Abstract
Background
No validated perioperative risk assessment models currently exist for use in humanitarian settings. To inform the development of a perioperative mortality risk assessment model applicable to humanitarian settings, we conducted a scoping review of the literature to identify reports that described perioperative risk assessment in surgical care in humanitarian settings and LMICs.
Methods
We conducted a scoping review of the literature to identify records that described perioperative risk assessment in low-resource or humanitarian settings. Searches were conducted in databases including: PubMed, Embase, Cumulative Index to Nursing and Allied Health Literature, Web of Science, World Health Organization Catalog, and Google Scholar.
Results
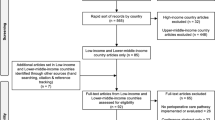
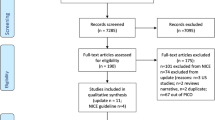
Our search identified 1582 records. After title/abstract and full text screening, 50 reports remained eligible for analysis in quantitative and qualitative synthesis. These reports presented data from over 37 countries from public, NGO, and military facilities. Data reporting was highly inconsistent: fewer than half of reports presented the indication for surgery; less than 25% of reports presented data on injury severity or prehospital data. Most elements of perioperative risk models designed for high-resource settings (e.g., vital signs, laboratory data, and medical comorbidities) were unavailable.
Conclusion
At present, no perioperative mortality risk assessment model exists for use in humanitarian settings. Limitations in consistency and quality of data reporting are a primary barrier, however, can be addressed through data-driven identification of several key variables encompassed by a minimum dataset. The development of such a score is a critical step toward improving the quality of care provided to populations affected by conflict and protracted humanitarian crises.




Similar content being viewed by others
References
Khuri SF, Daley J, Henderson WG (2002) The comparative assessment and improvement of quality of surgical care in the department of veterans affairs. Arch Surg 137:20–27. https://doi.org/10.1001/archsurg.137.1.20
Ng-Kamstra JS, Arya S, Greenberg SLM et al (2018) Perioperative mortality rates in low-income and middle-income countries: a systematic review and meta-analysis. BMJ Glob Health 3:e000810. https://doi.org/10.1136/bmjgh-2018-000810
Copeland GP (2002) The POSSUM system of surgical audit. Arch Surg 137:15–19. https://doi.org/10.1001/archsurg.137.1.15
Hornor MA, Hoeft C, Nathens AB (2018) quality benchmarking in trauma: from the NTDB to TQIP. Curr Trauma Rep 4:160–169. https://doi.org/10.1007/s40719-018-0127-1
Bilimoria KY, Liu Y, Paruch JL et al (2013) Development and evaluation of the universal ACS NSQIP surgical risk calculator: a decision aid and informed consent tool for patients and surgeons. J Am Coll Surg 217:833-842.e3. https://doi.org/10.1016/j.jamcollsurg.2013.07.385
Wild H, Stewart BT, LeBoa C et al (2020) Epidemiology of injuries sustained by civilians and local combatants in contemporary armed conflict: an appeal for a shared trauma registry among humanitarian actors. World J Surg. https://doi.org/10.1007/s00268-020-05428-y
Kluyts H-L, le Manach Y, Munlemvo DM et al (2018) The ASOS surgical risk calculator: development and validation of a tool for identifying African surgical patients at risk of severe postoperative complications. Br J Anaesth 121:1357–1363. https://doi.org/10.1016/j.bja.2018.08.005
Spence RT, Chang DC, Kaafarani HMA et al (2018) Derivation, validation and application of a pragmatic risk prediction index for benchmarking of surgical outcomes. World J Surg 42:533–540. https://doi.org/10.1007/s00268-017-4177-2
