Abstract
Background
Availability of surgical site infection (SSI) surveillance rates challenges clinicians, healthcare administrators and leaders and the public. The purpose of this report is to demonstrate the consequences patient self-assessment strategies have on SSI reporting rates.
Methods
We performed SSI surveillance among patients undergoing general surgery procedures, including telephone follow-up 30 days after surgery. Additionally we undertook a separate validation study in which we compared patient self-assessments of SSI with surgeon assessment. Finally, we performed a meta-analysis of similar validation studies of patient self-assessment strategies.
Results
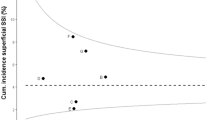
There were 22/266 in-hospital SSIs diagnosed (8.3%), and additional 16 cases were detected through the 30-day follow-up. In total, the SSI rate was 16.8% (95% CI 10.1–18.5). In the validation survey, we found patient telephone surveillance to have a sensitivity of 66% (95% CI 40–93%) and a specificity of 90% (95% CI 86–94%). The meta-analysis included five additional studies. The overall sensitivity was 83.3% (95% CI 79–88%), and the overall specificity was 97.4% (95% CI 97–98%). Simulation of the meta-analysis results divulged that when the true infection rate is 1%, reported rates would be 4%; a true rate of 50%, the reported rates would be 43%.
Conclusion
Patient self-assessment strategies in order to fulfill 30-day SSI surveillance misestimate SSI rates and lead to an erroneous overall appreciation of inter-institutional variation. Self-assessment strategies overestimate SSIs rate of institutions with high-quality performance and underestimate rates of poor performance. We propose such strategies be abandoned. Alternative strategies of patient follow-up strategies should be evaluated in order to provide valid and reliable information regarding institutional performance in preventing patient harm.

Similar content being viewed by others
References
National Nosocomial Infections Surveillance (NNIS) System Report (2004). Data summary from January 1992 through June 2004, issued October 2004. Am J Infect Control 32(8):470–485
Perencevich EN, Sands KE, Cosgrove SE, Guadagnoli E, Meara E, Platt R (2003) Health and economic impact of surgical site infections diagnosed after hospital discharge. Emerg Infect Dis 9(2):196–203
Gastmeier P (2006) Postdischarge surveillance for surgical site infection: the continuing challenge. Infect Control Hosp Epidemiol 27(12):1287–1290
Haley RW, Culver DH, White JW, Morgan WM, Emori TG, Munn VP et al (1985) The efficacy of infection surveillance and control programs in preventing nosocomial infections in US hospitals. Am J Epidemiol 121(2):182–205
Anderson DJ, Kaye KS, Classen D, Arias KM, Podgorny K, Burstin H et al (2008) Strategies to prevent surgical site infections in acute care hospitals. Infect Control Hosp Epidemiol 29(Suppl 1):S51–S61
Anderson DJ, Podgorny K, Berrios-Torres SI, Bratzler DW, Dellinger EP, Greene L et al (2014) Strategies to prevent surgical site infections in acute care hospitals: 2014 update. Infect Control Hosp Epidemiol 35(6):605–627
Joint., Comission (2015). http://www.jointcommission.org/surgical_care_improvement_project/
Horan TC, Gaynes RP, Martone WJ, Jarvis WR, Emori TG (1992) CDC definitions of nosocomial surgical site infections, 1992: a modification of CDC definitions of surgical wound infections. Infect Control Hosp Epidemiol 13(10):606–608
Sands K, Vineyard G, Platt R (1996) Surgical site infections occurring after hospital discharge. J Infect Dis 173(4):963–970
Consensus paper on the surveillance of surgical wound infections (1992) The Society for Hospital Epidemiology of America; The Association for Practitioners in Infection Control; The Centers for Disease Control; The Surgical Infection Society. Infect Control Hosp Epidemiol 13(10):599–605
Mertz D, Whitlock R, Kokoszka AY, Smith SW, Carignan A, Rehan M et al (2016) Routine surveillance versus independent assessment by an outcome adjudication committee in assessing patients for sternal surgical site infections after cardiac surgery. Infect Control Hosp Epidemiol 37(5):600–602
Talbot TR, Bratzler DW, Carrico RM, Diekema DJ, Hayden MK, Huang SS et al (2013) Public reporting of health care-associated surveillance data: recommendations from the healthcare infection control practices advisory committee. Ann Intern Med 159(9):631–635
Reilly J, Noone A, Clift A, Cochrane L, Johnston L, Rowley DI et al (2005) A study of telephone screening and direct observation of surgical wound infections after discharge from hospital. J Bone Joint Surg Br 87(7):997–999
Whitby M, McLaws ML, Doidge S, Collopy B (2007) Post-discharge surgical site surveillance: does patient education improve reliability of diagnosis? J Hosp Infect 66(3):237–242
Seaman M, Lammers R (1991) Inability of patients to self-diagnose wound infections. J Emerg Med 9(4):215–219
Mitchell DH, Swift G, Gilbert GL (1999) Surgical wound infection surveillance: the importance of infections that develop after hospital discharge. Aust N Z J Surg 69(2):117–120
Woods RK, Dellinger EP (1998) Current guidelines for antibiotic prophylaxis of surgical wounds. Am Fam Phys 57(11):2731–2740
Holtz TH, Wenzel RP (1992) Postdischarge surveillance for nosocomial wound infection: a brief review and commentary. Am J Infect Control 20(4):206–213
Weiss CA 3rd, Statz CL, Dahms RA, Remucal MJ, Dunn DL, Beilman GJ (1999) Six years of surgical wound infection surveillance at a tertiary care center: review of the microbiologic and epidemiological aspects of 20,007 wounds. Arch Surg 134(10):1041–1048
Weinwurm D (2005) Surveillance of selected bowel surgeries for surgical site infection (SSI) rates in-hospital plus post-discharge. Am J Infect Control 33(5):e169
Kasatpibal N, Jamulitrat S, Chongsuvivatwong V (2005) Standardized incidence rates of surgical site infection: a multicenter study in Thailand. Am J Infect Control 33(10):587–594
Soleto L, Pirard M, Boelaert M, Peredo R, Vargas R, Gianella A et al (2003) Incidence of surgical-site infections and the validity of the National Nosocomial Infections Surveillance System risk index in a general surgical ward in Santa Cruz, Bolivia. Infect Control Hosp Epidemiol 24(1):26–30
Reilly J, Allardice G, Bruce J, Hill R, McCoubrey J (2006) Procedure-specific surgical site infection rates and postdischarge surveillance in Scotland. Infect Control Hosp Epidemiol 27(12):1318–1323
Cohen MJ, Benenson S (2011) Surveillance quality in reporting nosocomial bloodstream infection rates. JAMA 305(8):779–80; author reply 80
Mistiaen P, Poot E (2006) Telephone follow-up, initiated by a hospital-based health professional, for postdischarge problems in patients discharged from hospital to home. Cochrane Database Syst Rev (4):CD004510
Author information
Authors and Affiliations
Corresponding author
Additional information
Vered Richter and Matan J. Cohen have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Richter, V., Cohen, M.J., Benenson, S. et al. Patient Self-Assessment of Surgical Site Infection is Inaccurate. World J Surg 41, 1935–1942 (2017). https://doi.org/10.1007/s00268-017-3974-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-017-3974-y