Abstract
Background
It is very important to generate a comprehensive assessment of the fat grafting field due to the rapid growth of scientific literature. The current study aimed to use bibliometric analysis to evaluate fat grafting research qualitatively and quantitatively and determine the research hotspots and trends in this field.
Methods
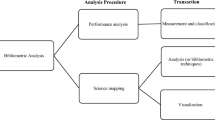
Publications on fat grafting research were extracted from the Web of Science core collection database. VOSviewer 1.6.18 was applied to perform the bibliometric analysis of these articles.
Results
A total of 2558 studies published by 594 different journals authored by 9097 researchers were contained in this study. In the co-authorship analysis, the bulk of the retrieved studies was conducted by the USA, followed by China, Italy and Japan, while the most productive institution, journal and author were Chinese Academy of Medicine Sciences, Plastic and Reconstruction Surgery and Klinger M, respectively. In the co-cited analysis, the most top cited author, journal, organization and country were Coleman Sr, Plastic and Reconstruction Surgery, New York University and the USA, respectively. The map of keywords occurrence revealed the most active research aspects were focused on “surgery,” “cell,” “breast reconstruction” and “survival” and the time overlay mapping showed that the most active research hotspots were “breast reconstruction” and “retention”.
Conclusions
The research hotspots include the following four aspects: aesthetic surgeries, cell-assisted lipotransfer, breast reconstruction and grafted fat survival. Breast fat grafting and volume retention may be trends in the future. We are willing to provide more beneficial data to contribute valuable research for the fat grafting through this study.
Level of Evidence III
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.








Similar content being viewed by others
References
Billings E Jr, May JW Jr (1989) Historical review and present status of free fat graft auto transplantation in plastic and reconstructive surgery. Plast Reconstr Surg 83(2):368–81
Chen C, Dubin R, Kim MC (2014) Emerging trends and new developments in regenerative medicine: a scientometric update (2000–2014). Expert Opin Biol Ther 14(9):1295–1317
van Eck NJ, Waltman L (2010) Software survey: VOSviewer, a computer program for bibliometric mapping. Scientometrics 84(2):523–538
van Eck NJ, Waltman L (2017) Citation-based clustering of publications using CitNetExplorer and VOSviewer. Scientometrics 111(2):1053–1070
Joyce CW et al (2015) Fat grafting: a citation analysis of the seminal articles. Plast Reconstr Surg Glob Open 3(1):e295
Fraser JF, Hultman CS (2010) America’s fertile frontier: how America surpassed Britain in the development and growth of plastic surgery during the interwar years of 1920–1940. Ann Plast Surg 64(5):610–613
Yoshimura K et al (2008) Cell-assisted lipotransfer for cosmetic breast augmentation: supportive use of adipose-derived stem/stromal cells. Aesthetic Plast Surg 32:48–55 (discussion 56-7)
Miranville A et al (2004) Improvement of postnatal neovascularization by human adipose tissue-derived stem cells. Circulation 110(3):349–355
Masuda T, Furue M, Matsuda T (2004) Novel strategy for soft tissue augmentation based on transplantation of fragmented omentum and preadipocytes. Tissue Eng 10(11–12):1672–1683
Planat-Benard V et al (2004) Plasticity of human adipose lineage cells toward endothelial cells: physiological and therapeutic perspectives. Circulation 109(5):656–663
Rehman J et al (2004) Secretion of angiogenic and antiapoptotic factors by human adipose stromal cells. Circulation 109(10):1292–1298
Matsumoto D et al (2006) Cell-assisted lipotransfer-supportive use of human adipose-derived cells for soft tissue augmentation with lipoinjection. Tissue Eng 12(12):3375–3382
Bourin P et al (2013) Stromal cells from the adipose tissue-derived stromal vascular fraction and culture expanded adipose tissue-derived stromal/stem cells: a joint statement of the international federation for adipose therapeutics and science (IFATS) and the international society for cellular therapy (ISCT). Cytotherapy 15(6):641–648
Zhou B et al (2011) Administering human adipose-derived mesenchymal stem cells to prevent and treat experimental arthritis. Clin Immunol 141(3):328–337
Fawzy El-Sayed KM et al (2013) Adult mesenchymal stem cells explored in the dental field. Adv Biochem Eng Biotechnol 130:89–103
