Abstract
Background
Total thyroidectomy is a well-established surgical approach for the management of papillary thyroid cancer (PTC). However, the best surgical approach for papillary microcarcinoma is nowadays still debated. Both total thyroidectomy and simple lobectomy are used. We report the experience of a single University center in the treatment of thyroid microcarcinoma.
Methods
A retrospective analysis on all patients who underwent thyroid surgery at our institution over a 24-year period (1991–2015) was performed. Patients were grouped according to whether they received total thyroidectomy (Group 1) or lobectomy (Group 2). Follow-up was made by routine clinical and ultrasound examination. Specific outcomes such as recurrence and need for reoperation as well as complications (transient vocal cord paralysis and hypocalcemia) were analyzed.
Results
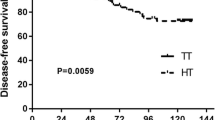
During the study period 880 patients underwent surgery for PTC. Group 1 and 2 consisted, respectively, of 756 and 124 patients. A micro PTC (<10 mm) was present in 251 and 69 specimen of Group 1 and 2. No evidence of disease recurrence in the follow-up was reported in patients with microPTC in Group 1 and in 57 patients of Group 2. In the remaining 12 patients completion thyroidectomy was carried out due to ultrasound findings of contralateral nodules (10), lymphadenopathy (1), and capsular invasion (1). Five of these patients had a contralateral papillary carcinoma on final histopathologic examination. Thus recurrence rate for patients of Group 2 was 7.3 %. Morbidity rates were, respectively, for Group 1 and 2: transient nerve palsy 81 and 5 (11 vs. 7.3 %, p = ns), transient hypoparathyroidism (Calcium <2.00 mmol/L) 137 (18.6 %) and 0 (p < 0.0001). Three of the 12 patients of Group 2 undergoing further surgery had a transient hypoparathyroidism.
Conclusions
Thyroid lobectomy is an effective surgical strategy to manage papillary microcarcinomas with low complications. Routine completion thyroidectomy is not mandatory. Appropriate selection excluding high-risk patients is of paramount importance in order to achieve the best results.

Similar content being viewed by others
References
American Cancer Society. Cancer Facts, Figures. 2014. Available at:http://www.cancer.org/acs/groups/content/@research/documents/webcontent/acspc-042151.pdf
Davies L, Welch HG (2006) Increasing incidence of thyroid cancer in the United States, 1973–2002. JAMA 295(18):2164–2167
Abdelgadir Adam M, Pura J, Goffredo P, Dinan MA, Hyslop T, Reed SD, Scheri RP, Roman SA, Sosa JA (2015) Impact of extent of surgery on survival for papillary thyroid cancer patients younger than 45 years. J Clin Endocrinol Metab 100(1):115–121. doi:10.1210/jc.2014-3039
Matsuzu K, Sugino K, Masudo K, Nagahama M, Kitagawa W, Shibuya H, Ohkuwa K, Uruno T, Suzuki A, Magoshi S, Akaishi J, Masaki C, Kawano M, Suganuma N, Rino Y, Masuda M, Kameyama K, Takami H, Ito K (2014) Thyroid lobectomy for papillary thyroid cancer: long-term follow-up study of 1088 cases. World J Surg 38(1):68–79. doi:10.1007/s00268-013-2224-1
Bilimoria KY, Bentrem DJ, Ko CY, Stewart AK, Winchester DP, Talamonti MS, Sturgeon C (2007) Extent of surgery affects survival for papillary thyroid cancer. Ann Surg 246(3):375–381 discussion 381–384
Hughes DT, Haymart MR, Miller BS, Gauger PG, Doherty GM (2011) The most commonly occurring papillary thyroid cancer in the United States is now a microcarcinoma in a patient older than 45 years. Thyroid 21(3):231–236. doi:10.1089/thy.2010.0137
