Abstract
Background
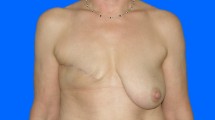
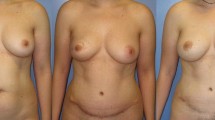
Autologous lipotransfer has increasingly become popular for breast reconstruction. Moreover, owing to the emergence of information regarding the efficacy of stromal vascular fraction (SVF) in terms of oncological safety and survival rate, procedures based on cell-assisted lipotransfer (CAL) have been widely employed recently. However, quantitative data of CAL with SVF are lacking. We evaluated the efficacy of CAL using SVF on survival rate in breast reconstruction.
Methods
A 12-month prospective study was conducted for 20 patients (20 breasts) requiring breast asymmetry correction due to volume deficit following autologous breast reconstruction using a transverse rectus abdominis myocutaneous flap or latissimus dorsi flap after total mastectomy. After the patients were equally divided into two groups—fat graft with SVF (Group 1, n = 10) and without SVF (Group 2, n = 10)—, the variance of breast volume was measured using three-dimensional scanning to analyze fat graft retention rate. Moreover, patient satisfaction and complications were investigated.
Results
Fat graft retention rate was higher in Group 1 than in Group 2 at both postoperative 6 months (73.8% vs. 62.2%; p = 0.03) and 12 months (65.4% vs. 48.4%; p = 0.03). Group 1 showed higher patient satisfaction. Regarding complications, fat necrosis occurred in 1 patient each in both groups. However, locoregional recurrence was not observed in any patient during follow-up.
Conclusions
CAL with SVF is effective in increasing survival rates of autologous fat grafts for correction of volume deficit after breast reconstruction. Moreover, it is associated with improved patient satisfaction in terms of the esthetic aspect.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266





Similar content being viewed by others
References
Coleman SR (1997) Facial recontouring with lipostructure. Clin Plast Surg 24(2):347–367
Billings E Jr, May JW Jr (1989) Historical review and present status of free fat graft autotransplantation in plastic and reconstructive surgery. Plast Reconstr Surg 83(2):368–381
Delay E, Garson S, Tousson G et al (2009) Fat injection to the breast: technique, results, and indications based on 880 procedures over 10 years. Aesth Surg J 29:360–376
Khouri RK et al (2012) Brava and autologous fat transfer is a safe and effective breast augmentation alternative: results of a 6-year, 81-patient prospective Multicenter study. Plast Reconstr Surg 129(5):1173–1187
Domenis R et al (2015) Adipose tissue derived stem cells: in vitro and in vivo analysis of a standard and three commercially available cell-assisted lipotransfer techniques. Stem Cell Res Ther 6(1):2
Yoshimura K, Sato K, Aoi N, Kurita M, Hirohi T, Harii K (2008) Cell-assisted lipotransfer for cosmetic breast augmentation: Supportive use of adipose-derived stem/stromal cells. Aesth Plast Surg 32:48–55
Gentile P, Scioli MG, Orlandi A, Cervelli V (2015) Breast reconstruction with enhanced stromal vascular fraction fat grafting: what is the best method. Plast Reconstr Surg Glob Open. 3(6):e406
Mandel K, Yang Y, Schambach A et al (2013) Mesenchymal stem cells directly interact with breast cancer cells and promote tumor cell growth in vitro and in vivo. Stem Cells Dev 22:3114–3127
Rowan BG, Gimble JM, Sheng M et al (2014) Human adipose tissue-derived stromal/stem cells promote migration and early metastasis of triple negative breast cancer xenografts. PLoS ONE 9:e89595
