Abstract
Background
Esophageal cancer has a poor prognosis because of its rapid progression and early and extensive lymph node metastasis. Simple, objective indicators for predicting long-term outcomes are needed to select optimal perioperative treatment and appropriate follow-up for patients with esophageal cancer. The aim of this study is to investigate the relationship between the lymphocyte-to-C-reactive protein ratio (LCR) and the survival of patients with esophageal cancer, by performing time-dependent receiver operating characteristic (ROC) curve analysis. The results were compared to those of traditional inflammation-based markers.
Methods
This study enrolled 495 patients who underwent thoracic esophagectomy for esophageal cancer as the primary treatment between 2000 and 2019 in our department. We investigated the predictability of the LCR for oncological outcomes compared to that of other traditional inflammatory markers.
Results
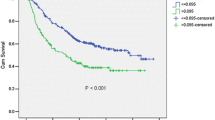
The 3-year overall survival (OS) and recurrence-free survival (RFS) were 72.6% and 57.5%, respectively. Low LCR was significantly associated with higher cancer stage, included depth of invasion (p < 0.001), lymph node metastasis (p < 0.001) and cStage (p < 0.001). The LCR had the highest AUC value (0.675) for predicting OS compared to the other examined inflammatory markers. In multivariate analysis, the LCR (optimal cutoff threshold = 19,000) was identified as a significant predictor of death (hazard ratio, 2.24; 95% confidence interval [CI], 1.61–3.12; p < 0.001) and recurrence (hazard ratio, 1.97; 95%CI, 1.48–2.63; p < 0.001).
Conclusion
The LCR is novel indicator for oncological outcomes for patients with esophageal cancer and may assist to facilitate personalized multidisciplinary treatments.



Similar content being viewed by others
References
Akutsu Y, Kato K, Igaki H et al (2016) The prevalence of overall and initial lymph node metastases in clinical T1N0 thoracic esophageal cancer: From the results of JCOG0502, a prospective multicenter study. Ann Surg 264:1009–1015
Aoyama J, Kawakubo H, Mayanagi S et al (2019) Discrepancy between the clinical and final pathological findings of lymph node metastasis in superficial esophageal cancer. Ann Surg Oncol 26:2874–2881
DeNardo DG, Johansson M, Coussens LM (2008) Immune cells as mediators of solid tumor metastasis. Cancer Metastasis Rev 27:11–18
Matsuda S, Takeuchi H, Kawakubo H et al (2015) Cumulative prognostic scores based on plasma fibrinogen and serum albumin levels in esophageal cancer patients treated with transthoracic esophagectomy: Comparison with the Glasgow prognostic score. Ann Surg Oncol 22:302–310
Matsuda S, Takeuchi H, Kawakubo H et al (2021) Validation study of fibrinogen and albumin score in esophageal cancer patients who underwent esophagectomy: Multicenter prospective cohort study. Ann Surg Oncol 28:774–784
Takeuchi M, Takeuchi H, Kawakubo H et al (2018) Perioperative risk calculator predicts long-term oncologic outcome for patients with esophageal carcinoma. Ann Surg Oncol 25:837–843
Sato H, Tsubosa Y, Kawano T (2012) Correlation between the pretherapeutic neutrophil to lymphocyte ratio and the pathologic response to neoadjuvant chemotherapy in patients with advanced esophageal cancer. World J Surg 36:617–622
Walsh SR, Cook EJ, Goulder F et al (2005) Neutrophil-lymphocyte ratio as a prognostic factor in colorectal cancer. J Surg Oncol 91:181–184
Hirahara N, Matsubara T, Mizota Y et al (2016) Prognostic value of preoperative inflammatory response biomarkers in patients with esophageal cancer who undergo a curative thoracoscopic esophagectomy. BMC Surg 16:1–12
Chan JCY, Chan DL, Diakos CI et al (2017) The lymphocyte-to-monocyte ratio is a superior predictor of overall survival in comparison to established biomarkers of resectable colorectal cancer. Ann Surg 265:539–546
Feng JF, Huang Y, Chen QX (2014) Preoperative platelet lymphocyte ratio (PLR) is superior to neutrophil lymphocyte ratio (NLR) as a predictive factor in patients with esophageal squamous cell carcinoma. World J Surg Oncol 12:1–6
Yuk HD, Hwang EC, Park JY et al (2020) The number of metabolic features as a significant prognostic factor in patients with metastatic renal cell carcinoma. Sci Rep 10:475–481
Wei XL, Wang FH, Zhang DS et al (2015) A novel inflammation-based prognostic score in esophageal squamous cell carcinoma: The C-reactive protein/albumin ratio. BMC Cancer 15:1–11
Liu Z, Jin K, Guo M et al (2017) Prognostic value of the CRP/Alb ratio, a novel inflammation-based score in pancreatic cancer. Ann Surg Oncol 24:561–568
Okugawa Y, Toiyama Y, Yamamoto A et al (2020) Lymphocyte-C-reactive protein ratio as promising new marker for predicting surgical and oncological outcomes in colorectal cancer. Ann Surg 272:342–351
