Abstract
Purpose
This study aims to provide a comprehensive review of the clinical benefits, complications, and safety profile associated with preoperative embolization in Glomus jugulare tumors (GJTs).
Materials and Methods
A comprehensive search in PubMed, Embase, and Web of Science was conducted for English articles published up to March 2023, focusing on GJTs and preoperative embolization. Included studies involved patients over 18 with GJTs. We excluded studies that explored embolization methods other than the standard endovascular approach, as well as studies involving paragangliomas that did not provide specific data related to GJTs. Key variables such as hemorrhage volume and surgical time, as well as clinical outcomes, were analyzed. Data were analyzed using a random-effects model meta-analysis, assessing heterogeneity with the I2 statistic.
Results
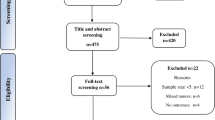
This review encompasses 19 studies with a total of 328 patients. The studies incorporated into our meta-analysis display considerable differences and inconsistencies in their data. The findings of the meta-analysis show a mean hemorrhage volume of 636 ml (95% confidence interval (CI) 473–799) following preoperative embolization, and a mean surgical duration of 487 min (95% CI 350–624). The study also notes potential complications: facial nerve deficits occurred in 20% of cases (95% CI 11–32%), and vagal nerve deficits in 22% (95% CI 13–31%).
Conclusion
This study suggests that preoperative embolization could decrease surgery duration and blood loss, but emphasizes the importance of evaluating risks like nerve damage. However, the generalizability of these findings is restricted due to the diversity of available data.
Graphical Abstract






Similar content being viewed by others
References
Erickson D, Kudva YC, Ebersold MJ, Thompson GB, Grant CS, van Heerden JA, Young WF Jr. Benign paragangliomas: clinical presentation and treatment outcomes in 236 patients. J Clin Endocrinol Metab. 2001;86(11):5210–6. https://doi.org/10.1210/jcem.86.11.8034.
Semaan MT, Megerian CA. Current assessment and management of glomus tumors. Curr Opin Otolaryngol Head Neck Surg. 2008;16(5):420–6. https://doi.org/10.1097/MOO.0b013e32830c4595.
Hosseinzadeh A, Rasekhi A, Borhani-Haghighi A, Asnaashari M, Abdollahifard S, Moein SA. Coil embolization of a pseudoaneurysm of the petrous internal carotid artery presenting with otorrhagia: A case report and review of the literature. Iran J Radiol. 2022;19(2):e119061. https://doi.org/10.5812/iranjradiol-119061.
Tokgoz SA, et al. Glomus tumors of the head and neck: thirteen years’ institutional experience and management. Acta Otolaryngol. 2019;139(10):930–3. https://doi.org/10.1080/00016489.2019.1655588.
Devuyst L, Defreyne L, Praet M, Geukens S, Dhooge I. Treatment of glomus tympanicum tumors by preoperative embolization and total surgical resection. Am J Otolaryngol. 2016;37(6):544–51. https://doi.org/10.1016/j.amjoto.2016.08.011.
Gaynor BG, Elhammady MS, Jethanamest D, Angeli SI, Aziz-Sultan MA. Incidence of cranial nerve palsy after preoperative embolization of glomus jugulare tumors using Onyx. J Neurosurg. 2014;120(2):377–81. https://doi.org/10.3171/2013.10.JNS13354.
Anakwenze OA, Parker WL, Schiefer TK, Inwards CY, Spinner RJ, Amadio PC. Clinical features of multiple glomus tumors. Dermatol Surg. 2008;34(7):884–90. https://doi.org/10.1111/j.1524-4725.2008.34173.x.
Saaiq M. Presentation and management outcome of glomus tumors of the hand. Arch Bone Jt Surg. 2021;9(3):312–8. https://doi.org/10.22038/abjs.2020.47878.2367.
Catapano JS, et al. Onyx embolization of skull base paragangliomas: a single-center experience. Acta Neurochir (Wien). 2020;162(4):821–9. https://doi.org/10.1007/s00701-019-04127-5.
Michelozzi C, et al. Arterial embolization with Onyx of head and neck paragangliomas. J Neurointerv Surg. 2016;8(6):626–35. https://doi.org/10.1136/neurintsurg-2014-011582.
Munn Z, Stone JC, Aromataris E, Klugar M, Sears K, Leonardi-Bee J, Barker TH. Assessing the risk of bias of quantitative analytical studies: introducing the vision for critical appraisal within JBI systematic reviews. JBI Evid Synth. 2023;21(3):467–71. https://doi.org/10.11124/jbies-22-00224.
Shi L, Lin L. The trim-and-fill method for publication bias: practical guidelines and recommendations based on a large database of meta-analyses, (in eng). Medicine (Baltimore). 2019;98(23):e15987. https://doi.org/10.1097/md.0000000000015987.
Simpson GT 2nd, Konrad HR, Takahashi M, House J. Immediate postembolization excision of glomus jugulare tumors: advantages of new combined techniques. Arch Otolaryngol. 1979;105(11):639–43. https://doi.org/10.1001/archotol.1979.00790230009002.
Helal A, et al. Preoperative embolization of jugular paraganglioma tumors using particles is safe and effective. Interv Neuroradiol. 2022;28(2):145–51. https://doi.org/10.1177/15910199211019175.
Murphy TP, Brackmann DE. Effects of preoperative embolization on glomus jugulare tumors. Laryngoscope. 1989;99(12):1244–7. https://doi.org/10.1288/00005537-198912000-00007.
