Abstract
Background
Some of patients are suffered from pitch lowering of voice after thyroidectomy. We sought to identify factors predictive of a recovery from lowered pitch voice after thyroid surgery.
Methods
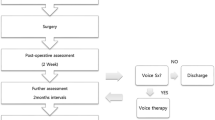
We retrospectively reviewed the records of 133 patients who underwent total thyroidectomy to treat papillary carcinoma between January 2012 and February 2013. Of these, we enrolled 78 who exhibited a lower-pitched voice (SFF fall > 12 Hz) at 2 weeks post-operatively than pre-operatively and investigated pitch recovery after 3 months. We subclassified patients into recovery and non-recovery groups and compared videostroboscopic findings, acoustic voice data, and thyroidectomy-related voice questionnaire scores pre-operatively and 2, 8, and 12 weeks post-operatively.
Results
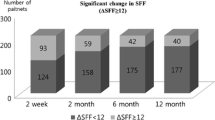
Vocal cord asymmetry on videostroboscopic examination at 2 weeks post-operatively (odds ratio 19.056, p = 0.001*) was more frequent in the non-recovery group. In acoustic analysis, mean pre-operative SFF was higher in the non-recovery group than the recovery group (190.9 ± 27.5 and 180.9 ± 24.6 Hz, respectively; p = 0.030*). Also, a reduction in the SFF of > 19.6 Hz, at 2 weeks post-operatively versus pre-operatively, predicted non-recovery of pitch-lowering in patients with reduced SFF within post-operative 3 months, with 72.0% sensitivity and 71.2% specificity. After 6 months of follow-up, no patient who exhibited an SFF fall > 19.6 Hz recovered to within 10 Hz of the pre-operative value.
Conclusion
A reduction in the speaking fundamental frequency (SFF) > 19.6 Hz at 2 weeks post-operatively predicted persisting lowering of voice pitch after thyroidectomy among those with lower-pitched voices after surgery. Pre-operative high SFF and post-operative stroboscopic findings including vocal cord asymmetry at 2 weeks post-operatively also predicted persisting lowering of voice pitch for 3 months.




Similar content being viewed by others
References
Chandrasekhar SS, Randolph GW, Seidman MD et al (2013) Clinical practice guideline: improving voice outcomes after thyroid surgery. Otolaryngol Head Neck Surg 148:S1–37
Steurer M, Passler C, Denk DM et al (2002) Advantages of recurrent laryngeal nerve identification in thyroidectomy and parathyroidectomy and the importance of preoperative and postoperative laryngoscopic examination in more than 1000 nerves at risk. Laryngoscope 112:124–133
Kuhn MA, Bloom G, Myssiorek D (2013) Patient perspectives on dysphonia after thyroidectomy for thyroid cancer. J Voice 27:111–114
Akyildiz S, Ogut F, Akyildiz M et al (2008) A multivariate analysis of objective voice changes after thyroidectomy without laryngeal nerve injury. Arch Otolaryngol Head Neck Surg 134:596–602
de Pedro NI, Fae A, Vartanian JG et al (2006) Voice and vocal self-assessment after thyroidectomy. Head Neck 28:1106–1114
Debruyne F, Ostyn F, Delaere P et al (1997) Acoustic analysis of the speaking voice after thyroidectomy. J Voice 11:479–482
Hong KH, Kim YK (1997) Phonatory characteristics of patients undergoing thyroidectomy without laryngeal nerve injury. Otolaryngol Head Neck Surg 117:399–404
Musholt TJ, Musholt PB, Garm J et al (2006) Changes of the speaking and singing voice after thyroid or parathyroid surgery. Surgery 140:978–988 discussion 988-979
Soylu L, Ozbas S, Uslu HY et al (2007) The evaluation of the causes of subjective voice disturbances after thyroid surgery. Am J Surg 194:317–322
Stojadinovic A, Shaha AR, Orlikoff RF et al (2002) Prospective functional voice assessment in patients undergoing thyroid surgery. Ann Surg 236:823–832
Sinagra DL, Montesinos MR, Tacchi VA et al (2004) Voice changes after thyroidectomy without recurrent laryngeal nerve injury. J Am Coll Surg 199:556–560
Chun BJ, Bae JS, Chae BJ et al (2012) Early postoperative vocal function evaluation after thyroidectomy using thyroidectomy related voice questionnaire. World J Surg 36:2503–2508. https://doi.org/10.1007/s00268-012-1667-0
