Abstract
Background
An objective assessment of the causes of age-related contour deformities of the soft tissues of the face and neck is very important in esthetic surgery, especially as minimally invasive techniques gain increasing popularity.
Methods
To visualize the tissues that cause age-related soft tissue changes, we performed cone-beam computed tomography (CBCT) in 37 patients who underwent facial and neck rejuvenation procedures in 2021–2022.
Results
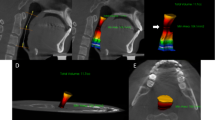
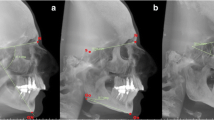
Vertical CBCT enabled visualization of the causes and degree of tissue involvement in age-related changes in the lower third of the face and neck. CBCT showed the location and condition of the platysma (hypo- [ptosis], normo-, or hyper-tonus), position, thickness, and location (above and/or below the platysma) of fat tissue, presence of ptosis of the submandibular salivary glands, condition of the anterior bellies of the digastric muscles, and the degree of their participation in contours of the cervicomandibular angle, and location of the hyoid bone. Moreover, CBCT enabled demonstrating for the patient the facial and neck contour deformations and discussing the suggested corrective methods using a clear objective visual image.
Conclusions
CBCT in the upright position enables objective assessment of each soft tissue in the age-related deformity of the cervicofacial region and provides an opportunity to plan the appropriate impact on the particular anatomical structures during rejuvenation procedures and estimate their results. This is the only study to date to objectively and clearly visualize the entire topographic anatomy of the soft tissues of the face and neck vertically for plastic surgeons and patients.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.



Similar content being viewed by others
References
Lu PH, Yang CH, Chang YC (2017) Quantitative analysis of face and neck skin tightening by microfocused ultrasound with visualization in Asians. Dermatol Surg 43:1332–1338. https://doi.org/10.1097/DSS.0000000000001181
Hwang K, Kim JY, Lim JH (2017) Anatomy of the platysma muscle. J Craniofac Surg 28:539–542. https://doi.org/10.1097/scs.0000000000003318
Rohrich RJ, Rios JL, Smith PD, Gutowski KA (2006) Neck rejuvenation revisited. Plast Reconstr Surg 118:1251–1263. https://doi.org/10.1097/01.prs.0000209406.80690.9f
Baker DC (2001) Minimal incision rhytidectomy (short scar face lift) with lateral SMASectomy: evolution and application. Aesthet Surg J 21:14–26. https://doi.org/10.1067/maj.2001.113557
Jacono AA, Malone MH (2017) Characterization of the cervical retaining ligaments during subplatysmal facelift dissection and its implications. Aesthet Surg J 37:495–501. https://doi.org/10.1093/asj/sjw274
Jacono AA, Bryant LM (2018) Extended deep plane facelift: incorporating facial retaining ligament release and composite flap shifts to maximize midface, jawline and neck rejuvenation. Clin Plast Surg 45:527–554. https://doi.org/10.1016/j.cps.2018.06.007
Sykes JM, Riedler KL, Cotofana S, Palhazi P (2020) Superficial and deep facial anatomy and its implications for rhytidectomy. Facial Plast Surg Clin North Am 28:243–251. https://doi.org/10.1016/j.fsc.2020.03.005
Quatela V, Montague A, Manning JP, Antunes M (2020) Extended superficial musculoaponeurotic system flap rhytidectomy. Facial Plast Surg Clin North Am 28:303–310. https://doi.org/10.1016/j.fsc.2020.03.007
Auersvald A, Auersvald LA, Oscar Uebel C (2017) Subplatysmal necklift: a retrospective analysis of 504 patients. Aesthet Surg J 37:1–11. https://doi.org/10.1093/asj/sjw107
Geister TL, Bleßmann-Gurk B, Rzany B, Harrington L, Görtelmeyer R, Pooth R (2013) Validated assessment scale for platysmal bands. Dermatol Surgery 39:1217–1225. https://doi.org/10.1111/dsu.12240
