Abstract
Background
Liquid rhinoplasty, a non-surgical procedure using hyaluronic acid (HA) to reshape and refine the nose, has gained in popularity as an alternative to traditional surgical rhinoplasty although its results are not definitive. However, the lack of standardized injection protocols has raised concerns about treatment consistency and patient safety.
Objectives
In this article, the authors propose a systematic protocol for the most common indications of liquid rhinoplasty.
Methods
By adopting a standardized methodology, healthcare professionals can enhance patient safety, improve treatment consistency, and optimize patient satisfaction.
Results
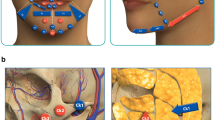
The protocol includes standardized injection sites categorized as dorsal, paramedian, tip and endonasal injections. Specific injection areas are recommended for different nasal shapes such as droopy noses, dorsal humps, nasal saddle deformity, inverted V deformity, tip shape abnormalities, twisted noses, revision cases with dorsal irregularities, and internal nasal valve dysfunction. While variations in filler dosages may be necessary based on individual patient needs, a conservative approach is recommended to maintain natural-looking results and reduce the risk of complications.
Conclusions
The increase in non-surgical techniques for nasal refinement offers patients more options, and systematized injection protocols based on different nasal types provide a structured framework for liquid rhinoplasty.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.





Similar content being viewed by others
References
Harb A, Brewster CT (2020) The nonsurgical rhinoplasty: a retrospective review of 5000 treatments. Plast Reconstr Surg 145:661–667. https://doi.org/10.1097/PRS.0000000000006554
Radulesco T, Winter C, Kestemont P et al (2022) Liquid spreader grafts: internal nasal valve opening with hyaluronic acid. Aesthetic Plast Surg 46:2912–2916. https://doi.org/10.1007/s00266-022-02913-8
Radulesco T, Braccini F, Kestemont P et al (2022) A safe nonsurgical rhinoplasty procedure. Plast Reconstr Surg 150:83e–86e. https://doi.org/10.1097/PRS.0000000000009226
Sahan A, Tamer F (2017) Non-surgical minimally invasive rhinoplasty: tips and tricks from the perspective of a dermatologist. Acta Dermatovenerol Alp Pannonica Adriat. https://doi.org/10.15570/actaapa.2017.29
Radulesco T, De Bonnecaze G, Penicaud M et al (2021) Patient satisfaction after non-surgical rhinoplasty using hyaluronic acid: a literature review. Aesthetic Plast Surg. https://doi.org/10.1007/s00266-021-02182-x
Pavicic T, Webb KL, Frank K et al (2019) Arterial wall penetration forces in needles versus cannulas. Plast Reconstr Surg 143:504e–512e. https://doi.org/10.1097/PRS.0000000000005321
de Maio M (2021) MD CodesTM: a methodological approach to facial aesthetic treatment with injectable hyaluronic acid fillers. Aesthetic Plast Surg 45:690–709. https://doi.org/10.1007/s00266-020-01762-7
Redaelli A (2008) Medical rhinoplasty with hyaluronic acid and botulinum toxin A: a very simple and quite effective technique. J Cosmet Dermatol 7:210–220. https://doi.org/10.1111/j.1473-2165.2008.00391.x
de la Guardia C, Virno A, Musumeci M et al (2022) Rheologic and physicochemical characteristics of hyaluronic acid fillers: overview and relationship to product performance. Facial Plast Surg FPS 38:116–123. https://doi.org/10.1055/s-0041-1741560
Radulesco T, Penicaud M, Santini L et al (2017) The MiRa scale, a new standardised scale for evaluating nasal deformities before and after septorhinoplasty: a prospective study comparing patient satisfaction and the surgeon’s assessment. Clin Otolaryngol 42:1350–1357. https://doi.org/10.1111/coa.12885
Konior RJ (2006) The droopy nasal tip. Facial Plast Surg Clin N Am 14(291–299):v. https://doi.org/10.1016/j.fsc.2006.06.002
de Maio M (2018) Myomodulation with Injectable Fillers: an innovative approach to addressing facial muscle movement. Aesthetic Plast Surg 42:798–814. https://doi.org/10.1007/s00266-018-1116-z
Nazım C (2017) Commentary on 3D photogrammetric analysis of the nasal tip projection and derotation based on the nasal tip quadripod concept. Aesthetic Plast Surg 41:1164–1166. https://doi.org/10.1007/s00266-017-0870-7
Chiang C-A, Tan P-C, Zhou S-B (2023) A reinforced framework construction technique using unilateral auricular cartilage in Asian rhinoplasty to prevent long-term nasal tip drooping. J Plast Reconstr Aesthetic Surg JPRAS 85:134–142. https://doi.org/10.1016/j.bjps.2023.07.001
