Abstract
Background
The objective of the present meta-analysis was to evaluate the clinicopathological significance and prognosis of micro-MTC compared to macro-MTC.
Methods
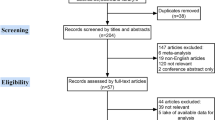
Relevant articles were obtained by searching the PubMed and MEDLINE databases. A meta-analysis was performed using 15 eligible studies. In addition, subgroup analysis based on heredity was performed in patients diagnosed with micro-MTC.
Results
The rate of extrathyroidal extension of micro-MTC [0.118 (95% CI 0.073–0.185)] was significantly lower than that of macro-MTC [0.303 (95% CI 0.224–0.395)]. Micro-MTC [0.229 (95% CI 0.161–0.314)] had a significantly lower rate of cervical lymph node (LN) metastasis compared to macro-MTC [0.595 (95% CI 0.486–0.694)]. The rate of multifocality was not significantly different between micro-MTC and macro-MTC [0.394 (95% CI 0.244–0.566) vs. 0.320 (95% CI 0.234–0.421), respectively]. The rate of distant metastasis did not differ significantly between micro-MTC [0.082 (95% CI 0.017–0.314)] and macro-MTC [0.068 (95% CI 0.009–0.376)]. Patients with micro-MTC showed significantly higher disease-free survival rates [hazard ratio [HR] 0.406 (95% CI 0.288–0.575), I 2 = 40.563%] compared to patients with macro-MTC.
Conclusion
Micro-MTC has aggressive features, such as multifocality and distant metastasis, similar to macro-MTC and a non-negligible rate of extrathyroidal extension and cervical LN metastasis. We suggest that treatment of micro-MTC should be approached with a similar focus as that of macro-MTC. Considering that less extrathyroidal extension and cervical LN metastasis occur in patients with micro-MTC compared to macro-MTC, we propose that treatment of micro-MTC, which has a relatively low disease burden status, should be viewed as an opportunity for improving prognosis.


Similar content being viewed by others
References
Hundahl SA, Fleming ID, Fremgen AM et al (1998) A National Cancer Data Base report on 53,856 cases of thyroid carcinoma treated in the U.S., 1985–1995. Cancer 83:2638–2648
Scollo C, Baudin E, Travagli JP et al (2003) Rationale for central and bilateral lymph node dissection in sporadic and hereditary medullary thyroid cancer. J Clin Endocrinol Metab 88:2070–2075
Wells SA Jr, Asa SL, Dralle H, American Thyroid Association Guidelines Task Force on Medullary Thyroid Carcinoma et al (2015) Revised American Thyroid Association guidelines for the management of medullary thyroid carcinoma. Thyroid 25:567–610
Kwon H, Kim WG, Sung TY et al (2016) Changing trends in the clinicopathological features and clinical outcomes of medullary thyroid carcinoma. J Surg Oncol 113:152–158
Beressi N, Campos JM, Beressi JP et al (1998) Sporadic medullary microcarcinoma of the thyroid: a retrospective analysis of eighty cases. Thyroid 8:1039–1044
Hamy A, Pessaux P, Mirallié E et al (2005) Central neck dissection in the management of sporadic medullary thyroid microcarcinoma. Eur J Surg Oncol 31:774–777
Kaserer K, Scheuba C, Neuhold N et al (2001) Sporadic versus familial medullary thyroid microcarcinoma: a histopathologic study of 50 consecutive patients. Am J Surg Pathol 25:1245–1251
Kazaure HS, Roman SA, Sosa JA (2012) Medullary thyroid microcarcinoma: a population-level analysis of 310 patients. Cancer 118:620–627
Machens A, Dralle H (2012) Biological relevance of medullary thyroid microcarcinoma. J Clin Endocrinol Metab 97:1547–1553
Pillarisetty VG, Katz SC, Ghossein RA et al (2009) Micromedullary thyroid cancer: How micro is truly micro? Ann Surg Oncol 16:2875–2881
Boschin IM, Torresan F, Toniato A et al (2014) Incidental medullary thyroid microcarcinoma revealed by mild increase of preoperative serum calcitonin levels: therapeutic implications. Endocrine 45:448–453
Esfandiari NH, Hughes DT, Yin H et al (2014) The effect of extent of surgery and number of lymph node metastases on overall survival in patients with medullary thyroid cancer. J Clin Endocrinol Metab 99:448–454
