Abstract
Background
Melatonin is a widely used drug that can affect adipocyte inflammation, resulting in adipose tissue browning. Inducing the browning of white fat and changing the inflammatory microenvironment of early transplanted fat have positive effects on the retention rate of fat grafts. This study aimed to evaluate the effects of melatonin on fat graft retention, determine whether it is related to adipose tissue browning and the inflammatory microenvironment, and explore the underlying mechanisms.
Methods
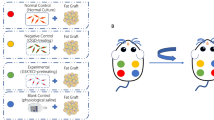
A C57BL/6 mice fat transplantation model was established. The mice were divided into a control group (ethanol), a high-dose group (40 mg/kg/day melatonin), a medium-dose group (20 mg/kg/day melatonin), and a low-dose group (10 mg/kg/day melatonin). They were also given oral gavage treatment for 2 weeks. The grafted fat was collected 2, 4, and 12 weeks after treatment.
Results
The medium-dose and high-dose melatonin groups had significantly higher fat graft retention rates than the control group at 12 weeks. The medium-dose melatonin group had smaller multilocular adipocytes, which enhanced the expression of uncoupling protein 1 and increased neovascularization in the grafted fat. The medium-dose group also had a higher distribution of M2 macrophages.
Conclusions
These findings suggest that melatonin administration can improve the retention of fat grafts through polarization of macrophages toward the anti-inflammatory type and induction of adipose tissue browning.
No Level Assigned
This journal requires that authors assign a level of evidence to each submission to which Evidence-Based Medicine rankings are applicable. This excludes Review Articles, Book Reviews, and manuscripts that concern Basic Science, Animal Studies, Cadaver Studies, and Experimental Studies. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.






Similar content being viewed by others
References
Hanson SE (2021) The future of fat grafting. Aesthet Surg J 41(Suppl 1):S69–S74
Zhu H, Quan Y, Wang J et al (2021) Improving low-density fat by condensing cellular and collagen content through a mechanical process: basic research and clinical applications. Plast Reconstr Surg 148(5):1029–1039
Chen X, Chen Y, Wang Z et al (2022) Adipose-derived stem cells regulate CD4+ T-cell-mediated macrophage polarization and fibrosis in fat grafting in a mouse model. Heliyon. 8(11):e11538
Kato H, Mineda K (2014) Eto H Degeneration, regeneration, and cicatrization after fat grafting: dynamic total tissue remodeling during the first 3 months. Plast Reconstr Surg 133(3):303e–313e
Kato H, Araki J, Doi K et al (2014) Normobaric hyperoxygenation enhances initial survival, regeneration, and final retention in fat grafting. Plast Reconstr Surg 134(5): 951–959
Kerfant N, Albacete G, Guernec A et al (2020) Fat grafting: early hypoxia, oxidative stress, and inflammation developing prior to injection. J Plast Reconstr Aesthet Surg 73:1775–1784
Zhang Y, Cai J, Zhou T et al (2018) Improved long-term volume retention of stromal vascular fraction gel grafting with enhanced angiogenesis and adipogenesis. Plast Reconstr Surg 141(5):676e–686e
Eto H, Kato H, Suga H et al (2012) The fate of adipocytes after nonvascularized fat grafting: evidence of early death and replacement of adipocytes. Plast Reconstr Surg 129(5):1081–1092
Suga H, Eto H, Aoi N et al (2010) Adipose tissue remodeling under ischemia: death of adipocytes and activation of stem/progenitor cells. Plast Reconstr Surg 126(6):1911–1923
Chen K, Xiong J, Xu S et al (2022) Adipose-derived stem cells exosomes improve fat graft survival by promoting prolipogenetic abilities through Wnt/beta-Catenin pathway. Stem Cells Int. 2022:5014895
Ghiasloo M, De Wilde L, Singh K et al (2021) A systematic review on extracellular vesicles-enriched fat grafting: a shifting paradigm. Aesthet Surg J 41(11):NP1695–NP1705
Jiang W, Cai J, Guan J et al (2021) Characterized the adipogenic capacity of adipose-derived stem cell, extracellular matrix, and microenvironment with fat components grafting. Front Cell Dev Biol. 9:723057
Chen Q, Liu S, Cao L, Yu M, Wang H (2022) Effects of macrophage regulation on fat grafting survival: Improvement, mechanisms, and potential application-A review. J Cosmet Dermatol 21(1):54–61
Shukla L, Yuan Y, Shayan R, Greening DW, Karnezis T (2020) Fat therapeutics: the clinical capacity of adipose-derived stem cells and exosomes for human disease and tissue regeneration. Front Pharmacol 11:158
Xia J, Zhu H, Zhu S et al (2021) Induced Beige adipocytes improved fat graft retention by promoting adipogenesis and angiogenesis. Plast Reconstr Surg 148(3):549–558
Cai J, Li B, Wang J et al (2018) Tamoxifen-prefabricated Beige adipose tissue improves fat graft survival in mice. Plast Reconstr Surg 141(4):930–940
