Abstract
Purpose
Endovenous laser ablation may be associated with significant pain when performed under standard local tumescent anesthesia. The purpose of this study was to investigate the efficacy of femoral and sciatic nerve blocks for analgesia during endovenous ablation in patients with lower extremity venous insufficiency.
Methods
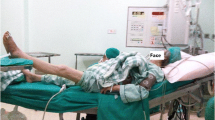
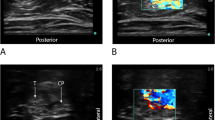
During a 28-month period, ultrasound-guided femoral or sciatic nerve blocks were performed to provide analgesia during endovenous laser ablation in 506 legs and 307 patients. The femoral block (n = 402) was performed at the level of the inguinal ligament, and the sciatic block at the posterior midthigh (n = 124), by injecting a diluted lidocaine solution under ultrasound guidance. After the blocks, endovenous laser ablations and other treatments (phlebectomy or foam sclerotherapy) were performed in the standard fashion. After the procedures, a visual analogue pain scale (1–10) was used for pain assessment.
Results
After the blocks, pain scores were 0 or 1 (no pain) in 240 legs, 2 or 3 (uncomfortable) in 225 legs, and 4 or 5 (annoying) in 41 legs. Patients never experienced any pain higher than score 5. The statistical analysis revealed no significant difference between the pain scores of the right leg versus the left leg (p = 0.321) and between the pain scores after the femoral versus sciatic block (p = 0.7).
Conclusions
Ultrasound-guided femoral and sciatic nerve blocks may provide considerable reduction of pain during endovenous laser and other treatments, such as ambulatory phlebectomy and foam sclerotherapy. They may make these procedures more comfortable for the patient and easier for the operator.




Similar content being viewed by others
References
Min RJ, Khilnani NM (2005) Endovenous laser ablation of varicose veins. J Cardiovasc Surg 46:395–405
Yilmaz S, Ceken K, Alparslan A et al (2007) Endovenous laser ablation for saphenous vein insufficiency: immediate and short-term results of our first 60 procedures. Diagn Interv Radiol 13:156–163
Hoggan BL et al (2009) Systematic review of the endovenous laser therapy versus surgery for the treatment of saphenous varicose veins. Ann Vasc Surg 23(2):277–287
Oguzkurt L (2011) Endovenous laser ablation for the treatment of varicose veins. Diagn Interv Radiol. doi:10.4261/1305-3825.DIR.5248-11.0
Van den Bos R et al (2009) Endovenous therapies of lower extremity varicosities: a meta-analysis. J Vasc Surg 49(1):230–239
Yilmaz S, Ceken K, Alparslan A et al (2011) Endovenous laser ablation and concomitant foam sclerotherapy: experience in 504 patients. Cardiovasc Intervent Radiol. doi:10.1007/s00270-011-0329-1
van den Bos R, Arends L, Kockaert M et al (2009) Endovenous therapies of lower extremity varicosities: a meta-analysis. J Vasc Surg 49:230–239
Dzieciuchowicz L, Espinosa G, Grochowicz L (2010) Evaluation of ultrasound-guided femoral nerve block in endoluminal laser ablation of the greater saphenous vein. Ann Vasc Surg 24(7):930–934
Marsh P, Price BA, Holdstock J et al (2010) Deep vein thrombosis (DVT) after venous thermoablation techniques: rates of endovenous heat-induced thrombosis (EHIT) and classical DVT after radiofrequency and endovenous laser ablation in a single centre. Eur J Vasc Endovasc Surg 40(4):521–527
Van Den Bos RR, Neumann M, De Roos KP et al (2009) Endovenous laser ablation-induced complications: review of the literature and new cases. Dermatol Surg 35:1206–1214
Auroy Y, Narchi P, Messiah A et al (1997) Serious complications related to regional anesthesia: results of a prospective survey in France. Anesthesiology 87(3):479–486
Svircevic V, van Dijk D, Nierich AP et al (2011) Meta-analysis of thoracic epidural anesthesia versus general anesthesia for cardiac surgery. Anesthesiology 114(2):271–282
Mulroy MF, Larkin KL, Batra MS et al (2001) Femoral nerve block with 0.25% or 0.5% bupivacaine improves postoperative analgesia following outpatient arthroscopic anterior cruciate ligament repair. Reg Anesth Pain Med 26:24–29
Mariano ER, Loland VJ, Sandhu NS et al (2009) Ultrasound guidance versus electrical stimulation for femoral perineural catheter insertion. J Ultrasound Med 28(11):1453–1460
Taylor EW, Fielding JW, Keighley MR et al (1981) Long saphenous vein stripping under local anaesthesia. Ann R Coll Surg Engl 63:206–207
Vloka JD, Hadzic A, Mulcare R et al (1997) Femoral and genitofemoral nerve blocks versus spinal anesthesia for outpatients undergoing long saphenous vein stripping surgery. Anesth Analg 84:749–752
Meier G, Buettner J (2007) Peripheral regional anesthesia. An atlas of anatomy and techniques. Georg Thieme Verlag, New York, pp 92–94
Mulroy FM, Bernards CM, McDonald SB et al (2009) A practical approach to regional anesthesia. Lippincott Williams & Wilkins, Philadelphia, pp 11–24
Fingerman M, Benonis JG, Martin G (2009) A practical guide to commonly performed ultrasound-guided peripheral-nerve blocks. Curr Opin Anaesthesiol 22:600–607
Coleridge Smith P (2009) Sclerotherapy and foam sclerotherapy for varicose veins. Phlebology 24:260–269
Mysore V, IADVL Dermatosurgery Task Force (2008) Tumescent liposuction: standard guidelines of care. Indian J Dermatol Venereol Leprol 74(Suppl):S54–S60
Ostad A, Kageyama N, Moy RL (1996) Tumescent anesthesia with a lidocaine dose of 55 mg/kg is safe for liposuction. Dermatol Surg 22(11):921–927
Brull R, Macfarlane AJ, Parrington SJ et al (2011) Is circumferential injection advantageous for ultrasound-guided popliteal sciatic nerve block? A proof-of-concept study. Reg Anesth Pain Med 36(3):266–270
Ilfeld BM (2011) Continuous peripheral nerve blocks: a review of the published evidence. Anesth Analg 113(4):904–925
Acknowledgment
The authors thank Akdeniz University Scientific Research Projects Unit for supporting this study. None of the authors has a financial arrangement or other relationship that could be construed as a conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yilmaz, S., Ceken, K., Alimoglu, E. et al. US-Guided Femoral and Sciatic Nerve Blocks for Analgesia During Endovenous Laser Ablation. Cardiovasc Intervent Radiol 36, 150–157 (2013). https://doi.org/10.1007/s00270-012-0366-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-012-0366-4