Abstract
Background
Virtual reality (VR) simulators and Web-based instructional videos are valuable supplemental training resources in surgical programs, but it is unclear how to optimally integrate them into minimally invasive surgical training.
Methods
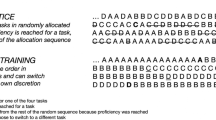
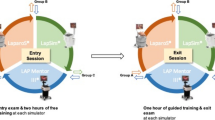
Medical students were randomized to proficiency-based training on VR laparoscopy and endoscopy simulators by two different methods: proctored training (automated simulator feedback plus human expert feedback) or independent training (simulator feedback alone). After achieving simulator proficiency, trainees performed a series of laparoscopic and endoscopic tasks in a live porcine model. Prior to their entry into the animal lab, all trainees watched an instructional video of the procedure and were randomly assigned to either observe or not observe the actual procedure before performing it themselves. The joint effects of VR training method and procedure observation on time to successful task completion were evaluated with Cox regression models.
Results
Thirty-two students (16 proctored, 16 independent) completed VR training. Cox regression modeling with adjustment for relevant covariates demonstrated no significant difference in the likelihood of successful task completion for independent versus proctored training [Hazard Ratio (HR) 1.28; 95% Confidence Interval (CI) 0.96–1.72; p = 0.09]. Trainees who observed the actual procedure were more likely to be successful than those who watched the instructional video alone (HR 1.47; 95% CI 1.09–1.98; p = 0.01).
Conclusions
Proctored VR training is no more effective than independent training with respect to surgical performance. Therefore, time-consuming human expert feedback during VR training may be unnecessary. Instructional videos, while useful, may not be adequate substitutes for actual observation when trainees are learning minimally invasive surgical procedures.


Similar content being viewed by others
References
Canes D, Desai MM, Aron M et al (2008) Transumbilical single-port surgery: evolution and current status. Eur Urol 54:1020–1029
Pearl JP, Ponsky JL (2008) Natural orifice translumenal endoscopic surgery: a critical review. J Gastrointest Surg 12:1293–1300
Wu C, Prachand VN (2008) Reverse NOTES: a hybrid technique of laparoscopic and endoscopic retrieval of an ingested foreign body. JSLS 12:395–398
Gorman PJ, Meier AH, Rawn C et al (2000) The future of medical education is no longer blood and guts, it is bits and bytes. Am J Surg 180:353–356
Rehrig ST, Powers K, Jones DB (2008) Integrating simulation in surgery as a teaching tool and credentialing standard. J Gastrointest Surg 12:222–233
Scott DJ, Cendan JC, Pugh CM et al (2008) The changing face of surgical education: simulation as the new paradigm. J Surg Res 147:189–193
Ahlberg G, Hultcrantz R, Jaramillo E et al (2005) Virtual reality colonoscopy simulation: a compulsory practice for the future colonoscopist? Endoscopy 37:1198–1204
Gallagher AG, Ritter EM, Champion H et al (2005) Virtual reality simulation for the operating room: proficiency-based training as a paradigm shift in surgical skills training. Ann Surg 241:364–372
Gurusamy KS, Aggarwal R, Palanivelu L et al (2009) Virtual reality training for surgical trainees in laparoscopic surgery. Cochrane Database Syst Rev (1) Art. No.: CD006575. doi: 10.1002/14651858.CD006575.pub2
Seymour NE (2008) VR to OR: a review of the evidence that virtual reality simulation improves operating room performance. World J Surg 32:182–188
Sturm LP, Windsor JA, Cosman PH et al (2008) A systematic review of skills transfer after surgical simulation training. Ann Surg 248:166–179
Hogle NJ, Widmann WD, Ude AO et al (2008) Does training novices to criteria and does rapid acquisition of skills on laparoscopic simulators have predictive validity or are we just playing video games? J Surg Educ 65:431–435
