Abstract
Introduction
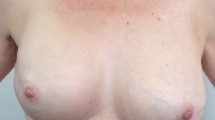
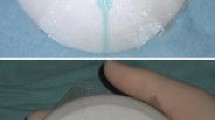
One-stage implant-based breast reconstruction using titanium-coated polypropylene mesh is a novel approach widely used in Europe. Complication rates in breast reconstruction with the use of titanium-coated meshes seem to be comparable to those in patients with implant-based breast reconstruction alone. However, the use of synthetic meshes in implant-based breast reconstructive surgery leads to new clinical scenarios with the need for the breast surgeon to face new complications. We present an innovative treatment of implant exposure in the absence of infection in patients who underwent nipple-sparing mastectomy and immediate breast reconstruction with silicone implants and titanium-coated polypropylene mesh by using a pedicled sub-mammary intercostal perforator flap.
Cases Presentation
Four patients who experienced implant exposure without infection have been treated with the use of a sub-mammary intercostal perforator flap. Whole coverage of the exposed implant/mesh with a sub-mammary intercostal perforator flap was obtained in all cases. No post-operative complications have been observed, whereas a pleasant aesthetic result has been achieved. Patients’ post-operative quality of life and satisfaction levels were measured by the European Organisation for Research and Treatment of Cancer breast cancer-specific quality of life QLQ-BR23 questionnaire and showed an average good satisfaction with the post-operative outcomes (mean QLQ-BR23 score 1.9).
Discussion
For the first time, a sub-mammary intercostal perforator flap has been used with the aim of treating implant exposures without removing the prosthesis even in the presence of synthetic meshes, when wound infection was excluded. Although tested on a small series, the sub-mammary intercostal perforator flap might represent a simple, versatile and cost-effective procedure for the management of implant exposure following nipple-sparing mastectomy and immediate reconstruction with silicone implants and synthetic meshes. It should be considered to avoid implant removal followed by delayed free flap reconstruction as “salvage surgery.”
Level of Evidence V
This journal requires that the authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.





Similar content being viewed by others
References
American Society of Plastic Surgery procedural statistics, reconstructive breast surgery (2014). http://www.plasticsurgery.org/news-and-resources/2014-plastic-surgery-statistics.htm. Accessed Apr 2016
Handel N, Cordray T, Gutierrez J, Jensen JA (2006) A long-term study of outcomes, complications, and patient satisfaction with breast implants. Plast Reconstr Surg 117:757–767 (discussion 768)
Djohan R, Gage E, Bernard S (2008) Breast reconstruction options following mastectomy. Cleve Clin J Med 75(Suppl 1):S17–S23
Logan Ellis H, Asaolu O, Nebo V, Kasem A (2016) Biological and synthetic mesh use in breast reconstructive surgery: a literature review. World J Surg Oncol 14(1):121
Dietrich M, Reimer T, Dietrich H, Stubert J, Gerber B (2012) A short-term follow-up of implant based breast reconstruction using a titanium-coated polypropylene mesh (TiLoop Bra). Eur J Surg Oncol 38(12):1225–1230
Dieterich M, Dieterich H, Timme S, Reimer T, Gerber B, Stubert J (2012) Using a titanium-coated polypropylene mesh (TiLOOP® Bra) for implant-based breast reconstruction: case report and histological analysis. Arch Gynecol Obstet 286(273–276):7
Spear SL, Howard MA, Boehmler JH, Ducic I, Low M, Abbruzzese MR (2004) The infected or exposed breast implant: management and treatment strategies. Plast Reconstr Surg 113(6):1634–1644
Juri J, Valotta F, Leriz MS (2004) Submammary flap for correction of severe sequelae from augmentation mammaplasty. Plast Reconstr Surg 114(2):567–574
Aaronson NK, Ahmedzai S, Bergman B, Bullinger M, Cull A, Duez NJ et al (1993) The European Organization for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst 85(5):365–376
Casella D, Bernini M, