Abstract
Introduction
Surgical resection of oesophageal cancer is a major procedure with potential for significant morbidity and mortality. Patient selection can be challenging, as operative benefit must be balanced against risk and impact on quality of life. This study defines modern trends in patient selection, and evaluates the impact of age, stage, and comorbidities on complications and survival following oesophagectomy, in a tertiary Australian experience.
Methods
Data were compiled across two 15-year operative eras (‘Era 1’: 1981–1995; and ‘Era 2’: 1996–2010), with patients followed minimum 3 years. A total of 180 unselected records were analysed (powered for a relative hazard ratio of 0.5). Analyses defined patient selection trends, and for Era 2, the impact of age, comorbidities (Charlson score), and disease (T/N stage) on complications (Clavien-Dindo grade) and survival (Kaplan–Meier). A further sub-analysis was conducted with data divided into three 10-year periods.
Results
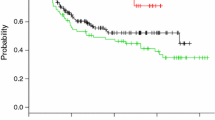
The age of operated patients increased from Era 1 to 2 (mean + 5 years; P < 0.001), but survival and complication rates were unchanged, including in patients ≥ 75 years (P > 0.5). In Era 2, reflecting recent practice, survival duration matched T/N stage (P < 0.001) but was independent of age at surgery (P = 0.56) and comorbidity score (P = 0.78). However, grade of worst post-operative complication, including death (rate: 3.8 %), was correlated with both age (P < 0.01) and comorbidity score (P < 0.01).
Discussion
Older patients are now undergoing oesophagectomy. However, if they are selected appropriately, then older patients and those with comorbidities can expect similar stage-matched survival outcomes to younger fitter patients, despite their higher operative risk. Poor outcomes persist in patients with locally advanced disease, and selection in this group should prioritise quality of life.



Similar content being viewed by others
References
Stavrou E, Baker D, McElroy H, Bishop J (2009) Oesophageal cancer in New South Wales. Cancer Institute NSW, Sydney
Raymond D (2012) Complications of esophagectomy. Surg Clin North Am 92:1299–1313
Bollschweiler E, Schroder W, Holscher AH, Siewert JR (2000) Preoperative risk analysis in patients with adenocarcinoma or squamous cell carcinoma of the oesophagus. Br J Surg 87:1106–1110
Sanghera SS, Nurkin SJ, Demmy TL (2012) Quality of life after an esophagectomy. Surg Clin North Am 92:1315–1335
Blazeby JM, Farndon JR, Donovan J, Alderson D (2000) A prospective longitudinal study examining the quality of life of patients with esophageal carcinoma. Cancer 88:1781–1787
Sobin LH, Gospodarowicz MK, Wittekind C (eds) (2010) TNM classification of malignant tumours, 7th edn. Blackwell Publishing Ltd, Oxford
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Clavien PA, Barkun J, de Oliveira ML et al (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196
Chang AC, Ji H, Birkmeyer NJ, Orringer MB, Birkmeyer JD (2008) Outcomes after transhiatal and transthoracic esophagectomy for cancer. Ann Thorac Surg 85:424–429
van Blankenstein M, Looman CW, Siersema PD, Kuipers EJ, Coebergh JW (2007) Trends in the incidence of adenocarcinoma of the oesophagus and cardia in the Netherlands 1989–2003. Br J Cancer 96:1767–1771
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D (2011) Global cancer statistics. CA Cancer J Clin 61:69–90
Atkins BZ, Shah AS, Hutcheson KA et al (2004) Reducing hospital morbidity and mortality following oesophagectomy. Ann Thorac Surg 78:1170–1176
Abunasra H, Lewis S, Beggs L, Duffy J, Beggs D, Morgan E (2005) Predictors of operative death after oesophagectomy for carcinoma. Br J Surg 92:1029–1033
