Abstract
Background
Acute respiratory distress syndrome (ARDS) is associated with high morbidity and mortality. In addition, its aetiologies are heterogeneous, and the outcome depends on the underlying cause. In trauma care, changes in diagnostics, management and treatment may influence the outcome of posttraumatic ARDS over time, which are attributable to geographic distribution, relate to the definition used and depend on the injury severity.
Methods
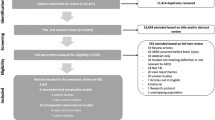
We selected studies by searching PubMed using the MeSH terms “acute respiratory distress syndrome”, “mortality” and “trauma” and all their combinations. Studies that reported mortality rates for polytrauma patients with ARDS were included. We excluded studies with selected population collectives (e.g. burn patients, isolated thoracic trauma and paediatric trauma) and non-trauma studies. Studies were stratified according to the recruitment year of patients into Decade 1 (prior 1990), Decade 2(1990–1999), Decade 3 (2000–2009) and Decade 4 (later 2009); geographic location (North America or Europe), the definition used in the different studies (American European Consensus Conference (AECC) definition or Berlin definition) and the mean injury severity of the patient populations, respectively.
Results
Twenty-three studies between 1 January 1980 and 30 June 2018 were included in the analysis (486,861 patients, 52,561 with posttraumatic ARDS). There was a wide variation in mortality rates among the studies (4–39%). The overall pooled mean mortality rate for all studies was 21.8%, SD ± 8.3%. The mean mortality over the last four decades was similar between decade 1 (25.8%), decade 2 (20.6%), decade 3 (20.7%) and decade 4 (22.5%). Geographical observations comparing Europe and North America revealed no difference [Europe (22.1%) and North America (21.7%)]. The ARDS mortality in publications using the Berlin definition (23%) was comparable to the mortality rate in publications using the AECC definition (22.9%). The mortality rate based on the injury severity showed no alteration (ISS ≤ 25 points, 22.6%, ISS > 25 points, 22.6%).
Conclusion
In this systematic review, there was no change in the mortality rate over the last four decades, no geographical difference within Western societies, no dependence on the ARDS definition used and no association with injury severity, respectively.

Similar content being viewed by others
References
Sigurdsson MI, Sigvaldason K, Gunnarsson TS et al (2013) Acute respiratory distress syndrome: nationwide changes in incidence, treatment and mortality over 23 years. Acta Anaesthesiol Scand 57:37–45. https://doi.org/10.1111/aas.12001
Bellani G, Laffey JG, Pham T et al (2016) Epidemiology, patterns of care, and mortality for patients with acute respiratory distress syndrome in intensive care units in 50 countries. JAMA 315:788. https://doi.org/10.1001/jama.2016.0291
Villar J, Blanco J, Añón JM et al (2011) The ALIEN study: incidence and outcome of acute respiratory distress syndrome in the era of lung protective ventilation. Intensive Care Med 37:1932–1941. https://doi.org/10.1007/s00134-011-2380-4
Ashbaugh D, Boyd Bigelow D, Petty T, Levine B (1967) Acute respiratory distress syndrome in adults. Lancet 290:319–323. https://doi.org/10.1016/S0140-6736(67)90168-7
Ranieri VM, Rubenfeld GD, Thompson BT et al (2012) Acute respiratory distress syndrome: the Berlin definition. JAMA - J Am Med Assoc 307:2526–2533. https://doi.org/10.1001/jama.2012.5669
Laffey JG, Bellani G, Pham T et al (2016) Potentially modifiable factors contributing to outcome from acute respiratory distress syndrome: the LUNG SAFE study. Intensive Care Med 42:1865–1876. https://doi.org/10.1007/s00134-016-4571-5
Ware L (2006) Pathophysiology of acute lung injury and the acute respiratory distress syndrome. Semin Respir Crit Care Med 27:337–349. https://doi.org/10.1055/s-2006-948288
Daurat A, Millet I, Roustan J-P et al (2016) Thoracic Trauma Severity score on admission allows to determine the risk of delayed ARDS in trauma patients with pulmonary contusion. Injury 47:147–153. https://doi.org/10.1016/j.injury.2015.08.031
Rezoagli E, Fumagalli R, Bellani G (2017) Definition and epidemiology of acute respiratory distress syndrome. Ann Transl Med 5:282. https://doi.org/10.21037/atm.2017.06.62
Michalewicz E, Pape H-C (2014) Adult respiratory distress syndrome induced by blunt trauma—a dying threat throughout the world? Injury 45:643–644. https://doi.org/10.1016/j.injury.2013.12.008
Wu R, Lin S-Y, Zhao H-M (2015) Albuterol in the treatment of acute respiratory distress syndrome: a meta-analysis of randomized controlled trials. World J Emerg Med 6:165–171. https://doi.org/10.5847/wjem.j.1920-8642.2015.03.001
Kolarik M, Roberts E (2017) Permissive hypotension and trauma: can fluid restriction reduce the incidence of ARDS? J Trauma Nurs 24:19–24. https://doi.org/10.1097/JTN.0000000000000257
Briel M, Meade M, Mercat A et al (2010) Higher vs lower positive end-expiratory pressure in patients with acute lung injury and acute respiratory distress syndrome. JAMA 303:865. https://doi.org/10.1001/jama.2010.218
Schreiber A, Yıldırım F, Ferrari G et al (2018) Non-invasive mechanical ventilation in critically ill trauma patients: a systematic review. Turkish J Anaesthesiol Reanim 46:88–95. https://doi.org/10.5152/TJAR.2018.46762
Watson GA, Sperry JL, Rosengart MR et al (2009) Fresh frozen plasma is independently associated with a higher risk of multiple organ failure and acute respiratory distress syndrome. J Trauma 67:221–227. https://doi.org/10.1097/TA.0b013e3181ad5957discussion 228–230
Teman NR, Thomas J, Bryner BS et al (2015) Inhaled nitric oxide to improve oxygenation for safe critical care transport of adults with severe hypoxemia. Am J Crit Care 24:110–117. https://doi.org/10.4037/ajcc2015570
Afshari A, Brok J, Møller AM, Wetterslev J (2011) Inhaled nitric oxide for acute respiratory distress syndrome and acute lung injury in adults and children. Anesth Analg 112:1411–1421. https://doi.org/10.1213/ANE.0b013e31820bd185
Langan NR, Eckert M, Martin MJ (2014) Changing patterns of in-hospital deaths following implementation of damage control resuscitation practices in US forward military treatment facilities. JAMA Surg 149:904. https://doi.org/10.1001/jamasurg.2014.940
Hirshberg A, Hoyt DB, Mattox KL (2007) From “leaky buckets” to vascular injuries: understanding models of uncontrolled hemorrhage. J Am Coll Surg 204:665–672. https://doi.org/10.1016/J.JAMCOLLSURG.2007.01.005
Kahl JE, Calvo RY, Sise MJ et al (2013) The changing nature of death on the trauma service. J Trauma Acute Care Surg 75:195–201. https://doi.org/10.1097/TA.0b013e3182997865
Pape HC, Remmers D, Rice J et al (2000) Appraisal of early evaluation of blunt chest trauma: development of a standardized scoring system for initial clinical decision making. J Trauma - Inj Infect Crit Care 49:496–504. https://doi.org/10.1097/00005373-200009000-00018
Pfeifer R, Heussen N, Michalewicz E et al (2017) Incidence of adult respiratory distress syndrome in trauma patients: a systematic review and meta-analysis over a period of three decades. J Trauma Acute Care Surg 83:496–506. https://doi.org/10.1097/TA.0000000000001571
Andrews PL, Shiber JR, Jaruga-Killeen E et al (2013) Early application of airway pressure release ventilation may reduce mortality in high-risk trauma patients: a systematic review of observational trauma ARDS literature. J Trauma Acute Care Surg 75:635–641. https://doi.org/10.1097/TA.0b013e31829d3504
Liberati A, Altman DG, Tetzlaff J et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339:b2700. https://doi.org/10.1136/bmj.b2700
Moher D, Liberati A, Tezlaff J, Altman D (2009) PRISMA 2009 checklist. www.prisma-statement.org. Accessed 9 Apr 2019
Baker SP, O’Neill B, Haddon W, Long WB (1974) The injury severity score: a method for describing patients with multiple injuries and evaluating emergency care. J Trauma 14:187–196
Bernard GR, Artigas A, Brigham KL et al (1994) The American-European Consensus Conference on ARDS. Definitions, mechanisms, relevant outcomes, and clinical trial coordination. Am J Respir Crit Care Med 149:818–824. https://doi.org/10.1164/ajrccm.149.3.7509706
Regel G, Lobenhoffer P, Grotz M et al (1995) Treatment results of patients with multiple trauma: an analysis of 3406 cases treated between 1972 and 1991 at a German Level I Trauma Center. J Trauma 38:70–78