Snyder CW, Vandromme MJ, Tyra SL et al (2009) Proficiency-based laparoscopic and endoscopic training with virtual reality simulators: a comparison of proctored and independent approaches. J Surg Educ 66:201–207
Halsted WS (1904) The training of the surgeon. Bull Johns Hopkins Hosp 15:267–276
Custers EJ, Regehr G, McCulloch W et al (1999) The effects of modeling on learning a simple surgical procedure: see one, do one or see many, do one? Adv Health Sci Educ Theory Pract 4:123–143
Laguna PL (2008) Task complexity and sources of task-related information during the observational learning process. J Sports Sci 26:1097–1113
Weeks DL, Anderson LP (2000) The interaction of observational learning with overt practice: effects on motor skill learning. Acta Psychol (Amst) 104:259–271
Prentice RL, Williams BJ, Peterson AV (1981) On the regression analysis of multivariate failure time data. Biometrika 68:373–379
Moher D, Schulz KF, Altman D (2001) The CONSORT statement: revised recommendations for improving the quality of reports of parallel-group randomized trials. J Am Med Assoc 285:1987–1991
Kaufman HH, Wiegand RL, Tunick RH (1987) Teaching surgeons to operate—principles of psychomotor skills training. Acta Neurochir (Wien) 87:1–7
Wulf G, Shea CH (2002) Principles derived from the study of simple skills do not generalize to complex skill learning. Psychon Bull Rev 9:185–211
Xeroulis GJ, Park J, Moulton CA et al (2007) Teaching suturing and knot-tying skills to medical students: a randomized controlled study comparing computer-based video instruction and (concurrent and summary) expert feedback. Surgery 141:442–449
Risucci D, Cohen JA, Garbus JE (2001) The effects of practice and instruction on speed and accuracy during resident acquisition of simulated laparoscopic skills. Curr Surg 58:230–235
Badets A, Blandin Y (2004) The role of knowledge of results frequency in learning through observation. J Mot Behav 36:62–70
Porte MC, Xeroulis G, Reznick RK et al (2007) Verbal feedback from an expert is more effective than self-accessed feedback about motion efficiency in learning new surgical skills. Am J Surg 193:105–110
Pollock BJ, Lee TD (1992) Effects of the model’s skill level on observational motor learning. Res Q Exerc Sport 63:25–29
Badets A, Blandin Y, Bouquet CA et al (2006) The intention superiority effect in motor skill learning. J Exp Psychol Learn Mem Cogn 32:491–505
Bergamaschi R, Dicko A (2000) Instruction versus passive observation: a randomized educational research study on laparoscopic suture skills. Surg Laparosc Endosc Percutan Tech 10:319–322
Masters RS, Lo CY, Maxwell JP et al (2008) Implicit motor learning in surgery: implications for multi-tasking. Surgery 143:140–145
Stefanidis D, Korndorffer JR Jr, Sierra R et al (2005) Skill retention following proficiency-based laparoscopic simulator training. Surgery 138:165–170
Andreatta PB, Woodrum DT, Birkmeyer JT et al (2006) Laparoscopic skills are improved with LapMentor training: results of a randomized, double-blinded study. Ann Surg 243:854–860; discussion 860–863
Acknowledgments
The authors acknowledge Joshua L. Argo and Wai M. A. Yeung for their assistance with data acquisition. They are also grateful to Olympus of America and Covidien for equipment donation and technical assistance. The study received no external funding, although Christopher W. Snyder received salary support under an educational grant from Olympus America Inc.
Conflict of interest
Dr. Snyder received salary support under an educational grant from Olympus America Inc. Drs. Vandromme, Argo, Yeung, Porterfield, Clements, and Hawn have no conflicts of interest or financial ties to disclose. Ms. Tyra has no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Snyder, C.W., Vandromme, M.J., Tyra, S.L. et al. Effects of Virtual Reality Simulator Training Method and Observational Learning on Surgical Performance. World J Surg 35, 245–252 (2011). https://doi.org/10.1007/s00268-010-0861-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-010-0861-1