Abstract
Objectives
This study was designed to evaluate the clinical relevance of the World Health Organization (WHO) and tumor node metastasis (TNM) classifications in patients affected by pancreatic endocrine tumors.
Methods
Data from 76 consecutive patients with pancreatic endocrine tumors who underwent surgery were analyzed.
Results
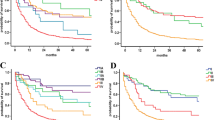
Well-differentiated tumors were observed more frequently (57.9%) than well or poorly differentiated carcinomas (26.3% and 15.8%, respectively). The TNM stage was I in 27.6%, II in 39.5%, III in 19.7%, and IV in 13.2%. Univariate analysis of disease-specific survival showed that patients with stages I–II had a significantly better survival rate than those with stages III–IV (hazard ratio (HR), 12.46; 95% confidence interval (CI), 1.53–101.32; P = 0.018; HR, 25.74; 95% CI, 3.07–216.07; P = 0.003, respectively). Regarding the WHO classification, poorly differentiated carcinomas had the worst prognosis (HR, 79.13; 95% CI, 9.99–626.60; P < 0.001). Multivariate Cox regression analysis of disease-specific survival showed that the WHO classification is the only independent factors of improved survival: both poorly and well-differentiated carcinomas had an increased risk of death compared with WDTs (HR, 100.42; 95% CI, 12.16–829.40; P < 0.001; HR, 10.73; 95% CI, 1.12–104.17; P = 0.040, respectively). TNM classification and the WHO system are highly correlated (P < 0.001).
Conclusions
TNM stage and the WHO classification seems to be equally reliable, even if TNM classification tends to understage the patients classified using the WHO system.
Similar content being viewed by others
References
Eriksson B, Oberg K (2000) Neuroendocrine tumours of the pancreas. Br J Surg 87:129–131
Moldow RE, Connelly RR (1968) Epidemiology of pancreatic cancer in Connecticut. Gastroenterology 55:677–686
Lam KY, Lo CY (1997) Pancreatic endocrine tumour: a 22-year clinicopathological experience with morphological, immunohistochemical observation and a review of the literature. Eur J Surg Oncol 23:36–42
Kloppel G, Heitz PU (1988) Pancreatic endocrine tumors. Pathol Res Pract 183:155–168
Maton PN, Gardner JD, Jensen RT (1989) Diagnosis and management of Zollinger–Ellison syndrome. Endocrinol Metab Clin North Am 18:519–543
Phan GQ, Yeo CJ, Hruban RH et al (1998) Surgical experience with pancreatic and peripancreatic neuroendocrine tumors: review of 125 patients. J Gastrointest Surg 2:472–482
Capella C, Heitz PU, Hofler H et al (1995) Revised classification of neuroendocrine tumours of the lung, pancreas and gut. Virchows Arch 425:547–560
Solcia E, Kloppel G, Sobin L et al (2000) Histological typing of endocrine tumours. World Health Organization International Histological Classification of Tumours, 2nd edn. Springer, Berlin
Rindi G, Kloppel G, Alhman H et al (2006) TNM staging of foregut (neuro)endocrine tumors: a consensus proposal including a grading system. Virchows Arch 449:395–401
Fischer L, Kleeff J, Esposito I et al (2008) Clinical outcome and long-term survival in 118 consecutive patients with neuroendocrine tumours of the pancreas. Br J Surg 95:627–635
Bettini R, Boninsegna L, Mantovani W et al (2008) Prognostic factors at diagnosis and value of WHO classification in a mono-institutional series of 180 non-functioning pancreatic endocrine tumours. Ann Oncol 19:903–908
La Rosa S, Klersy C, Uccella S et al (2009) Improved histologic and clinicopathologic criteria for prognostic evaluation of pancreatic endocrine tumors. Hum Pathol 40:30–40
Bassi C, Dervenis C, Butturini G et al (2005) International Study Group on pancreatic fistula definition. Al postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery 138:8–13
Casadei R, Zanini N, Morselli-Labate AM et al (2006) Prognostic factors in periampullary and pancreatic tumor resection in elderly patients. World J Surg 30:1992–2003
O’Grady HL, Conlon KC (2008) Pancreatic neuroendocrine tumours. EJSO 34:324–332
Halfdanarson TR, Rubin J, Farnell MB, Grant CS, Petersen GM (2008) Pancreatic endocrine neoplasms: epidemiology and prognosis of pancreatic endocrine tumors. Endocrine-Relat Cancer 15:409–427
Bilimoria KY, Talamonti S, Tomlinson JS, Stewt AK, Winchester DP, Ko CY, Bentrem DJ (2008) Prognostic score predicting survival after resection of pancreatic neuroendocrine tumors. Analysis of 3851 patients. Ann Surg 247:490–500
Bettini R, Mantovani W, Boninsegna L, Crippa S, Capelli P, Bassi C, Scarpa A, Pederzoli P, Falconi M (2009) Primary tumour resection in metastatic non-functioning pancreatic endocrine carcinomas. Dig Liver Dis 41:49–55
Panzuto F, Nasoni S, Falconi M et al (2005) Prognostic factors and survival in endocrine tumor patients: comparison between gastrointestinal and pancreatic localization. Endocr Relat Cancer 12:1083–1092
Gullo L, Migliori M, Falconi M et al (2003) Nonfunctioning pancreatic endocrine tumors: a multicenter clinical study. Am J Gastroenterol 98:2435–2439
Chu QD, Hill HC, Douglass HO Jr et al (2002) Predictive factors associated with long term survival in patients with neuroendocrine tumors of the pancreas. Ann Surg Oncol 9:855–862
Pape UF, Jann H, Müller-Nordhorn J, Bockelbrink A, Berndt U, Willich SN, Koch M, Röcken C, Rindi G, Wiedenmann B (2008) Prognostic relevance of a novel TNM classification system for upper gastroenteropancreatic neuroendocrine tumors. Cancer 113:256–265
Schmitt AM, Anlauf M, Rousson V, Schmid S, Kofler A, Riniker F, Bauersfeld J, Barghorn A, Probst-Hensch NM, Moch H, Heitz PU, Kloeppel G, Komminoth P, Perren A (2007) WHO 2004 criteria and CK19 are reliable prognostic markers in pancreatic endocrine tumors. Am J Surg Pathol 31:1677–1682
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Casadei, R., Ricci, C., Pezzilli, R. et al. Value of Both WHO and TNM Classification Systems for Patients with Pancreatic Endocrine Tumors: Results of a Single-Center Series. World J Surg 33, 2458–2463 (2009). https://doi.org/10.1007/s00268-009-0182-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-009-0182-4