Abstract
Purpose
The aim of the present study was to identify the hepatic vascular variations with visual three-dimensional (3D) reconstruction of vessels in pediatric patients with choledochal cyst (CDC).
Methods
We retrospectively analyzed the data of 84 children with pathologically confirmed CDCs treated in the Children's Hospital of Soochow University. 180 patients without CDCs as a control to analysis the hepatic artery and portal vein anatomy. All patients were examined by multi-slice spiral CT (MSCT) and the images of children with CDC were reconstructed by Hisense computer-assisted surgery system (Hisense CAS) to obtain visual 3D images.
Results
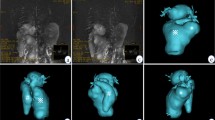
There were 71 females and 13 males diagnosed with CDC. According to Todani classification of CDC, there were 42 cases of type Ia, 10 cases of type Ic and 32 cases of type IVa. There were 10 (11.9%) patients with hepatic artery variations, 14 (16.7%) patients with right hepatic artery located on the ventral side of the CDC, and 16 (19.0%) patients with portal vein variations. Sex, age and types of the cyst were not associated with the presence of vascular variations. There was no significant difference in hepatic vascular variation between CDCs and control groups. Visual 3D images clearly displayed the hepatic vascular variations and the spatial structure of the CDC in pediatric patients with CDC.
Conclusions
Hepatic artery and portal vein variations can be detected in pediatric patients with CDC. Visual 3D technique can visually and stereoscopically display the anatomical variations of the hepatic artery and portal vein.













Similar content being viewed by others
Abbreviations
- CDC:
-
Choledochal cyst
- 3D:
-
Three-dimensional
- MSCT:
-
Multi-slice spiral CT
- Hisense CAS:
-
Hisense computer-assisted surgery
- MPR:
-
Multiplanar reformation
- MIP:
-
Maximum intensity projection
- LHA:
-
Left hepatic artery
- RHA:
-
Right hepatic artery
- LGA:
-
Left gastric artery
- SMA:
-
Superior mesenteric artery
- MPV:
-
Main portal vein
- MPV:
-
Main portal vein
- RPV:
-
Right portal vein
- LPV:
-
Left portal vein
- RAPV:
-
Right anterior portal vein
- RPPV:
-
Right posterior portal vein
- CHD:
-
Common hepatic duct
- CBD:
-
Common bile duct
References
Albers BK, Khanna G (2019) Vascular anomalies of the pediatric liver. Radiographics 39(3):842–856. https://doi.org/10.1148/rg.2019180146
Atasoy C, Ozyürek E (2006) Prevalence and types of main and right portal vein branching variations on MDCT. AJR Am J Roentgenol 187(3):676–681. https://doi.org/10.2214/AJR.05.0847
Blumgart LH, Hann LE (2000) Surgical and radiological anatomy of the liver and biliary tree. In: Blumgart LH, Fong Y (eds) Surgery of the liver and biliary tract, 3rd edn. Saunders, New York, pp 3–34
Chamberlain RS, El-Sedfy A, Rajkumar D (2011) Aberrant hepatic arterial anatomy and the whipple procedure: lessons learned. Am Surg 77(5):517–526
Chand K, Bhatnagar V, Agarwala S et al (2015) The incidence of portal hypertension in children with choledochal cyst and the correlation of nitric oxide levels in the peripheral blood with portal pressure and liver histology. J Indian Assoc Pediatr Surg 20(3):133–138. https://doi.org/10.4103/0971-9261.159024
Couinaud C (1999) Liver anatomy portal (and suprahepatic) or biliary segmentation. Dig Surg 16(9):459–467. https://doi.org/10.1159/000018770
Diao M, Li L, Li Q et al (2014) Challenges and strategies for single-incision laparoscopic Roux-en-Y hepaticojejunostomy in managing giant choledochal cysts. Int J Surg 12(5):412–417. https://doi.org/10.1016/j.ijsu.2014.03.007
Gadelhak N, Shehta A, Hamed H (2014) Diagnosis and management of choledochal cyst: 20 years of single center experience. World J Gastroenterol 20(22):7061–7066. https://doi.org/10.3748/wjg.v20.i22.7061
Hiatt JR, Gabbay J, Busuttil RW (1994) Surgical anatomy of the hepatic arteries in 1000 cases. Ann Surg 220(1):50–52. https://doi.org/10.1097/00000658-199407000-00008
Jang JY, Yoon YS, Kang MJ et al (2013) Laparoscopic excision of a choledochal cyst in 82 consecutive patients. Surg Endosc 27(5):1648–1652. https://doi.org/10.1007/s00464-012-2646-0
