Abstract
Background
Outcomes of gender-affirming chest surgery can be variable. Placement of nipple-areolar complexes and orientation of scars can drastically affect the aesthetic outcomes of these procedures, as may observer gender identity. Here, we compared attention and perception of outcomes following gender-affirming chest surgery between laypersons, based on gender identity.
Methods
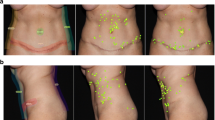
Transgender and cisgender participants were enrolled and shown images of surgery naïve chests and postoperative masculinized and feminized chests, blinded to the gender identity of the photographed subject. Gaze data were captured using the Tobii X2 60 eye-tracking device. Participants scored the perceived gender and aesthetic appearance of each image.
Results
Eighteen cisgender and 14 transgender participants were enrolled. When viewing male chests, transgender participants spent significantly longer fixated on the nipples (naïve: 802 vs. 395 ms; p = 0.02, masculinized: 940 vs. 692 ms, p = 0.002). For masculinized chests, cisgender participants spent significantly longer fixated on the inframammary scar (483 vs. 391 ms; p = 0.04). On images of feminized chests, transgender participants spent longer viewing the nipples when compared to cisgender participants (1017 vs. 847 ms; p = 0.04). Cisgender viewers spent longer fixating on the postoperative scar on feminized chests (113 vs. 59 ms; p = 0.02) and also viewed feminized chests as significantly more masculine and masculinized chests as more feminine, when compared to transgender participants (p < 0.05).
Conclusions
This is the first study to use eye-tracking to assess how laypersons assess chests for gender determination. The findings suggest that observer gender identity has an effect on areas of focus and gender perception of chests that underwent gender-affirmation surgery.
Level of Evidence III
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine Ratings, please refer to Table of Contents or online Instructions to Authors www.springer.com/00266.


Similar content being viewed by others
References
van Boerum MS, Salibian AA, Bluebond-langner R, Agarwal C (2019) Chest and facial surgery for the transgender patient. Transl Androl Urol 8:219–227
Morrison SD, Wilson SC, Mosser SW (2018) Breast and body contouring for transgender and gender nonconforming individuals. Clin Plast Surg 45:333–342. https://doi.org/10.1016/j.cps.2018.03.015
Miller TJ, Wilson SC, Massie JP et al (2019) Breast augmentation in male-to-female transgender patients: technical considerations and outcomes. JPRAS Open 21:63–74. https://doi.org/10.1016/j.jpra.2019.03.003
Hughes SM, Gallup GG (2003) Sex differences in morphological predictors of sexual behavior. Evol Hum Behav 24:173–178. https://doi.org/10.1016/S1090-5138(02)00149-6
Fan J, Dai W, Liu F, Wu J (2005) Visual perception of male body attractiveness. Proc Biol Sci 272:219–226. https://doi.org/10.1098/rspb.2004.2922
Walzer NK, Rivera A, Wright L, Agarwal CA (2017) Female-to-male chest reconstruction. Ann Plast Surg 79:259–263. https://doi.org/10.1097/SAP.0000000000001099
Salim AM, Deschamps-braly JC (2019) Current concepts in feminizing gender surgery. Plast Reconstr Surg. https://doi.org/10.1097/PRS.0000000000005595
Lane M, Ives GC, Sluiter EC et al (2015) Trends in gender-affirming surgery in insured patients in the United States. Plast Reconstr Surg Glob Open. https://doi.org/10.1097/GOX.0000000000001738
Sutcliffe PA, Dixon S, Akehurst RL et al (2009) Evaluation of surgical procedures for sex reassignment: a systematic review. Br J Plast Surg 62:294–306. https://doi.org/10.1016/j.bjps.2007.12.009
Frison E, Sessiecq Q, Al MK (2012) Patient satisfaction with breasts and psychosocial, sexual, and physical well-being after breast augmentation in male-to-female transsexuals. Plast Reconstr Surg. https://doi.org/10.1097/01.prs.0000434415.70711.49
Klassen AF, McEvenue G, Wang Y et al (2020) The BODY-Q chest module: further validation in a Canadian chest masculinization surgery sample. Aesthet Surg J. https://doi.org/10.1093/asj/sjaa224
Klassen AF, Kaur M, Poulsen L et al (2018) Development of the BODY-Q chest module evaluating outcomes following chest contouring surgery. Plast Reconstr Surg 142:1600–1608. https://doi.org/10.1097/PRS.0000000000004978
Nolan IT, Hazen A, Morrison SD (2018) On the gender identity of breast patients. JAMA Surg 153:1164. https://doi.org/10.1001/jamasurg.2018.3227
Olson-Kennedy J, Warus J, Okonta V et al (2018) Chest Reconstruction and chest dysphoria in transmasculine minors and young adults: comparisons of nonsurgical and postsurgical cohorts. JAMA Pediatr 172:431–436. https://doi.org/10.1001/jamapediatrics.2017.5440
Klassen AF, Kaur M, Johnson N et al (2018) International phase I study protocol to develop a patient-reported outcome measure for adolescents and adults receiving gender-affirming treatments (the GENDER-Q). BMJ Open 8:e025435. https://doi.org/10.1136/bmjopen-2018-025435