Wankhade UD, Shen M, Yadav H, Thakali KM (2016) Novel browning agents, mechanisms, and therapeutic potentials of brown adipose tissue. Biomed Res Int 2016:2365609
Dang J, Yang J, Yu Z et al (2022) Bone marrow mesenchymal stem cells enhance angiogenesis and promote fat retention in fat grafting via polarized macrophages. Stem Cell Res Ther 13(1):52
Wu X, Qiao S, Wang W et al (2021) Melatonin prevents periimplantitis via suppression of TLR4/NF-kappaB. Acta Biomater 134:325–336
Chitimus DM, Popescu MR, Voiculescu SE et al (2020) Melatonin’s impact on antioxidative and anti-inflammatory reprogramming in homeostasis and disease. Biomolecules 10(9):1211
Manchester LC, Coto-Montes A, Boga JA et al (2015) Melatonin: an ancient molecule that makes oxygen metabolically tolerable. J Pineal Res 59(4):403–419
Zisapel N (2018) New perspectives on the role of melatonin in human sleep, circadian rhythms and their regulation. Br J Pharmacol 175(16):3190–3199
Liu Z, Gan L, Zhang T, Ren Q, Sun C (2018) Melatonin alleviates adipose inflammation through elevating alpha-ketoglutarate and diverting adipose-derived exosomes to macrophages in mice. J Pineal Res 64(1)
Xu Z, You W, Liu J, Wang Y, Shan T (2020) Elucidating the regulatory role of melatonin in brown, white, and Beige adipocytes. Adv Nutr 11(2):447–460
Cipolla-Neto J, Amaral FG, Afeche SC, Tan DX, Reiter RJ (2014) Melatonin, energy metabolism, and obesity: a review. J Pineal Res 56(4):371–381
Kim M, Lee SM, Jung J et al (2020) Pinealectomy increases thermogenesis and decreases lipogenesis. Mol Med Rep 22(5):4289–4297
Abdullahi A, Auger C, Stanojcic M et al (2019) Alternatively activated macrophages drive browning of white adipose tissue in burns. Ann Surg 269(3):554–563
Jimenez-Aranda A, Fernandez-Vazquez G, Campos D et al (2013) Melatonin induces browning of inguinal white adipose tissue in Zucker diabetic fatty rats. J Pineal Res 55(4):416–423
Xue Y, Petrovic N, Cao R et al (2009) Hypoxia-independent angiogenesis in adipose tissues during cold acclimation. Cell Metab 9(1):99–109
Mineda K, Kuno S, Kato H et al (2014) Chronic inflammation and progressive calcification as a result of fat necrosis: the worst outcome in fat grafting. Plast Reconstr Surg 133(5):1064–1072
Giralt M, Villarroya F (2013) White, brown, beige/brite: different adipose cells for different functions? Endocrinology 154(9):2992–3000
Qiu L, Zhang Z, Zheng H et al (2018) Browning of human subcutaneous adipose tissue after its transplantation in nude mice. Plast Reconstr Surg 142(2):392–400
de Souza CAP, Gallo CC, de Camargo LS et al (2019) Melatonin multiple effects on brown adipose tissue molecular machinery. J Pineal Res 66(2):e12549
Cypess AM (2022) Reassessing human adipose tissue. N Engl J Med 386(8):768–779
Cai J, Feng J, Liu K, Zhou S, Lu F (2018) Early Macrophage infiltration improves fat graft survival by inducing angiogenesis and hematopoietic stem cell recruitment. Plast Reconstr Surg 141(2):376–386
Wang Z, Chen Y, Zhu S et al (2020) The effects of macrophage-mediated inflammatory response to the donor site on long-term retention of a fat graft in the recipient site in a mice model. J Cell Physiol 235(12):10012–10023
Xia Y, Chen S, Zeng S et al (2019) Melatonin in macrophage biology: current understanding and future perspectives. J Pineal Res 66(2):e12547
Liu PS, Lin YW, Burton FH, Wei LN (2015) Injecting engineered anti-inflammatory macrophages therapeutically induces white adipose tissue browning and improves diet-induced insulin resistance. Adipocyte 4(2):123–128
Tan SS, Zhan W, Poon CJ et al (2018) Melatonin promotes survival of nonvascularized fat grafts and enhances the viability and migration of human adipose-derived stem cells via down-regulation of acute inflammatory cytokines. J Tissue Eng Regen Med 12(2):382–392
Phipps KD, Gebremeskel S, Gillis J et al (2015) Alternatively activated M2 macrophages improve autologous Fat Graft survival in a mouse model through induction of angiogenesis. Plast Reconstr Surg 135(1):140–149
Funding
This work was supported by the Foundation of National Natural Science Foundation of China (82202478).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest related to the publication of this manuscript.
Ethics Approval
All animal experiments were approved by the Institutional Animal Ethics Committee Laboratory, following the guidelines the Air Force Military Medical University (IACUC-20120561).
Informed Consent
As the subjects were animals, the principle of informed consent was not applicable to this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dang, J., Yu, Z., Wang, T. et al. Effects of Melatonin on Fat Graft Retention Through Browning of Adipose Tissue and Alternative Macrophage Polarization. Aesth Plast Surg 47, 1578–1586 (2023). https://doi.org/10.1007/s00266-022-03242-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-022-03242-6