Abstract
Background
Diameters greater than 1.5 mm are considered one of the generally accepted criteria for utilizing superficial epigastric artery (SIEA) flaps for breast reconstruction. However, this standard fails to consider individual differences among patients or deep inferior epigastric perforator (DIEP) perfusion of the same angiosome as the SIEA. This study combined the SIEA system with the DIEP system and explored the relationship between the two systems and body mass index (BMI) to theoretically provide a reference for flap choice in the preoperative surgical plan.
Methods
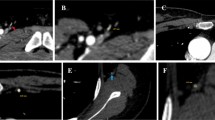
This study analysed preoperative computed tomography angiography (CTA) data from patients who received systematically postoperative treatment for unilateral breast cancer and were scheduled for breast reconstruction from 2013 to 2018 in our centre. All patients included had no past medical history that might have influenced the diameter of the SIEA, and their CTA data showed the presence of SIEA.
Results
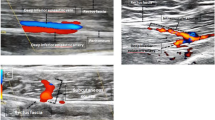
Twenty-five females with a mean BMI of 23.6 ± 3.3 kg/m2 were included. A total of 30 hemi-abdomens identified with the SIEA were assessed. The measured mean diameter of the SIEA was 1.63 ± 0.55 mm, showing a highly linear correlation with BMI (r = 0.73, p < 0.001), while the maximum diameter of the deep inferior epigastric perforator (DIEPmax) and the number of dominant perforators originating from the deep inferior epigastric artery (DIEA) were not related to BMI. It was analysed from the equation between the calibre of the SIEA and BMI that when the BMI was greater than or equal to 24 kg/m2, the minimum diameter of the SIEA was at least 1.5 mm; when the BMI was 25 kg/m2, the diameter of the SIEA was, at most, 2.0 mm. Based on the linear correlation described above, we proposed that if the diameter of the SIEA was greater than or equal to 2.0 mm, a BMI ≥ 25 kg/m2 could be fully guaranteed. In terms of the advantageous single pedicle for reconstruction, the ratio of the SIEA diameter to DIEPmax (SIEA/DIEPmax) showed a significant linear correlation with BMI (r = 0.82, p < 0.001), and when the BMI was greater than or equal to 25 kg/m2, the lower limit of its predicted value was above 1.0; in other words, the SIEA diameter was advantageous compared with DIEPmax for the use of a single pedicle. In terms of perfusion, the SIEA system was positively correlated with BMI (p < 0.001), while the DIEP system was not. The difference in perfusion level between the SIEA and DIEP systems showed a positive correlation with BMI (p = 0.001), while the sum of the two systems only tended to be correlated, without statistical significance (p = 0.06).
Conclusions
For patients with a BMI ≥ 25 kg/m2 or an SIEA diameter ≥ 2.0 mm, application of an SIEA flap is theoretically a preferable choice in preoperative surgical planning for breast reconstruction. And the patients should meet two conditions: the first one is the absence of past medical history that might potentially influence the diameter of the SIEA; the second is the presence of the SIEA, which has already been shown by the preoperative imaging data. Through perfusion-related studies, we propose that the SIEA is likely a compensatory vessel that is inclined to present in people with larger BMIs.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.