Patel S, Brown J, Pimentel T, Kelly RD, Abella F, Durack C (2019) Cone beam computed tomography in endodontics - a review of the literature. Int Endod J 52:1138–1152. https://doi.org/10.1111/iej.13115
Zhang Y, Wang Y, Zhang Y, Li S, Wang L, Qian Y (2019) Cone-beam computed tomography evaluation of skeletal deformities and pharyngeal airway in Chinese han individuals with nonsyndromic unilateral cleft lip and palate. Cleft Palate-Craniofacial J 57:65–72. https://doi.org/10.1177/1055665619860700
Lentzen MP, Zirk M, Riekert M, Buller J, Kreppel M (2020) Anatomical and volumetric analysis of the sphenoid sinus by semiautomatic segmentation of cone beam computed tomography. J Craniofacial Surg 32:1166–1170. https://doi.org/10.1097/scs.0000000000007209
Bellity P, Bellity J (2017) Facial rejuvenation enhancing cheek lift. Arch Plastic Surg 44:559–563. https://doi.org/10.5999/aps.2016.01858
Busso M (2021) A new approach to thread facelifting. J Drugs Dermatol 20:1085–1090. https://doi.org/10.36849/jdd.6139
Gasperoni C, Gasperoni P, Pino V (2021) Conservative neck rejuvenation. Facial Plast Surg 37:400–406. https://doi.org/10.1055/s-0041-1725167
Feldman JJ (2017) Discussion: platysma bands: is a change needed in the surgical paradigm? Plast Reconstr Surg 139:48–49. https://doi.org/10.1097/prs.0000000000002895
Knipper P, Mitz V (2017) Platysma bands: is a change needed in the surgical paradigm? Plast Reconstr Surg 140:755e. https://doi.org/10.1097/prs.0000000000003783
Trévidic P, Criollo-Lamilla G (2017) Reply: platysma bands: is a change needed in the surgical paradigm? Plast Reconstr Surg 140:755e–756e. https://doi.org/10.1097/prs.0000000000003784
Matarasso A, Matarasso SL, Brandt FS, Bellman B (1999) Botulinum a exotoxin for the management of platysma bands. Plast Reconstr Surg 103:645–652. https://doi.org/10.1097/00006534-199902000-00043
Trévidic P, Criollo-Lamilla G (2019) Surgical denervation of platysma bands. Plast Reconstr Surg 144:798e–802e. https://doi.org/10.1097/prs.0000000000006148
Daher JC (2011) Closed platysmotomy: a new procedure for the treatment of platysma bands without skin dissection. Aesthet Plast Surg 35:866–877. https://doi.org/10.1007/s00266-011-9782-0
Pelle-Ceravolo M, Angelini M (2019) Lateral skin-platysma displacement. Clinics in Plast Surg 46:587–602. https://doi.org/10.1016/j.cps.2019.06.006
Cotofana S, Lachman N (2019) Anatomy of the facial fat compartments and their relevance in aesthetic surgery. JDDG: J der Deutschen Dermatologischen Gesellschaft 17: 399-413. https://doi.org/10.1111/ddg.13737
Okuda I, Yoshioka N, Shirakabe Y, Akita K (2019) Basic analysis of facial ageing: the relationship between the superficial musculoaponeurotic system and age. Exp Dermatol 28:38–42. https://doi.org/10.1111/exd.13827
Gierloff M, Stöhring C, Buder T, Gassling V, Açil Y, Wiltfang J (2012) Aging changes of the midfacial fat compartments: a computed tomographic study. Plast Reconstr Surg 129:263–273. https://doi.org/10.1097/prs.0b013e3182362b96
Tower JI, Seifert K, Paskhover B (2018) Patterns of superficial midfacial fat volume distribution differ by age and body mass index. Aesthet Plast Surg 43:83–90. https://doi.org/10.1007/s00266-018-1249-0
Wysong A, Joseph T, Kim D, Tang JY, Gladstone HB (2013) Quantifying soft tissue loss in facial aging: a study in women using magnetic resonance imaging. Dermatol Surg 39:1895–1902. https://doi.org/10.1111/dsu.12362
Schenck TL, Koban KC, Schlattau A (2018) The functional anatomy of the superficial fat compartments of the face: a detailed imaging study. Plast Reconstr Surg 141(6):1351–1359. https://doi.org/10.1097/prs.0000000000004364