Pacini F, Schlumberger M, Dralle H, Elisei R, Smit JW, Wiersinga W (2006) European Thyroid Cancer Taskforce. European consensus for the management of patients with differentiated thyroid carcinoma of the follicular epithelium. Eur J Endocrinol 154(6):787–803. No abstract available. Erratum in: Eur J Endocrinol. 2006 155(2):385
American Thyroid Association (ATA) Guidelines Taskforce on Thyroid Nodules and Differentiated Thyroid Cancer, Cooper DS, Doherty GM, Haugen BR, Kloos RT, Lee SL, Mandel SJ, Mazzaferri EL, McIver B, Pacini F, Schlumberger M, Sherman SI, Steward DL, Tuttle RM (2009) Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid. 2009 19(11):1167–1214. doi: 10.1089/thy.2009.0110. Erratum in: Thyroid. 2010 20(8):942. Hauger, Bryan R [corrected to Haugen, Bryan R]. Thyroid. 2010 20(6):674–675
Perros P, Boelaert K, Colley S, Evans C, Evans RM, Gerrard Ba G, Gilbert J, Harrison B, Johnson SJ, Giles TE, Moss L, Lewington V, Newbold K, Taylor J, Thakker RV, Watkinson J, Williams GR (2014) British Thyroid Association. Guidelines for the management of thyroid cancer. Clin Endocrinol (Oxf). 81(Suppl 1):1–122. doi: 10.1111/cen.12515 (No abstract available)
Takami H, Ito Y, Okamoto T, Onoda N, Noguchi H, Yoshida A (2014) Revisiting the guidelines issued by the Japanese Society of Thyroid Surgeons and Japan Association of Endocrine Surgeons: a gradual move towards consensus between Japanese and western practice in the management of thyroid carcinoma. World J Surg 38(8):2002–2010. doi:10.1007/s00268-014-2498-y
Kebebew E, Clark OH (2000) Differentiated thyroid cancer: “complete” rational approach. World J Surg 24(8):942–951. doi:10.1007/s002680010165 Review
Mendelsohn AH, Elashoff DA, Abemayor E (2010) St John MA. Surgery for papillary thyroid carcinoma: is lobectomy enough? Arch Otolaryngol Head Neck Surg 136(11):1055–1061. doi:10.1001/archoto.2010.181
Rosato L, Avenia N, Bernante P, De Palma M, Gulino G, Nasi PG, Pelizzo MR, Pezzullo L (2004) Complications of thyroid surgery: analysis of a multicentric study on 14,934 patients operated on in Italy over 5 years. World J Surg 28(3):271–276. doi:10.1007/s00268-003-6903-1
Adam MA, Pura J, Gu L, Dinan MA, Tyler DS, Reed SD, Scheri R, Roman SA, Sosa JA (2014) Extent of surgery for papillary thyroid cancer is not associated with survival: an analysis of 61,775 patients. Ann Surg 260(4):601–605. doi:10.1097/SLA.0000000000000925 (discussion 605–607)
Verburg FA, Mäder U, Tanase K, Thies ED, Diessl S, Buck AK, Luster M, Reiners C (2013) Life expectancy is reduced in differentiated thyroid cancer patients ≥45 years old with extensive local tumor invasion, lateral lymph node, or distant metastases at diagnosis and normal in all other DTC patients. J Clin Endocrinol Metab 98(1):172–180. doi:10.1210/jc.2012-2458
Hay ID, Thompson GB, Grant CS, Bergstralh EJ, Dvorak CE, Gorman CA, Maurer MS, McIver B, Mullan BP, Oberg AL, Powell CC, van Heerden JA, Goellner JR (2002) Papillary thyroid carcinoma managed at the Mayo Clinic during six decades (1940–1999): temporal trends in initial therapy and long-term outcome in 2444 consecutively treated patients. World J Surg 26(8):879–885. doi:10.1007/s00268-002-6612-1
Udelsman R, Shaha A (2005) Is total thyroidectomy the best possible surgical management for well-differentiated thyroid carcinoma? Lancet Oncol 6:529–531
Wanebo H, Coburn M, Teates D, Cole B (1998) Total thyroidectomy does not enhance disease control or survival even in high-risk patients with differentiated thyroid cancer. Ann Surg 227(6):912–921
Haigh PI, Urbach DR, Rotstein LE (2005) Extent of thyroidectomy is not a major determinant of survival in low- or high-risk papillary thyroid cancer. Ann Surg Oncol 12(1):81–89