Massaut J, Valles P, Ghismonde A et al (2017) The modified south African triage scale system for mortality prediction in resource-constrained emergency surgical centers: a retrospective cohort study. BMC Health Serv Res 17:594. https://doi.org/10.1186/s12913-017-2541-4
Biccard BM, Madiba TE, Kluyts H-L et al (2018) Perioperative patient outcomes in the African surgical outcomes study: a 7-day prospective observational cohort study. Lancet 391:1589–1598. https://doi.org/10.1016/S0140-6736(18)30001-1
Davies JF, Lenglet A, van Wijhe M, Ariti C (2016) Perioperative mortality: analysis of 3 years of operative data across 7 general surgical projects of Médecins Sans Frontières in Democratic Republic of Congo, Central African Republic, and South Sudan. Surgery 159:1269–1278. https://doi.org/10.1016/j.surg.2015.12.022
Ndayizeye L, Ngarambe C, Smart B et al (2016) Peritonitis in Rwanda: epidemiology and risk factors for morbidity and mortality. Surgery 160:1645–1656. https://doi.org/10.1016/j.surg.2016.08.036
Rickard JL, Ntakiyiruta G, Chu KM (2016) Associations with perioperative mortality rate at a major referral hospital in Rwanda. World J Surg 40:784–790. https://doi.org/10.1007/s00268-015-3308-x
FactSheet13en.pdf
World Bank Country and Lending Groups—World Bank Data Help Desk. https://datahelpdesk.worldbank.org/knowledgebase/articles/906519-world-bank-country-and-lending-groups. Accessed 14 Nov 2021
Tricco AC, Lillie E, Zarin W et al (2018) PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med 169:467–473. https://doi.org/10.7326/M18-0850
Peters MDJ, Marnie C, Tricco AC et al (2020) Updated methodological guidance for the conduct of scoping reviews. JBI Evid Synth 18:2119–2126. https://doi.org/10.11124/JBIES-20-00167
Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (eds) (2019) Cochrane handbook for systematic reviews of interventions. John Wiley & Sons
Marks IH, Fong ZV, Stapleton SM et al (2018) How much data are good enough? Using simulation to determine the reliability of estimating POMR for resource-constrained settings. World J Surg 42:2344–2347. https://doi.org/10.1007/s00268-018-4529-6
Burkle FM, Nickerson JW, von Schreeb J et al (2012) Emergency surgery data and documentation reporting forms for sudden-onset humanitarian crises, natural disasters and the existing burden of surgical disease. Prehosp Disaster Med 27:577–582. https://doi.org/10.1017/S1049023X12001306
Anderson GA, Ilcisin L, Abesiga L et al (2017) Surgical volume and postoperative mortality rate at a referral hospital in Western Uganda: measuring the lancet commission on global surgery indicators in low-resource settings. Surgery 161:1710–1719. https://doi.org/10.1016/j.surg.2017.01.009
AlWaqfi N, Khader Y, Ibrahim K (2012) Coronary artery bypass: predictors of 30-day operative mortality in Jordanians. Asian Cardiovasc Thorac Ann 20:245–251. https://doi.org/10.1177/0218492311434647
Ariyaratnam R, Palmqvist CL, Hider P et al (2015) Toward a standard approach to measurement and reporting of perioperative mortality rate as a global indicator for surgery. Surgery 158:17–26. https://doi.org/10.1016/j.surg.2015.03.024
Bunogerane GJ, Rickard J (2019) A cross sectional survey of factors influencing mortality in Rwandan surgical patients in the intensive care unit. Surgery 166:193–197. https://doi.org/10.1016/j.surg.2019.04.010
Harunani S, Imbaya K, Kuremu T (2020) Non-traumatic abdominal surgical emergencies in children. Ann Afr Surg 17:3–6
Khan A, Abdullah A, Ahmad H et al (2017) Impact of international quality improvement collaborative on congenital heart surgery in Pakistan. Heart 103:1680–1686. https://doi.org/10.1136/heartjnl-2016-310533