Law S, Wong KH, Kwok KF, Chu KM, Wong J (2004) Predictive factors for postoperative pulmonary complications and mortality after esophagectomy for cancer. Ann Surg 240:791–800
McLoughlin JM, Lewis JM, Meredith KL (2013) The impact of age on morbidity and mortality following esophagectomy for esophageal cancer. Cancer Control 20:144–150
Internullo E, Moons J, Nafteux P et al (2008) Outcome after esophagectomy for cancer of the esophagus and GEJ in patients aged over 75 years. Eur J Cardiothorac Surg 33:1096–1104
Poon RT, Law SY, Chu KM, Branicki FJ, Wong J (1998) Esophagectomy for carcinoma of the esophagus in the elderly: results of current surgical management. Ann Surg 227:357–364
Cijs TM, Verhoef C, Steyerberg EW et al (2010) Outcome of esophagectomy for cancer in elderly patients. Ann Thorac Surg 90:900–907
Hashimi S, Smith M (2012) Medical evaluation of patients preparing for an esophagectomy. Surg Clin North Am 92:1127–1133
Markar SR, Low DE (2013) Physiology, not chronology, dictates outcomes after esophagectomy for esophageal cancer: outcomes in patients 80 years and older. Ann Surg Oncol 20:1020–1026
Steyerberg EW, Neville BA, Koppert LB et al (2006) Surgical mortality in patients with esophageal cancer: development and validation of a simple risk score. J Clin Oncol 24:4277–4284
Bosch DJ, Pultrum BB, de Bock GH, Oosterhuis JK, Rodgers MG, Plukker JT (2011) Comparison of different risk-adjustment models in assessing short-term surgical outcome after transthoracic esophagectomy in patients with esophageal cancer. Am J Surg 202:303–309
Ra J, Paulson EC, Kucharczuk J et al (2008) Postoperative mortality after esophagectomy for cancer: development of a preoperative risk prediction model. Ann Surg Oncol 15:1577–1584
Finlayson E, Fan Z, Birkmeyer JD (2007) Outcomes in octogenarians undergoing high-risk cancer operation: a national study. J Am Coll Surg 205:729–734
Metzger R, Bollschweiler E, Vallbohmer D, Maish M, DeMeester TR, Holscher AH (2004) High volume centers for esophagectomy: what is the number needed to achieve low postoperative mortality? Dis Esophagus 17:310–314
Pal N, Axisa B, Yusof S et al (2008) Volume and outcome for major upper GI surgery in England. J Gastrointest Surg 12:353–357
Sgourakis G, Gockel I, Radtke A et al (2010) Minimally invasive versus open esophagectomy: meta-analysis of outcomes. Dig Dis Sci 55:3031–3040
Dantoc MM, Cox MR, Eslick GD (2012) Does minimally invasive esophagectomy (MIE) provide for comparable oncologic outcomes to open techniques? A systematic review. J Gastrointest Surg 16:486–494
Hulscher JB, van Sandick JW, DB AG, Wijnhoven BPL, Tijssen JGP, Fockens P (2002) Extended transthoracic resection compared with limited transhiatal resection for adenocarcinoma of the esophagus. NEJM 347:1662–1669
Rentz J, Bull D, Harpole D et al (2003) Transthoracic versus transhiatal esophagectomy: a prospective study of 945 patients. J Thorac Cardiovasc Surg 125:1114–1120
Abrams JA, Buono DL, Strauss J, McBride RB, Hershman DL, Neugut AI (2009) Esophagectomy compared with chemoradiation for early stage esophageal cancer in the elderly. Cancer 115:4924–4933
Davies L, Lewis WG, Arnold DT et al (2010) Prognostic significance of age in the radical treatment of oesophageal cancer with surgery or chemoradiotherapy: a prospective observational cohort study. Clin Oncol 22:578–585
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
O’Grady, G., Hameed, A.M., Pang, T.C. et al. Patient Selection for Oesophagectomy: Impact of Age and Comorbidities on Outcome. World J Surg 39, 1994–1999 (2015). https://doi.org/10.1007/s00268-015-3072-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-015-3072-y