Davidson TA, Rubenfeld GD, Caldwell ES et al (1999) The effect of acute respiratory distress syndrome on long-term survival. Am J Respir Crit Care Med 160:1838–1842. https://doi.org/10.1164/ajrccm.160.6.9903058
Navarrete-Navarro P, Ruiz-Bailén M, Rivera-Fernández R et al (2000) Acute respiratory distress syndrome in trauma patients: ICU mortality and prediction factors. Intensive Care Med 26:1624–1629. https://doi.org/10.1007/s001340000683
Navarrete-Navarro P, Rodriguez A, Reynolds N et al (2001) Acute respiratory distress syndrome among trauma patients: trends in ICU mortality, risk factors, complications and resource utilization. Intensive Care Med 27:1133–1140. https://doi.org/10.1007/s001340100955
Johnston CJ, Rubenfeld GD, Hudson LD (2003) Effect of age on the development of ARDS in trauma patients. Chest 124:653–659. https://doi.org/10.1378/chest.124.2.653
Treggiari MM, Hudson LD, Martin DP et al (2004) Effect of acute lung injury and acute respiratory distress syndrome on outcome in critically ill trauma patients. Crit Care Med 32:327–331. https://doi.org/10.1097/01.CCM.0000108870.09693.42
Martin M, Salim A, Murray J et al (2005) The decreasing incidence and mortality of acute respiratory distress syndrome after injury: a 5-year observational study. J Trauma - Inj Infect Crit Care 59:1107–1113. https://doi.org/10.1097/01.ta.0000188633.94766.d0
Recinos G, DuBose JJ, Teixeira PGR et al (2009) ACS trauma centre designation and outcomes of post-traumatic ARDS: NTDB analysis and implications for trauma quality improvement. Injury 40:856–859. https://doi.org/10.1016/j.injury.2008.11.001
Shah CV, Lanken PN, Localio AR et al (2010) An alternative method of acute lung injury classification for use in observational studies. Chest 138:1054–1061. https://doi.org/10.1378/chest.09-2697
Plurad DS, Bricker S, Talving P et al (2011) Trauma center designation and the decreasing incidence of post-traumatic acute respiratory distress syndrome: a potential guidepost for quality improvement. Am J Surg 202:829–836. https://doi.org/10.1016/j.amjsurg.2011.07.007
Strumwasser A, Chu E, Yeung L et al (2011) A novel CT volume index score correlates with outcomes in polytrauma patients with pulmonary contusion. J Surg Res 170:280–285. https://doi.org/10.1016/j.jss.2011.03.022
Zielinski MD, Jenkins D, Cotton BA et al (2014) Adult respiratory distress syndrome risk factors for injured patients undergoing damage-control laparotomy: AAST multicenter post hoc analysis. J Trauma Acute Care Surg 77:886–891. https://doi.org/10.1097/TA.0000000000000421
Reilly JP, Bellamy S, Shashaty MGS et al (2014) Heterogeneous phenotypes of acute respiratory distress syndrome after major trauma. Ann Am Thorac Soc 11:728–736. https://doi.org/10.1513/AnnalsATS.201308-280OC
Haider AH, Gupta S, Zogg CK et al (2015) Beyond incidence: costs of complications in trauma and what it means for those who pay. Surgery (United States) 158:96–103. https://doi.org/10.1016/j.surg.2015.02.015
Howard BM, Kornblith LZ, Hendrickson CM et al (2015) Differences in degree, differences in kind: characterizing lung injury in trauma. J Trauma Acute Care Surg 78:735–741. https://doi.org/10.1097/TA.0000000000000583
O’Leary MP, Keeley JA, Yule A et al (2016) Clinical predictors of early acute respiratory distress syndrome in trauma patients. Am J Surg 212:1096–1100. https://doi.org/10.1016/j.amjsurg.2016.09.008
Park PK, Cannon JW, Ye W et al (2016) Incidence, risk factors, and mortality associated with acute respiratory distress syndrome in combat casualty care. J Trauma Acute Care Surg 81:S150–S156. https://doi.org/10.1097/TA.0000000000001183
Engström J, Reinius H, Ström J et al (2016) Lung complications are common in intensive care treated patients with pelvis fractures: a retrospective cohort study. Scand J Trauma Resusc Emerg Med 24:1–9. https://doi.org/10.1186/s13049-016-0244-1
Fahr M, Jones G, O’Neal H et al (2017) Acute respiratory distress syndrome incidence, but not mortality, has decreased nationwide: a national trauma data bank study. Am Surg 83:323–331
