Abstract
Background
Esophagectomy has a high risk of postoperative morbidity, and pulmonary complications are the most common causes of serious morbidity. Thoracoscopic esophagectomy has been reported to reduce postoperative pulmonary complications; however, it remains unclear whether laparoscopic gastric mobilization can reduce the occurrence of postoperative pulmonary complications after open thoracotomy or thoracoscopic esophagectomy. The present meta-analysis assessed the ability of laparoscopic gastric mobilization to prevent postoperative complications after open thoracotomy or thoracoscopic esophagectomy.
Method
Studies reported between January 2000 and April 2019 in the PubMed and the Cochrane Library databases that analyzed the impact of laparoscopy on postoperative complications were systematically reviewed. In the meta-analysis, data were pooled and the primary outcome was postoperative pulmonary complications. The secondary outcomes were other postoperative complications, operative details, length of hospital stay and postoperative mortality.
Results
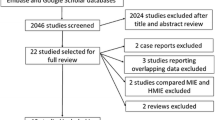
A total of 13 studies (1915 patients; 1 randomized trial, 1 prospective study and 11 observational studies) were included. Laparoscopic gastric mobilization after open thoracotomy resulted in significantly reduced postoperative pulmonary complications (OR = 0.47, 95% confidence interval (CI): 0.27–0.82, p = 0.008) and postoperative mortality (OR = 0.49, 95%CI: 0.25–0.94, p = 0.03). Similarly, laparoscopic gastric mobilization after thoracoscopic esophagectomy resulted in significantly reduced postoperative pulmonary complications (OR = 0.56, 95%CI: 0.37–0.84, p = 0.005) and anastomotic leakage (OR = 0.59, 95%CI: 0.39–0.91, p = 0.02).
Conclusions
Laparoscopic gastric mobilization could be recommended for reducing postoperative pulmonary complications after esophagectomy irrespective of the thoracic approach.



Similar content being viewed by others
References
Torre LA, Bray F, Siegel RL et al (2015) Global cancer statistics, 2012. CA Cancer J Clin 65:87–108
Ando N, Ozawa S, Kitagawa Y et al (2000) Improvement in the results of surgical treatment of advanced squamous esophageal carcinoma during 15 consecutive years. Ann Surg 232:225–232
Cooper JS, Guo MD, Herskovic A et al (1999) Chemoradiotherapy of locally advanced esophageal cancer: long-term follow-up of a prospective randomized trial (RTOG 85-01). Radiat Ther Oncol Group JAMA 281:1623–1627
Takeuchi H, Saikawa Y, Oyama T et al (2010) Factors influencing the long-term survival in patients with esophageal cancer who underwent esophagectomy after chemoradiotherapy. World J Surg 34:277–284. https://doi.org/10.1007/s00268-009-0331-9
Takeuchi H, Miyata H, Gotoh M et al (2014) A risk model for esophagectomy using data of 5354 patients included in a Japanese nationwide web-based database. Ann Surg 260:259–266
Booka E, Takeuchi H, Kikuchi H et al (2019) Recent advances in thoracoscopic esophagectomy for esophageal cancer. Asian J Endosc Surg 12:19–29
Guo W, Ma X, Yang S et al (2016) Combined thoracoscopic–laparoscopic esophagectomy versus open esophagectomy: a meta-analysis of outcomes. Surg Endosc 30:3873–3881
Stroup DF, Berlin JA, Morton SC et al (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis of observational studies in epidemiology (MOOSE) group. JAMA 283:2008–2012
Balshem H, Helfand M, Schunemann HJ et al (2011) GRADE guidelines: 3. Rating the quality of evidence. J Clin Epidemiol 64:401–406
Clavien PA, Barkun J, de Oliveira ML et al (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196
Briez N, Piessen G, Torres F et al (2012) Effects of hybrid minimally invasive oesophagectomy on major postoperative pulmonary complications. Br J Surg 99:1547–1553
Bailey L, Khan O, Willows E et al (2013) Open and laparoscopically assisted oesophagectomy: a prospective comparative study. Eur J Cardiothorac Surg 43:268–273
Kitagawa H, Namikawa T, Iwabu J et al (2013) Efficacy of laparoscopic gastric mobilization for esophagectomy: comparison with open thoraco-abdominal approach. J Laparoendosc Adv Surg Tech A 23:452–455
Findlay L, Yao C, Bennett DH et al (2017) Non-inferiority of minimally invasive oesophagectomy: an 8-year retrospective case series. Surg Endosc 31:3681–3689
Glatz T, Marjanovic G, Kulemann B et al (2017) Hybrid minimally invasive esophagectomy vs. open esophagectomy: a matched case analysis in 120 patients. Langenbeck’s Arch Surg / Deutsche Gesellschaft fur Chirurgie 402:323–331
Nozaki I, Mizusawa J, Kato K et al (2018) Impact of laparoscopy on the prevention of pulmonary complications after thoracoscopic esophagectomy using data from JCOG0502: a prospective multicenter study. Surg Endosc 32:651–659
