Abstract
Background
The burden of surgical disease in refugee and internally displaced person (IDP) populations has not been well defined. Populations fleeing conflict are mobile, limiting the effectiveness of traditional sampling methods. We employed novel sampling and survey techniques to conduct a population-based surgical needs assessment amongst IDPs in Kerenik, West Darfur, Sudan, over 4 weeks in 2008.
Methods
Satellite imagery was used to identify man-made structures. Ground teams were guided by GPS to randomly selected households. A newly created surgical needs survey was administered by surgeons to household members. One randomly selected individual answered demographic and medical history questions pertaining to themselves and first-degree blood relatives. All household members were offered a physical examination looking for surgical disease.
Findings
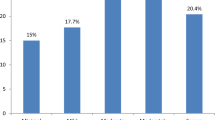
There were 780 study participants; 82% were IDPs. A history since displacement of surgical and potentially surgical conditions was reported in 38% of respondents and by 73% of respondents in first-degree blood relatives. Surgical histories included trauma (gunshots, stabbings, assaults) (5% respondents; 27% relatives), burns (6% respondents; 14% relatives), and obstetrical problems (5% female respondents; 11% relatives). 1485 individuals agreed to physical examinations. Untreated surgical and potentially surgical disease was identified in 25% of participants.
Interpretation
We identified and characterized a high burden of surgical and potentially surgical disease in an IDP population in West Darfur. Our study is unique in its direct assessment of a traumatized, mobile, vulnerable population. Health officials and agencies charged with the care of IDP and refugee populations should be aware of the high prevalence of surgical and potentially surgical conditions in these communities. This study adds to the growing body of evidence that investment in surgical resources may address a significant portion of the overall burden of disease in marginalized populations.


Similar content being viewed by others
References
Meara JG, Leather AJM, Hagander L et al (2015) Global Surgery 2030: evidence and solutions for achieving health, welfare, and economic development. Lancet 386:569–624
Bickler S, Ozgediz D, Gosselin R et al (2010) Key concepts for estimating the burden of surgical conditions and the unmet need for surgical care. World J Surg 34:374–380. https://doi.org/10.1007/s00268-009-0261-6
Groen RS, Samai M, Stewart K-A et al (2012) Untreated surgical conditions in Sierra Leone: a cluster randomised, cross-sectional, countrywide survey. Lancet 380:1082–1087
Petroze RT, Joharifard S, Groen RS et al (2015) Injury, disability and access to care in Rwanda: results of a nationwide cross-sectional population study. World J Surg 39:62–69. https://doi.org/10.1007/s00268-014-2544-9
Tran TM, Fuller AT, Butler EK et al (2017) Burden of surgical conditions in Uganda: a cross-sectional nationwide household survey. Ann Surg 266:389–399
Varela C, Young S, Groen R, Banza L, Mkandawire NC, Viste A (2017) Untreated surgical conditions in Malawi: a randomised cross-sectional nationwide household survey. Malawi Med J 29:231–236
Ang JW, Chia C, Koh CJ et al (2017) Healthcare-seeking behaviour, barriers and mental health of non-domestic migrant workers in Singapore. BMJ Glob Heal 2:e000213
Wångdahl J, Lytsy P, Mårtensson L, Westerling R (2018) Poor health and refraining from seeking healthcare are associated with comprehensive health literacy among refugees: a Swedish cross-sectional study. Int J Public Health 63:409–419
UN: 460,000 displaced in Darfur this year. Al Jazeera. 2013. https://www.aljazeera.com/news/africa/2013/11/un-displaced-violence-darfur-20131114132610566629.html
Coalition for International Justice. Chronology of Reporting on Events Concerning the Conflict in Darfur, Sudan. 2006
Yagub AIA, Mtshali K (2015) The role of non-governmental organizations in providing curative health services in North Darfur State, Sudan. Afr Health Sci 15:1049–1055
Lin Y, Kuwayama DP (2016) Using satellite imagery and GPS technology to create random sampling frames in high risk environments. Int J Surg 32:123–128
Zha Y, Stewart B, Lee E et al (2016) Global estimation of surgical procedures needed for forcibly displaced persons. World J Surg 40:2628–2634. https://doi.org/10.1007/s00268-016-3579-x
Kandasamy T, Cherniak R, Shah R, Yudin MH, Spitzer R (2014) Obstetric risks and outcomes of refugee women at a single centre in Toronto. J Obstet Gynaecol Canada 36:296–302
Niclas Broer P, Juran S (2016) Letter to the editor: surgical needs of refugee populations in the European Union: implications for plastic and reconstructive surgery. World J Plast Surg 5:325–327
Gibson-Helm M, Teede H, Block A et al (2014) Maternal health and pregnancy outcomes among women of refugee background from African countries: a retrospective, observational study in Australia. BMC Pregnancy Childbirth 14:392
Loucas M, Loucas R, Muensterer OJ (2018) Surgical health needs of minor refugees in Germany: a cross-sectional study. Eur J Pediatr Surg 28:60–66
Trudeau MO, Rothstein DH (2016) Injuries and surgical needs of children in conflict and disaster: from Boston to Haiti and beyond. Semin Pediatr Surg 25:23–31
WHO Expanded Programme on Immunization. The EPI coverage survey. In: Training for mid-level managers. 2008: 90
Bennett S, Radalowicz A, Vella V, Tomkins A (1994) A computer simulation of household sampling schemes for health surveys in developing countries. Int J Epidemiol 23:1282–1291
Grais RF, Rose AMC, Guthmann J-P (2007) Don’t spin the pen: two alternative methods for second-stage sampling in urban cluster surveys. Emerg Themes Epidemiol 4:1–7
Sonderman KA, Citron I, Meara JG (2018) National surgical, obstetric, and anesthesia planning in the context of global surgery: the way forward. JAMA Surg 153:E1–E2
Price R, Makasa E, Hollands M (2015) World health assembly resolution WHA68.15: ‘strengthening emergency and essential surgical care and anesthesia as a component of universal health coverage’—addressing the public health gaps arising from lack of safe, affordable and accessible surgical and anesthetic services. World J Surg 39:2115–2125. https://doi.org/10.1007/s00268-015-3153-y
Funding
Dr. Kuwayama reports a grant from Princeton University’s Woodrow Wilson School of Public and International Affairs, and non-financial support from Save The Children—Sudan, during the conduct of the study. Dr. Frist was the U.S. Senate Majority Leader from 2003 to 2008 and was involved in formulation of U.S. policy toward Sudan.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The other authors have nothing to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
Appendix

Rights and permissions
About this article
Cite this article
Kuwayama, D.P., Chu, K.M., Hartman, Z. et al. Surgical Needs of Internally Displaced Persons in Kerenik, West Darfur, Sudan. World J Surg 44, 3224–3236 (2020). https://doi.org/10.1007/s00268-020-05603-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-020-05603-1