Haider T, Halat G, Heinz T et al (2017) Thoracic trauma and acute respiratory distress syndrome in polytraumatized patients: a retrospective analysis. Minerva Anestesiol 83:1026–1033. https://doi.org/10.23736/S0375-9393.17.11728-1
Robles AJ, Kornblith LZ, Hendrickson CM et al (2018) Health care utilization and the cost of post-traumatic ARDS care. J Trauma Acute Care Surg. https://doi.org/10.1117/1.JBO.17.9.097001
Daher P, Teixeira PG, Coopwood TB et al (2018) Mild to moderate to severe: What drives the severity of ARDS in trauma patients? Am Surg 84:813–819
O’Toole RV, O’Brien M, Scalea TM et al (2009) Resuscitation before stabilization of femoral fractures limits acute respiratory distress syndrome in patients with multiple traumatic injuries despite low use of damage control orthopedics. J Trauma Inj Infect Crit Care 67:1013–1021. https://doi.org/10.1097/TA.0b013e3181b890be
Nahm NJ, Vallier HA (2012) Timing of definitive treatment of femoral shaft fractures in patients with multiple injuries. J Trauma Acute Care Surg 73:1046–1063. https://doi.org/10.1097/TA.0b013e3182701ded
Higgins JPT, Altman DG, Gotzsche PC et al (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343:d5928. https://doi.org/10.1136/bmj.d5928
Higgins JP, Altman DG, Sterne JA (2011) Chapter 8: assessing risk of bias in included studies. In: Higgins JP, Green S (eds) Cochrane handbook for systematic reviews of interventions. Wiley, Hoboken
Wind J, Versteegt J, Twisk J et al (2007) Epidemiology of acute lung injury and acute respiratory distress syndrome in The Netherlands: a survey. Respir Med 101:2091–2098. https://doi.org/10.1016/j.rmed.2007.05.021
Ware LB, Matthay MA (2000) The acute respiratory distress syndrome. N Engl J Med 342:1334–1349. https://doi.org/10.1056/NEJM200005043421806
Stapleton RD, Wang BM, Hudson LD et al (2005) Causes and timing of death in patients with ARDS. Chest 128:525–532. https://doi.org/10.1378/CHEST.128.2.525
Erickson SE, Martin GS, Davis JL et al (2009) Recent trends in acute lung injury mortality: 1996–2005. Crit Care Med 37:1574–1579. https://doi.org/10.1097/CCM.0b013e31819fefdf
Pfeifer R, Tarkin IS, Rocos B, Pape H-C (2009) Patterns of mortality and causes of death in polytrauma patients—has anything changed? Injury 40:907–911. https://doi.org/10.1016/j.injury.2009.05.006
Hofman M, Sellei R, Peralta R et al (2012) Trauma systems: models of prehospital and inhospital care. Eur J Trauma Emerg Surg 38:253–260. https://doi.org/10.1007/s00068-012-0192-z
D’Alleyrand J-CG, O’Toole RV (2013) The evolution of damage control orthopedics. Orthop Clin North Am 44:499–507. https://doi.org/10.1016/j.ocl.2013.06.004
Pape H-C, Tornetta P, Tarkin I et al (2009) Timing of fracture fixation in multitrauma patients: the role of early total care and damage control surgery. J Am Acad Orthop Surg 17:541–549
Schreiber VM, Tarkin IS, Hildebrand F et al (2011) The timing of definitive fixation for major fractures in polytrauma—a matched-pair comparison between a US and European level I centres: analysis of current fracture management practice in polytrauma. Injury 42:650–654. https://doi.org/10.1016/j.injury.2010.07.248
Villar J, Sulemanji D, Kacmarek RM (2014) The acute respiratory distress syndrome: incidence and mortality, has it changed? Curr Opin Crit Care 20:3–9. https://doi.org/10.1097/MCC.0000000000000057
Rubenfeld GD, Caldwell E, Peabody E et al (2005) Incidence and outcomes of acute lung injury. N Engl J Med 353:1685–1693. https://doi.org/10.1056/NEJMoa050333
Thille AW, Esteban A, Fernández-Segoviano P et al (2013) Comparison of the Berlin definition for acute respiratory distress syndrome with autopsy. Am J Respir Crit Care Med 187:761–767. https://doi.org/10.1164/rccm.201211-1981OC
Hughes KT, Beasley MB (2017) Pulmonary manifestations of acute lung injury: more than just diffuse alveolar damage. Arch Pathol Lab Med 141:916–922. https://doi.org/10.5858/arpa.2016-0342-RA
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Birkner, D.R., Halvachizadeh, S., Pape, HC. et al. Mortality of Adult Respiratory Distress Syndrome in Trauma Patients: A Systematic Review over a Period of Four Decades. World J Surg 44, 2243–2254 (2020). https://doi.org/10.1007/s00268-020-05483-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-020-05483-5