Segreto F, Marangi GF, Cerbone V et al (2019) Nonsurgical rhinoplasty: a graft-based technique. Plast Reconstr Surg Glob Open 7:e2241. https://doi.org/10.1097/GOX.0000000000002241
Wang F, Garza LA, Kang S, Varani J, Orringer JS, Fisher GJ, Voorhees JJ (2007) In vivo stimulation of de novo collagen production caused by cross-linked hyaluronic acid dermal filler injections in photodamaged human skin. Arch Dermatol 143:155–163. https://doi.org/10.1001/archderm.143.2.155. (PMID: 17309996)
Ogilvie P, Benouaiche L, Philipp-Dormston WG et al (2020) VYC-25L hyaluronic acid injectable gel is safe and effective for long-term restoration and creation of volume of the lower face. Aesthet Surg J 40:NP499–NP510. https://doi.org/10.1093/asj/sjaa013
Beneduce N, Botter C, Coiante E et al (2023) The longevity of the nonsurgical rhinoplasty: a literature review. J Stomatol Oral Maxillofac Surg 124:101319. https://doi.org/10.1016/j.jormas.2022.10.018
Rohrich RJ, Novak M, Alleyne B, Bellamy J (2023) Five-principle and five-step liquid rhinoplasty. Plast Reconstr Surg 152(4):633e–636e. https://doi.org/10.1097/PRS.0000000000010162
Hall SS, Kontis TC (2023) Nonsurgical rhinoplasty. World J Otorhinolaryngol - Head Neck Surg 9:212–219. https://doi.org/10.1002/wjo2.104
Kassir R, Venkataram A, Malek A, Rao D (2021) Non-surgical rhinoplasty: the ascending technique and a 14-year retrospective study of 2130 cases. Aesthetic Plast Surg 45:1154–1168. https://doi.org/10.1007/s00266-020-02048-8
Chen Q, Liu Y, Fan D (2016) Serious vascular complications after nonsurgical rhinoplasty: a case report. Plast Reconstr Surg Glob Open 4:e683. https://doi.org/10.1097/GOX.0000000000000668
Mortada H, Korb A, Mawdsley E et al (2023) The use of hyaluronic acid in non-surgical rhinoplasty: a systematic review of complications, clinical, and patient-reported outcomes. Aesthetic Plast Surg. https://doi.org/10.1007/s00266-023-03386-z
DeVictor S, Ong AA, Sherris DA (2021) Complications secondary to nonsurgical rhinoplasty: a systematic review and meta-analysis. Otolaryngol-Head Neck Surg Off J Am Acad Otolaryngol-Head Neck Surg 165:611–616. https://doi.org/10.1177/0194599820987827
Jolly R, Bhalla M, Zakir R, Joshi N (2021) Visual loss from dermal fillers. Eur J Ophthalmol 31:NP102–NP105. https://doi.org/10.1177/1120672119855856
Wollina U, Goldman A (2020) Facial vascular danger zones for filler injections. Dermatol Ther 33:e14285. https://doi.org/10.1111/dth.14285
Lu Y, Hong W-J, Luo C-E et al (2022) Vasculature of the nasal cartilage region related to filler injection. Aesthetic Plast Surg 46:2461–2468. https://doi.org/10.1007/s00266-022-02942-3
Ugradar S, Hoenig J (2019) Measurement of the force required by blunt-tipped microcannulas to perforate the facial artery. Ophthal Plast Reconstr Surg 35:444–446. https://doi.org/10.1097/IOP.0000000000001302
Magacho-Vieira FN, Alfertshofer MG, Cotofana S (2022) The deep columellar approach for liquid rhinoplasty - a case series of 511 procedures over 16 years. Facial Plast Surg Clin N Am 30:193–203. https://doi.org/10.1016/j.fsc.2022.01.005
Mehta U, Fridirici Z (2019) Advanced techniques in nonsurgical rhinoplasty. Facial Plast Surg Clin N Am 27:355–365. https://doi.org/10.1016/j.fsc.2019.04.008
Goodman GJ, Magnusson MR, Callan P et al (2022) Aspiration before tissue filler-an exercise in futility and unsafe practice. Aesthet Surg J 42:89–101. https://doi.org/10.1093/asj/sjab036
Lin F, Goodman GJ, Magnusson M et al (2022) Movement of the syringe during filler aspiration: an ultrasound study. Aesthet Surg J 42:1109–1116. https://doi.org/10.1093/asj/sjac032
Acknowledgments
None.
Funding
All authors have nothing to disclose. No funding was received for this article
Author information
Authors and Affiliations
Contributions
TR contributed to writing–original draft, supervision, writing–review & editing. DE contributed to reviewing and data collection. JM contributed to validation, writing–review & editing
Corresponding author
Ethics declarations
Conflict of interest
No conflict of interest. The authors declare that they have no conflicts of interest to disclose.
Human and Animals Participants
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed Consent
Patients provided written informed consent for the use of their images.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Radulesco, T., Ebode, D. & Michel, J. Advancing the Era of Liquid Rhinoplasty: A Methodological Approach to Injection Protocols. Aesth Plast Surg (2024). https://doi.org/10.1007/s00266-024-04025-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00266-024-04025-x