Abstract
Background
The aim of this study was to evaluate the effectiveness of the intravenous, oral and local application of tranexamic acid in operation time, intraoperative bleeding, postoperative edema and ecchymosis in rhinoplasty.
Methods
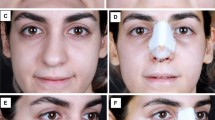
This was a randomized, double-blinded, prospective study. We included 146 patients who underwent rhinoplasty at the Bezmialem Vakif University Medical Faculty Otorhinolaryngology Clinic between April 2021 and April 2022. The patients were divided into four groups: Group 1 (intravenous TXA), Group 2 (oral TXA), Group 3 (topical TXA), and Group 4 (control). Operation time was recorded. Bleeding volume was measured in the suction chamber and nasopharyngeal pack. Postoperative edema and ecchymosis were evaluated using a scale at the end of the operation, on the 1st, 3rd, and 7th days.
Results
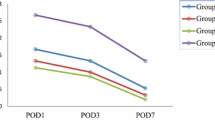
There was no statistically significant difference between groups in terms of mean operation time (p = 0.894). There was a statistically significant lower mean intraoperative bleeding level in Group 2 from the other groups (p = 0.020). Group 3 had significantly lower scores for postoperative edema than the other groups at the end of the operation, on the 1st, 3rd, and 7th days (p < 0.05), and significantly lower scores for postoperative ecchymosis at the end of the operation (p = 0.013) and on the 3rd day (p = 0.024). Although group 3 had a lower score than the other groups in the ecchymosis measurements on the 1st, and 7th days, no statistically significant results were obtained.
Conclusions
Local application of tranexamic acid is founded more beneficial for reducing postoperative edema and ecchymosis in rhinoplasty than intravenous and/or oral applications in this study.
Level of Evidence I
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.


Similar content being viewed by others
References
Heilbronn C, Cragun D, Wong BJ (2020) Complications in rhinoplasty: a literature review and comparison with a survey of consent forms. Fac Plast Surg Aesthet Med 22(1):50–56
Nilsson IM (1980) Clinical pharmacology of aminocaproic and tranexamic acids. J Clin Pathol Suppl (R Coll Pathol) 14:41
Fu DJ, Chen C, Guo L, Yang L (2013) Use of intravenous tranexamic acid in total knee arthroplasty: a meta-analysis of randomized controlled trials. Chin J Traumatol 16(02):67–76
Zhang F, Wang K, Li FN, Huang X, Li Q, Chen Z, Song QX (2014) Effectiveness of tranexamic acid in reducing blood loss in spinal surgery: a meta-analysis. BMC Musculoskelet Disord 15(1):1–9
Avci H (2021) The effect of different dose regimens of tranexamic acid in reducing blood loss in rhinoplasty: a prospective randomized controlled study. J Craniofac Surg 32(5):e442–e444
McGuire C, Nurmsoo S, Samargandi OA, Bezuhly M (2019) Role of tranexamic acid in reducing intraoperative blood loss and postoperative edema and ecchymosis in primary elective rhinoplasty. JAMA Fac Plast Surg. https://doi.org/10.1001/jamafacial.2018.1737
Ipek HD, Bezgin SÜ, Çakabay T, Çelebi S (2021) The effects of intraoperative local tranexamic acid on periorbital edema and ecchymosis in septorhinoplasty. J Craniofac Surg 32(6):e526–e530
Ghavimi MA, Talesh KT, Ghoreishizadeh A, Chavoshzadeh MA, Zarandi A (2017) Efficacy of tranexamic acid on side effects of rhinoplasty: a randomized double-blind study. J Cranio-Maxillofac Surg 45(6):897–902
Hoffmann DF, Cook TA, Quatela VC, Wang TD, Brownrigg PJ, Brummett RE (1991) Steroids and rhinoplasty: a double-blind study. Arch Otolaryngol Head Neck Surg 117(9):990–993
Sowerby L, Kim LM, Chow W, Moore C (2019) Intra-operative nasal compression after lateral osteotomy to minimize post-operative Peri-orbital ecchymosis and edema. J Otolaryngol Head Neck Surg 48(1):1–5
Levin M, Ziai H, Roskies M (2022) Modalities of post-rhinoplasty edema and ecchymosis measurement: a systematic review. Plast Surg 30(2):164–174
de Vasconcellos SJDA, do Nascimento-Júnior EM, de Aguiar Menezes MV, Mendes MLT, de Souza Dantas R, Martins-Filho PRS (2018) Preoperative tranexamic acid for treatment of bleeding, edema, and ecchymosis in patients undergoing rhinoplasty: a systematic review and meta-analysis. JAMA Otolaryngol Head Neck Surg 144(9):816–823
Rahimzadeh P, Faiz SHR, Alebouyeh MR (2012) Effects of premedication with metoprolol on bleeding and induced hypotension in nasal surgery. Anesthesiol Pain Med 1(3):157
Gun R, Yorgancilar E, Yildirim M, Bakir S, Topcu I, Akkus Z (2011) Effects of lidocaine and adrenaline combination on postoperative edema and ecchymosis in rhinoplasty. Int J Oral Maxillofac Surg 40(7):722–729
Kosucu M, Ömür S, Besir A, Uraloglu M, Topbas M, Livaoglu M (2014) Effects of perioperative remifentanil with controlled hypotension on intraoperative bleeding and postoperative edema and ecchymosis in open rhinoplasty. J Craniofac Surg 25(2):471–475
Tuncel U, Turan A, Bayraktar MA, Erkorkmaz U, Kostakoglu N (2013) Efficacy of dexamethasone with controlled hypotension on intraoperative bleeding, postoperative oedema and ecchymosis in rhinoplasty. J Cranio-Maxillofac Surg 41(2):124–128
Gruber RP, Zeidler KR, Berkowitz RL (2015) Desmopressin as a hemostatic agent to provide a dry intraoperative field in rhinoplasty. Plast Reconstr Surg 135(5):1337–1340
Ong AA, Farhood Z, Kyle AR, Patel KG (2016) Interventions to decrease postoperative edema and ecchymosis after rhinoplasty: a systematic review of the literature. Plast Reconstr Surg 137(5):1448–1462
Wu B, Chen S, Sun K, Xu X (2021) Complications associated with rhinoplasty: an umbrella review of meta-analyses. Aesthet Plast Surg 46:1–13
Mannucci PM (1998) Hemostatic drugs. N Engl J Med 339(4):245–253
Zhang LK, Ma JX, Kuang MJ, Zhao J, Wang Y, Lu B, Ma XL (2017) Comparison of oral versus intravenous application of tranexamic acid in total knee and hip arthroplasty: a systematic review and meta-analysis. Int J Surg 45:77–84
Pilbrant Å, Schannong M, Vessman J (1981) Pharmacokinetics and bioavailability of tranexamic acid. Eur J Clin Pharmacol 20(1):65–72
Wei Z, Liu M (2015) The effectiveness and safety of tranexamic acid in total hip or knee arthroplasty: a meta-analysis of 2720 cases. Transfus Med 25(3):151–162
Poeran J, Rasul R, Suzuki S, Danninger T, Mazumdar M, Opperer M, Memtsoudis SG (2014) Tranexamic acid use and postoperative outcomes in patients undergoing total hip or knee arthroplasty in the United States: retrospective analysis of effectiveness and safety. BMJ. https://doi.org/10.1136/bmj.g4829
Meaidi A, Mørch L, Torp-Pedersen C, Lidegaard O (2021) Oral tranexamic acid and thrombosis risk in women. EClinicalMedicine 35:100882
Van Der Staak FHJ, De Haan AFJ, Geven WB, Festen C (1997) Surgical repair of congenital diaphragmatic hernia during extracorporeal membrane oxygenation: hemorrhagic complications and the effect of tranexamic acid. J Pediatr Surg 32(4):594–599
Ker K, Edwards P, Perel P, Shakur H, Roberts I (2012) Effect of tranexamic acid on surgical bleeding: systematic review and cumulative meta-analysis. BMJ 344:e3054
Laoruengthana A, Rattanaprichavej P, Chaibhuddanugul N, Varakornpipat P, Galassi M, Pongpirul K (2019) Blood loss reduction: effect of different knee prosthesis designs and use of tranexamic acid—a randomized controlled trial. Eur J Orthop Surg Traumatol 29(7):1519–1524
Cristel RT, Demesh D, Patel MJ, Shah AR (2022) Quantitative analysis of tranexamic acid effects on ecchymosis in rhinoplasty. Fac Plast Surg Aesthet Med 24(3):228–232
Afzali SL, Panahi H, Ganji F, Ziaei S, Sedaghat N (2022) Re-evaluating the effect of preoperative tranexamic acid on blood loss and field quality during rhinoplasty: a randomized double-blinded controlled trial. Aesthet Plast Surg 46(3):1314–1320
Eftekharian HR, Rajabzadeh Z (2016) The efficacy of preoperative oral tranexamic acid on intraoperative bleeding during rhinoplasty. J Craniofac Surg 27(1):97–100
Hazrati E, Masnour-Ghanaei A, Soleimanlo A, Rafiei M (2021) Evaluation of local tranexamic acid on septoplastic surgery quality. J Plast Reconstr Aesthet Surg 74(10):2744–2750
Acknowledgements
The authors declare that they have no conflict of interest.
Funding
The authors received no financial support for the research, authorship, and publication of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Approval
All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1954 Helsinki Declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sezen Göktaş, S., Yenigün, A., Sütcü, A.O. et al. Tranexamic Acid and Rhinoplasty: How Do Different Administration Routes Affect Effectiveness?. Aesth Plast Surg (2024). https://doi.org/10.1007/s00266-024-03951-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00266-024-03951-0