Nam IC, Bae JS, Chae BJ et al (2013) Therapeutic approach to patients with a lower-pitched voice after thyroidectomy. World J Surg 37:1940–1950. https://doi.org/10.1007/s00268-013-2167-6
Nam IC, Bae JS, Shim MR et al (2012) The importance of preoperative laryngeal examination before thyroidectomy and the usefulness of a voice questionnaire in screening. World J Surg 36:303–309. https://doi.org/10.1007/s00268-011-1347-5
McIvor NP, Flint DJ, Gillibrand J et al (2000) Thyroid surgery and voice-related outcomes. Aust N Z J Surg 70:179–183
Cernea CR, Nishio S, Hojaij FC (1995) Identification of the external branch of the superior laryngeal nerve (EBSLN) in large goiters. Am J Otolaryngol 16:307–311
Cernea CR, Ferraz AR, Furlani J et al (1992) Identification of the external branch of the superior laryngeal nerve during thyroidectomy. Am J Surg 164:634–639
Jaffe V, Young AE (1993) Strap muscles in thyroid surgery: to cut or not to cut? Ann R Coll Surg Engl 75:118
Vilkman E, Sonninen A, Hurme P et al (1996) External laryngeal frame function in voice production revisited: a review. J Voice 10:78–92
Hamdan AL, Kanazi G, Rameh C et al (2008) Immediate post-operative vocal changes in patients using laryngeal mask airway versus endotracheal tube. J Laryngol Otol 122:829–835
Kim CS, Park JO, Bae JS et al (2017) Long-lasting voice-related symptoms in patients without vocal cord palsy after thyroidectomy. World J Surg 42:2109–2116. https://doi.org/10.1007/s00268-017-4438-0
Van Lierde K, D'Haeseleer E, Wuyts FL et al (2010) Impact of thyroidectomy without laryngeal nerve injury on vocal quality characteristics: an objective multiparameter approach. Laryngoscope 120:338–345
Chun BJ, Bae JS, Lee SH et al (2015) A prospective randomized controlled trial of the laryngeal mask airway versus the endotracheal intubation in the thyroid surgery: evaluation of postoperative voice, and laryngopharyngeal symptom. World J Surg 39:1713–1720. https://doi.org/10.1007/s00268-015-2995-7
Lee JS, Kim JP, Ryu JS et al (2018) Effect of wound massage on neck discomfort and voice changes after thyroidectomy. Surgery 164:965–971
Chan WF, Lang BH, Lo CY (2006) The role of intraoperative neuromonitoring of recurrent laryngeal nerve during thyroidectomy: a comparative study on 1000 nerves at risk. Surgery 140:866–872 discussion 872-863
Wong KP, Mak KL, Wong CK et al (2017) Systematic review and meta-analysis on intra-operative neuro-monitoring in high-risk thyroidectomy. Int J Surg 38:21–30
Higgins TS, Gupta R, Ketcham AS et al (2011) Recurrent laryngeal nerve monitoring versus identification alone on post-thyroidectomy true vocal fold palsy: a meta-analysis. Laryngoscope 121:1009–1017
Pisanu A, Porceddu G, Podda M et al (2014) Systematic review with meta-analysis of studies comparing intraoperative neuromonitoring of recurrent laryngeal nerves versus visualization alone during thyroidectomy. J Surg Res 188:152–161
Engelsman AF, Warhurst S, Fraser S et al (2018) Influence of neural monitoring during thyroid surgery on nerve integrity and postoperative vocal function. BJS open 2:135–141
Stemple JC, Lee L, D'Amico B et al (1994) Efficacy of vocal function exercises as a method of improving voice production. J Voice 8:271–278
Borel F, Tresallet C, Hamy A et al (2020) Self-assessment of voice outcomes after total thyroidectomy using the voice handicap index questionnaire: results of a prospective multicenter study. Surgery 167:129–136
Funding
The authors have no commercial interests related to the subject of the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have declared that no competing interest exists.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kim, SY., Park, JO., Bae, JS. et al. How Can We Predict the Recovery from Pitch Lowering After Thyroidectomy?. World J Surg 44, 3395–3404 (2020). https://doi.org/10.1007/s00268-020-05628-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-020-05628-6