Abstract
Background
While involvement of macrometastatic lymph nodes is a recognized independent predictor of an adverse course in papillary thyroid cancer (PTC) patients, the clinicopathological variables associated with disease persistence/recurrence in clinically node-negative (cN0) disease are not well defined. The indications for prophylactic central neck dissection (pCND) in this patient group remain unclear as well. We aim to investigate the risk factors associated with short- and long-term persistence/recurrence of PTC in patients with cN0 disease at presentation compared to patients with PTC and cervical lymph node involvement (N1) and the response to initial treatment in these subgroups of patients.
Methods
Data were collected retrospectively for 392 consecutive patients with PTC, 223 with cN0 disease and 169 with N1 disease, who were treated and followed at a single tertiary medical center in which pCND is not routinely performed for PTC.
Results
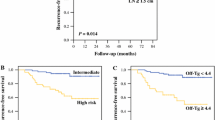
Compared to patients with N1 disease, patients with cN0 disease had significantly smaller tumors, lower rates of multifocality, and less extrathyroidal extension. Persistency rates at 1 year were 6.7 % in the cN0 group and 47 % in the N1 group, and at last follow-up, 3.6 and 33.5 %, respectively (p = 0.001 for both time points). Within the cN0 group, those with persistent disease at 1 year (n = 15) had significantly larger tumors and higher stimulated thyroglobulin. Only six had structural residual disease, four of them lymph node metastases. All patients with persistent disease were initially treated with total thyroidectomy and radioiodine. Recurrence occurred in only three patients. After 8.3 ± 3.8 years of follow-up, eight patients with cN0 had persistent disease, three of them biochemical. Higher American Joint Committee of Cancer stage and extrathyroidal extension were the only factors that predicted disease persistence at the last follow-up in this group.
Conclusions
Patients with cN0 PTC and no distant metastases are usually disease free after thyroidectomy with/without radioactive iodine and do not need further interventions. The initial staging in these patients is a valid prognostic factor for disease outcomes.

Similar content being viewed by others
References
Mazzaferri EL, Jhiang SM (1994) Long-term impact of initial surgical and medical therapy on papillary and follicular thyroid cancer. Am J Med 97:418–428
Podnos YD, Smith D, Wagman LD, Ellenhorn JD (2005) The implication of lymph node metastasis on survival on patients with well-differentiated thyroid cancer. Am Surg 71:731–734
Cooper DS, Doherty GM, Haugen BR, Kloos RT, Lee SL, Mandel SJ, Mazzaferri EL, McIver B, Pacini F, Schlumberger M, Sherman SI, Steward DL, Tuttle RM (2009) American Thyroid Association (ATA) guidelines taskforce on thyroid nodules and differentiated thyroid cancer. Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid 19:1167–1214
Lang BH, Ng SH, Lau LL, Cowling BJ, Wong KP, Wan KY (2013) A systematic review and meta-analysis of prophylactic central neck dissection on short-term locoregional recurrence in papillary thyroid carcinoma after total thyroidectomy. Thyroid 23:1087–1098. doi:10.1089/thy.2012.0608
Glover AR, Gundara JS, Norlén O, Lee JC, Sidhu SB (2013) The pros and cons of prophylactic central neck dissection in papillary thyroid carcinoma. Gland Surg 2:196–205
Viola D, Materazzi G, Valerio L, Molinaro E, Agate L, Faviana P, Seccia V, Sensi E, Romei C, Piaggi P, Torregrossa L, Sellari-Franceschini S, Basolo F, Vitti P, Elisei R, Miccoli P (2015) Prophylactic central compartment lymph node dissection in papillary thyroid carcinoma: clinical implications derived from the first prospective randomized controlled single institution study. J Clin Endocrinol Metab 100:1316–1324
