Abstract
Purpose
To identify pretreatment predictors of procedural costs in percutaneous and surgical interventions for intermittent claudication due to aortoiliac and/or femoropopliteal disease.
Methods
A retrospective study was conducted in 97 consecutive patients who underwent percutaneous or surgical interventions over 15 months at a tertiary care center. Nineteen clinical predictive variables were collected at baseline. Procedural costs (outcome) were assessed from the perspective of the hospital by direct calculation, not based on ratios of costs-to-charges. A multivariable regression model was built to identify significant cost predictors. Follow-up information was obtained to provide multidimensional assessment of clinical outcome, including technical success (arteriographic score) and clinical result (changes in ankle-brachial pressure index; cumulative patency, mortality, and complication rates).
Results
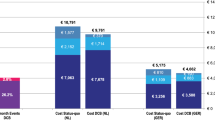
The linear regression model shows that procedural costs per patient are 25% lower in percutaneous patients (versus surgical), 42% lower for patients without rest pain than for those with, 28% lower if treated lesions are unilateral (versus bilateral), 12% lower if the treated lesion is stenotic rather than occlusive, 34% higher in sedentary patients, and 11% higher in patients with a history of cardiac disease. After a mean clinical follow-up >2 years, between-group differences between percutaneous and surgical patients were small and of limited significance in all dimensions of clinical outcome.
Conclusion
Predictors of clinical outcome are different from predictors of costs, and one should include both types of variables in the decision-making process. The choice of percutaneous versus surgical strategy, the presence of rest pain, and the bilaterality of the culprit lesions were the main pretreatment determinants of procedural costs. When possible choices of treatment strategy overlap, percutaneous treatment should provide an acceptable result that is less expensive (although not equal to surgery).


Similar content being viewed by others
References
Hunink MG, Cullen KA, Donaldson MC (1994) Hospital costs of revascularization procedures for femoropopliteal arterial disease. J Vasc Surg 19:632–641
Dormandy JA, Rutherford RB (2000) Management of peripheral arterial disease (PAD). TASC Working Group. TransAtlantic Inter-Society Consensus (TASC). J Vasc Surg 31:S1–S296
Janne d’Othée B, Langdon DR, Bell GK, Bettmann MA (2006) Operating expenses for the diagnosis and treatment of peripheral vascular disease in an academic interventional radiology department: Cost calculations according to a microeconomic method. J Vasc Interv Radiol 17:85–94
Hoch JS, Briggs AH, Willan AR (2002) Something old, something new, something borrowed, something blue: A framework for the marriage of health econometrics and cost-effectiveness analysis. Health Econ 11:415–430
Dacey LJ, Dow RW, McDaniel MD, Walsh DB, Zwolak RM, Cronenwett JL (1988) Cost-effectiveness of intra-arterial thrombolytic therapy. Arch Surg 123:1218–1223
Rutherford RB, Baker JD, Ernst C, et al (1997) Recommended standards for reports dealing with lower extremity ischemia: Revised version. J Vasc Surg 26:517–538
Jansen RM, de Vries SO, Cullen KA, Donaldson MC, Hunink MG (1998) Cost-identification analysis of revascularization procedures on patients with peripheral arterial occlusive disease. J Vasc Surg 28:617–623
Doubilet P, Abrams HL (1984) The cost of underutilization. Percutaneous transluminal angioplasty for peripheral vascular disease. N Engl J Med 310:95–102
Bolia A (1998) Percutaneous intentional extraluminal (subintimal) recanalization of crural arteries. Eur J Radiol 28:199–204
Spinosa DJ, Leung DA, Harthun NL, et al (2003) Simultaneous antegrade and retrograde access for subintimal recanalization of peripheral arterial occlusion. J Vasc Interv Radiol 14:1449–1454
Treiman GS, Whiting JH, Treiman RL, McNamara RM, Ashrafi A (2003) Treatment of limb-threatening ischemia with percutaneous intentional extraluminal recanalization: A preliminary evaluation. J Vasc Surg 38:29–35
