Abstract
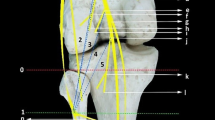
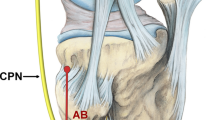
The tibial nerve has been reported to be often iatrogenically injured during fibular graft harvest, high tibial osteotomy and fascial release procedures. Despite this complication, there are limited data available in the literature concerning the surgical anatomy of tibial nerve branches in the deep posterior compartment of the leg. The aim of the present study was to quantitative and localize the motor nerve points for the flexor hallucis longus (FHL), tibialis posterior (TP) and flexor digitorum longus muscles (FDL) in relation to a regional bony landmark. The range for the number of branches of the tibial nerve and the terminal motor points of each muscle were identified and measurements were made with a digital caliper from these points to the apex of the head of fibula. Three particular types in the branching of tibial nerve were determined. In 55.6% of the cases there were separate branches to each of the muscles in the deep posterior compartment of the leg (Type I). In 30.6% of the cases there were two main branches of the tibial nerve that provided motor branches (Type II). Finally, the tibial nerve had one main branch, which gave rise to separate motor branches to each of the muscles in 13.8% (Type III). In 61.1% of the cases the FHL was innervated by proximal and distal branches of the tibial nerve. In 38.9% of the cases, it was innervated only by one proximal branch. In all of our cases, the TP was innervated by both proximal and distal branches and the FDL innervated only distally. This provided a detailed anatomical description of the tibial nerve in the deep posterior compartment of the leg. Knowledge of the variable peripheral course of the tibial nerve, as well as the detailed anatomy of its motor branches may decrease iatrogenic injuries and motor loss of the foot during surgical procedures.




Similar content being viewed by others
References
Babovic S, Johnson CH, Finical SJ (2000) Free fibula donor-site morbidity: the Mayo experience with 100 consecutive harvests. J Reconstr Microsurg 16:107–110
Belt PJ, Dickinson IC, Theile DR (2005) Vascularised free fibular flap in bone resection and reconstruction. Br J Plast Surg 58:425–430
Bodily KD, Spinner RJ, Bishop AT (2004) Restoration of motor function of the deep fibular (peroneal) nerve by direct nerve transfer of branches from the tibial nerve: an anatomical study. Clin Anat 17:201–205
Daniels TR, Thomas R, Bell TH, Neligan PC (2005) Functional outcome of the foot and ankle after free fibular graft. Foot Ankle Int 26:597–601
Georgoulis AD, Makris CA, Papageorgiou CD, Moebius UG, Xenakis T, Soucacos PN (1999) Nerve and vessel injuries during high tibial osteotomy combined with distal fibular osteotomy: a clinically relevant anatomic study. Knee Surg Sports Traumatol Arthrosc 7:15–19
Hidalgo DA, Rekow A (1995) A review of 60 consecutive fibula free flap mandible reconstructions. Plast Reconstr Surg 96:585–596
Kim MW, Kim JH, Yang YJ, Ko YJ (2005) Anatomic localization of motor points in gastrocnemius and soleus muscles. Am J Phys Med Rehabil 84:680–683
Kwiatkowski TC, Detmer DE (1997) Anatomical dissection of the deep posterior compartment and its correlation with clinical reports of chronic compartment syndrome involving the deep posterior compartment. Clin Anat 10:104–111
Minami A, Kasashima T, Iwasaki N, Kato H, Kaneda K (2000) Vascularised fibular grafts. An experience of 102 patients. J Bone Joint Surg Br 82:1022–1025
Nathan SS, Hung-Yi L, Disa JJ, Athanasian E, Boland P, Cordeiro PG, Healey JH (2005) Ankle instability after vascularized fibular harvest for tumor reconstruction. Ann Surg Oncol 12:57–64
Romanes GJ (1972) The peripheral nervous system. In: Cunningham’s textbook of anatomy. Oxford University Press, London, pp 765–770
Ruch DS, Koman LA (1997) The fibula-flexor hallucis longus osteomuscular flap. J Bone Joint Surg Br 79:964–988
Rupp RE, Podeszwa D, Ebraheim NA (1994) Danger zones associated with fibular osteotomy. J Orthop Trauma 8:54–58
Sindou M, Mertens P (1988) Selective neurotomy of the tibial nerve for treatment of the spastic foot. Neurosurgery 23:738–744
Stitgen SH, Cairns ER, Ebraheim NA, Niemann JM, Jackson WT (1992) Anatomic considerations of pin placement in the proximal tibia and its relationship to the peroneal nerve. Clin Orthop Relat Res 278:134–137
Standring S (2005) Gray’s anatomy. Elsevier Churchill Livingstone, London, pp 1504–1505
Vail TP, Urbaniak JR (1996) Donor-site morbidity with use of vascularized autogenous fibular grafts. J Bone Joint Surg Am 78:204–211
Williams PL (1999) Gray’s anatomy. Churchill Livingstone, London, pp 1284–1286
Wongphaet P, Chinsethagij K, Suarchawaratana S, Dangprasert T, Wongphaet W (2005) Precise localization of motor branching and motor points: a cadeveric study. J Med Assoc Thai 88:1884–1891
Wootton JR, Ashworth MJ, MacLaren CA (1995) Neurological complications of high tibial osteotomy-the fibular osteotomy as a causative factor: a clinical and anatomical study. Ann R Coll Surg Engl 77:31–34
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Apaydin, N., Loukas, M., Kendir, S. et al. The precise localization of distal motor branches of the tibial nerve in the deep posterior compartment of the leg. Surg Radiol Anat 30, 291–295 (2008). https://doi.org/10.1007/s00276-008-0321-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-008-0321-x