Abstract
Background
Sarcopenia describes a loss of muscle mass and resultant decrease in strength, mobility, and function that can be quantified by CT. We hypothesized that sarcopenia and related frailty characteristics are related to discharge disposition after blunt traumatic injury in the elderly.
Methods
We reviewed charts of 252 elderly blunt trauma patients who underwent abdominal CT prior to hospital admission. Data for thirteen frailty characteristics were abstracted. Sarcopenia was measured by obtaining skeletal muscle cross-sectional area (CSA) from each patient’s psoas major muscle using Slice-O-Matic® software. Dispositions were grouped as dependent and independent based on discharge location. χ 2, Fisher’s exact, and logistic regression were used to determine factors associated with discharge dependence.
Results
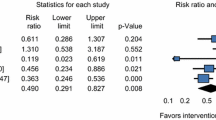
Mean age 76 years, 49 % male, median ISS 9.0 (IQR = 8.0–17.0). Discharge destination was independent in 61.5 %, dependent in 29 %, and 9.5 % of patients died. Each 1 cm2 increase in psoas muscle CSA was associated with a 20 % decrease in dependent living (p < 0.0001). Gender, weakness, hospital complication, and cognitive impairment were also associated with disposition; ISS was not (p = 0.4754).
Conclusions
Lower psoas major muscle CSA is related to discharge destination in elderly trauma patients and can be obtained from the admission CT. Lower psoas muscle CSA is related to loss of independence upon discharge in the elderly. The early availability of this variable during the hospitalization of elderly trauma patients may aid in discharge planning and the transition to dependent living.
Similar content being viewed by others
References
Fielding RA, Vellas B, Evans WJ et al (2011) Sarcopenia: an undiagnosed condition in older adults, current consensus definition, prevalence, etiology, and consequences. J Am Med Dir Assoc 12(4):249–256
Cruz-Jentoft A, Landib F, Topinkova E et al (2010) Understanding sarcopenia as a geriatric syndrome. Curr Opin Clin Nutr Metab Care 13:1–7
Goodpaster B, Carlson C, Visser M et al (2001) Attenuation of skeletal muscle and strength in the elderly: the health ABC study. J Appl Physiol 90(6):2157–2165
Lang T, Streeper T, Cawthon P et al (2010) Sarcopenia: etiology, clinical consequences, intervention, and assessment. Osteoporosis Int 210(4):543–559
Taaffe DR, Henwood TR, Nalls MA et al (2009) Alterations in muscle attenuation following detraining and retraining in resistance-trained older adults. Gerontology 55(2):217–223
Visser M, Goodpaster B, Kritchevsky S et al (2005) Muscle mass, muscle strength, and muscle fat infiltration as predictors of incident mobility limitations in well-functioning older persons. J Gerontol 60(3):324–333
Prado C, Birdsell L, Baracos V (2009) The emerging role of computerized tomography in assessing cancer cachexia. Current Opinion in Supportive and Palliative Care 3:269–275
Stevens-Simon C, Thureen P, Stamm E et al (2001) A comparison of four techniques for measuring central adiposity in postpartum adolescents. J Matern Fetal Med 10(3):209–213
Mourtzakis M, Prado C, Lieffers J et al (2008) A practical and precise approach to quantification of body composition in cancer patients using computed tomography images acquired during routine care. Appl Physiol Nutr Metab 33:997–1006
Cooper C, Dere W, Evans W et al (2012) Frailty and sarcopenia: definitions and outcome parameters. Osteoporosis Int 23:1839–1848
Studenski S (2013) Evidence-based criteria for sarcopenia with clinically important weakness. Semin Arthritis Rheum 42:447–449
Broos P, D’Hoorel A, Vanderschot P et al (1993) Multiple trauma in elderly patients. Factors influencing outcome: importance of aggressive care. Injury 24:365–368
Hsia R, Wang E, Saynina O et al (2011) Factors associated with trauma center use for elderly patients with trauma. Arch Surg 146:585–592
Perdue P, Watts D, Kaufmann C et al (1998) Differences in mortality between elderly and younger adult trauma patients: geriatric status increases risk of delayed death. J Trauma 45:805–810
Robinson T, Wallace J, Wu D et al (2011) Accumulated frailty characteristics predict postoperative discharge institutionalization in the geriatric patient. J Am Coll Surg 213:37–42
Lang T, Cauley J, Tylavsky F et al (2010) Computed tomographic measurements of thigh muscle cross-sectional area and attenuation coefficient predict hip fracture: the health, aging, and body composition study. J Bone Miner Res 25:513–519
Morely J et al (2012) Sarcopenia in the Elderly. Fam Pract 29:144–148
Ruiz M, Cefalu C, Reske T (2012) Frailty syndrome in geriatric medicine. Am J Med Sci 5:395–398
Koopman R (2011) Dietary protein and exercise training in ageing. Proc Nutr Soc 70:104–113
Nair KS (1995) Muscle protein turnover: methodological issues and the effect of aging. J Gerontol A Biol Sci Med Sci 50:107–112
Houston DK, Nicklas BJ, Ding J et al (2008) Dietary protein intake is associated with lean mass change in older, community- dwelling adults: the health, aging, and body composition (Health ABC) study. Am J Clin Nutr 87:150–155
Morris MS, Jacques PF (2013) British Journal of Nutrition. Total protein, animal protein and physical activity in relation to muscle mass in middle-aged and older Americans 109:1294–1303
Robinson T, Wu D, Pointer L et al (2013) Simple frailty score predicts postoperative complications across surgical specialties. Am J Surg 206(4):544–550
Kane RL (2011) Finding the right level of post-hospital care: “We didn’t realize there was any other option for him”. JAMA 305(3):284–293
Acknowledgments
Funding for this project was supported in part by Centers for Disease Control and Prevention Grant R49/CE001175 and in part by the National Institute on Aging Training Grant T35 AG029793-05. Imaging Software was funded through the MCW Research Affairs Committee Grant.
Conflict of interest
There are no real or potential conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fairchild, B., Webb, T.P., Xiang, Q. et al. Sarcopenia and Frailty in Elderly Trauma Patients. World J Surg 39, 373–379 (2015). https://doi.org/10.1007/s00268-014-2785-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-014-2785-7