Nixon IJ, Ganly I, Patel SG, Palmer FL, Whitcher MM, Tuttle RM, Shaha A, Shah JP (2012) Thyroid lobectomy for treatment of well differentiated intrathyroid malignancy. Surgery. 151(4):571–579. doi:10.1016/j.surg.2011.08.016
Grant CS (2015) Recurrence of papillary thyroid cancer after optimized surgery. Gland Surg 4(1):52–62. doi:10.3978/j.issn.2227-684X.2014.12.06 Review
Pacini F, Schlumberger M, Harmer C, Berg GG, Cohen O, Duntas L, Jamar F, Jarzab B, Limbert E, Lind P, Reiners C (2005) Sanchez Franco F, Smit J, Wiersinga W. Post-surgical use of radioiodine (131I) in patients with papillary and follicular thyroid cancer and the issue of remnant ablation: a consensus report. Eur J Endocrinol 153(5):651–659 Review
Schlumberger M, Catargi B, Borget I, Deandreis D, Zerdoud S, Bridji B, Bardet S, Leenhardt L, Bastie D, Schvartz C, Vera P, Morel O, Benisvy D, Bournaud C, Bonichon F, Dejax C, Toubert ME, Leboulleux S, Ricard M, Benhamou E (2012) Tumeurs de la Thyroïde Refractaires Network for the Essai Stimulation Ablation Equivalence Trial. Strategies of radioiodine ablation in patients with low-risk thyroid cancer. N Engl J Med 366(18):1663–1673. doi:10.1056/NEJMoa1108586
Iyer NG, Morris LG, Tuttle RM, Shaha AR, Ganly I (2011) Rising incidence of second cancers in patients with low-risk (T1N0) thyroid cancer who receive radioactive iodine therapy. Cancer 117(19):4439–4446. doi:10.1002/cncr.26070
Ito Y, Uruno T, Nakano K, Takamura Y, Miya A, Kobayashi K, Yokozawa T, Matsuzuka F, Kuma S, Kuma K, Miyauchi A (2003) An observation trial without surgical treatment in patients with papillary microcarcinoma of the thyroid. Thyroid. 13(4):381–387
Ito Y, Miyauchi A, Inoue H, Fukushima M, Kihara M, Higashiyama T, Tomoda C, Takamura Y, Kobayashi K, Miya A (2010) An observational trial for papillary thyroid microcarcinoma in Japanese patients. World J Surg 34(1):28–35. doi:10.1007/s00268-009-0303-0
Hay ID, Hutchinson ME, Gonzalez-Losada T, McIver B, Reinalda ME, Grant CS, Thompson GB, Sebo TJ, Goellner JR (2008) Papillary thyroid microcarcinoma: a study of 900 cases observed in a 60-year period. Surgery 144(6):980–987. doi:10.1016/j.surg.2008.08.035 discussion 987–988
Baudin E, Travagli JP, Ropers J, Mancusi F, Bruno-Bossio G, Caillou B, Cailleux AF, Lumbroso JD, Parmentier C, Schlumberger M (1998) Microcarcinoma of the thyroid gland: the Gustave–Roussy Institute experience. Cancer 83(3):553–559
Roti E, DegliUberti EC, Bondanelli M, Braverman LE (2008) Thyroid papillary microcarcinoma: a descriptive and meta-analysis study. Eur J Endocrinol 159(6):659–673. doi:10.1530/EJE-07-0896 Review
Hauch A, Al-Qurayshi Z, Randolph G, Kandil E (2014) Total thyroidectomy is associated with increased risk of complications for low- and high-volume surgeons. Ann Surg Oncol 21(12):3844–3852. doi:10.1245/s10434-014-3846-8
Macedo FI, Mittal VK (2015) Total thyroidectomy versus lobectomy as initial operation for small unilateral papillary thyroid carcinoma: a meta-analysis. Surg Oncol. doi:10.1016/j.suronc.2015.04.005
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
The authors have nothing to disclose.
Additional information
Paper Accepted at the IAES 2015 meeting in Bangkok, 23rd–27th August 2015.
Rights and permissions
About this article
Cite this article
Donatini, G., Castagnet, M., Desurmont, T. et al. Partial Thyroidectomy for Papillary Thyroid Microcarcinoma: Is Completion Total Thyroidectomy Indicated?. World J Surg 40, 510–515 (2016). https://doi.org/10.1007/s00268-015-3327-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-015-3327-7