Nakayama K, Oshiro Y, Miyamoto R et al (2017) The effect of three-dimensional preoperative simulation on liver surgery. World J Surg 41(7):1840–1847. https://doi.org/10.1007/s00268-017-3933-7
Kurumi YTT, Hanasawa K et al (2000) The prevention of bile duct injury during laparoscopic cholecystectomy from the point of view of anatomic variation. Surg Laparosc Endosc Percutan Tech 10(4):192. https://doi.org/10.1097/00019509-200008000-00002
Lal R, Behari A, Hari RH et al (2013) Variations in biliary ductal and hepatic vascular anatomy and their relevance to the surgical management of choledochal cysts. Pediatr Surg Int 29(8):777–786. https://doi.org/10.1007/s00383-013-3333-5
Park SW, Koh H, Oh JT et al (2014) Relationship between anomalous pancreaticobiliary ductal union and pathologic inflammation of bile duct in choledochal cyst. Pediatr Gastroenterol Hepatol Nutr 17(3):170–177. https://doi.org/10.5223/pghn.2014.17.3.170
Ronnekleiv-Kelly SM, Soares KC, Ejaz A, Pawlik TM (2016) Management of CDCs. Curr Opin Gastroenterol 32(3):225–231. https://doi.org/10.1097/MOG.0000000000000256
Sarin Y (2005) Biliary ductal and vascular anomalies associated with choledochal cyst. J Indian Assoc Pediatr Surg. https://doi.org/10.4103/0971-9261.16467
Schmidt SC, Settmacher U, Langrehr JM et al (2004) Management and outcome of patients with combined bile duct and hepatic arterial injuries after laparoscopic cholecystectomy. Surgery 135(6):613–618. https://doi.org/10.1016/j.surg.2003.11.018
Shimotakahara A, Yamataka A, Yanai T et al (2005) Roux-en-Y hepaticojejunostomy or hepaticoduodenostomy for biliary reconstruction during the surgical treatment of choledochal cyst: which is better? Pediatr Surg Int 21(1):5–7. https://doi.org/10.1007/s00383-004-1252-1
Shinozaki K, Ajiki T, Matsumoto T et al (2016) Anatomical variations of liver blood supply in patients with pancreaticobiliary maljunction. Surg Today 46(2):169–175. https://doi.org/10.1007/s00595-015-1118-2
Shukla PJ, Barreto SG, Kulkarni A et al (2010) Vascular anomalies encountered during pancreatoduodenectomy: do they influence outcomes? Ann Surg Oncol 17(1):186–193. https://doi.org/10.1245/s10434-009-0757-1
Soares KC, Goldstein SD, Ghaseb MA et al (2017) Pediatric choledochal cysts: diagnosis and current management. Pediatr Surg Int 33(6):637–650. https://doi.org/10.1007/s00383-017-4083-6
Su L, Dong Q, Zhang H et al (2016) Clinical application of a three-dimensional imaging technique in infants and young children with complex liver tumors. Pediatr Surg Int 32(4):387–395. https://doi.org/10.1007/s00383-016-3864-7
Sureka B, Mukund A (2017) Review of imaging in post-laparoscopy cholecystectomy complications. Indian J Radiol Imaging 27(4):470–481. https://doi.org/10.4103/ijri.IJRI_489_16
Ten Hove A, de Meijer VE, Hulscher JBF, Kleine RHJ (2018) Meta-analysis of risk of developing malignancy in congenital choledochal malformation. Br J Surg 105(5):482–490. https://doi.org/10.1002/bjs.10798
Todani T, Watanabe Y, Narusue M et al (1977) Congenital bile duct cysts: classification, operative procedures, and review of thirty-seven cases including cancer arising from choledochal cyst. Am J Surg 134(2):263–269. https://doi.org/10.1016/0002-9610(77)90359-2
Tyson GL, El-Serag HB (2011) Risk factors for cholangiocarcinoma. Hepatology 54(1):173–184. https://doi.org/10.1002/hep.24351
Wang DC, Liu ZP, Li ZH et al (2012) Surgical treatment of congenital biliary duct cyst. BMC Gastroenterol 12:29. https://doi.org/10.1186/1471-230X-12-29
Funding
This work was supported by the National Natural Science Foundation of China [Grant no. 81971685].
Author information
Authors and Affiliations
Contributions
JW: protocol/project development; WC, LZ, WG: data collection or management; LZ, WC: data analysis; WC, WG: manuscript writing/editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chen, W., Zhao, L., Wang, J. et al. Hepatic vascular variations and visual three-dimensional reconstruction technique in pediatric patients with choledochal cyst. Surg Radiol Anat 42, 1489–1499 (2020). https://doi.org/10.1007/s00276-020-02590-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-020-02590-9