Abstract
Background
Operative notes are the gold standard for detecting adverse events and near misses and form the basis for scientific research. In order to guarantee safe patient care, operative notes must be objective, complete, and accurate. This study explores the current routine of note writing for laparoscopic cholecystectomy (LC) and the differences between the notes of attendings and residents.
Methods
Attendings and residents were sent a DVD with footage of three LCs and were asked to “write” the corresponding notes and to complete a questionnaire. Dictation tapes were transcribed and items in the notes were analyzed for each procedure (“item described” or “item not described”). Fisher’s exact tests were performed using SPSS 16.0 for Mac.
Results
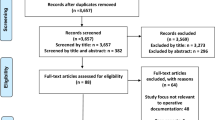
Thirteen sets of typewritten notes and 10 dictation tapes were returned. The results of the questionnaire showed that 16 of the 23 sets of notes were dictated. Eight participants found the current system for generating notes inadequate. 14 items (31 %) were included more often in the attendings’ notes and 25 items (56 %) were included more often in the residents’ notes. Overall, residents significantly more often described the location of the epigastric trocar (P = 0.018), the size of both working trocars (P = 0.019), the opening of the peritoneal envelope (P = 0.002), Critical View of Safety reached (P = 0.002), and the location for removing the gallbladder (P = 0.019). With the exception of “gallbladder perforation” (20 of 21 notes), complications were underreported.
Conclusions
In this study residents described more items than attendings. All notes lacked information concerning complications in the procedure, which makes the notes subjective and incomplete. A procedure-specific template or black-box-based operative notes based on established guidelines could improve the quality of the notes of both attendings and residents.


Similar content being viewed by others
References
Parikh JA, Yermilov I, Jain S et al (2007) How much do standardized forms improve the documentation of quality of care? J Surg Res 143:158–163
Menzin AW, Spitzer M (2003) Teaching operative dictation. A survey of obstetrics/gynecology residency program directors. J Reprod Med 48:850–852
Eichholz AC, Van Voorhis BJ, Sorosky JI et al (2004) Operative note dictation: should it be taught routinely in residency programs? Obstet Gynecol 103:342–346
Lefter LP, Walker SR, Dewhurst F et al (2008) An audit of operative notes: facts and ways to improve. ANZ J Surg 78:800–802
Cohen MM, Ammon AA (1998) A solution to the problem of undictated operative reports by residents. Am J Surg 176:475–480
Gillman LM, Vergis A, Hardy K et al (2010) Resident training and the dictated operative report: a national perspective. Can J Surg 53:246–250
Gillman LM, Vergis A, Park J et al (2010) Structured operative reporting: a randomized trial using dictation templates to improve operative reporting. Am J Surg 199:846–850
Porterfield JR Jr, Altom LK, Graham LA et al (2011) Descriptive operative reports: teaching, learning, and milestones to safe surgery. J Surg Educ 68:452–458
Scherer R, Zhu Q, Langenberg P et al (2003) Comparison of information obtained by operative note abstraction with that recorded on a standardized data collection form. Surgery 133:324–330
Edhemovic I, Temple WJ, de Gara CJ et al (2004) The computer synoptic operative report–a leap forward in the science of surgery. Ann Surg Oncol 11:941–947
Novitsky YW, Sing RF, Kercher KW et al (2005) Prospective, blinded evaluation of accuracy of operative reports dictated by surgical residents. Am Surg 71:627–631 discussion 631–622
Rafiq A, Zhao X, Tamariz F et al (2007) A user-centred framework for an electronic multimedia surgical information system in operating rooms. J Inf Technol Healthc 5:5–17
Mack LA, Bathe OF, Hebert MA et al (2009) Opening the black box of cancer surgery quality: WebSMR and the Alberta experience. J Surg Oncol 99:525–530