Sheiman RG, Janne d’Othée BJ (2007) Screening carotid sonography before elective coronary artery bypass graft surgery: Who needs it? AJR Am J Roentgenol 188:W475–479
Currie IC, Wilson YG, Baird RN, Lamont PM (1995) Treatment of intermittent claudication: The impact on quality of life. Eur J Vasc Endovasc Surg 10:356–361
Khaira HS, Hanger R, Shearman CP (1996) Quality of life in patients with intermittent claudication. Eur J Vasc Endovasc Surg 11:65–69
Whyman MR, Fowkes FG, Kerracher EM, et al (1997) Is intermittent claudication improved by percutaneous transluminal angioplasty? A randomized controlled trial. J Vasc Surg 26:551–557
Zannetti S, L’Italien GJ, Cambria RP (1996) Functional outcome after surgical treatment for intermittent claudication. J Vasc Surg 24:65–73
Weinstein MC, Stason WB (1982) Cost-effectiveness of coronary artery bypass surgery. Circulation 66:III56–66
Albers M, Fratezi AC, De Luccia N (1996) Walking ability and quality of life as outcome measures in a comparison of arterial reconstruction and leg amputation for the treatment of vascular disease. Eur J Vasc Endovasc Surg 11:308–314
Gibbons GW, Burgess AM, Guadagnoli E, et al (1995) Return to well-being and function after infrainguinal revascularization. J Vasc Surg 21:35–44; discussion 44–45
Jenkinson C, Gray A, Doll H, Lawrence K, Keoghane S, Layte R (1997) Evaluation of index and profile measures of health status in a randomized controlled trial. Comparison of the Medical Outcomes Study 36-Item Short Form Health Survey, EuroQol, and disease specific measures. Med Care 35:1109–1118
Pell JP (1995) Impact of intermittent claudication on quality of life. The Scottish Vascular Audit Group. Eur J Vasc Endovasc Surg 9:469–472
Dorman P, Slattery J, Farrell B, Dennis M, Sandercock P (1998) Qualitative comparison of the reliability of health status assessments with the EuroQol and SF-36 questionnaires after stroke. United Kingdom Collaborators in the International Stroke Trial. Stroke 29:63–68
Busschbach JJ, McDonnell J, Tangelder MJ, et al (1999) EuroQol values for economic modeling quality of life after infrainguinal bypass grafting surgery: a rectification. J Vasc Surg 30:1162–1163
Hiatt WR (1997) Quality of life assessment in peripheral arterial disease. Atherosclerosis 131(Suppl):S35–36
Meltzer D, Johannesson M (1999) Inconsistencies in the “societal perspective” on costs of the Panel on Cost-Effectiveness in Health and Medicine. Med Decis Making 19:371–377
Powe NR (1994) Economic and cost-effectiveness investigations of radiologic practices. Radiology 192:11–18
Powe NR (1995) Cost-effectiveness analyses. N Engl J Med 332:123–124; discussion 124–125
Janne d’Othée B, Faintuch S, Reedy AW, Nickerson CF, Rosen MP (2008) Retrievable versus permanent caval filter procedures: When are they cost-effective for Interventional Radiology? J Vasc Interv Radiol: in press
Huber TS, Seeger JM (2001) Dartmouth Atlas of Vascular Health Care review: Impact of hospital volume, surgeon volume, and training on outcome. J Vasc Surg 34:751–756
Dartmouth Medical School CfECS (2000) The Dartmouth Atlas of Vascular Health Care. AHA Press, Health Forum, Chicago
Acknowledgments
The authors thank their patients who filled the quality-of-life questionnaires, and Shirley A. Henry and Charles H. Allen for their help in collecting cost data. The insightful help of Jeffrey Hoch, PhD, was also greatly appreciated during preparation of the manuscript. Bertrand Janne d’Othée was supported by a Research Grant from the French Society of Radiology (Société Française de Radiologie) and by Dartmouth College.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Janne d’Othée, B., Morris, M.F., Powell, R.J. et al. Cost Determinants of Percutaneous and Surgical Interventions for Treatment of Intermittent Claudication from the Perspective of the Hospital. Cardiovasc Intervent Radiol 31, 56–65 (2008). https://doi.org/10.1007/s00270-007-9221-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-007-9221-4