Abstract
Background
Advances in surgical techniques have significantly improved the safety of thyroidectomy. Quality of life issues, such as voice changes, however continue to be important considerations. This study evaluated the prevalence and determinants of voice changes following thyroidectomies for non-malignant goiters in a Nigerian Hospital.
Methodology
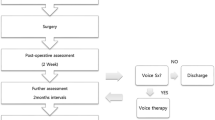
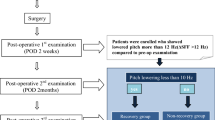
Consecutive adults who had thyroidectomy for non-malignant goiters were evaluated. Preoperatively, each participant had laryngoscopy and voice assessment using the Voice Handicap Index-10. At surgery, the intubation difficulty score, size of endotracheal tubes, and duration of operation were recorded. Laryngoscopy and VHI-10 assessments were repeated 1 week, 1 month, and 3 months after surgery. Pre and postoperative assessments were compared.
Result
Fifty-four patients completed the study. Subtotal thyroidectomy was the commonest operation performed in 17 patients (31.48%), with 14 (25.93%) having total thyroidectomy. Baseline median VHI-10 score was 6.5(IQR-10). Five patients had abnormal preoperative laryngoscopy findings (benign vocal cord lesions). Postoperatively, seven patients had endoscopic evidence of vocal cord paralysis, six were unilateral while one was bilateral. Ten patients (18.5%) had early voice changes. Median VHI-10 score at one week was significantly higher than baseline (10 vs. 6.5, p = 0.01). At 3 months, VHI-10 reverted back to baseline in five of the ten patients while five patients (9.3%) had persistent voice changes. Abnormal endoscopic findings predicted the occurrence of early postoperative voice changes.
Conclusion
Thyroidectomy for non-malignant goiters is associated with transient voice changes, many of which revert to normal over time. Abnormal endoscopic findings predict its occurrence.

Similar content being viewed by others
References
Cheng H, Soleas I, Ferko NC, Clymer JW, Amaral JF (2015) A systematic review and meta-analysis of harmonic focus in thyroidectomy compared to conventional techniques. Thyroid Res 8:15
Arowolo OA, Olasehinde O, Adisa AO, Adeyemo A, Alatise OI, Wuraola F (2019) Early experience with ligasure thyroidectomy in a Nigeria teaching hospital. Niger J Surg Off Publ Niger Surg Res Soc 25:64
Ruben RJ (2000) Redefining the survival of the fittest: communication disorders in the 21st century. Laryngoscope 110:241
Mencke T, Echternach M, Kleinschmidt S, Lux P, Barth V, Plinkert PK et al (2003) Laryngeal morbidity and quality of tracheal intubation a randomized controlled trial. J Am Soc Anesthesiol 98:1049–1056
de Pedro NI, Fae A, Vartanian JG, Barros APB, Correia LM, Toledo RN et al (2006) Voice and vocal self-assessment after thyroidectomy. Head Neck 28:1106–1114
Lee CY, Long KL, Eldridge RJ, Davenport DL, Sloan DA (2014) Preoperative laryngoscopy in thyroid surgery: Do patients’ subjective voice complaints matter? Surgery 156:1477–1483
Schlosser K, Zeuner M, Wagner M, Slater EP, Fernández ED, Rothmund M et al (2007) Laryngoscopy in thyroid surgery––essential standard or unnecessary routine? Surgery 142:858–864
BAETS (2007) British association of endocrine surgeons second national audit report. Dendrite Clinical Systems, Oxford
Chuhwak E, Ohwovoriole AE (2005) Clinical features of goitres on the Nigerian Plateau. Niger Postgrad Med J 12(4):2
Misono S, Yueh B, Stockness AN, House ME, Marmor S (2017) Minimal important difference in voice handicap index-10. JAMA Otolaryngol Head Neck Surg 143(11):1098–1103
Tedla M, Chakrabarti S, Suchankova M et al (2016) Voice outcomes after thyroidectomy without superior and recurrent laryngeal nerve injury: VoiSS questionnaire and GRBAS tool assessment. Eur Arch Otorhinolaryngol 273:4543–4547. https://doi.org/10.1007/s00405-016-4163-6
Shin Y, Hong K, Hong Y, Oh J, Yoon Y, Lee H (2014) Aerodynamic analysis of voice in patients with thyroidectomy. J Korean Thyroid Assoc 7(1):77–82
Kovatch KJ, Reyes-Gastelum D, Hughes DT, Hamilton AS, Ward KC, Haymart MR (2019) Assessment of voice outcomes following surgery for thyroid cancer. JAMA Otolaryngol Head Neck Surg 145:823–829