Baigrie RJ, Dowling BL, Birch D et al (1994) An audit of the quality of operation notes in two district general hospitals. Are we following Royal College guidelines? Ann R Coll Surg Engl 76:8–10
Rogers A, Bunting M, Atherstone A (2008) The quality of operative notes at a general surgery unit. S Afr Med J 98:726–728
Osborn GD, Pike H, Smith M et al (2005) Quality of clinical case note entries: how good are we at achieving set standards? Ann R Coll Surg Engl 87:458–460
Borchert D, Harshen R, Kemps M et al (2006) Operative notes teaching: re-discovery of an effective teaching tool in surgical training. Internet J Surg 8:1–11
Moore RA (2000) The dictated operative note: important but is it being taught? J Am Coll Surg 190:639–640
Zehetner J, Shamiyeh A, Wayand W (2007) Lost gallstones in laparoscopic cholecystectomy: all possible complications. Am J Surg 193:73–78
Lien HH, Huang CC, Liu JS et al (2007) System approach to prevent common bile duct injury and enhance performance of laparoscopic cholecystectomy. Surg Laparosc Endosc Percutan Tech 17:164–170
Dutch Society of Surgery (2006) Advice: guideline laparoscopic cholecystectomy. http://www.artsennet.nl/Richtlijnen/Richtlijn/70715/Laparoscopische-Cholecystectomie.htm. Accessed 16 April 2013
Strasberg SM (2002) Avoidance of biliary injury during laparoscopic cholecystectomy. J Hepatobiliary Pancreat Surg 9:543–547
Reason J (2000) Human error: models and management. BMJ 320:768–770
Leape LL (1997) A systems analysis approach to medical error. J Eval Clin Pract 3:213–222
Stewart L, Hunter JG, Wetter A et al (2010) Operative reports: form and function. Arch Surg 145:865–871
Mackenzie CF, Xiao Y, Hu FM et al (2007) Video as a tool for improving tracheal intubation tasks for emergency medical and trauma care. Ann Emerg Med 50:436–442, 442 e431
de Reuver PR, Dijkgraaf MG, Gevers SK et al (2008) Poor agreement among expert witnesses in bile duct injury malpractice litigation: an expert panel survey. Ann Surg 248:815–820
Gur I, Gur D, Recabaren JA (2012) The computerized synoptic operative report: a novel tool in surgical residency education. Arch Surg 147:71–74
Wauben LS, Goossens RH, van Eijk DJ et al (2008) Evaluation of protocol uniformity concerning laparoscopic cholecystectomy in the Netherlands. World J Surg 32:613–620. doi:10.1007/s00268-007-9323-9
Kuwada T (2005) Highlights of The Society of American Gastrointestinal and Endoscopic Surgeons Annual Meeting, Ft. Lauderdale, FL, April 13–16, 2005. http://www.medscape.com/viewarticle/506432. Accessed 16 April 2013
Neugebauer EAM, Sauerland S, Fingerhut A et al (2006) EAES guidelines for endoscopic surgery. Springer, Berlin
The Joint Commission (2008) Operative Reports. http://www.jointcommission.org/standards_information/jcfaqdetails.aspx?StandardsFaqId=215&ProgramId=47. Accessed 16 April 2013
The Royal College of Surgeons of England (2008) Good Surgical Practice. http://www.rcseng.ac.uk/publications/docs/good-surgical-practice-1. Accessed 16 April 2013
Vergis A, Gillman L, Minor S et al (2008) Structured assessment format for evaluating operative reports in general surgery. Am J Surg 195:24–29
Guerlain S, Adams RB, Turrentine FB et al (2005) Assessing team performance in the operating room: development and use of a “black-box” recorder and other tools for the intraoperative environment. J Am Coll Surg 200:29–37
Gale EA (2004) The Hawthorne studies—a fable for our times? QJM 97:439–449
Acknowledgments
The authors thank the participating attendings and residents for taking part in the study.
Conflict of interest
The authors have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wauben, L.S.G.L., Goossens, R.H.M. & Lange, J.F. Differences Between Attendings’ and Residents’ Operative Notes for Laparoscopic Cholecystectomy. World J Surg 37, 1841–1850 (2013). https://doi.org/10.1007/s00268-013-2050-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-013-2050-5