Larouere MJ, Zappia JJ, Wilner HI, Graham MD, Lundy LB. Selective embolization of glomus jugulare tumors. Skull Base Surg. 1994;4(1):21–5. https://doi.org/10.1055/s-2008-1058984.
Young NM, Wiet RJ, Russell EJ, Monsell EM. Superselective embolization of glomus jugulare tumors. Ann Otol Rhinol Laryngol. 1988;97(6 Pt 1):613–20. https://doi.org/10.1177/000348948809700607.
Jacobs JM, Shelton C, Thompson BG. Combined transarterial and transvenous embolisation of jugulotympanic paragangliomas. Interv Neuroradiol. 1998;4(3):223–30. https://doi.org/10.1177/159101999800400306.
Siedek V, Waggershauser T, Berghaus A, Matthias C. Intraoperative monitoring of intraarterial paraganglioma embolization by indocyaningreen fluorescence angiography. Eur Arch Otorhinolaryngol. 2009;266(9):1449–54. https://doi.org/10.1007/s00405-008-0879-2.
Iampreechakul P, Tirakotai W, Lertbutsayanukul P, Siriwimonmas S, Liengudom A. Pre-operative embolization of intracranial and extracranial tumors: a review of 37 cases. J Med Assoc Thai. 2016;99(Suppl 3):S91-119.
Makiese O, Chibbaro S, Marsella M, Tran Ba Huy P, George B. Jugular foramen paragangliomas: Management, outcome and avoidance of complications in a series of 75 cases. Neurosurg Rev. 2012;35(20):185–94. https://doi.org/10.1007/s10143-011-0346-1.
Karaman E, et al. Management of jugular paragangliomas in otolaryngology practice. J Craniofac Surg. 2010;21(1):117–20. https://doi.org/10.1097/SCS.0b013e3181c466ce.
Abud DG, Mounayer C, Benndorf G, Piotin M, Spelle L, Moret J. Intratumoral injection of cyanoacrylate glue in head and neck paragangliomas. AJNR Am J Neuroradiol. 2004;25(9):1457–62.
Rebol J. Jugular paraganglioma treatment at the UMC Maribor. 2017. https://doi.org/10.6016/ZdravVestn.2491
Ladner TR, He L, Davis BJ, Yang GL, Wanna GB, Mocco J. Initial experience with dual-lumen balloon catheter injection for preoperative Onyx embolization of skull base paragangliomas. J Neurosurg. 2016;124(6):1813–9. https://doi.org/10.3171/2015.5.JNS15124.
Warren FM 3rd, McCool RR, Hunt JO, Hu N, Ng PP, Buchmann LP, Shelton C. Preoperative embolization of the inferior petrosal sinus in surgery for glomus jugulare tumors. Otol Neurotol. 2011;32(9):1538–41. https://doi.org/10.1097/MAO.0b013e318237fcf6.
White JB, Link MJ, Cloft HJ. Endovascular embolization of paragangliomas: a safe adjuvant to treatment. J Vasc Interv Neurol. 2008;1(2):37–41.
Boublata L. "Infratemporal approach with anterior transposition of facial nerve in paraganglioma surgery. Interdiscip Neurosurg. 2019. https://doi.org/10.1016/j.inat.2018.10.006.
Persky MS, Setton A, Niimi Y, Hartman J, Frank D, Berenstein A. Combined endovascular and surgical treatment of head and neck paragangliomas–a team approach. Head Neck. 2002;24(5):423–31. https://doi.org/10.1002/hed.10068.
Huy PT, Kania R, Duet M, Dessard-Diana B, Mazeron JJ, Benhamed R. Evolving concepts in the management of jugular paraganglioma: a comparison of radiotherapy and surgery in 88 cases. Skull Base. 2009;19(1):83–91. https://doi.org/10.1055/s-0028-1103125.
Harati A, Deitmer T, Rohde S, Ranft A, Weber W, Schultheiss R. Microsurgical treatment of large and giant tympanojugular paragangliomas. Surg Neurol Int. 2014;5:179. https://doi.org/10.4103/2152-7806.146833.
Pedro MKF. Preoperative endovascular embolization of glomus jugulare tumors: a retrospective case series of 22 embolizations in 20 patients and literature review. Arq Bras Neurocir Braz Neurosurg. 2021. https://doi.org/10.1136/neurintsurg-2014-011582.
Paramasivam S. Paraganglioma—Role of preoperative evaluation and endovascular embolization. Oper Tech Otolaryngol-Head Neck Surg. 2016. https://doi.org/10.1016/j.otot.2015.12.004.
De Marini P, et al. Safety and technical efficacy of pre-operative embolization of head and neck paragangliomas: A 10-year mono-centric experience and systematic review. Clin Imaging. 2021;80:292–9. https://doi.org/10.1016/j.clinimag.2021.08.014.
Moore MG, Netterville JL, Mendenhall WM, Isaacson B, Nussenbaum B. Head and neck paragangliomas: an update on evaluation and management. Otolaryngol Head Neck Surg. 2016;154(4):597–605. https://doi.org/10.1177/0194599815627667.
Funding
This study was not supported by any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed Consent
For this type of study informed consent is not required.
Consent for Publication
For this type of study consent for publication is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ghanaati, H., Zarei, D., Issaiy, M. et al. Efficacy and Safety of Preoperative Embolization in Glomus Jugulare Tumors: A Systematic Review and Meta-analysis of Clinical Outcomes and Complications. Cardiovasc Intervent Radiol 47, 416–431 (2024). https://doi.org/10.1007/s00270-024-03687-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-024-03687-z