Guyétant S, Dupre F, Bigorgne JC et al (1999) Medullary thyroid microcarcinoma: a clinicopathologic retrospective study of 38 patients with no prior familial disease. Hum Pathol 30:957–963
Jung KY, Kim SM, Yoo WS et al (2016) Postoperative biochemical remission of serum calcitonin is the best predictive factor for recurrence-free survival of medullary thyroid cancer: a large-scale retrospective analysis over 30 years. Clin Endocrinol (Oxf) 84:587–597
Koperek O, Prinz A, Scheuba C et al (2009) Tenascin C in medullary thyroid microcarcinoma and C-cell hyperplasia. Virchows Arch 455:43–48
Krueger JE, Maitra A, Albores-Saavedra J (2000) Inherited medullary microcarcinoma of the thyroid: a study of 11 cases. Am J Surg Pathol 24:853–858
Saltiki K, Rentziou G, Stamatelopoulos K et al (2014) Small medullary thyroid carcinoma: post-operative calcitonin rather than tumour size predicts disease persistence and progression. Eur J Endocrinol 171:117–126
Scheuba C, Kaserer K, Bieglmayer C et al (2007) Medullary thyroid microcarcinoma recommendations for treatment—a single-center experience. Surgery 142:1003
Higgins JPT, Sterne JAC (2011) Chapter 8: Assessing risk of bias in included studies. In: Higgins JPT, Green S (eds) Cochrane handbook for systematic reviews of interventions version 510 cochrane collaboration. Wiley, Hoboken
Parmar MK, Torri V, Stewart L (1998) Extracting summary statistics to perform meta-analyses of the published literature for survival endpoints. Stat Med 17:2815–2834
Saad MF, Ordonez NG, Rashid RK et al (1984) Medullary carcinoma of the thyroid. A study of the clinical features and prognostic factors in 161 patients. Medicine (Baltimore) 63:319–342
Kebebew E, Ituarte PH, Siperstein AE et al (2000) Medullary thyroid carcinoma: clinical characteristics, treatment, prognostic factors, and a comparison of staging systems. Cancer 88:1139–1148
Kim BH, Kim IJ (2016) Recent updates on the management of medullary thyroid carcinoma. Endocrinol Metab (Seoul) 31:392–399
Davies L, Welch HG (2006) Increasing incidence of thyroid cancer in the United States, 1973–2002. JAMA 295:2164–2167
Haugen BR, Alexander EK, Bible KC et al (2016) 2015 American Thyroid Association Management Guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: the American Thyroid Association guidelines task force on thyroid nodules and differentiated thyroid cancer. Thyroid 26:1–133
Machens A, Dralle H (2013) Prognostic impact of N staging in 715 medullary thyroid cancer patients: proposal for a revised staging system. Ann Surg 257:323–329
Machens A, Schneyer U, Holzhausen HJ et al (2005) Prospects of remission in medullary thyroid carcinoma according to basal calcitonin level. J Clin Endocrinol Metab 90:2029–2034
Raffel A, Cupisti K, Krausch M et al (2004) Incidentally found medullary thyroid cancer: treatment rationale for small tumors. World J Surg 28:397–401. doi:10.1007/s00268-003-7121-6
Kebebew E, Greenspan FS, Clark OH et al (2005) Extent of disease and practice patterns for medullary thyroid cancer. J Am Coll Surg 200:890–896
Elisei R, Bottici V, Luchetti F et al (2004) Impact of routine measurement of serum calcitonin on the diagnosis and outcome of medullary thyroid cancer: experience in 10,864 patients with nodular thyroid disorders. J Clin Endocrinol Metab 89:163–168
Vierhapper H, Raber W, Bieglmayer C et al (1997) Routine measurement of plasma calcitonin in nodular thyroid diseases. J Clin Endocrinol Metab 82:1589–1593
Acknowledgements
This study was supported by research fund from Chosun University Hospital, 2016.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Kim, J.H., Pyo, JS. & Cho, W.J. Clinicopathological Significance and Prognosis of Medullary Thyroid Microcarcinoma: A Meta-analysis. World J Surg 41, 2551–2558 (2017). https://doi.org/10.1007/s00268-017-4031-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-017-4031-6