Abstract
Purpose
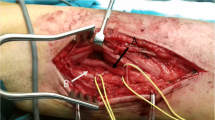
The neurotomy of musculocutaneous nerve is a treatment for patients who suffer from spastic elbow flexion when medical and reeducative treatments have failed. It consists in sectioning motor branches of musculocutaneous nerve which are destined to the biceps brachii and brachialis muscles, both being the main elbow flexor muscles. The aim of this study was to analyse the distance, where each motor branch arises from the musculocutaneous nerve to both biceps brachii and brachialis muscles, to establish precisely the localisation and length of the necessary incision to reach its branches for surgery.
Materials and methods
Eighteen musculocutaneous nerves from ten cadavers were dissected. None of them reported with a previous pathology. The cadavers were laid on the back with 30–35° of abduction, a complete extension, and supination of the upper limb.
Results
The localization of motor branches was to be found in the middle third of the upper arm, with an average from the base of the humeral major tubercle of 11.46, 12.40, and 12.87 cm for the biceps brachii and 16.36, 19.10, and 16.88 cm for the brachialis muscle.
Conclusion
The incision needed to reach the motor branches of the musculocutaneous nerve should be localised between 10 and 20 cm from the major humeral tubercle and may be shorter than usual.




Similar content being viewed by others
References
Netter FH (2011) Atlas d’anatomie humaine, Section VI, Membre supérieur, 5ème edition. Elsevier-Masson, Issy-les-Moulineaux, pp 400–404, 442–443
Kamina P (2009) Anatomie clinique, Tome 1, Anatomie générale-membres, 4ème edition. Maloine, pp 122–128, 219–222, 265–268, 293–314
Lazorthes G (1981) Le système nerveux périphérique, 3ème edition. Masson, Paris
Sunderland S (1972) Nerves and Nerve Injuries. Churchill Livingstone, Edinburgh
Carlson MG, Hearns KA, Inkellis E, Leach ME (2011) Early results of surgical intervention for elbow deformity in cerebral palsy based on degree of contracture. J Hand Surg-am 37(8):1665–1671
Gracies JM, Bayle N, Goldberg S, Simpson DM (2014) Botulinum toxin type B in the spastic arm: a randomized, double-blind, placebo-controlled, preliminary study. Arch Phys Med Rehabil 95(7):1303–1311
Takekawa T, Abo M, Ebihara K, Taguchi K, Sase Y, Kakuda W (2013) Long-term effects of injection of botulinum toxin type A combined with home-based functional training for post-stroke patients with spastic upper limb hemiparesis. Acta Neurol Belg 113(4):469–475
Buxton N (2011) Neurosurgical management of spasticity. Paediatr Child Health 21(10):473–474
Maarrawi J, Mertens, Sindou M (2005) Surgery in the peripheral nerves for upper limb spasticity. Oper Tech Neurosurg 7(3):147–152
Puligopu AK1, Purohit AK (2011) Outcome of selective motor fasciculotomy in the treatment of upper limb spasticity. J Pediatr Neurosci 6:S118–S125
Bird SJ (2014) The musculocutaneous nerve. Encycl Neurol Sci 215–216:303–304
Lee JH, Kim HW, Im S, An X, Lee MS, Lee UY, Han SH (2009) Localization of motor entry points and terminal intramuscular nerve endings of the musculocutaneous nerve to biceps and brachialis muscles. Surg Radiol Anat 32(3):213–220
IlayperumaI, Nanayakkara BG, Hasan R, Uluwitiya SM, Palahepitiya KN (2015) Coracobrachialis muscle: morphology, morphometry and gender differences. Surg Radiol Anat. doi:10.1007/s00276-015-1564-y
Gümüşalan Y, Yazar F, Ozan H (1998) Variant innervation of the coracobrachialis muscle and unusual course of the musculocutaneous nerve in man. Kaibogaku Zasshi 73(3):269–272
Remerand F, Laulan J, Couvret C, Palud M, Baud A, Velut S, Laffon M, Fusciardi J (2010) Is the musculocutaneous nerve really in the coracobrachialis muscle when performing an axillary block? An ultrasound study. Anesth Analg 110:1729–1734
Sung-Yoon W, Young-Hoon C, You-Jin C, Vittorio F, Hee-Soon W, Ki-Yeon C, Kyung-Seok H, Hee-Jin K (2015) Intramuscular innervation patterns of the brachialis muscle. Clin Anat 28:123–127
Cage TA, Simon NG, Bourque S, Noss R, Engstrom JW, Ralph JW, Kliot M (2013) Dual reinnervation of biceps muscle after side-to-side anastomosis of an intact median nerve and a damaged musculocutaneous nerve. J Neurosurg 119(4):929–933
Kjelstrup T, Sauter AR, Hol PK (2015) The relationship of the musculocutaneous nerve to the brachial plexus evaluated by MRI. J Clin Monit Comp. doi:10.1007/s10877-015-9807-3
Lafosse T, Masmejean E, Bihel T, Lafosse L (2015) Brachial plexus endoscopic dissection and correlation with open dissection. Chir Main 34(6):286–293
Sethi PM, Vadasdi K, Greene RT, Vitale MA, Duong M, Miller SR (2015) Safety of open suprapectoral and subpectoral biceps tenodesis: an anatomic assessment of risk for neurologic injury. J Shoulder Elb Surg 24:138–142
Pianezza A, Salces y Nedeo A, Chaynes P, Bickler PE, Minville V (2012) The emergence level of the musculocutaneous nerve from the brachial plexus: implications for infraclavicular nerve blocks. Anesth Analg 114(5):1131–1133
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Thieffry, C., Chenin, L., Foulon, P. et al. Microsurgical anatomy of branches of musculocutaneous nerve: clinical relevance for spastic elbow surgery. Surg Radiol Anat 39, 773–778 (2017). https://doi.org/10.1007/s00276-016-1800-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-016-1800-0