Abstract
Objectives
The inferior and middle turbinates have crucial roles in nasal function, but their enlargement can cause obstructive effects, which can lead to breathing difficulties, sleep and smell disorders, and headaches. Partial turbinectomy is a common surgical technique used to address this issue during septorhinoplasty, but it carries risks such as empty nose syndrome. A clinical trial was designed to evaluate the functional outcomes of middle and inferior partial turbinectomy with a holistic approach.
Methods
Patients with NOSE questionnaire scores of 30 or higher, and grade 4 inferior turbinates and/or advanced middle concha bullosa were included. Patients completed questionnaires related to breathing, empty nose syndrome, headache, and olfaction preoperatively and at one-month, three-month, six-month, and first-year periods postoperatively. The partial excisions of the inferior and middle turbinates were carried out with serrated scissors while trying to preserve adequate turbinate size to maintain function.
Results
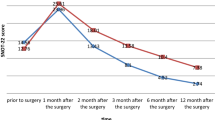
This study found that NOSE scores, headache frequency, and severity improved postoperatively. The olfactory-related quality of life of the patients with impairments in this area significantly improved found to be improved at all postoperative evaluations. None of the patients experienced prolonged bleeding requiring surgical intervention. No cases of anosmia and empty nose syndrome were reported.
Conclusion
Partial turbinectomy of middle and inferior turbinates during septorhinoplasty can alleviate symptoms of turbinate hypertrophy, such as breathing issues, olfactory disorders, and headaches. It is an easy, reliable, and efficient surgical maneuver. Proper technique can minimize the risk of empty nose syndrome and other complications of turbinectomy surgery.
Level of Evidence III
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.








Similar content being viewed by others
References
Balikci HH, Gurdal MM (2014) Satisfaction outcomes in open functional septorhinoplasty: prospective analysis. J Craniofac Surg 25(2):377–379. https://doi.org/10.1097/scs.0000000000000638
Georgalas C (2011) The role of the nose in snoring and obstructive sleep apnoea: an update. Eur Arch Otorhinolaryngol 268(9):1365–1373. https://doi.org/10.1007/s00405-010-1469-7
Shapiro GG (1988) The role of nasal airway obstruction in sinus disease and facial development. J Allergy Clin Immunol 82(5 Pt 2):935–940. https://doi.org/10.1016/0091-6749(88)90036-x
Nurse LA, Duncavage JA (2009) Surgery of the inferior and middle turbinates. Otolaryngol Clin North Am 42(2):295–309. https://doi.org/10.1016/j.otc.2009.01.009
Smith DH, Brook CD, Virani S, Platt MP (2018) The inferior turbinate: an autonomic organ. Am J Otolaryngol 39(6):771–775. https://doi.org/10.1016/j.amjoto.2018.08.009
Lenders H, Schaefer J, Pirsig W (1991) Turbinate hypertrophy in habitual snorers and patients with obstructive sleep apnea: findings of acoustic rhinometry. Laryngoscope 101(6 Pt 1):614–618. https://doi.org/10.1288/00005537-199106000-00007
Garcia JPT, Moura BH, Rodrigues VH, Vivan MA et al (2022) Inferior turbinate reduction during rhinoplasty: is there any effect on rhinitis symptoms? Int Arch Otorhinolaryngol 26(1):e111–e118. https://doi.org/10.1055/s-0041-1726046
Gunhan K, Unlu H, Yuceturk AV, Songu M (2011) Intranasal steroids or radiofrequency turbinoplasty in persistent allergic rhinitis: effects on quality of life and objective parameters. Eur Arch Otorhinolaryngol 268(6):845–850. https://doi.org/10.1007/s00405-010-1462-1
Mohamed NN, Khamis W, Abdelbary EH, Alkabeer TY (2022) Diode laser-assisted inferior turbinoplasty in resistant cases of allergic rhinitis: a clinical and histopathological study. Lasers Med Sci 37(3):2053–2061. https://doi.org/10.1007/s10103-021-03477-w
Zhang K, Pipaliya RM, Miglani A, Nguyen SA et al (2023) Systematic review of surgical interventions for inferior turbinate hypertrophy. Am J Rhinol Allergy 37(1):110–122. https://doi.org/10.1177/19458924221134555
Gordiienko IM, Gubar OS, Sulik R, Kunakh T et al (2021) Empty nose syndrome pathogenesis and cell-based biotechnology products as a new option for treatment. World J Stem Cells 13(9):1293–1306. https://doi.org/10.4252/wjsc.v13.i9.1293
de Moura BH, Migliavacca RO, Lima RK, Dolci JEL et al (2018) Partial inferior turbinectomy in rhinoseptoplasty has no effect in quality-of-life outcomes: a randomized clinical trial. Laryngoscope 128(1):57–63. https://doi.org/10.1002/lary.26831
Levy E, Ronen O, Sela E, Layos E et al (2022) Inferior turbinate reduction: comparing post-operative bleeding between different surgical techniques. J Laryngol Otol 136(5):427–432. https://doi.org/10.1017/s0022215121003297
Stewart MG, Witsell DL, Smith TL, Weaver EM et al (2004) Development and validation of the nasal obstruction symptom evaluation (NOSE) scale. Otolaryngol Head Neck Surg 130(2):157–163. https://doi.org/10.1016/j.otohns.2003.09.016
Camacho M, Zaghi S, Certal V, Abdullatif J et al (2015) Inferior turbinate classification system, grades 1 to 4: development and validation study. Laryngoscope 125(2):296–302. https://doi.org/10.1002/lary.24923
Pusswald G, Auff E, Lehrner J (2012) Development of a brief self-report inventory to measure olfactory dysfunction and quality of life in patients with problems with the sense of smell. Chemosens Percept. https://doi.org/10.1007/s12078-012-9127-7