Guy A, Hirsch D, Shohat T, Bachar G, Tirosh A, Robenshtok E, Shimon I, Benbassat CA (2014) Papillary thyroid cancer: factors involved in restaging N1 disease after total thyroidectomy and radioactive iodine treatment. J Clin Endocrinol Metab 99:4167–4173
DeGroot LJ, Kaplan EL, McCormick M, Straus FH (1990) Natural history, treatment, and course of papillary thyroid carcinoma. J Clin Endocrinol Metab 71:414–424
Harwood J, Clark OH, Dunphy JE (1978) Significance of lymph node metastasis in differentiated thyroid cancer. Am J Surg 136:107–112
McConahey WM, Hay ID, Woolner LB, van Heerden JA, Taylor WF (1986) Papillary thyroid cancer treated at the Mayo Clinic, 1946 through 1970: initial manifestations, pathologic findings, therapy, and outcome. Mayo Clin Proc 61:978–996
Byar DP, Green SB, Dor P, Williams ED, Colon J, van Gilse HA, Mayer M, Sylvester RJ, van Glabbeke M (1979) A prognostic index for thyroid carcinoma: a study of the E.O.R.T.C. thyroid cancer cooperative group. Eur J Cancer 15:1033–1041
Hay ID, Grant CS, Taylor WF, McConahey WM (1987) Ipsilateral lobectomy versus bilateral lobar resection in papillary thyroid carcinoma: a retrospective analysis of surgical outcome using a novel prognostic scoring system. Surgery 102:1088–1095
Hay ID, Bergstralh EJ, Goellner JR, Ebersold JR, Grant CS (1993) Predicting outcome in papillary thyroid carcinoma: development of a reliable prognostic scoring system in a cohort of 1779 patients surgically treated at one institution during 1940 through 1989. Surgery 114:1050–1058
Cady B, Rossi R (1988) An expanded view of risk-group definition in differentiated thyroid carcinoma. Surgery 104:947–953
Kukkonen ST, Haapiainen RK, Rranssila KO, Sivula AH (1990) Papillary thyroid carcinoma: the new, age-related TNM classification system in a retrospective analysis of 199 patients. World J Surg 14:837–842. doi:10.1007/BF01670533
Mazzaferri EL, Young RL (1981) Papillary thyroid carcinoma: a 10 year follow-up report of the impact of therapy in 576 patients. Am J Med 70:511–518
McHenry CR, Rosen IB, Walfish PG (1991) Prospective management of nodal metastases in differentiated thyroid cancer. Am J Surg 162:353–356
Scheumann GF, Gimm O, Wegener G, Hundeshagen H, Dralle H (1994) Prognostic significance and surgical management of locoregional lymph node metastases in papillary thyroid cancer. World J Surg 18:559–568. doi:10.1007/BF00353765
Clark OH (2011) Thyroid cancer and lymph node metastases. J Surg Oncol 103:615–618
Cranshaw IM, Carnaille B (2008) Micrometastases in thyroid cancer. An important finding? Surg Oncol 17:253–258
Wada N, Duh QY, Sugino K, Iwasaki H, Kameyama K, Mimura T, Ito K, Takami H, Takanashi Y (2003) Lymph node metastasis from 259 papillary thyroid microcarcinomas: frequency, pattern of occurrence and recurrence, and optimal strategy for neck dissection. Ann Surg 237:399–407
Wada N, Masudo K, Nakayama H, Suganuma N, Matsuzu K, Hirakawa S, Rino Y, Masuda M, Imada T (2008) Clinical outcomes in older or younger patients with papillary thyroid carcinoma: impact of lymphadenopathy and patient age. Eur J Surg Oncol 34:202–207
Bardet S, Malville E, Rame JP, Babin E, Samama G, De Raucourt D, Michels JJ, Reznik Y, Henry-Amar M (2008) Macroscopic lymph-node involvement and neck dissection predict lymph-node recurrence in papillary thyroid carcinoma. Eur J Endocrinol 158:551–560
Gyorki DE, Untch B, Tuttle RM, Shaha AR (2013) Prophylactic central neck dissection in differentiated thyroid cancer: an assessment of the evidence. Ann Surg Oncol 20:2285–2289