Borel F, Christou N, Marret O, Mathonnet M, Caillard C, Bannani S et al (2018) Long-term voice quality outcomes after total thyroidectomy: a prospective multicenter study. Surgery 163:796–800
Chun BJ, Bae JS, Chae BJ, Hwang YS, Shim MR, Sun DI (2012) Early postoperative vocal function evaluation after thyroidectomy using thyroidectomy related voice questionnaire. World J Surg 36(10):2503–2508. https://doi.org/10.1007/s00268-012-1667-0
Liang TJ, Wang NY, Liu SI et al (2021) Vocal cord granuloma after transoral thyroidectomy using oral endotracheal intubation: two case reports. BMC Anesthesiol 21:170. https://doi.org/10.1186/s12871-021-01393-8
Echternach M, Maurer C, Mencke T, Schilling M, Verse T, Richter B (2009) Laryngeal complications after thyroidectomy: Is it always the surgeon? Arch Surg 144(2):149–153
Hermann M, Keminger K, Kober F (1991) Risk factors of recurrent nerve palsy: a statistical analysis of 7566 thyroid operations. Chirurgie 62:182–188
Rathi PK, Shaikh AR, Shaikh GA (2010) Identification of recurrent laryngeal nerve during thyroidectomy decreases the risk of nerve injury. Pak J Med Sci 26(1):148–151
Steurer M, Passler C, Denk DM, Schneider B, Niederle B, Bigenzahn W (2002) Advantages of recurrent laryngeal nerve identification in thyroidectomy and parathyroidectomy and the importance of preoperative and postoperative laryngoscopic examination in more than 1000 nerves at risk. Laryngoscope 112(1):124–133
Kim SY, Kim GJ, Lee DH, Bae JS, Lee SH, Kim JS, Hwang YS, Shim MR, Park YH, Sun DI (2020) Voice change after thyroidectomy without vocal cord paralysis: analysis of 2,297 thyroidectomy patients. Surgery 168(6):1086–1094
Moran K, Grigorian A, Elfenbein D, Schubl S, Jutric Z, Lekawa M et al (2020) Energy vessel sealant devices are associated with decreased risk of neck hematoma after thyroid surgery. Updat Surg 72:1135–1141
Cheng H, Soleas I, Ferko NC, Clymer JW, Amaral JF (2015) A systematic review and meta-analysis of harmonic focus in thyroidectomy compared to conventional techniques. Thyroid Res 8:1–13
Sinagra DL, Montesinos MR, Tacchi VA, Moreno JC, Falco JE, Mezzadri NA, Debonis DL, Curutchet HP (2004) Voice changes after thyroidectomy without recurrent laryngeal nerve injury. J Am Coll Surg 199(4):556–560. https://doi.org/10.1016/j.jamcollsurg.2004.06.020
Akyildiz S, Ogut F, Akyildiz M, Engin EZ (2008) A multivariate analysis of objective voice changes after thyroidectomy without laryngeal nerve injury. Arch Otolaryngol Head Neck Surg 134(6):596–602. https://doi.org/10.1001/archotol.134.6.596
Afolabi AO, Ayandipo OO, Afuwape OO, Ogundoyin OA (2016) A fifteen year experience of total thyroidectomy for the management of simple multinodular goitres in a low medium income country. S Afr J Surg 54(4):40–45
Samuel SA, Rebecca SH (2019) Complications of thyroidectomy at a tertiary health institution in Nigeria. Sub Sahar Afr J Med 6(1):1
Jeannon JP, Orabi AA, Bruch GA, Abdalsalam HA, Simo R (2009) Diagnosis of recurrent laryngeal nerve palsy after thyroidectomy: a systematic review. Int J Clin Pract 63(4):624–629
Gardiner KR, Russell CF (1995) Thyroidectomy for large multinodular colloid goitre. J R Coll Surg Edinb 40(6):367–370
Tsuzuki N, Wasano K, Kawasaki T, Sasaki SI, Ogawa K (2019) Thyroid lobe size predicts risk of postoperative temporary recurrent laryngeal nerve paralysis. Laryngosc Investig Otolaryngol 4(6):708–713
Godballe C, Madsen AR, Sørensen CH, Schytte S, Trolle W, Helweg-Larsen J, Barfoed L, Kristiansen L, Sørensen VZ, Samuelsen G, Pedersen HB (2014) Risk factors for recurrent nerve palsy after thyroid surgery: a national study of patients treated at Danish departments of ENT head and neck surgery. Eur Arch Otorhinolaryngol 271(8):2267–2276
Zakaria HM, Al Awad NA, Al Kreedes AS, Al-Mulhim AM, Al-Sharway MA, Hadi MA, Al Sayyah AA (2011) Recurrent laryngeal nerve injury in thyroid surgery. Oman Med J 26(1):34
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author’s declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Adeyemo, A., Olasehinde, O., Owojuyigbe, A.M. et al. Prevalence and Predictors of Post-Thyroidectomy Voice Dysfunction in a Nigerian Cohort. World J Surg 47, 682–689 (2023). https://doi.org/10.1007/s00268-022-06858-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-022-06858-6