Morrison SD, Massie JP, Crowe CS, Smith JR (2018) Patient-reported outcomes needed for chest masculinization. Ann Plast Surg 80:90–91. https://doi.org/10.1097/SAP.0000000000001130
Cai LZ, Paro JAM, Lee GK, Nazerali RS (2018) Where do we look? assessing gaze patterns in breast reconstructive surgery with eye-tracking technology. Plast Reconstr Surg 141:331e–340e. https://doi.org/10.1097/PRS.0000000000004106
Cai L, Kwong J, Azad A et al (2019) Where do we look? assessing gaze patterns in cosmetic face-lift surgery with eye tracking technology. Plast Reconstr Surg 144:63–70. https://doi.org/10.1097/PRS.0000000000005700
Peterson MF, Eckstein MP (2013) Individual differences in eye movements during face identification reflect observer-specific optimal points of fixation. Psychol Sci 24:1216–1225. https://doi.org/10.1177/0956797612471684
American Society of Plastic Surgeon (2021) Before & after photos. https://www.plasticsurgery.org/photo-gallery. Accessed Jan 2021
Olsen A (2012) The Tobii I-VT fixation filter. www.tobiipro.com. Accessed Oct 2020
Boardman JP, Fletcher-Watson S (2017) What can eye-tracking tell us? Arch Dis Child 102:301–302. https://doi.org/10.1136/archdischild-2016-311693
Dindaroğlu F, Doğan S, Amado S, Doğan E (2017) Visual perception of faces with unilateral and bilateral cleft lip and palate: an eye-tracking study. Orthod Craniofac Res 20:44–54. https://doi.org/10.1111/ocr.12140
Adetayo AM, James O, Adeyemo WL et al (2018) Unilateral cleft lip repair: a comparison of treatment outcome with two surgical techniques using quantitative (anthropometry) assessment. J Korean Assoc Oral Maxillofac Surg 44:3. https://doi.org/10.5125/jkaoms.2018.44.1.3
Mallucci P, Branford OA (2012) Concepts in aesthetic breast dimensions: analysis of the ideal breast. J Plast Reconstr Aesthet Surg 65:8–16. https://doi.org/10.1016/j.bjps.2011.08.006
Lewin R, Amoroso M, Plate N et al (2020) The aesthetically ideal position of the nipple-areola complex on the breast. Aesthet Plast Surg 44:1130–1138. https://doi.org/10.1007/s00266-020-01814-y
Ayyala HS, Mukherjee TJ, Le T-M et al (2020) A three-step technique for optimal nipple position in transgender chest masculinization. Aesthet Surg J. https://doi.org/10.1093/asj/sjaa150
Top H, Balta S (2017) Transsexual mastectomy: selection of appropriate technique according to breast characteristics. Balkan Med J 34:147–155. https://doi.org/10.4274/balkanmedj.2016.0093
Maas M, Howell AC, Gould DJ, Ray EC (2020) The ideal male nipple-areola complex: a critical review of the literature and discussion of surgical techniques for female-to-male gender-confirming surgery. Ann Plast Surg 84:334–340. https://doi.org/10.1097/SAP.0000000000002018
Wilson SC, Morrison SD, Anzai L et al (2018) Masculinizing top surgery: a systematic review of techniques and outcomes. Ann Plast Surg 80:679–683. https://doi.org/10.1097/SAP.0000000000001354
Tanini S, Calabrese S, Lo Russo G (2020) The importance of nipple-areola complex position in chest masculinization surgery. Aesthet Plast Surg. https://doi.org/10.1007/s00266-020-01707-0
Sun J, Mu D, Liu C et al (2019) The comparison of scars in breast implantation surgery with inframammary fold incision versus axillary incision: a prospective cohort study in Chinese patients. Aesthet Plast Surg 43:328–335. https://doi.org/10.1007/s00266-018-1299-3
Randquist C, Por YC, Yeow V et al (2018) Breast augmentation surgery using an inframammary fold incision in Southeast Asian women: patient-reported outcomes. Arch Plast Surg 45:367–374. https://doi.org/10.5999/aps.2018.00045
Bekeny JC, Zolper EG, Fan KL, Del Corral G (2020) Breast augmentation for transfeminine patients: methods, complications, and outcomes. Gland Surg 9:788–796
McEvenue G, Xu FZ, Cai R, McLean H (2018) Female-to-male gender affirming top surgery: a single surgeon’s 15-year retrospective review and treatment algorithm. Aesthet Surg J 38:49–57. https://doi.org/10.1093/asj/sjx116
Broussard KA, Warner RH (2019) Gender nonconformity is perceived differently for cisgender and transgender targets. Sex Roles 80:409–428. https://doi.org/10.1007/s11199-018-0947-z
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None declared
Ethical Approval
Institutional review board approval was obtained for the study.
Informed Consent
All patients provided informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
US Professional Association for Transgender Health 2019, Washington D.C. and California Society of Plastic Surgeons Annual Meeting 2020, Virtual Meeting.
Rights and permissions
About this article
Cite this article
Martin, S.A., Patel, V., Morrison, S.D. et al. Assessing Gender-Affirming Chest Surgery Outcomes: Does Gender Identity Alter Gaze?. Aesth Plast Surg 45, 1860–1868 (2021). https://doi.org/10.1007/s00266-021-02378-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-021-02378-1