Similar content being viewed by others
References
Rozen WM, Chubb D, Grinsell D et al (2010) The variability of the superficial inferior epigastric artery (SIEA) and its angiosome: a clinical anatomical study. Microsurgery 30:386–391
Charlotte H, Martina M, Eugen HF et al (2008) Interindividual variability of the SIEA Angiosome: effects on operative strategies in breast reconstruction. Plast Reconstr Surg 122:1612–1620
Park JE, Shenaq DS, Silva AK et al (2016) Breast reconstruction with SIEA flaps: a single-institution experience with 145 free flaps. Plast Reconstr Surg 137:1682
Fukaya E, Kuwatsuru R, Iimura H et al (2011) Imaging of the superficial inferior epigastric vascular anatomy and preoperative planning for the SIEA flap using MDCTA. J Plast Reconstr Aesth Surg JPRAS 64:63–68
Dorafshar AH, Januszyk M, Song DH (2010) Anatomical and technical tips for use of the superficial inferior epigastric artery (SIEA) flap in breast reconstructive surgery. J Reconstr Microsurg 26:381–389
Akita S, Yamaji Y, Tokumoto H et al (2018) Intraoperative objective evaluation of venous congestion in deep epigastric artery perforator flap breast reconstruction: a pilot study. Microsurgery 38:407–412
Rozen WM, Chubb D, Whitaker IS et al (2011) The importance of the superficial venous anatomy of the abdominal wall in planning a superficial inferior epigastric artery (SIEA) flap: case report and clinical study. Microsurgery 31:454–457
Spiegel AJ, Khan FN (2007) An Intraoperative algorithm for use of the SIEA flap for breast reconstruction. Plast Reconstr Surg 120:1450–1459
Henry FP, Butler DP, Wood SH et al (2017) Predicting and planning for SIEA flap utilisation in breast reconstruction: an algorithm combining pre-operative computed tomography analysis and intra-operative angiosome assessment. J Plast Reconstr Aesthet Surg 70:795
Angelini F, Herzel S (2008) Interindividual variability of the SIEA Angiosome: effects on operative strategies in breast reconstruction. Plast Reconstr Surg 122:1612–1620
Gusenoff JA, Devin C, Carolyn DLC et al (2008) Superficial inferior epigastric vessels in the massive weight loss population: implications for breast reconstruction. Plast Reconstr Surg 122:1621–1626
Coroneos CJ, Heller AM, Voineskos SH et al (2015) SIEA versus DIEP arterial complications: a cohort study. Plast Reconstr Surg 135:802e
Gregorič M, Flis V, Milotić F et al (2011) Delaying the superficial inferior epigastric artery flap: a solution to the problem of the small calibre of the donor artery. J Plast Reconstr Aesthet Surg 64:1181–1186
Griffiths M, Chae MP, Rozen WM (2016) Indocyanine green-based fluorescent angiography in breast reconstruction. Gland Surg 5:133–149
Miyamoto S, Fujiki M (2016) Criteria for the use of the SIEA flap for breast reconstruction. Plast Reconstr Surg 137:474e
Ludescher B, Rommel M, Willmer T et al (2011) Subcutaneous adipose tissue thickness in adults—correlation with BMI and recommendations for pen needle lengths for subcutaneous self-injection. Clin Endocrinol 75:786–790
Lazzer S, Bedogni G, Lafortuna CL et al (2010) Relationship between basal metabolic rate, gender, age, and body composition in 8,780 white obese subjects. Obesity (Silver Spring, Md.) 18:71–78
Andree C, Langer S, Seidenstuecker K et al (2013) A single center prospective study of bilateral breast reconstruction with free abdominal flaps: a critical analyses of 144 patients. Med Sci Monit 19:467–474
Roy M, Sebastiampillai S, Zhong T et al (2019) Synergistic interaction increases complication rates following microvascular breast reconstruction. Plast Reconstr Surg 144:1e–8e
Alstrup T, Christensen BO, Damsgaard TE (2018) ICG angiography in immediate and delayed autologous breast reconstructions: peroperative evaluation and postoperative outcomes. J Plast Surg Hand Surg 52:307–311
Frey JD, Salibian AA, Choi M et al (2019) The importance of tissue perfusion in reconstructive breast surgery. Plast Reconstr Surg 144:21S–29S
Funding
No financial support or benefits have been received by the author or any co-author to accomplish this manuscript
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This study was approved by the research ethics committee.
Informed Consent
Not required for this type of study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhang, X., Mu, D., Yang, Y. et al. Predicting the Feasibility of Utilizing SIEA Flap for Breast Reconstruction with Preoperative BMI and Computed Tomography Angiography (CTA) Data. Aesth Plast Surg 45, 100–107 (2021). https://doi.org/10.1007/s00266-019-01605-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-019-01605-0