Maine RG, Kajombo C, Purcell L et al (2019) Effect of in-hospital delays on surgical mortality for emergency general surgery conditions at a tertiary hospital in Malawi. BJS Open 3:367–375. https://doi.org/10.1002/bjs5.50152
Mansourati M, Kumar V, Khajanchi M et al (2018) Mortality following surgery for trauma in an Indian trauma cohort. Br J Surg 105:1274–1282. https://doi.org/10.1002/bjs.10862
Rahman AS, Chao TE, Trelles M et al (2021) The effect of conflict on obstetric and non-obstetric surgical needs and operative mortality in fragile states. World J Surg 45:1400–1408. https://doi.org/10.1007/s00268-021-05972-1
Rahman S, Zheleva B, Cherian KM et al (2019) Linking world bank development indicators and outcomes of congenital heart surgery in low-income and middle-income countries: retrospective analysis of quality improvement data. BMJ Open 9:e028307. https://doi.org/10.1136/bmjopen-2018-028307
Reddy NS, Kappanayil M, Balachandran R et al (2015) Preoperative determinants of outcomes of infant heart surgery in a limited-resource setting. Semin Thorac Cardiovasc Surg 27:331–338. https://doi.org/10.1053/j.semtcvs.2015.09.008
Schidlow DN, Jenkins KJ, Gauvreau K et al (2017) Transposition of the great arteries in the developing world: surgery and outcomes. J Am Coll Cardiol 69:43–51. https://doi.org/10.1016/j.jacc.2016.10.051
Shanthamurthy D, Manesh A, Zacchaeus NG et al (2018) Perioperative outcomes in human immunodeficiency virus-infected patients—the PRO HIV study. Int J STD AIDS 29:968–973. https://doi.org/10.1177/0956462418764485
Sileshi B, Hurt SE, McEvoy MD et al (2016) Pediatric perioperative mortality rates in a sample of Kenyan hospitals: preliminary results in over 3000 cases. Ann Glob Health 82:434–435. https://doi.org/10.1016/j.aogh.2016.04.207
Talabi AO, Etonyeaku AC, Sowande OA et al (2014) Predictors of mortality in children with typhoid ileal perforation in a Nigerian tertiary hospital. Pediatr Surg Int 30:1121–1127. https://doi.org/10.1007/s00383-014-3592-9
Talabi AO, Sowande OA, Adenekan AT et al (2018) A 10 year retrospective review of perioperative mortality in pediatric general surgery at Ile-Ife hospital, Nigeria. J Pediatr Surg 53:2072–2076. https://doi.org/10.1016/j.jpedsurg.2018.03.005
Tarekegn F, Asfaw G, Mossie M (2020) Perioperative mortality at Tibebe Ghion Specialized Teaching Hospital, Ethiopia: a longitudinal study design. Int J Surg Open 26:81–85. https://doi.org/10.1016/j.ijso.2020.08.011
Tarekegn F, Seyoum R, Abebe G, Terefe M (2021) Perioperative pediatric mortality in Ethiopia: a prospective cohort study. Ann Med Surg (Lond) 67:102396. https://doi.org/10.1016/j.amsu.2021.102396
Torborg A, Cronje L, Thomas J et al (2019) South African Paediatric Surgical Outcomes Study: a 14-day prospective, observational cohort study of paediatric surgical patients. Br J Anaesth 122:224–232. https://doi.org/10.1016/j.bja.2018.11.015
Vashistha N, Singhal D, Budhiraja S et al (2018) Outcomes of emergency laparotomy (EL) care protocol at tertiary care center from low-middle-income country (LMIC). World J Surg 42:1278–1284. https://doi.org/10.1007/s00268-017-4333-8
Atashi A, Amini S, Tashnizi MA et al (2018) External validation of european system for cardiac operative risk evaluation II (EuroSCORE II) for risk prioritization in an Iranian population. Braz J Cardiovasc Surg 33:40–46. https://doi.org/10.21470/1678-9741-2017-0030
Berger JH, Jiang Z, O’Reilly EB, Christman MS (2018) First do no harm: predicting surgical morbidity during humanitarian medical missions. World J Surg 42:3856–3860. https://doi.org/10.1007/s00268-018-4720-9
