Abstract
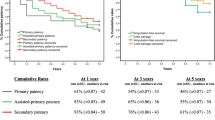
Our objective was to evaluate the possible role of endovascular recanalization of occluded native artery after a failed bypass graft in the case of either acute or chronic limb-threatening ischemia otherwise leading to amputation. In a single-center retrospective clinical analysis, from January 2004 to March 2007 we collected 31 consecutive high-surgical-risk patients (32 limbs) with critical limb ischemia following late (>30 days after surgery) failure of open surgery bypass graft reconstruction. All patients deemed unfit for surgery underwent tentative endovascular recanalization of the native occluded arterial tract. The mean follow-up period was 24 (range, 6–42) months. Technical success was achieved in 30 (93.7%) of 32 limbs. The cumulative primary assisted patency calculated by Kaplan–Meyer analysis was 92% and 88%, respectively, at 12 and 24 months. The limb salvage rate approached 90% at 30 months. In conclusion, our experience shows the feasibility of occluded native artery endovascular recanalization after a failed bypass graft, with optimal results in terms of midterm arterial patency and limb salvage. Our opinion is that successful recanalization of the arterial tract previously considered unsuitable for endovascular approach is allowed by improved competency and experience of vascular specialists, as well as the advances made in catheter and guidewire technology. This group of patients would previously have been relegated to repeat bypass grafts, with their inherently inferior patency and recognized added technical demands. We recognize previous surgical native artery disconnection and lack of pedal runoff to be the main cause of technical failure.



Similar content being viewed by others
References
Brewster DC, LaSalle AJ, Robison JG et al (1984) Femoropopliteal graft failures: clinical consequences and success of secondary reconstructions. Arch Surg 118:1043–1050
Rutherford RB, Jones DN, Bergentz S et al (1984) The efficacy of dextran 40 in preventing early postoperative thrombosis following difficult lower extremity bypass. J Vasc Surg 1:765–771
Donaldson MC, Mannick JA, Whittemore AD (1991) Femoral-distal bypass with in situ greater saphenous vein: long term results using the Mills valvulatome. Ann Surg 213:457–465
Leather KP, Shah DJ, Chang BB et al (1988) Resurrection of the in situ saphenous vein bypass: 1000 cases later. Ann Surg 208:435–442
Taylor LM, Edwards JM, Porter JM (1990) Present status of reversed vein bypass grafting: five year results of a modern series. J Vasc Surg 11:193–206
Donaldson MC, Mannick JA, Whittemore AD (1992) Causes of primary graft failure after in situ saphenous vein bypass grafting. J Vasc Surg 15:113–120
Cohen JR, Mannick JA, Couch NP et al (1986) Recognition and management of impending vein graft failure. Arch Surg 121:758–759
Whittemore AD, Clowes AW, Couch NP et al (1981) Secondary femoropopliteal reconstruction. Ann Surg 193:35–42
Qnifiones-Baldrich WJ, Prego A, Ucelay-Gomez R et al (1991) Failure of PTFE infrainguinal revascularization: patterns, management alternatives and outcome. Ann Vasc Surg 5:163–169
Whittemore AD, Kent CK, Donaldson MC et al (1989) What is the role of polytetrafluoroethylene grafts in infrainguinal reconstruction? J Vasc Surg 10:299–305
Belkin M, Donaldson MC, Whittemore AD et al (1990) Observations on the use of thrombolytic agents for thrombotic occlusions of infrainguinal vein grafts. J Vasc Surg 11:289–296
Graor RA, Risus B, Young JR et al (1988) Thrombolysis of peripheral arterial bypass grafts: surgical thrombectomy compared with thrombolysis. J Vasc Surg 7:347–355
Parent FN, Prowski JJ, Bernhard VM et al (1991) Outcome of intraarterial urokinase for acute vascular occlusion. J Cardiovasc Surg 32:680–690
Edwards JE, Taylor LM, Porter JM (1990) Treatment of failed lower extremity bypass grafts with new autogenous vein bypass grafting. J Vasc Surg 11:136–145
Bartlett ST, Olinde AJ, Flinn WR et al (1987) The reoperative potential of infrainguinal bypass: long-term limb and patient survival. J Vasc Surg 5:170–179
Ascer E, Collier P, Gupta SK, Veith FJ (1987) Reoperation for polytetrafluoroethylene bypass failure: the importance of distal outflow site and operative technique in determining outcome. J Vasc Surg 5:298–310
Yang PM, Wengerter KR, Veith FJ et al (1991) Value and limitations of secondary femoropopliteal bypasses with polytettattuoroethylene. J Vasc Surg 14:292–298
Met R, Van Lienden KP, Koelemay MJ, Bipat S, Legemate DA, Reekers JA (2008) Subintimal angioplasty for peripheral arterial occlusive disease: a systematic review. Cardiovasc Interv Radiol 31(4):687–697
Loftus IM, Hayes PD, Bell PR (2004) Subintimal angioplasty in lower limb ischaemia. Cardiovasc Surg (Torino) 45(3):217–229
Scott EC, Biuckians A, Light RE, Scibelli CD, Milner TP, Meier GH III, Panneton JM (2007) Subintimal angioplasty for the treatment of claudication and critical limb ischemia: 3-year results. J Vasc Surg 46(5):959–964
Gandini R, Pipitone V, Stefanini M, Maresca L, Spinelli A, Colangelo V, Reale CA, Pampana E, Simonetti G (2007) The “Safari” technique to perform difficult subintimal infragenicular vessels. Cardiovasc Interv Radiol 30(3):469–473
Belkin M (1993) Thrombolytic therapy for arterial occlusive disease. Adv Vasc Surg 1:189–211
Harward TRS, Coe D, Flynn TC, Seeger JM (1992) The use of arm vein conduits during infrageniculate arterial bypass. J Vasc Surg 16:420–427
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gandini, R., Chiappa, R., Di Primio, M. et al. Recanalization of the Native Artery in Patients with Bypass Failure. Cardiovasc Intervent Radiol 32, 1146–1153 (2009). https://doi.org/10.1007/s00270-009-9690-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-009-9690-8