Saatci Ö, Arici Duz O, Altundag A (2020) Reliability and validity of the Turkish version of the questionnaire for the assessment of self-reported olfactory functioning and olfaction-related quality of life. J Acad Res Med 10:277–282. https://doi.org/10.4274/jarem.galenos.2020.3579
Velasquez N, Thamboo A, Habib AR, Huang Z et al (2017) The empty nose syndrome 6-item questionnaire (ENS6Q): a validated 6-item questionnaire as a diagnostic aid for empty nose syndrome patients. Int Forum Allergy Rhinol 7(1):64–71. https://doi.org/10.1002/alr.21842
Chan BKC (2018) Data analysis using R programming. Adv Exp Med Biol 1082:47–122. https://doi.org/10.1007/978-3-319-93791-5_2
Chen XB, Lee HP, Chong VF, De Wang Y (2010) Impact of inferior turbinate hypertrophy on the aerodynamic pattern and physiological functions of the turbulent airflow - a CFD simulation model. Rhinology 48(2):163–168. https://doi.org/10.4193/Rhin09.093
Kennedy DW (1998) Middle turbinate resection: evaluating the issues–should we resect normal middle turbinates? Arch. Otolaryngol Head Neck Surg 124(1):107. https://doi.org/10.1001/archotol.124.1.107
Hong HR, Jang YJ (2016) Correlation between remnant inferior turbinate volume and symptom severity of empty nose syndrome. Laryngoscope 126(6):1290–1295. https://doi.org/10.1002/lary.25830
Karamatzanis I, Kosmidou P, Ntarladima V, Catalli B et al (2022) Inferior Turbinate hypertrophy: a comparison of surgical techniques. Cureus 14(12):e32579. https://doi.org/10.7759/cureus.32579
Sinno S, Mehta K, Lee ZH, Kidwai S et al (2016) Inferior turbinate hypertrophy in rhinoplasty: systematic review of surgical techniques. Plast Reconstr Surg 138(3):419e–429e. https://doi.org/10.1097/prs.0000000000002433
Cavaliere M, Mottola G, Iemma M (2007) Monopolar and bipolar radiofrequency thermal ablation of inferior turbinates: 20-month follow-up. Otolaryngol Head Neck Surg 137(2):256–263. https://doi.org/10.1016/j.otohns.2007.01.001
Kilavuz AE, Songu M, Ozkul Y, Ozturkcan S et al (2014) Radiofrequency versus electrocautery for inferior turbinate hypertrophy. J Craniofac Surg 25(6):1998–2001. https://doi.org/10.1097/scs.0000000000001032
Law RH, Bazzi TD, Van Harn M, Craig JR et al (2021) Predictors of long-term nasal obstruction symptom evaluation score stability following septoplasty with inferior turbinate reduction. Laryngoscope 131(7):E2105-e2110. https://doi.org/10.1002/lary.29229
Anselmo-Lima WT, de Oliveira JA, Speciali JG, Bordini C et al (1997) Middle turbinate headache syndrome. Headache 37(2):102–106. https://doi.org/10.1046/j.1526-4610.1997.3702102.x
Tosun F, Gerek M, Ozkaptan Y (2000) Nasal surgery for contact point headaches. Headache 40(3):237–240. https://doi.org/10.1046/j.1526-4610.2000.00034.x
Inan S, Gultekin G, Yilmaz I, Buyuklu AF (2023) Effect of functional Septorhinoplasty with concha bullosa resection on Sinonasal symptoms. Laryngoscope 133(6):1375–1381. https://doi.org/10.1002/lary.30428
Akkoca Ö, Tüzüner A, Ünlü CE, Şimşek G et al (2020) Comparison of the effects of 2 surgical techniques used in the treatment of concha bullosa on olfactory functions. Ear Nose Throat J 99(7):437–441. https://doi.org/10.1177/0145561319881061
Moore EJ, Kern EB (2001) Atrophic rhinitis: a review of 242 cases. Am J Rhinol 15(6):355–361
Chhabra N, Houser SM (2009) The diagnosis and management of empty nose syndrome. Otolaryngol Clin North Am 42(2):311–330. https://doi.org/10.1016/j.otc.2009.02.001
Funding
The authors received no financial support for this article's research, authorship, and publication.
Author information
Authors and Affiliations
Contributions
MÇ: Substantial contributions to Conception and design, analysis and interpretation of the data, drafting the article or revising it critically for important intellectual content; and (3) final approval of the version to be published. SKA: Substantial contributions to Conception and design, analysis and interpretation of the data, drafting the article critically for important intellectual content; and (3) final approval of the version to be published. UK: Substantial contributions to design, analysis, and interpretation of the data, drafting the article for important intellectual content; and (3) final approval of the version to be published. AK: Substantial contributions to Conception and design, analysis and interpretation of the data, drafting the article or revising it critically for important intellectual content; and (3) final approval of the version to be published
Corresponding author
Ethics declarations
Conflict of interest
The authors declared no potential conflicts of interest concerning this article's research, authorship, and publication.
Ethical Approval
This material is the author’s original work, which has not been previously published elsewhere. This study was performed by research ethical guidelines. There are no human subjects in this article and informed consent is not applicable. All authors have contributed to the paper and have permitted their names to be included as co-authors. This manuscript is not submitted to or is currently under review at any other journal.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Çelik, M., Altunal, S.K., Kocer, U. et al. Comprehensive Assessment of the Functional Outcomes of Partial Turbinectomy: A Prospective Clinical Trial. Aesth Plast Surg 48, 1547–1556 (2024). https://doi.org/10.1007/s00266-023-03503-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-023-03503-y