Abstract
Background
Patients with Cushing’s Syndrome (CS) and Conn’s Syndrome with bilateral adrenal masses pose a dilemma. Uptake of 18F-FDG by hyperfunctioning adrenal glands has not been previously reported and may help lateralize. The aim was to determine if 18F-FDG PET/CT scan could identify hyperfunctioning adrenal masses and determine a biological basis for uptake.
Methods
Patients with nonfunctional adenomas (n = 9), CS (n = 11), and Conn’s syndrome (n = 4) underwent an 18F-FDG PET/CT scan with a volume of interest circumscribing each mass to obtain a maximal standardized uptake value (SUVmax). Thirty-two adrenal masses were analyzed. Genome-wide expression data from an independent cohort were analyzed in nonfunctioning adenomas (n = 20), Conn’s syndrome (n = 29), and CS (n = 24) focusing on GLUT genes. For genes differentially expressed, immunohistochemistry was performed on tissue samples.
Results
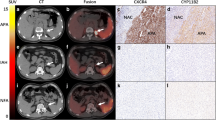
Cortisol-secreting masses (n = 16) had a higher average SUVmax of 5.9 compared to nonfunctioning masses (n = 11, average SUVmax 4.2) and aldosterone-hypersecreting masses (n = 5, average SUVmax 3.2) (p = 0.007). SUVmax cut-off of 5.33 had 50.0 % sensitivity and 81.8 % specificity in localizing a cortisol-secreting mass. GLUT3 expression was 2.19-fold higher in patients with CS compared to patients with nonfunctioning adenomas (p = 0.003) and 2.16-fold higher in patients with CS compared to Conn’s syndrome (p = 0.006). GLUT3 immunohistochemistry showed 2.2-fold higher staining in CS tumor samples compared to nonfunctioning adenomas.
Conclusions
Differential 18F-FDG PET/CT uptake was observed in patients with nonfunctioning, aldosterone-hypersecreting, and cortisol-secreting masses. GLUT3 overexpression in cortisol-secreting tumor likely accounts for the differential uptake. Future larger cohort studies will need to be conducted to determine if 18F-FDG PET/CT uptake can lateralize cortisol-secreting adrenal masses in patients with bilateral adrenal masses.



Similar content being viewed by others
References
Guaraldi F, Salvatori R (2012) Cushing syndrome: maybe not so uncommon of an endocrine disease. J Am Board Fam Med 25:199–208
Ganguly A (1998) Primary aldosteronism. N Engl J Med 339:1828–1834
Funder JW, Carey RM, Fardella C et al (2008) Case detection, diagnosis, and treatment of patients with primary aldosteronism: an endocrine society clinical practice guideline. J Clin Endocrinol Metab 93:3266–3281
Kasperlik-Zaluska AA, Slowinska-Srzednicka J, Roslonowska E et al (2010) Bilateral, incidentally found adrenal tumours—results of observation of 1790 patients registered at a single endocrinological centre. Endokrynol Pol 61:69–73
Kempers MJ, Lenders JW, van Outheusden L et al (2009) Systematic review: diagnostic procedures to differentiate unilateral from bilateral adrenal abnormality in primary aldosteronism. Ann Intern Med 151:329–337
Young WF Jr, du Plessis H, Thompson GB et al (2008) The clinical conundrum of corticotropin-independent autonomous cortisol secretion in patients with bilateral adrenal masses. World J Surg 32:856–862. doi:10.1007/s00268-007-9332-8
Naji M, Hodolic M, El-Refai S et al (2010) Endocrine tumors: the evolving role of positron emission tomography in diagnosis and management. J Endocrinol Invest 33:54–60
Groussin L, Bonardel G, Silvera S et al (2009) 18F-Fluorodeoxyglucose positron emission tomography for the diagnosis of adrenocortical tumors: a prospective study in 77 operated patients. J Clin Endocrinol Metab 94:1713–1722
Kaira K, Okumura T, Ohde Y et al (2011) Correlation between 18F-FDG uptake on PET and molecular biology in metastatic pulmonary tumors. J Nucl Med 52:705–711
Charnley N, Airley R, Du Plessis D et al (2008) No relationship between 18F-fluorodeoxyglucose positron emission tomography and expression of Glut-1 and -3 and hexokinase I and II in high-grade glioma. Oncol Rep 20:537–542
Park SG, Lee JH, Lee WA et al (2012) Biologic correlation between glucose transporters, hexokinase-II, Ki-67 and FDG uptake in malignant melanoma. Nucl Med Biol 39:1167–1172
Fernandez-Ranvier GG, Weng J, Yeh RF et al (2008) Identification of biomarkers of adrenocortical carcinoma using genomewide gene expression profiling. Arch Surg 143:841–846
Bolstad BM, Irizarry RA, Astrand M et al (2003) A comparison of normalization methods for high density oligonucleotide array data based on variance and bias. Bioinformatics 19:185–193
Benjamini Y, Drai D, Elmer G et al (2001) Controlling the false discovery rate in behavior genetics research. Behav Brain Res 125:279–284
Vassiliadi DA, Ntali G, Vicha E et al (2011) High prevalence of subclinical hypercortisolism in patients with bilateral adrenal incidentalomas: a challenge to management. Clin Endocrinol 74:438–444
Yu KC, Alexander HR, Ziessman HA et al (1995) Role of preoperative iodocholesterol scintiscanning in patients undergoing adrenalectomy for Cushing’s syndrome. Surgery 118:981–987
Reincke M (2000) Subclinical Cushing’s syndrome. Endocrinol Metab Clin N Am 29:43–56
Chiodini I (2011) Clinical review: diagnosis and treatment of subclinical hypercortisolism. J Clin Endocrinol Metab 96:1223–1236
Young WF Jr (2000) Management approaches to adrenal incidentalomas. A view from Rochester, Minnesota. Endocrinol Metab Clin N Am 29:159–185
Shimzu Y, Matsui S, Harada J (2003) Evaluation of micro-organic pollution in lake sediments: application to Akanoi Bay Lake Biwa, Japan. Environ Technol 24:889–896
Meinardi JR, Wolffenbuttel BH (2007) Dullaart RP cyclic Cushing’s syndrome: a clinical challenge. Eur J Endocrinol 157:245–254
Nieman LK, Biller BM, Findling JW et al (2008) The diagnosis of Cushing’s syndrome: an endocrine society clinical practice guideline. J Clin Endocrinol Metab 93:1154–1526
Financial support
This research was supported by the intramural research program of the Center for Cancer Research, National Cancer Institute, National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Patel, D., Gara, S.K., Ellis, R.J. et al. FDG PET/CT Scan and Functional Adrenal Tumors: A Pilot Study for Lateralization. World J Surg 40, 683–689 (2016). https://doi.org/10.1007/s00268-015-3242-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-015-3242-y