Zetoune T, Keutgen X, Buitrago D, Aldailami H, Shao H, Mazumdar M, Fahey TJ 3rd, Zarnegar R (2010) Prophylactic central neck dissection and local recurrence in papillary thyroid cancer: a meta-analysis. Ann Surg Oncol 17:3287–3293
Shan CX, Zhang W, Jiang DZ, Zheng XM, Liu S, Qiu M (2012) Routine central neck dissection in differentiated thyroid carcinoma: a systematic review and meta-analysis. Laryngoscope 122:797–804
Popadich A, Levin O, Lee JC, Smooke-Praw S, Ro K, Fazel M, Arora A, Tolley NS, Palazzo F, Learoyd DL, Sidhu S, Delbridge L, Sywak M, Yeh MW (2011) A multicenter cohort study of total thyroidectomy and routine central lymph node dissection for cN0 papillary thyroid cancer. Surgery 150:1048–1057
Barczyński M, Konturek A, Stopa M, Nowak W (2013) Prophylactic central neck dissection for papillary thyroid cancer. Br J Surg 100:410–418
Xing M (2005) BRAF mutation in thyroid cancer. Endocr Relat Cancer 12:245–262
Fugazzola L, Puxeddu E, Avenia N, Romei C, Cirello V, Cavaliere A, Faviana P, Mannavola D, Moretti S, Rossi S, Sculli M, Bottici V, Beck-Peccoz P, Pacini F, Pinchera A, Santeusanio F, Elisei R (2006) Correlation between B-RAFV600E mutation and clinico-pathologic parameters in papillary thyroid. Endocr Relat Cancer 13:455–464
Lee JH, Lee ES, Kim YS (2007) Clinicopathologic significance of BRAF V600E mutation in papillary carcinomas of the thyroid: a meta-analysis. Cancer 110:38–46
Xing M, Westra WH, Tufano RP, Cohen Y, Rosenbaum E, Rhoden KJ, Carson KA, Vasko V, Larin A, Tallini G, Tolaney S, Holt EH, Hui P, Umbricht CB, Basaria S, Ewertz M, Tufaro AP, Califano JA, Ringel MD, Zeiger MA, Sidransky D, Ladenson PW (2005) BRAF mutation predicts a poorer clinical prognosis for papillary thyroid cancer. J Clin Endocrinol Metab 90:6373–6379
Lassalle S, Hofman V, Ilie M, Butori C, Bozec A, Santini J, Vielh P, Hofman P (2010) Clinical impact of the detection of BRAF mutations in thyroid pathology: potential usefulness as diagnostic, prognostic and theragnostic applications. Curr Med Chem 17:1839–1850
Handkiewicz-Junak D, Czarniecka A, Jarzab B (2010) Molecular prognostic markers in papillary and follicular thyroid cancer: current status and future directions. Mol Cell Endocrinol 322:8–28
Ito Y, Yoshida H, Maruo R, Morita S, Takano T, Hirokawa M, Yabuta T, Fukushima M, Inoue H, Tomoda C, Kihara M, Uruno T, Higashiyama T, Takamura Y, Miya A, Kobayashi K, Matsuzuka F, Miyauchi A (2009) BRAF mutation in papillary thyroid carcinoma in a Japanese population: its lack of correlation with high-risk clinicopathological features and disease-free survival of patients. Endocr J 56:89–97
Niederer-Wüst SM, Jochum W, Förbs D, Brändle M, Bilz S, Clerici T, Oettli R, Müller J, Haile SR, Ess S, Stoeckli SJ, Broglie MA (2015) Impact of clinical risk scores and BRAF V600E mutation status on outcome in papillary thyroid cancer. Surgery 157:119–125
Soares P, Celestino R, Melo M, Fonseca E, Sobrinho-Simões M (2014) Prognostic biomarkers in thyroid cancer. Virchows Arch 464:333–346
Lee JW, Koo BS (2013) The prognostic implication and potential role of BRAF mutation in the decision to perform elective neck dissection for thyroid cancer. Gland Surg 2:206–211
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
The authors have nothing to disclose and no conflicts of interests.
Rights and permissions
About this article
Cite this article
Gorshtein, A., Benbassat, C., Robenshtok, E. et al. Response to Treatment is Highly Predictable in cN0 Patients with Papillary Thyroid Carcinoma. World J Surg 40, 2123–2130 (2016). https://doi.org/10.1007/s00268-016-3507-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-016-3507-0