Mariette C, Markar SR, Dabakuyo-Yonli TS et al (2019) Hybrid minimally invasive esophagectomy for esophageal cancer. N Engl J Med 380:152–162
Lee JM, Cheng JW, Lin MT et al (2011) Is there any benefit to incorporating a laparoscopic procedure into minimally invasive esophagectomy? The impact on perioperative results in patients with esophageal cancer. World J Surg 35:790–797. https://doi.org/10.1007/s00268-011-0955-4
Kinjo Y, Kurita N, Nakamura F et al (2012) Effectiveness of combined thoracoscopic–laparoscopic esophagectomy: comparison of postoperative complications and midterm oncological outcomes in patients with esophageal cancer. Surg Endosc 26:381–390
Ichikawa H, Miyata G, Miyazaki S et al (2013) Esophagectomy using a thoracoscopic approach with an open laparotomic or hand-assisted laparoscopic abdominal stage for esophageal cancer: analysis of survival and prognostic factors in 315 patients. Ann Surg 257:873–885
Daiko H, Fujita T (2015) Laparoscopic assisted versus open gastric pull-up following thoracoscopic esophagectomy: A cohort study. Int J Surg 19:61–66
Oshikiri T, Yasuda T, Kawasaki K et al (2016) Hand-assisted laparoscopic surgery (HALS) is associated with less-restrictive ventilatory impairment and less risk for pulmonary complication than open laparotomy in thoracoscopic esophagectomy. Surgery 159:459–466
Yao F, Wang J, Yao J et al (2017) Is thoracoscopic–laparoscopic esophagectomy a better alternative to thoracoscopic esophagectomy? Int J Surg 48:105–109
Booka E, Takeuchi H, Nishi T et al (2015) The impact of postoperative complications on survivals after esophagectomy for esophageal cancer. Medicine 94:e1369
Booka E, Takeuchi H, Suda K et al (2018) Meta-analysis of the impact of postoperative complications on survival after oesophagectomy for cancer. BJS Open 2:276–284
Biere SS, van Berge Henegouwen MI, Maas KW et al (2012) Minimally invasive versus open oesophagectomy for patients with oesophageal cancer: a multicentre, open-label, randomised controlled trial. Lancet 379:1887–1892
Findlay JM, Gillies RS, Millo J et al (2014) Enhanced recovery for esophagectomy: a systematic review and evidence-based guidelines. Ann Surg 259:413–431
Kitano S, Shiraishi N, Fujii K et al (2002) A randomized controlled trial comparing open vs laparoscopy-assisted distal gastrectomy for the treatment of early gastric cancer: an interim report. Surgery 131:S306–S311
Booka E, Nakano Y, Mihara K et al (2019) The impact of epidural catheter insertion level on pain control after esophagectomy for esophageal cancer. Esophagus. https://doi.org/10.1007/s10388-019-00682-z
Bhat MA, Dar MA, Lone GN et al (2006) Use of pedicled omentum in esophagogastric anastomosis for prevention of anastomotic leak. Ann Thorac Surg 82:1857–1862
Kataoka K, Takeuchi H, Mizusawa J et al (2016) A randomized Phase III trial of thoracoscopic versus open esophagectomy for thoracic esophageal cancer: Japan Clinical Oncology Group Study JCOG1409. Jpn J Clin Oncol 46:174–177
Acknowledgements
The authors thank Mutsumi Yamazaki of Shizuoka Cancer Center Medical Library for assisting in the systematic literature search.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical statement
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
268_2019_5272_MOESM1_ESM.tiff
Supplementary Figure 1. Forest plots comparing the impacts of laparoscopic gastric mobilization and open gastric mobilization after open esophagectomy on pneumonia only. The Mantel–Haenszel random-effect model was used for the meta-analysis. Odds ratios are shown with 95% confidence intervals. (TIFF 470 kb)
268_2019_5272_MOESM2_ESM.tiff
Supplementary Figure 2. Forest plots comparing the impacts of laparoscopic gastric mobilization and open gastric mobilization after thoracoscopic esophagectomy on pneumonia only. The Mantel–Haenszel random-effect model was used for the meta-analysis. Odds ratios are shown with 95% confidence intervals. (TIFF 438 kb)
268_2019_5272_MOESM3_ESM.tiff
Supplementary Figure 3. Forest plots comparing the impacts of laparoscopic gastric mobilization and open gastric mobilization after thoracoscopic esophagectomy on severe pulmonary complications (Clavien–Dindo classification grade of III or higher). The Mantel–Haenszel fixed-effect model was used for the meta-analysis. Odds ratios are shown with 95% confidence intervals. (TIFF 419 kb)
Rights and permissions
About this article
Cite this article
Booka, E., Tsubosa, Y., Haneda, R. et al. Ability of Laparoscopic Gastric Mobilization to Prevent Pulmonary Complications After Open Thoracotomy or Thoracoscopic Esophagectomy for Esophageal Cancer: A Systematic Review and Meta-analysis. World J Surg 44, 980–989 (2020). https://doi.org/10.1007/s00268-019-05272-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-019-05272-9