):1739–1747. https://doi.org/10.1097/PRS.0000000000002192
Funding
None.
Author information
Authors and Affiliations
Contributions
Stivala A. Data management. di Summa P. Manuscript writing. Bernard C. Data analysis. Moris V. Data collection. See L.A. Manuscript editing. Loffroy R. Protocol development. Zwetyenga N. Project development. Cheynel N. Project development. Guillier D. Protocol and project developments, Manuscript writing and editing.
Corresponding author
Ethics declarations
Conflict of interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Stivala, A., di Summa, P.G., Bernard, C. et al. The infragluteal fold: An appraisal by MRI combined with an anatomic study. Surg Radiol Anat 43, 1131–1139 (2021). https://doi.org/10.1007/s00276-020-02636-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-020-02636-y