Abstract
Purpose
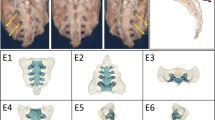
Identification of the second dorsal sacral foramen (S2F) by sonographic imaging is a possible first step in localising the branches of the dorsal sacral rami. The aim of this investigation is to develop an imaging approach to assist the rapid identification of S2F using a well-known regional landmark, the posterior superior iliac spine (PSIS).
Methods
Twenty-seven skeletal specimens were digitally imaged. Repeated measurements were undertaken of the angle and distance (D1) between PSIS and S2F, maximum width of S2F (D2), interforaminal distance between contralateral S2F (D3), distance between S1F and S2F (D4), and distance between S2F and S3F (D5). Sonographically guided needle placement was further undertaken to validate these osseous measurements in five intact cadavers.
Results
In skeletal material, repeated measurements indicated high intraclass correlation coefficients. No statistically significant difference existed in any measure between sides. Combined measurements indicated that S2F was located 46.4 ± 14.9° from the PSIS in both sexes, with a statistical trend toward a greater angle in females. D1 had a mean value 2.2 ± 0.62 cm but was significantly shorter in females. The mean values of D2 and D3 were 0.75 ± 0.18 cm and 2.98 ± 0.27 cm, respectively, with no significant difference between sexes. The mean value of D4 was 1.42 ± 0.27 cm with a statistical trend toward a slightly smaller value in females. The mean value for D5 was 1.28 ± 0.15 cm. Sonographically guided needle placement in cadavers tended to validate these osseous measurements.
Conclusions
S2F has a mean maximum width of 0.76 cm and lies approximately 2–3 cm from the PSIS, 45° inferior to the horizontal. The medial left and right borders of S2F are approximately 3 cm apart. The upper three ipsilateral dorsal sacral foramina are 1–1.5 cm apart. These measurements may be useful for sonographers imaging the dorsal sacral region and eventually, for the potential identification of neurovascular branches of the dorsal sacral rami.



Similar content being viewed by others
References
Asher MA, Strippgen WE (1986) Anthropometric studies of the human sacrum relating to dorsal trans-sacral implant designs. Clin Orthop Relat Res 203:58–62
Berthelot J-M, Labat J-J, Le Goff B (2009) Origine ligamentaire de certaines douleurs sacro-iliaques (concept de sacro-iliaque lato sensu) Sacro-iliac pain from ligamentous origin. Rev Rhum 76:786–794
Braun J, Bollow M, Seyrekbasan F et al (1996) Computed tomography guided corticosteroid injection of sacroiliac joint in patients with spondyloarthropathy with sacroiliitis: clinical outcome and follow up by dynamic magnetic resonance imaging. J Rheumatol 23:659–664
Chakraverty R, Pynsent P, Isaacs K (2007) Which spinal levels are identified by palpation of the iliac crests and the posterior superior iliac spines? J Anat 210:232–236
Cohen SP, Hurley RW, Buckenmaier CC et al (2008) Randomized placebo-controlled study evaluating lateral branch radiofrequency denervation for sacroiliac joint pain. Anesthesiology 109:279–288
Danelli G, Gardini M, Gemmi D et al (2009) Ultrasound and peripheral blocks for acute and chronic pain: a review. Eur J Pain 3:145–148
Dreyfuss P, Henning T, Malladi N et al (2009) The ability of multi-site, multi-depth sacral lateral branch blocks to anesthetize the sacroiliac joint complex. Pain Med 10:679–688
Hendrix RW, Lin PP, Kane WJ (1982) Simplified aspiration or injection technique for the sacroiliac joint. J Bone Joint Surg Am 64:1249–1252
Kaul A, Bauer B, Bernhardt J et al (1997) Effective doses to members of the public from the diagnostic application of ionizing radiation in Germany. Eur Radiol 7:1127–1132
Kim HW, Ko YJ, Rhee WI et al (2007) Interexaminer reliability and accuracy of posterior superior iliac spine and iliac crest palpation for spinal level estimations. J Manipulative Physiol Ther 30:386–389
Klauser A, De Zordo T, Feuchtner G et al (2008) Feasibility of ultrasound guided sacroiliac joint injection considering sonographic landmarks at two different levels in cadavers and patients. Arthritis Rheum 59:1618–1624
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
McGaugh JM, Brismee JM, Dedrick GS (2007) Comparing the anatomical consistency of the posterior superior iliac spine to the iliac crest as reference landmarks for the lumbopelvic spine: a retrospective radiological study. Clin Anat 20:819–825
McGrath C, Nicholson H, Hurst P (2010) Branch blockade of the sacral dorsal rami. Pain Med 11:281–282
McGrath C, Nicholson H, Hurst P (2009) The long posterior sacroiliac ligament: a histological study of morphological relations in the posterior sacroiliac region. Joint Bone Spine 76:57–62
McMinn RM (1998) Last’s Anatomy (1998), 9th edn. Churchill Livingstone Elsevier, Edinburgh, pp 217
Muhlner SB (2009) Review article: radiofrequency neurotomy for the treatment of sacroiliac joint syndrome. Curr Rev Musculoskelet Med 2:10–14
O’Haire C, Gibbons P (2000) Inter-examiner and intra-examiner agreement for assessing sacroiliac anatomical landmarks using palpation and observation: pilot study. Man Ther 5:13–20
Rosse C, Gaddum-Rosse P (1997) Hollinshead’s textbook of anatomy, 5th edn. Lippencott-Raven, Philadelphia, pp 311
Saladin KS (2007) Anatomy and physiology: the unity of form and function, 4th edn. McGraw Hill, New York, pp 394
Standring S (2008) Gray’s anatomy—the anatomical basis of clinical practice, 40th edn. Churchill Livingstone, Edinburgh, pp 747, 1340, 1366
Yin W, Willard F, Carreiro J et al (2003) Sensory stimulation-guided sacroiliac joint radiofrequency neurotomy: technique based on neuroanatomy of the dorsal sacral plexus. Spine 28:2419–2425
Acknowledgments
Gratitude is extended to the following: Mr. Tom Lawson, economics honours student, University of Otago, for statistical assistance and to Mr. Andrew Gray, Research Fellow, Biostatistical Support Service, Department of Preventive and Social Medicine, University of Otago, for his initial comments; Ms. Ruth Jeffrey BA, MSc, Medical Radiation Technologist (Ultrasound and Nuclear Medicine), provided invaluable technical assistance.
Conflict of interest
MCM holds an unpaid visiting research position and MDS is an employed academic of the University of Otago. The authors identify no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
McGrath, M.C., Stringer, M.D. Bony landmarks in the sacral region: the posterior superior iliac spine and the second dorsal sacral foramina: a potential guide for sonography. Surg Radiol Anat 33, 279–286 (2011). https://doi.org/10.1007/s00276-010-0735-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-010-0735-0