Biccard B, Nepaul S (2010) Risk factors associated with intermediate and long-term mortality following vascular surgery in South African patients. Cardiovasc J Afr 21:263–267. https://doi.org/10.5830/CVJA-2010-016
Chardoli M, Rahimi-Movaghar V (2006) Analysis of trauma outcome at a university hospital in Zahedan, Iran using the TRISS method. East Afr Med J 83:440–442. https://doi.org/10.4314/eamj.v83i8.9458
Hariharan S, Chen D, Ramkissoon A et al (2009) Perioperative outcome of colorectal cancer and validation of CR-POSSUM in a Caribbean country. Int J Surg 7:534–538. https://doi.org/10.1016/j.ijsu.2009.08.009
Isbister WH, Al-Sanea N (2002) POSSUM: a re-evaluation in patients undergoing surgery for rectal cancer. The physiological and operative severity score for enumeration of mortality and morbidity. ANZ J Surg 72:421–425. https://doi.org/10.1046/j.1445-2197.2002.02436.x
Liebenberg JJ, Doubell A, Van Wyk J et al (2020) Predictors of 1 year survival in South African transcatheter aortic valve implant candidates. S Afr Med J 110:491–496. https://doi.org/10.7196/SAMJ.2020.v110i6.14123
Osinaike B, Ayandipo O, Onyeka T et al (2019) Nigerian surgical outcomes—Report of a 7-day prospective cohort study and external validation of the African surgical outcomes study surgical risk calculator. Int J Surg 68:148–156. https://doi.org/10.1016/j.ijsu.2019.06.003
Mohil RS, Bhatnagar D, Bahadur L et al (2004) POSSUM and P-POSSUM for risk-adjusted audit of patients undergoing emergency laparotomy. Br J Surg 91:500–503. https://doi.org/10.1002/bjs.4465
Sadeghi MM, Arasteh M, Gharipour M et al (2011) Evaluation of accuracy of Euroscore risk model in prediction of perioperative mortality after coronary bypass graft surgery in Isfahan. J Res Med Sci 16:787–792
Samuel JC, Varela C, Cairns BA, Charles AG (2014) Application of SIRS criteria to a paediatric surgical population in Malawi. J Trop Pediatr 60:326–328. https://doi.org/10.1093/tropej/fmu021
Sileshi B, McEvoy MD, Wanderer JP et al (2015) Surgical Apgar score and safe surgery checklist use in Kenya: preliminary results of over 3000 cases at a single tertiary care center. Ann Glob Health 81:200–201. https://doi.org/10.1016/j.aogh.2015.02.961
Srinath S (2013) Risk prediction of morbidity and mortality in emergency laparotomy by possum equation. Res J Pharm Biol Chem Sci 4:206
Muhrbeck M, Osman Z, von Schreeb J et al (2021) Predicting surgical resource consumption and in-hospital mortality in resource-scarce conflict settings: a retrospective study. BMC Emerg Med 21:1–11. https://doi.org/10.1186/s12873-021-00488-2
Gutierrez CS, Passos SC, Castro SMJ et al (2021) Few and feasible preoperative variables can identify high-risk surgical patients: derivation and validation of the ex-care risk model. Br J Anaesth 126:525–532. https://doi.org/10.1016/j.bja.2020.09.036
Kluyts H-L, Conradie W, Cloete E et al (2021) Development of a clinical prediction model for in-hospital mortality from the South African Cohort of the African Surgical Outcomes Study. World J Surg 45:404–416. https://doi.org/10.1007/s00268-020-05843-1
Weeks SR, Juillard CJ, Monono ME et al (2014) Is the Kampala trauma score an effective predictor of mortality in low-resource settings? A comparison of multiple trauma severity scores. World J Surg 38:1905–1911. https://doi.org/10.1007/s00268-014-2496-0
Long C, Esquivel MM, Uribe-Leitz T et al (2016) Lessons learned from implementing a hospital-based trauma registry in rural Cameroon. Ann Glob Health 82:535–536. https://doi.org/10.1016/j.aogh.2016.04.447
Sileshi B, Newton MW, Kiptanui J et al (2017) Monitoring anesthesia care delivery and perioperative mortality in Kenya utilizing a provider-driven novel data collection tool. Anesthesiology 127:250–271. https://doi.org/10.1097/ALN.0000000000001713