Zimmerlin L, Donnenberg AD, Rubin JP et al (2011) Regenerative therapy and cancer: in vitro and in vivo studies of the interaction between adipose-derived stem cells and breast cancer cells from clinical isolates. Tissue Eng Part A 17:93–106
Largo RD, Tchang LA, Mele V et al (2014) Efficacy, safety and complications of autologous fat grafting to healthy breast tissue: a systematic review. J Plast Reconstr Aesth Surg 67(4):437–448
Claro F Jr, Figueiredo JC, Zampar AG, Pinto-Neto AM (2012) Applicability and safety of autologous fat for reconstruction of the breast. Br J Surg 99:768–780
Lee JS et al (2019) Effects of stromal vascular fraction on breast cancer growth and fat engraftment in NOD/SCID mice. Aesth Plast Surg 43(2):498–513
Tissiani LAL, Alonso N (2016) A prospective and controlled clinical trial on stromal vascular fraction enriched fat grafts in secondary breast reconstruction. Stem Cells Int 2:1–12
Krastev TK, Jonasse Y, Kon M (2013) Oncological safety of autologous lipoaspirate grafting in breast cancer patients: a systematic review. Ann Surg Oncol 20(1):111–119
Riggio E, Bordoni D, Nava MB (2013) Oncologic surveillance of breast cancer patients after lipofilling. Aesth Plast Surg 37(4):728–735
Czerny V (1895) Plastischer ersatz der brustdruse durch ein lipom. Zent Chir 27:72
Bircoll M (1987) Cosmetic breast augmentation utilizing autologous fat and liposuction techniques. Plast Reconstr Surg. 79(2):267–271. https://doi.org/10.1097/00006534-198702000-00022
Coleman SR (2001) Structural fat grafts: the ideal filler? Clin Plast surg 28:111–119
Hou WK, Xu YX, Yu T, Zhang L, Zhang WW, Fu CL, Sun Y, Wu Q, Chen L (2007) Adipocytokines and breast cancer risk. Chin Med J (Engl). 120(18):1592–1596
Lohsiriwat V, Curigliano G, Rietjens M, Goldhirsch A, Petit JY (2011) Autologous fat transplantation in patients with breast cancer: "silencing" or "fueling" cancer recurrence? Breast 20(4):351–357
Kronowitz SJ, Mandujano CC, Liu J, Kuerer HM, Smith B, Garvey P, Jagsi R, Hsu L, Hanson S, Valero V (2016) Lipofilling of the breast does not increase the risk of recurrence of breast cancer: a matched controlled study. Plast Reconstr Surg 137(2):385–393
Gale KL, Rakha EA, Ball G, Tan VK, McCulley SJ, Macmillan RD (2015) A case-controlled study of the oncologic safety of fat grafting. Plast Reconstr Surg 135(5):1263–1275
Herold C, Ueberreiter K, Busche MN, Vogt PM (2013) Autologous fat transplantation: volumetric tools for estimation of volume survival—a systematic review. Aesth Plast Surg 37:380–387
Matsumoto D, Sato K, Gonda K et al (2006) Cell-assisted lipotransfer:supportive use of human adipose-derived cellsfor soft tissue augmentation with lipoinjection. Tissue Eng. https://doi.org/10.1089/ten.2006.12.3375
Jung HK, Kim CH, Song SY (2016) Prospective 1-year follow-up study of breast augmentation by cell-assisted lipotransfer. Aesth Surg J 36(2):179–190
Choi M, Small K, Levovitz C, Lee C, Fadl A, Karp NS (2013) The volumetric analysis of fat graft survival in breast reconstruction. Plast Reconstr Surg 131(2):185–191
Losken A, Pinell XA, Sikoro K, Yezhelyev MV, Anderson E, Carlson GW (2011) Autologous fat grafting in secondary breast reconstruction. Ann Plast Surg 66(5):518–522
Funding
The authors received no specific funding for this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all participants.
Human or Animal Rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jeon, H.J., Choi, D.H., Lee, J.H. et al. A Prospective Study of the Efficacy of Cell-Assisted Lipotransfer with Stromal Vascular Fraction to Correct Contour Deformities of the Autologous Reconstructed Breast. Aesth Plast Surg 45, 853–863 (2021). https://doi.org/10.1007/s00266-020-01981-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-020-01981-y