Macchi V, Tiengo C, Porzionato A (2007) Anatomo-radiological study of the superficial musculo-aponeurotic system of the face. Ital J Anat Embryol 112:247–253
Mashkevich G, Wang J, Rawnsley J, Keller GS (2009) The utility of ultrasound in the evaluation of submental fullness in aging necks. Arch Facial Plast Surg 11:240–245. https://doi.org/10.1001/archfacial.2009.47
Agbolade O, Nazri A, Yaakob R, Ghani AA, Cheah YK (2020) Morphometric approach to 3D soft-tissue craniofacial analysis and classification of ethnicity, sex, and age. PLoS ONE 15:e0228402. https://doi.org/10.1371/journal.pone.0228402
Windhager S, Mitteroecker P, Rupić I, Lauc T, Polašek O, Schaefer K (2019) Facial aging trajectories: a common shape pattern in male and female faces is disrupted after menopause. Am J Phys Anthropol 169:678–688. https://doi.org/10.1002/ajpa.23878
Ozsoy U, Sekerci R, Ogut E (2015) Effect of sitting, standing, and supine body positions on facial soft tissue: detailed 3D analysis. Int J Oral Maxillofac Surg 44:1309–1316. https://doi.org/10.1016/j.ijom.2015.06.005
Yamaguchi Y, Yamauchi K, Suzuki H, Sai Y, Nogami S, Takahashi T (2018) Volumetric comparison of maxillofacial soft tissue morphology: computed tomography in the supine position versus three-dimensional optical scanning in the sitting position. Oral Surg Oral Med Oral Pathol Oral Radiol 125:351–357. https://doi.org/10.1016/j.oooo.2017.12.018
Munn L, Stephan CN (2018) Changes in face topography from supine-to-upright position-and soft tissue correction values for craniofacial identification. Forensic Sci Int 289:40–50. https://doi.org/10.1016/j.forsciint.2018.05.016
Bulut O, Jessica Liu CY, Koca F, Wilkinson C (2017) Comparison of three-dimensional facial morphology between upright and supine positions employing three-dimensional scanner from live subjects. Leg Med 27:32–37. https://doi.org/10.1016/j.legalmed.2017.06.002
McCleary SP, Moghadam S, Le C, Perez K, Sim MS, Roostaeian J (2022) Age-related changes in the submandibular gland: an imaging study of gland ptosis versus volume. Aesthet Surg J 42:1222–1235. https://doi.org/10.1093/asj/sjac129
Sharobaro V, Alimova S, Telnova A, Shamanaeva L (2020) Ultrasound diagnosis of age-related involutional changes in the lower third of face and neck to determine treatment techniques. Pak J Med Sci https://doi.org/10.12669/pjms.37.1.3034
Alimova S, Sharobaro V, Yukhno A, Bondarenko E (2023) Possibilities of ultrasound examination in the assessment of age-related changes in the soft tissues of the face and neck: a review. Appl Sci 13:1128. https://doi.org/10.3390/app13021128
Dau M, Edalatpour A, Schulze R, Al-Nawas B, Alshihri A, Kammerer P (2017) Presurgical evaluation of bony implant sites using panoramic radiography and cone beam computed tomography—influence of medical education. Dentomaxillofac Radiol 46:2. https://doi.org/10.1259/dmfr.20160081
Acknowledgments
We would like to thank Editage (www.editage.com) for English language editing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest to disclose.
Ethical Approval
The study was conducted in accordance with the Declaration of Helsinki, and approved by local Ethics Committee of Pirogov Russian National Research Medical University (protocol code 170 and date of approval 18/12/2017).
Informed Consent
Informed consent was obtained from all subjects involved in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Alimova, S.M., Sharobaro, V.I., Avdeev, A.E. et al. Cone-Beam Computed Tomography for Objective Diagnosis of Age-Related Soft Tissue Changes in Lower Face and Neck. Aesth Plast Surg 47, 2370–2377 (2023). https://doi.org/10.1007/s00266-023-03401-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-023-03401-3