Rice TW, Patil DT, Blackstone EH (2017) 8th edition AJCC/UICC staging of cancers of the esophagus and esophagogastric junction: Application to clinical practice. Ann Cardiothorac Surg 6:119–130
Kaburagi T, Takeuchi H, Kawakubo H et al (2014) Clinical utility of a novel hybrid position combining the left lateral decubitus and prone positions during thoracoscopic esophagectomy. World J Surg 38:410–418
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: A new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Takeuchi M, Kawakubo H, Mayanagi S et al (2019) Perioperative risk calculator for distal gastrectomy predicts overall survival in patients with gastric cancer. Gastric Cancer 22:624–631
Suzuki S, Akiyoshi T, Oba K et al (2020) Comprehensive comparative analysis of prognostic value of systemic inflammatory biomarkers for patients with stage II/III colon cancer. Ann Surg Oncol 27:844–852
Okugawa Y, Toiyama Y, Yamamoto A et al (2020) Lymphocyte-to-C-reactive protein ratio and score are clinically feasible nutrition-inflammation markers of outcome in patients with gastric cancer. Clin Nutr 39:1209–1217
Cheng C, Zhang Q, Zhuang LP, Sun J (2020) Prognostic value of lymphocyte-to-C-reactive protein ratio in patients with gastric cancer after surgery: A multicentre study. Jpn J Clin Oncol 50:1141–1149
Yamamoto A, Toiyama Y, Okugawa Y et al (2021) Clinical implications of the preoperative lymphocyte C-reactive protein ratio in esophageal cancer patients. Surg Today 51:745–755. https://doi.org/10.1007/s00595-020-02166-5
Okamura A, Takeuchi H, Matsuda S et al (2015) Factors affecting cytokine change after esophagectomy for esophageal cancer. Ann Surg Oncol 22:3130–3135
Ogura M, Takeuchi H, Kawakubo H et al (2013) Clinical significance of CXCL-8/CXCR-2 network in esophageal squamous cell carcinoma. Surgery 154:512–520
Lin EY, Pollard JW (2004) Role of infiltrated leucocytes in tumour growth and spread. Br J Cancer 90:2053–2058
Grivennikov SI, Greten FR, Karin M (2010) Immunity, inflammation and cancer. Cell 140:883–899
Huber C, Bobek N, Kuball J et al (2005) Inhibitors of apoptosis confer resistance to tumour suppression by adoptively transplanted cytotoxic T-lymphocytes in vitro and in vivo. Cell Death Differ 12:317–325
Forrest LM, McMillan DC, McArdle CS et al (2003) Evaluation of cumulative prognostic scores based on the systemic inflammatory response in patients with inoperable nonsmall- cell lung cancer. Br J Cancer 89:1028–1030
McMillan DC (2013) The systemic inflammation-based Glasgow Prognostic Score: A decade of experience in patients with cancer. Cancer Treat Rev 39:534–540
Fearon K, Strasser F, Anker SD et al (2011) Definition and classification of cancer cachexia: An international consensus. Lancet Oncol 12:489–495
Kitagawa Y, Uno T, Oyama T et al (2019) Esophageal cancer practice guidelines 2017 edited by the Japan Esophageal Society: part 1. Esophagus 16:1–24
Kato H, Fukuchi M, Miyazaki T et al (2005) Classification of recurrent esophageal cancer after radical esophagectomy with two- or three-field lymphadenectomy. Anticancer Res 25:3461–3467
Wu Y, Li C, Zhao J et al (2016) Neutrophil-to-lymphocyte and platelet-to-lymphocyte ratios predict chemotherapy outcomes and prognosis in patients with colorectal cancer and synchronous liver metastasis. World J Surg Oncol 14:1–8
Acknowledgements
We wish to thank Kumiko Motooka, a staff member at the Department of Surgery in Keio University School of Medicine, for her help with the preparation of this manuscript.
Funding
No funding was obtained for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Y.K. received lecture fees from Chugai Pharmaceutical Co., Ltd., Taiho Pharmaceutical Co., Ltd, Asahi Kasei Pharma Corporation, Otsuka Pharmaceutical Factory Inc., Shionogi & Co., Ltd., Nippon Covidien Inc., Ono Pharmaceutical Co., Ltd. and Bristol-Myers Squibb K.K. Y.K. was supported by grants from Chugai Pharmaceutical Co., Ltd., Taiho Pharmaceutical Co., Ltd, Yakult Honsha Co. Ltd., Asahi KASEI Co., Ltd., Otsuka Pharmaceutical Co., Ltd., Takeda Pharmaceutical Co., Ltd., Ono Pharmaceutical Co., Ltd., Tsumura & CO., Kyouwa Hakkou Kirin Co., Ltd., Dainippon Sumitomo Pharma Co., Ltd., EA Pharma Co., Ltd., Astellas Pharma Inc., Toyama Chemical Co., Ltd., Medicon Inc., Kaken Pharmaceutical Co. Ltd., Eisai Co., Ltd., Otsuka Pharmaceutical Factory Inc., Teijin Pharma Limited., Nihon Pharmaceutical Co., Ltd. and Nippon Covidien Inc. Y.K. also holds an endowed chair provided by Chugai Pharmaceutical Co., Ltd. and Taiho Pharmaceutical Co., Ltd., outside the submitted work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Takeuchi, M., Kawakubo, H., Hoshino, S. et al. Lymphocyte-to-C-Reactive Protein Ratio as a Novel Marker for Predicting Oncological Outcomes in Patients with Esophageal Cancer. World J Surg 45, 3370–3377 (2021). https://doi.org/10.1007/s00268-021-06269-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-021-06269-z