Abstract
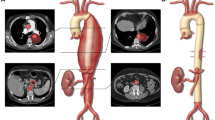
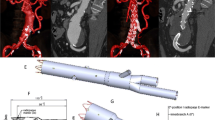
Endovascular treatment is an established therapy for thoracic aortic disease. Collapse of the endograft is a potentially fatal complication. We reviewed 16 patients with a thoracic endograft between 2001 and 2006. Medical records of the treated patients were studied. Data collected include age, gender, diagnosis, indication for endoluminal treatment, type of endograft, and time of follow up. All patients (n = 16; mean age, 61 years; range, 21–82 years) underwent computed tomography (CT) for location of the lesion and planning of the intervention. Time of follow-up with CT scan ranged from 1 to 61 months. Indications for endovascular treatment were degenerative aneurysm (n = 7; 44%), aortic dissection (n = 2; 12%), perforated aortic ulcer (n = 4; 25%), and traumatic aortic injury (n = 3; 19%). Three patients suffered from a collapse of the endograft (one patient distal, two patients proximal) between 3 and 8 days after endovascular treatment. These patients were younger (mean age, 37 ± 25 years vs. 67 ± 16 years; P < 0.05) and showed more oversizing (proximal, 36 ± 19.8% vs. 29 ± 20.7% [P > 0.05]; distal, 45 ± 23.5% vs. 38 ± 21.7% [P > 0.05]). Proximal collapse was corrected by placing a bare stent. In conclusion, risk factors for stent-graft collapse are a small lumen of the aorta and a small radius of the aortic arch curvature (young patients), as well as oversizing, which is an important risk factor and is described for different types of endografts and protheses (Gore TAG and Cook Zenith). Dilatation of the collapsed stent-graft is not sufficient. Following therapy implantation of a second stent or surgery is necessary in patients with a proximal endograft collapse. Distal endograft collapse can possibly be treated conservatively under close follow-up.




Similar content being viewed by others
References
Neuhauser B, Czermak B, Jaschke W, Waldenberger P, Fraedrich G, Perkmann R (2004) Stent-graft repair for acute traumatic thoracic aortic rupture. Am Surg 70:1039–1044
Kato N, Dake MD, Miller DC, Semba CP, Mitchell RS, Razavi MK, Kee ST (1997) Traumatic thoracic aortic aneurysm: treatment with endovascular stent-grafts. Radiology 205:657–662
Nienaber CA, Fattori R, Lund G, Dieckmann C, Wolf W, von Kodolitsch Y, Nicolas V, Pierangeli A (1999) Nonsurgical reconstruction of thoracic aortic dissection by stent-graft placement. N Engl J Med 340:1539–1545
Hoffer EK, Forauer AR, Silas AM, Gemery JM (2008) Endovascular stent-graft or open surgical repair for blunt thoracic aortic trauma: systematic review. J Vasc Interv Radiol 19:1153–1164
Steinbauer MG, Stehr A, Pfister K, Herold T, Zorger N, Toepel I, Paetzel C, Kasprzak P (2006) Endovascular repair of proximal endograft collapse after treatment for thoracic aortic disease. J Vasc Surg 43(3):609–612
Agnoletti G, Bonnet D, Sidi D (2005) Secondary collapse of a Plamaz stent implanted for native aortic coarctation. Heart 91:506
Borsa JJ, Hoffer EK, Karmy-Jones R, Fontaine AB, Bloch RD, Yoon JK, So CR, Meissner MH, Demirer S (2002) Angiographic description of blunt traumatic injuries to the thoracic aorta with specific relevance to endograft repair. J Endovasc Ther Suppl II:II84–II91
Lin PH, Lumsden AB (2006) Traumatic thoracic aortic injury. Should endovascular repair be considered the standard treatment? Endovasc Today 58–66
Idu MM, Reekers JA, Balm R, Ponsen KJ, de Mol BA, Legemate DA (2005) Collapse of a stent-graft following treatment of a traumatic thoracic aortic rupture. J Endovasc Ther 12:503–507
Hoornweg LL, Dinkelman MK, Goslings JC, Reekers JA, Verhagen HJ, Verhoeven EL, Schurink GWH, Balm R 92006) Endovascular management of traumatic ruptures of the thoracic aorta: a retrospective multicenter analysis of 28 cases in The Netherlands. J Vasc Surg 43:1096–1101
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bandorski, D., Brück, M., Günther, HU. et al. Endograft Collapse After Endovascular Treatment for Thoracic Aortic Disease. Cardiovasc Intervent Radiol 33, 492–497 (2010). https://doi.org/10.1007/s00270-009-9773-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-009-9773-6