Yoo KH et al (2009) Comparison of immunomodulatory properties of mesenchymal stem cells derived from adult human tissues. Cell Immunol 259(2):150–156
Puissant B et al (2005) Immunomodulatory effect of human adipose tissue-derived adult stem cells: comparison with bone marrow mesenchymal stem cells. Br J Haematol 129(1):118–129
Okura H et al (2012) Intracoronary artery transplantation of cardiomyoblast-like cells from human adipose tissue-derived multi-lineage progenitor cells improve left ventricular dysfunction and survival in a swine model of chronic myocardial infarction. Biochem Biophys Res Commun 425(4):859–865
Oh JS et al (2012) Transplantation of an adipose stem cell cluster in a spinal cord injury. NeuroReport 23(5):277–282
Illouz YG (1983) Body contouring by lipolysis- A 5-year experience with over 3000 cases. Plast Reconstr Surg 72(5):591–597
Coleman SR (1995) Long-term survival of fat transplants- controlled demonstrations. Aesthetic Plast Surg 19(5):421–425
Coleman SR (2001) Structural fat grafts: the ideal filler? Clin Plast Surg 28(1):111–119
Van RL, Bayliss CE, Roncari DA (1976) Cytological and enzymological characterization of adult human adipocyte precursors in culture. J Clin Invest 58(3):699–704
Zuk PA et al (2001) Multilineage cells from human adipose tissue- implications for cell-based therapies. Tissue Eng 7(2):211–228
Zeltzer AA, Tonnard PL, Verpaele AM (2012) Sharp-needle intradermal fat grafting (SNIF). Aesthet Surg J 32(5):554–561
Riesco B et al (2018) Autologous fat transfer with SEFFI (superficial enhanced fluid fat injection) technique in periocular reconstruction. Orbit 37(3):191–195
Trivisonno A et al (2017) Facial skin rejuvenation by autologous dermal microfat transfer in photoaged patients: clinical evaluation and skin surface digital profilometry analysis. J Plast Reconstr Aesthet Surg 70(8):1118–1128
Gennai A et al (2017) Skin rejuvenation and volume enhancement with the micro superficial enhanced fluid fat injection (M-SEFFI) for skin aging of the periocular and perioral regions. Aesthet Surg J 37(1):14–23
Bernardini FP et al (2015) Superficial enhanced fluid fat injection (SEFFI) to correct volume defects and skin aging of the face and periocular region. Aesthet Surg J 35(5):504–515
Tonnard P et al (2013) Nanofat grafting- basic research and clinical applications. Plast Reconstr Surg 132(4):1017–1026
Tonnard P, Verpaele A, Carvas M (2020) Fat grafting for facial rejuvenation with nanofat grafts. Clin Plast Surg 47(1):53–62
Uyulmaz S et al (2018) Nanofat grafting for scar treatment and skin quality improvement. Aesthet Surg J 38(4):421–428
Menkes S et al (2020) Subcutaneous injections of nanofat adipose-derived stem cell grafting in facial rejuvenation. Plast Reconstr Surg Glob Open 8(1):e2550
Silverstein MJ et al (1988) Breast cancer in women after augmentation mammoplasty. Arch Surg 123(6):681–685
Bircoll M, Novack BH (1987) Autologous fat transplantation employing liposuction techniques. Ann Plast Surg 18(4):327–329
Rubin E (2011) Breast imaging considerations in fat grafting to the breast. Plast Reconstr Surg 128(5):570e–571e
Coleman SR, Saboeiro AP (2007) Fat grafting to the breast revisited: safety and efficacy. Plast Reconstr Surg 119(3):775–85 (discussion 786-7)
Gutowski KA, Force AFGT (2009) Current applications and safety of autologous fat grafts: a report of the ASPS fat graft task force. Plast Reconstr Surg 124(1):272–280
Illouz YG, Sterodimas A (2009) Autologous fat transplantation to the breast: a personal technique with 25 years of experience. Aesthetic Plast Surg 33(5):706–715
Kanchwala SK et al (2009) Autologous fat grafting to the reconstructed breast: the management of acquired contour deformities. Plast Reconstr Surg 124(2):409–418
Maione L et al (2014) Autologous fat graft in postmastectomy pain syndrome following breast conservative surgery and radiotherapy. Aesthetic Plast Surg 38(3):528–532
Khouri RK et al (2014) Aesthetic applications of Brava-assisted megavolume fat grafting to the breasts: a 9-year, 476-patient, multicenter experience. Plast Reconstr Surg 133(4):796–807
Serra-Renom JM, Munoz-Olmo JL, Serra-Mestre JM (2010) Fat grafting in postmastectomy breast reconstruction with expanders and prostheses in patients who have received radiotherapy: formation of new subcutaneous tissue. Plast Reconstr Surg 125(1):12–18
