Abstract
Purpose: To examine changes in the reference segment luminal diameter after coronary angioplasty.
Methods: Sixty-one patients with stable angina pectoris or old myocardial infarction were examined. Coronary angiograms were recorded before coronary angioplasty (pre-angioplasty) and immediately after (post-angioplasty), as well as 3 months after. Artery diameters were measured on cine-film using quantitative coronary angiographic analysis.
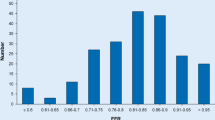
Results: The diameters of the proximal segment not involved in the balloon inflation and segments in the other artery did not change significantly after angioplasty, but the reference segment diameter significantly decreased (4.7%). More than 10% luminal reduction was observed in seven patients (11 %) and more than 5% reduction was observed in 25 patients (41%). More than 5% underestimation of the stenosis was observed in 22 patients (36%) when the post-angioplasty reference diameter was used as the reference diameter, compared with when the pre-angioplasty measurement was used and more than 10% underestimation was observed in five patients (8%).
Conclusion: This study indicated that evaluation by percent diameter stenosis, with the reference diameter from immediately after angioplasty, overestimates the dilative effects of coronary angioplasty, and that it is thus better to evaluate the efficacy of angioplasty using the absolute diameter in addition to percent luminal stenosis.
Similar content being viewed by others
References
Detre K, Holubkov R, Kelsey S, Cowley M. Kent K, Williams D, Myler R, Faxon D, Holmes D, Bourassa M, Block P, Gosselin A, Bentivoglio L, Leatherman L, Dorros G, King S. Galichia J, Al-Bassam M, Leon M, Robertson T, Passamani E, and the Coinvestigators of the NHLBI’s PTCA Registry (1988) Percutaneous transluminal coronary angioplasty in 1985–1986 and 1977–1981. The National Heart, Lung, and Blood Institute Registry. N Engl J Med 318:265–270
Topol EJ, Ellis SG, Cosgrove DM. Bates ER, Muller DWM, Schork NJ, Schork MA, Loop FD (1993) Analysis of coronary angioplasty practice in the United States with an insurance-claims data base. Circulation 87:1489–1497
Virmani R, Farb A, Burke AP (1994) Coronary angioplasty from the perspective of atherosclerotic plaque: Morphologic predictors of immediate success and restenosis. Am Heart J 127:163–179
Golino P, Ashton JH, Buja M, Rosolowsky M, Taylor AL, McNatt J, Campbell WB, Willerson JT (1989) Local platelet activation causes vasoconstriction of large epicardial canine coronary arteries in vivo: Thromboxane A2 and serotonin are possible mediators. Circulation 79:154–166
Arnett EN, Isner JM, Redwood DR, Kent KM, Baker WP, Ackerstein H, Roberts WC (1979) Coronary artery narrowing in coronary heart disease. Comparison of cineangiography and necropsy findings. Ann Int Med 91:350–356
Clowes AW, Reidy MA, Clowes M (1983) Kinetics of cellular proliferation after arterial injury. I. Smooth muscle growth in the absence of endothelium. Lab Invest 49:327–333
Baumgartner HR, Spaet TH (1970) Endothelial replacement in rabbit arteries. Fed Proc 29:710–715
de Feyter PJ, Serruys PW, Davies MJ, Richardson P, Lubsen J, Oliver MF (1991) Quantitative coronary angiography to measure progression and regression of coronary atherosclerosis: Value, limitations, and implications for clinical trials. Circulation 84:412–423
Strauss BH, Escaned J, Foley DP, di Mario C, Haase J, Keane D, Hermans WRM, ter de Feyter PJ, Serruys PW (1994) Technologic considerations and practical limitations in the use of quantitative angiography during percutaneous coronary recanalization. Prog Cardiovasc Dis 36:343–362
Nissen SE (1993) Radiographic principles in cardiac catheterization. In: Roubin GS, Califf RM O’Neill W. Phillips H, Slack RS (eds) Interventional Cardiac Catheterization: Principles and Practice. Churchill Livingstone, New York, pp 409–425
Fischell TA, Nellessen U, Johnson DE, Ginsburg R (1989) Endothclium-dependent arterial vasoconstriction after balloon angioplasty. Circulation 79:899–910
El-Tamimi H, Davies GJ, Hackett D, Sritara P. Bertrand O. Crea F. Maseri A (1991) Abnormal vasomotor changes early after coronary angioplasty: A quantitative arteriographic study of their lime course. Circulation 84:1198–1202
Gregorini L, Fajadet J, Robert G, Cassagneau B, Bernis M, Marco J (1994) Coronary vasoconstriction after percutaneous-iransluminal coronary angioplasty is attenuated by antiadrenergic agents. Circulation 90:895–907
Foley DP, Deckers J, van den Bos AA, Heyndrickx GR, Laarman G, Suryapranata H, Zijlstra F, Serruys P (1993) Usefulness of repeat coronary angiography 24 hours after successful balloon angioplasty to evaluate early luminal deterioration and facilitate quantitative analysis. Am J Cardiol 72:1341–1347
Hermans WRM, Foley DP, Rensing BJ, Serruys PW (1994) Morphologic changes during follow-up after successful percutaneous transluminal coronary balloon angioplasty: Quantitative angiographic analysis in 778 lesions—further evidence for the restenosis paradox. Am Heart J 127:483–494
Beatt KJ, Luijten HE, de Feyter PJ, van den Brand M, Reiber JHC, Serruys PW (1988) Changes in diameter of coronary artery segments adjacent to stenosis after percutaneous transluminal coronary angioplasty: Failure of percent diameter stenosis measurement to reflect morphologic changes induced by balloon dilation. J Am Coll Cardiol 12:315–323
Rensing BJ, Hermans WRM, Deckers JW, de Feyter PJ, Tijssen JGP. Serruys PW (1992) Lumen narrowing after percutaneous transluminal coronary balloon angioplasty follows a near Gaussian distribution: A quantitative angiographic studv in 1,445 successfully dilated lesions. J Am Coll Cardiof 19:939–945
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Hirami, R., Iwasaki, K., Kusachi, S. et al. Instability of reference diameter in the evaluation of stenosis after coronary angioplasty: Percent diameter stenosis overestimates dilative effects due to reference diameter reduction. Cardiovasc Intervent Radiol 23, 182–186 (2000). https://doi.org/10.1007/s002700010040
Issue Date:
DOI: https://doi.org/10.1007/s002700010040