Abstract
Background
Adhesion barriers are increasingly used in hepatobiliary surgery. However, there has been no solid evidence yet in support of their safety.
Methods
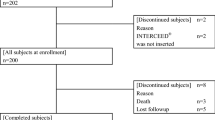
Incidences of global postoperative morbidities and major abdominal morbidities were compared between 101 consecutive patients who received a sheet-type adhesion barrier (Interceed®) and 134 patients who did not receive any adhesion barriers during hepatectomy. Propensity score (PS) adjustment was used to account for potential bias to receive Interceed.
Results
In the PS-adjusted population, the incidences of both global postoperative morbidities and major abdominal morbidities showed no significant difference between the Interceed group and the control group (17.9% vs. 17.6%; P = 0.948 and 7.8% vs. 9.1%; P = 0.813, respectively). Multivariate analysis showed that age + 10 years (odds ratio [OR], 1.70; 95% CI, 1.15–2.50; P = 0.007), estimated blood loss + 100 mL (OR, 1.05; 95% CI, 1.01–1.09, P = 0.009), and laparoscopic approach (OR, 0.10; 95% CI, 0.01–0.75; P = 0.026) were independent predictors for global postoperative morbidities and operation time + 1 h (OR, 1.56; 95% CI, 1.23–1.96; P < 0.001) was a risk factor for major abdominal morbidity, while no specific association between the use of Interceed and the risk of postoperative morbidity was observed.
Conclusions
Use of Interceed does not increase the risk of postoperative morbidities after hepatectomy.

Similar content being viewed by others
References
Oba M, Hasegawa K, Matsuyama Y, Shindoh J, Mise Y, Aoki T et al (2014) Discrepancy between recurrence-free survival and overall survival in patients with resectable colorectal liver metastases: a potential surrogate endpoint for time to surgical failure. Ann Surg Oncol 21(6):1817–1824
Oba M, Hasegawa K, Shindoh J, Yamashita S, Sakamoto Y, Makuuchi M et al (2016) Survival benefit of repeat resection of successive recurrences after the initial hepatic resection for colorectal liver metastases. Surgery 159(2):632–640
Shindoh J, Kawamura Y, Kobayashi Y, Akuta N, Kobayashi M, Suzuki Y et al (2020) Time-to-interventional failure as a new surrogate measure for survival outcomes after resection of hepatocellular carcinoma. J Gastrointest Surg 24:50–57
Kobayashi Y, Shindoh J, Igata Y, Okubo S, Hashimoto M (2020) A novel scoring system for evaluating the difficulty of lysis of adhesion and surgical risk at repeat hepatectomy. J Hepatobiliary Pancreat Sci 27:191–199
Naito M, Ogura N, Yamanashi T, Sato T, Nakamura T, Miura H et al (2017) Prospective randomized controlled study on the validity and safety of an absorbable adhesion barrier (Interceed®) made of oxidized regenerated cellulose for laparoscopic colorectal surgery. Asian J Endosc Surg 10(1):7–11
Watanabe J, Ishida F, Ishida H, Fukunaga Y, Watanabe K, Naito M et al (2019) A prospective multi-center registry concerning the clinical performance of laparoscopic colorectal surgery using an absorbable adhesion barrier (INTERCEED®) made of oxidized regenerated cellulose. Surg Today 49(10):877–884
Braunwarth E, Primavesi F, Gobel G, Cardini B, Oberhuber R, Margreiter C et al (2019) Is bile leakage after hepatic resection associated with impaired long-term survival? Eur J Surg Oncol J Eur Soc Surg Oncol Br Assoc Surg Oncol 45(6):1077–1083
Itoh S, Uchiyama H, Ikeda Y, Morita K, Harada N, Sugimachi K et al (2017) Post-hepatectomy refractory ascites in cirrhotic patients with hepatocellular carcinoma: risk factor analysis to overcome this problematic complication. Anticancer Res 37(3):1381–1385
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD et al (2009) The Clavien–Dindo classification of surgical complications: five-year experience. Ann Surg 250(2):187–196
Koch M, Garden OJ, Padbury R, Rahbari NN, Adam R, Capussotti L et al (2011) Bile leakage after hepatobiliary and pancreatic surgery: a definition and grading of severity by the International Study Group of Liver Surgery. Surgery 149(5):680–688
Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR (1999) Guideline for prevention of surgical site infection, 1999. Centers for Disease Control and Prevention (CDC) hospital infection control practices advisory committee. Am J Infect Control 27(2):97–132 (quiz 3–4; discussion 96)
Azziz R (1993) Microsurgery alone or with INTERCEED absorbable adhesion barrier for pelvic sidewall adhesion re-formation. The INTERCEED (TC7) Adhesion Barrier Study Group II. Surg Gynecol Obstet 177(2):135–139
Franklin RR (1995) Reduction of ovarian adhesions by the use of Interceed. Ovarian Adhesion Study Group. Obstet Gynecol 86(3):335–340
Keckstein J, Ulrich U, Sasse V, Roth A, Tuttlies F, Karageorgieva E (1996) Reduction of postoperative adhesion formation after laparoscopic ovarian cystectomy. Hum Reprod 11(3):579–582
Larsson B (1996) Efficacy of Interceed in adhesion prevention in gynecologic surgery: a review of 13 clinical studies. J Reprod Med 41(1):27–34
Li TC, Cooke ID (1994) The value of an absorbable adhesion barrier, Interceed, in the prevention of adhesion reformation following microsurgical adhesiolysis. Br J Obstet Gynaecol 101(4):335–339
Mais V, Ajossa S, Piras B, Guerriero S, Marongiu D, Melis GB (1995) Prevention of de-novo adhesion formation after laparoscopic myomectomy: a randomized trial to evaluate the effectiveness of an oxidized regenerated cellulose absorbable barrier. Hum Reprod 10(12):3133–3135
Saravelos H, Li TC (1996) Post-operative adhesions after laparoscopic electrosurgical treatment for polycystic ovarian syndrome with the application of Interceed to one ovary: a prospective randomized controlled study. Hum Reprod 11(5):992–997
Sekiba K (1992) Use of Interceed(TC7) absorbable adhesion barrier to reduce postoperative adhesion reformation in infertility and endometriosis surgery. The Obstetrics and Gynecology Adhesion Prevention Committee. Obstet Gynecol 79(4):518–522
Tinelli A, Malvasi A, Guido M, Tsin DA, Hudelist G, Hurst B et al (2011) Adhesion formation after intracapsular myomectomy with or without adhesion barrier. Fertil Steril 95(5):1780–1785
Wallwiener D, Meyer A, Bastert G (1998) Adhesion formation of the parietal and visceral peritoneum: an explanation for the controversy on the use of autologous and alloplastic barriers? Fertil Steril 69(1):132–137
Mise Y, Hasegawa K, Shindoh J, Ishizawa T, Aoki T, Sakamoto Y et al (2015) The feasibility of third or more repeat hepatectomy for recurrent hepatocellular carcinoma. Ann Surg 262(2):347–357
Capussotti L, Ferrero A, Vigano L, Sgotto E, Muratore A, Polastri R (2006) Bile leakage and liver resection: where is the risk? Arch Surg 141(7):690–694 discussion 5
Nagano Y, Togo S, Tanaka K, Masui H, Endo I, Sekido H et al (2003) Risk factors and management of bile leakage after hepatic resection. World J Surg 27(6):695–698. https://doi.org/10.1007/s00268-003-6907-x
Sadamori H, Yagi T, Shinoura S, Umeda Y, Yoshida R, Satoh D et al (2013) Risk factors for major morbidity after liver resection for hepatocellular carcinoma. Br J Surg 100(1):122–129
Yamashita Y, Hamatsu T, Rikimaru T, Tanaka S, Shirabe K, Shimada M et al (2001) Bile leakage after hepatic resection. Ann Surg 233(1):45–50
Adams RB, Aloia TA, Loyer E, Pawlik TM, Taouli B, Vauthey JN et al (2013) Selection for hepatic resection of colorectal liver metastases: expert consensus statement. HPB (Oxford) 15(2):91–103
Funding
This study was supported by study grant from Okinaka Menorial Institute for Medical Disease.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors have no conflict of interest to disclose.
Ethical approval
This study was performed in accordance with the ethical guidelines for clinical study in Japan under approval of the institutional review board of Toranomon Hospital (No. 1919).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Okubo, S., Shindoh, J., Kobayashi, Y. et al. Safety of Use of a Sheet-Type Adhesion Barrier (Interceed®) During Liver Surgery. World J Surg 44, 4214–4220 (2020). https://doi.org/10.1007/s00268-020-05743-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-020-05743-4