Missana MC et al (2007) Autologous fat transfer in reconstructive breast surgery: indications, technique and results. Eur J Surg Oncol 33(6):685–690
Sinna R et al (2010) Breast fat grafting (lipomodelling) after extended latissimus dorsi flap breast reconstruction: a preliminary report of 200 consecutive cases. J Plast Reconstr Aesthet Surg 63(11):1769–1777
Khouri R, Del Vecchio D (2009) Breast reconstruction and augmentation using pre-expansion and autologous fat transplantation. Clin Plast Surg 36:269–80
Delay E et al (2009) Fat injection to the breast- technique, results, and indications based on 880 procedures over 10 years. Aesthet Surg J 29(5):360–376
Nishimura T et al (2000) Microvascular angiogenesis and apoptosis in the survival of free fat grafts. Laryngoscope 110(8):1333–1338
Hong KY et al (2018) The fate of the adipose-derived stromal cells during angiogenesis and adipogenesis after cell-assisted lipotransfer. Plast Reconstr Surg 141(2):365–375
Paik KJ et al (2015) Studies in fat grafting: part V. cell-assisted lipotransfer to enhance fat graft retention is dose dependent. Plast Reconstr Surg 136(1):67–75
Suga H et al (2014) Paracrine mechanism of angiogenesis in adipose-derived stem cell transplantation. Ann Plast Surg 72(2):234–241
Kølle S et al (2013) Enrichment of autologous fat grafts with ex-vivo expanded adipose tissue-derived stem cells for graft survival a randomised placebo-controlled trial. Lancet 28:1113–20
Chung MT et al (2013) Isolation of human adipose-derived stromal cells using laser-assisted liposuction and their therapeutic potential in regenerative medicine. Stem Cells Transl Med 2(10):808–817
Yao Y et al (2017) Adipose extracellular matrix/stromal vascular fraction gel: a novel adipose tissue-derived injectable for stem cell therapy. Plast Reconstr Surg 139(4):867–879
Kling RE et al (2013) Trends in autologous fat grafting to the breast: a national survey of the American society of plastic surgeons. Plast Reconstr Surg 132(1):35–46
Mofid MM et al (2017) Report on mortality from gluteal fat grafting: recommendations from the ASERF task force. Aesthet Surg J 37(7):796–806
Rigotti G et al (2007) Clinical treatment of radiotherapy tissue damage by lipoaspirate transplant: a healing process mediated by adipose-derived adult stem cells. Plast Reconstr Surg 119(5):1409–1422
Jackson IT et al (2001) A successful long-term method of fat grafting: recontouring of a large subcutaneous postradiation thigh defect with autologous fat transplantation. Aesthetic Plast Surg 25(3):165–169
Cantarella G et al (2005) Vocal fold augmentation by autologous fat injection with lipostructure procedure. Otolaryngol Head Neck Surg 132(2):239–243
Garcia-Olmo D et al (2003) Autologous stem cell transplantation for treatment of rectovaginal fistula in perianal Crohn’s disease: a new cell-based therapy. Int J Colorectal Dis 18(5):451–454
Garcia-Olmo D et al (2005) A phase I clinical trial of the treatment of Crohn’s fistula by adipose mesenchymal stem cell transplantation. Dis Colon Rectum 48(7):1416–1423
Lendeckel S et al (2004) Autologous stem cells (adipose) and fibrin glue used to treat widespread traumatic calvarial defects: case report. J Craniomaxillofac Surg 32(6):370–373
Peer LA (1950) Loss of weight and volume in human fat grafts with postulation of a “cell survival theory.” Plast Reconstr Surg 5:217–230
Funding
This research received no funding from any public or private organizations/institutions.
Author information
Authors and Affiliations
Contributions
Conceptualization was done by BL and CR; investigation was carried out by CR; data curation was done by BL and JM; writing—original draft preparation was done by BL; writing—review and editing were done by CR and JM; supervision and project administration were done by MZ. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest to disclose.
Ethical Approval
No ethical approval is required for such studies, as patients are not involved. The Ethics Committee of the Second Affiliation Hospital of Dalian Medical University approved this study.
Human or Animal Rights
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, informed consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, B., Ri, C., Mao, J. et al. A Bibliometric and Visualization Analysis on the Research of Fat Grafting from 1945 to 2021. Aesth Plast Surg 47, 397–411 (2023). https://doi.org/10.1007/s00266-022-03137-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-022-03137-6