Abstract
Background
The role of laparoscopic appendectomy (LA) in surgical training is unclear. Although LA as a therapeutic modality is potentially superior to open surgery, it has failed to become established as standard in training hospitals. The aim of the present study was to evaluate the outcome of LA performed by inexperienced surgeons in a training environment.
Materials and Methods
A retrospective analysis of all attempted LA performed over a 12-month period was undertaken. Data collected included operator grade (experienced and inexperienced), conversion rate and duration of surgery, complications, and postoperative stay.
Results
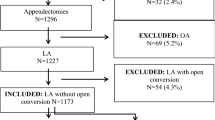
During the study period, 169 appendectomies were performed. The conversion rate to open surgery declined significantly from 28% in the first quarter to 9% in the last quarter, with no difference in the conversion rate between experienced and inexperienced surgeons. Operative time shortened significantly in the inexperienced group. Postoperative complications occurred in 8% of patients, independent of operative grade.
Conclusions
Our findings demonstrate that LA may be safely introduced as a teaching procedure. Time-to-train should not preclude institutions from adopting the laparoscopic approach in the treatment of acute appendicitis.




Similar content being viewed by others
References
Saurerland S, Lefering R, Neugebauer EAM. Laparoscopic versus open surgery for suspected appendicitis (Cochrane Review). The Cochrane Library, Issue 2, 2005, Chichester, UK, John Wiley & Sons, Ltd. Available at http://www.cochrane.org/cochrane/revabstr/AB001546.htm
Frazee RC, Roberts JW, Symmonds RE, et al. A prospective randomised trial comparing open versus laparoscopic appendectomy. Ann Surg 1994;219:725–731
Attwood SEA, Hill ADK, Murphy PG, et al. A prospective randomised trial comparing laparoscopic versus open appendectomy. Surgery 1992;112:497–501
Hansen JB, Smithers BM, Schache D, et al. Laparoscopic versus open appendectomy: prospective randomised trial. World J Surg 1996;20:17–21
Atabek U, Spence RK, Pello MJ, et al. Safety of teaching laparoscopic cholecystectomy to surgical residents. J Laparoendosc Surg 1993;3:23–26
Duff SE, Dixon AR. Laparoscopic appendectomy: safe and useful for training. Ann R Coll Surg Engl 2000;82:388–391
Scott-Connor CEH, Hall TJ, Anglin BL, et al. Laparoscopic appendectomy. Initial experience in a teaching program. Ann Surg 1992;215:660–667
Pier A, Goetz F, Bacher C, et al. Laparoscopic appendectomy. World J Surg 1993;17:29–33
Katkhouda N, Friedlander MH, Grant SW, et al. Intraabdominal abscess rate after laparoscopic appendectomy. Am J Surg 2000;180:456–461
McCormick PH, Tanner WA, Keane FBV, et al. Minimally invasive techniques in common surgical procedures: implications for training. Irish J Med Sci 2003;172:27–29
Tate JJ, Chung SC, Dawson J, et al. Conventional versus laparoscopic surgery for acute appendicitis. Br J Surg 1993;80:761–764
Nussbaum MS. Surgical endoscopy training is integral to general surgery residency and should be integrated into residency and fellowships abandoned. Semin Laparosc Surg 2002;9:212–215
M, Zacherl J, Rais A, Lipovac M, et al. Teaching laparoscopic cholecystectomy: do beginners adversely affect the outcome of the operation? Eur J Surg 2002;168:470–474
Carrasco-Prats M, Soria Aledo V, Lujan-Mompean JA, et al. Role of appendectomy in training for laparoscopic surgery. Surg Endosc 2003;17:111–114
Elder S, Kunin J, Chouri H, et al. Safety of laparoscopic cholecystectomy on a teaching service. Surg Laparosc Endosc 1996;6:218–220
Francis NK, Hanna GB, Cuschieri A. The performance of master surgeons on the Advanced Dundee Endoscopic Psychomotor Tester: contrast validity study. Arch Surg 2002;137:841–844
Rosen J, Solazzo M, Hannaford B, et al. Objective laparoscopic skills assessments of surgical residents using Hidden Markov Models based on haptic information and tool/tissue interactions. Stud Health Technol Inform 2001;81:417–423
Gallagher HJ, Allen JD, Tolley DA. Spatial awareness in urologists: are they different? Br J Urol Int 2001;88:666–670
Luckmann R, Davis P. The epidemiology of acute appendicitis in California: race, gender, and seasonal variation. Epidemiology 1991;2:323–330
Addiss DG, Shaffer N, Fowler BS, et al. The epidemiology of appendicitis and appendectomy in the United States. Am J Epidemiol 1990;132:910–925
Andersen BR, Kallehave FL, Andersen HK. Antibiotics versus placebo for prevention of postoperative infection after appendectomy (Cochrane Review). The Cochrane Library, Issue 2, 2005, Chichester, UK, John Wiley & Sons, Ltd. Available at http://www.cochrane.org/cochrane/revabstr/AB001439.htm
Chung RS, Rowland DY, Li P, et al. A meta-analysis of randomised controlled trials of laparoscopic versus conventional appendectomies. Am J Surg 1999;177:250–256
Garbutt JM, Soper NJ, Shannon WD, et al. Meta-analysis of randomised controlled trials comparing laparoscopic and open appendectomy. Surg Laparosc Endosc 1999;9:17–26
Fritts LL, Orlando R. Laparoscopic appendectomy: a safety and cost analysis. Arch Surg 1993;128:521–525
Meinke AK, Kossuth T. What is the learning curve for laparoscopic appendectomy? Surg Endosc 1994;8:371–375
Navez B, Penninckx F. Laparoscopic training: results of a Belgian survey in trainees. Belgian Group for Endoscopic Surgery (BGES). Acta Chir Belg 1999;99:53–58
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sweeney, K.J., Dillon, M., Johnston, S.M. et al. Training in Laparoscopic Appendectomy. World J. Surg. 30, 358–363 (2006). https://doi.org/10.1007/s00268-005-0311-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-005-0311-7