Croti UA, Murakami AN, De Marchi CH et al (2019) Impact of partnership between children’s HeartLink and IQIC database with a pediatric cardiology and cardiovascular surgery center in Brazil. World J Pediatr Congenit Heart Surg 10:270–275. https://doi.org/10.1177/2150135118825151
Watters DA, Hollands MJ, Gruen RL et al (2015) Perioperative mortality rate (POMR): a global indicator of access to safe surgery and anaesthesia. World J Surg 39:856–864. https://doi.org/10.1007/s00268-014-2638-4
Bruijns SR, Guly HR, Bouamra O et al (2013) The value of traditional vital signs, shock index, and age-based markers in predicting trauma mortality. J Trauma Acute Care Surg 74:1432–1437. https://doi.org/10.1097/TA.0b013e31829246c7
Liu NT, Holcomb JB, Wade CE, Salinas J (2015) Improving the prediction of mortality and the need for life-saving interventions in trauma patients using standard vital signs with heart-rate variability and complexity. Shock 43:549–555. https://doi.org/10.1097/SHK.0000000000000356
Dotan I, Shochat T, Shimon I, Akirov A (2021) The association between BMI and mortality in surgical patients. World J Surg 45:1390–1399. https://doi.org/10.1007/s00268-021-05961-4
Gibbs J, Cull W, Henderson W et al (1999) Preoperative serum albumin level as a predictor of operative mortality and morbidity: results from the national VA surgical risk study. Arch Surg 134:36–42. https://doi.org/10.1001/archsurg.134.1.36
Holcomb JB, Salinas J, McManus JM et al (2005) Manual vital signs reliably predict need for life-saving interventions in trauma patients. J Trauma Acute Care Surg 59:821–829. https://doi.org/10.1097/01.ta.0000188125.44129.7c
Theou O, Andrew M, Ahip SS et al (2019) The pictorial fit-frail scale: developing a visual scale to assess frailty. Can Geriatr J 22:64–74. https://doi.org/10.5770/cgj.22.357
Eastridge BJ, Mabry RL, Seguin P et al (2012) Death on the battlefield (2001–2011): implications for the future of combat casualty care. J Trauma Acute Care Surg 73:S431-437. https://doi.org/10.1097/TA.0b013e3182755dcc
Wild H, Stewart BT, LeBoa C et al (2021) Pediatric casualties in contemporary armed conflict: a systematic review to inform standardized reporting. Injury 52:1748–1756. https://doi.org/10.1016/j.injury.2021.04.055
Nashef SA, Roques F, Michel P et al (1999) European system for cardiac operative risk evaluation (EuroSCORE). Eur J Cardiothorac Surg 16:9–13. https://doi.org/10.1016/s1010-7940(99)00134-7
Copeland GP, Jones D, Walters M (1991) POSSUM: a scoring system for surgical audit. Br J Surg 78:355–360. https://doi.org/10.1002/bjs.1800780327
Brooks MJ, Sutton R, Sarin S (2005) Comparison of surgical risk score, POSSUM and p-POSSUM in higher-risk surgical patients. Br J Surg 92:1288–1292. https://doi.org/10.1002/bjs.5058
Schluter PJ, Nathens A, Neal ML et al (2010) Trauma and injury severity score (TRISS) coefficients 2009 revision. J Trauma Acute Care Surg 68:761–770. https://doi.org/10.1097/TA.0b013e3181d3223b
Hannan EL, Mendeloff J, Farrell LS et al (1995) Validation of TRISS and ASCOT using a non-MTOS trauma registry. J Trauma 38:83–88. https://doi.org/10.1097/00005373-199501000-00022
van Gennip L, Haverkamp FJC, Muhrbeck M et al (2020) Using the Red Cross wound classification to predict treatment needs in children with conflict-related limb injuries: a retrospective database study. World J Emerg Surg 15:52. https://doi.org/10.1186/s13017-020-00333-0
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wild, H., Stewart, B.T., LeBoa, C. et al. Perioperative Risk Assessment in Humanitarian Settings: A Scoping Review. World J Surg 47, 1092–1113 (2023). https://doi.org/10.1007/s00268-023-06893-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-023-06893-x