Abstract
Background
In cases of refractory gynecomastia, surgical excision of excess glandular breast tissue is often warranted. Closed-suction drain placement is commonplace; however, the effect of drains on preventing complications after male breast surgery has not been fully elucidated in the literature.
Objective
To investigate the effect of drains on reducing seroma and hematoma after subcutaneous mastectomy for gynecomastia.
Methods
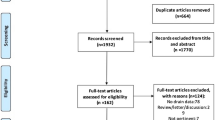
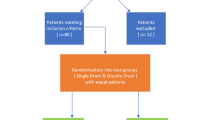
Retrospective chart review of patients undergoing subcutaneous mastectomy for gynecomastia over a 10-year period. Charts were reviewed for demographics, BMI, comorbidities, type of local anesthesia, specimen weight, use of liposuction, and placement of drains. Outcomes were determined by seroma or hematoma in the 30-day postoperative period.
Results
A total of 163 breasts were studied (group I = no-drain, n = 46; group II = drain, n = 117). Group I had a higher rate of clinically significant seromas requiring needle aspiration than group II (6.5 vs 0%, p = 0.0214). There was no difference in rates of hematoma (group I vs II, 2.2 vs 6.0%, p = 0.443) and total fluid collections (group I vs II, 19.6 vs 16.2%, p = 0.647). BMI, use of local anesthesia, specimen weight, and use of liposuction were not significantly associated with postoperative complications.
Conclusions
Closed-suction drains may reduce rates of clinically significant seromas requiring needle aspiration. Though drains carry their own pertinent adverse effects (e.g., patient discomfort and anxiety, cost, and additional clinic visits), there remains no universal standard of care and surgeon practices vary widely. Given the potential to reduce seroma rates, we recommend that surgeons consider placing drains and discuss with patients the benefits and risks of drains after surgical treatment of gynecomastia.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to Table of Contents or the online Instructions to Authors www.springer.com/00266.
Similar content being viewed by others
References
Brown R, Chang D, Siy R et al (2015) Trends in the surgical correction of gynecomastia. Semin Plast Surg 29:122–130
Kinsella C Jr, Landfair A, Rottgers SA et al (2012) The psychological burden of idiopathic adolescent gynecomastia. Plast Reconstr Surg 129(1):1–7
Rew L, Young C, Harrison T et al (2015) A systematic review of literature on psychosocial aspects of gynecomastia in adolescents and young men. J Adolesc 43:206–212
Rosenberg GJ (1987) Gynecomastia: suction lipectomy as a contemporary solution. Plast Reconstr Surg 80(3):379–386
Lista F, Ahmad J (2008) Power-assisted liposuction and the pull-through technique for the treatment of gynecomastia. Plast Reconstr Surg 121(3):740–747
Rohrich RJ, Ha RY, Kenkel JM et al (2003) Classification and management of gynecomastia: defining the role of ultrasound-assisted liposuction. Plast Reconstr Surg 111(2):909–923
Kasielska A, Antoszewski B (2013) Surgical management of gynecomastia: an outcome analysis. Ann Plast Surg 71(5):471–475
Fagerlund A, Lewin R, Rufolo G et al (2015) Gynecomastia: a systematic review. J Plast Surg Hand Surg 49(6):311–318
Teimourian B, Perlman R (1983) Surgery for gynecomastia. Aesthetic Plast Surg 7:155–157
Varley GW, Milner S, Turner GM et al (1994) Ultrasound assessment of the efficacy of wound drains. J R Coll Surg Edinb 39(2):97–99
Matarasso A, Wallach SG, Rankin M (1998) Reevaluating the need for routine drainage in reduction mammoplasty. Plast Reconstr Surg 102(6):1917–1921
Keskin M, Sutcu M, Cigsar B et al (2014) Necessity of suction drains in gynecomastia surgery. Aesthet Surg J 34(4):538–544
Handschin AE, Bietry D, Husler R et al (2008) Surgical management of gynecomastia—a 10-year analysis. World J Surg 32(1):38–44
Robinson JO (1986) Surgical drainage: a historical perspective. Br J Surg 73(6):422–426
Meyerson JM (2016) A brief history of 2 common surgical drains. Ann Plast Surg 77(1):4–5
Reiffel AJ, Pharmer LA, Weinstein AL et al (2013) A prospective analysis of the association between indwelling surgical drains and surgical site infection in plastic surgery. Ann Plast Surg 71(5):561–565
Reiffel AJ, Barie PS, Spector JA (2013) A multidisciplinary review of the potential association between closed-suction drains and surgical site infection. Surg Infect (Larchmt) 14(3):244–269
Suarez JC, McNamara CA, Barksdale LC et al (2016) Closed suction drainage has no benefits in anterior hip arthroplasty: a prospective, randomized trial. J Arthroplast 31(9):1954–1958
Liu JM, Chen WZ, Fu BQ et al (2016) The use of closed suction drainage in lumbar spinal surgery: is it really necessary? World Neurosurg 90:109–115
Woods RS, Woods JF, Duignan ES et al (2014) Systematic review and meta-analysis of wound drains after thyroid surgery. Br J Surg 101(5):446–456
Rodby KA, Stepniak J, Eisenhut N et al (2011) Abdominoplasty with suction undermining and plication of the superficial fascia without drains: a report of 113 consecutive patients. Plast Reconstr Surg 128(4):973–981
Arrowsmith J, Eltigani E, Krarup K et al (1999) An audit of breast reduction without drains. Br J Plast Surg 52:586–590
Corion L, Smeulders M, van Quijlen P et al (2009) Draining after breast reduction: a randomized controlled inter-patient study. J Plast Reconstr Aesthet Surg 62:865–868
Langer S, Guenther JM, DiFronzo LA (2003) Does fibrin sealant reduce drain output and allow earlier removal of drainage catheters in women undergoing operation for breast cancer? Am Surg 69(1):77–81
Hodgson EL, Fruhstorfer BH, Malata CM (2005) Ultrasonic liposuction in the treatment of gynecomastia. Plast Reconstr Surg 116(2):646–653
Steele SR, Martin MJ, Place RJ (2002) Gynecomastia: complications of the subcutaneous mastectomy. Am Surg 68(2):210–213
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors have any financial disclosures or conflicts of interest.
Rights and permissions
About this article
Cite this article
Chao, J.W., Raveendran, J.A., Maly, C. et al. Closed-Suction Drains After Subcutaneous Mastectomy for Gynecomastia: Do They Reduce Complications?. Aesth Plast Surg 41, 1291–1294 (2017). https://doi.org/10.1007/s00266-017-0959-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-017-0959-z