Abstract
Purpose
To report techniques and results of 16 cryoablation procedures in 11 patients treated for recurrent head and neck cancer.
Methods and Materials
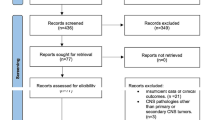
This retrospective study reviewed 11 consecutive patients with head and neck cancer recurrence after primary treatment by surgery and radiotherapy, treated with cryoablation between 2016 and 2020. Efficacy was measured by local control rate evaluated on MRI or/and PET. Tumor characteristics, number of cryoprobes, thermoprotective measures and complications were documented.
Results
Sixteen cryoablation procedures were performed in 11 patients with head and neck cancer recurrence after surgery or radiotherapy, deemed ineligible for classic salvage treatment. Among 11 patients, four were treated for an epidermoid carcinoma, four for an adenocarcinoma and three for other types: 1 muco-epidermoid carcinoma, 1 adenoid cystic carcinoma and 1 esthesioneuroblastoma, 10/11 patients had prior surgery, 7/11 patients had prior chemotherapy and 3/11 patients had prior radiotherapy. Median number of cryoprobes was 4, [IQR, 3–6 cryoprobes], thermoprotective measures to protect surrounding organs were required for 10/16 procedures. After cryoablation, local control rate was 45.4% at a mean follow-up of 11.7 months (range 3–34 months). Among the 16 cryoablation procedures, four resulted in complications, two were considered major complications: one septic shock on inhalation pneumopathy during extubation, requiring intensive care; and one dysphonia due to a recurrent nerve injury.
Conclusion
Cryoablation as a salvage treatment for recurrence of head and neck tumors after surgery and/or radiotherapy is an effective option, especially for patients that cannot benefit from salvage surgery.




Similar content being viewed by others
References
Pfister DG, Spencer S, Adelstein D, Adkins D, Anzai Y, Brizel DM, et al. Head and neck cancers, version 2.2020, NCCN clinical practice guidelines in oncology. J Natl Compr Cancer Netw. 2020;18:873–98.
Machiels J-P, René Leemans C, Golusinski W, Grau C, Licitra L, Gregoire V. Squamous cell carcinoma of the oral cavity, larynx, oropharynx and hypopharynx: EHNS–ESMO–ESTRO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2020;31:1462–75.
Chan ATC, Grégoire V, Lefebvre J-L, Licitra L, Hui EP, Leung SF, et al. Nasopharyngeal cancer: EHNS–ESMO–ESTRO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2012;23:vii83–5.
Zenga J, Graboyes E, Janz T, Drake V, Rettig E, Desai S, et al. Salvage of recurrence after surgery and adjuvant therapy: a multi-institutional study. Otolaryngol Head Neck Surg. 2019;161:74–81.
Dionisi F, Fiorica F, D’Angelo E, Maddalo M, Giacomelli I, Tornari E, et al. Organs at risk’s tolerance and dose limits for head and neck cancer re-irradiation: a literature review. Oral Oncol. 2019;98:35–47.
Hamoir M, Schmitz S, Suarez C, Strojan P, Hutcheson KA, Rodrigo JP, et al. The current role of salvage surgery in recurrent head and neck squamous cell carcinoma. Cancers [Internet]. 2018 [cited 2021 Apr 19]; 10. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6115801/
Rogers SN, Semple C, Babb M, Humphris G. Quality of life considerations in head and neck cancer: United Kingdom national multidisciplinary guidelines. J Laryngol Otol. 2016;130:S49-52.
Quek LHH, Lim MY, Cheo T, Teo HL, Pua U. Percutaneous management of recurrent head and neck cancer: current role and evolving principles in the multidisciplinary setting. Curr Oncol Rep. 2021;23:52.
Tsoumakidou G, Buy X, Garnon J, Enescu J, Gangi A. Percutaneous thermal ablation: how to protect the surrounding organs. Tech Vasc Interv Radiol. 2011;14:170–6.
Belfiore MP, Sciandra M, Romano F, Tartaglione T, Lucia GD, Volpe TD, et al. Preliminary results in unresectable head and neck cancer treated by radiofrequency and microwave ablation: feasibility, efficacy, and safety. J Vasc Interv Radiol Elsevier. 2015;26:1189–96.
Owen RP, Lee JS, Silver CE, Bäck L, Beitler JJ, Rinaldo A, et al. Radiofrequency ablation in advanced head and neck cancer. Eur Arch Otorhinolaryngol. 2014;271:207–10.
Brook AL, Gold MM, Miller TS, Gold T, Owen RP, Sanchez LS, et al. CT-guided radiofrequency ablation in the palliative treatment of recurrent advanced head and neck malignancies. J Vasc Interv Radiol. 2008;19:725–35.
Guenette JP, Tuncali K, Himes N, Shyn PB, Lee TC. Percutaneous image-guided cryoablation of head & neck tumors for local control, preservation of functional status, and pain relief. AJR Am J Roentgenol. 2017;208:453–8.
Gangi A, Cebula H, Cazzato RL, Ramamurthy N, Garnon J, Debry C, et al. “Keeping a cool head”: percutaneous imaging-guided cryo-ablation as salvage therapy for recurrent glioblastoma and head and neck tumours. Cardiovasc Intervent Radiol. 2020;43:172–5.
Magalov Z, Shitzer A, Degani D. Isothermal volume contours generated in a freezing gel by embedded cryo-needles with applications to cryo-surgery. Cryobiology. 2007;55:127–37.
Gangi A, Tsoumakidou G, Buy X, Quoix E. Quality improvement guidelines for bone tumour management. Cardiovasc Interv Radiol. 2010;33:706–13.
Robinson D, Halperin N, Nevo Z. Two freezing cycles ensure interface sterilization by cryosurgery during bone tumor resection. Cryobiology. 2001;43:4–10.
Kurup AN, Schmit GD, Morris JM, Atwell TD, Schmitz JJ, Weisbrod AJ, et al. Avoiding complications in bone and soft tissue ablation. Cardiovasc Interv Radiol. 2017;40:166–76.
Kurup AN, Morris JM, Schmit GD, Atwell TD, Weisbrod AJ, Murthy NS, et al. Neuroanatomic considerations in percutaneous tumor ablation. Radiographics. 2013;33:1195–215.
Filippiadis DK, Binkert C, Pellerin O, Hoffmann RT, Krajina A, Pereira PL. Cirse quality assurance document and standards for classification of complications: the cirse classification system. Cardiovasc Interv Radiol août. 2017;40(8):1141–6.
U.S department of health and human services. Common terminology criteria for adverse events (CTCAE), version 5.0 [Internet]. 2017 [cited 2018 Feb 20]. Available from: https://ctep.cancer.gov/protocoldevelopment/electronic_applications/docs/CTCAE_v5_Quick_Reference_5x7.pdf
Matoscevic K, Graf N, Pezier TF, Huber GF. Success of salvage treatment: a critical appraisal of salvage rates for different subsites of HNSCC. Otolaryngol Head Neck Surg. 2014;151:454–61.
Spencer SA, Harris J, Wheeler RH, Machtay M, Schultz C, Spanos W, et al. Final report of RTOG 9610, a multi-institutional trial of reirradiation and chemotherapy for unresectable recurrent squamous cell carcinoma of the head and neck. Head Neck. 2008;30:281–8.
Langer CJ, Harris J, Horwitz EM, Nicolaou N, Kies M, Curran W, et al. Phase II study of low-dose paclitaxel and cisplatin in combination with split-course concomitant twice-daily reirradiation in recurrent squamous cell carcinoma of the head and neck: results of Radiation Therapy Oncology Group Protocol 9911. J Clin Oncol. 2007;25:4800–5.
Vargo JA, Ward MC, Caudell JJ, Riaz N, Dunlap NE, Isrow D, et al. A multi-institutional comparison of SBRT and IMRT for definitive reirradiation of recurrent or second primary head and neck cancer. Int J Radiat Oncol Biol Phys. 2018;100:595–605.
Anand AK, Dua B, Bansal AK, Singh HM, Verma A, Kumar A. Stereotactic ablative radiotherapy (SABR) for recurrent and previously irradiated head and neck cancers. BJR Open [Internet]. 2020 [cited 2021 Apr 27]; 2. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7594905/
Vermorken JB, Mesia R, Rivera F, Remenar E, Kawecki A, Rottey S, et al. Platinum-based chemotherapy plus cetuximab in head and neck cancer [Internet]. Massachusetts Medical Society; 2009 [cited 2021 Apr 28]. Available from: https://doi.org/10.1056/NEJMoa0802656
Owen RP, Khan SA, Negassa A, Beitler JJ, Bello JA, Brook A, et al. Radiofrequency ablation of advanced head and neck cancer. Arch Otolaryngol Head Neck Surg. 2011;137(5):493.
Cazzato RL, Garnon J, Shaygi B, Tsoumakidou G, Caudrelier J, Koch G, et al. How to perform a routine cryoablation under MRI guidance. Top Magn Reson Imaging TMRI. 2018;27:33–8.
Funding
This study was not supported by any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Julien Garnon, MD, PhD: Proctor, Galil Medical Ltd. Afshin Gangi, MD, PhD: Proctor, Galil Medical Ltd. Other authors declare that they have no conflict of interest.
Ethical Approval
For this type of study formal consent is not required.
Informed Consent
Informed consent was obtained from all individual participants (or their parent) included in the study.
Consent for Publication
Consent for publication was obtained for every individual person’s data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Schwartz, J., Auloge, P., Koch, G. et al. Percutaneous Cryoablation for Recurrent Head and Neck Tumors. Cardiovasc Intervent Radiol 45, 791–799 (2022). https://doi.org/10.1007/s00270-022-03120-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-022-03120-3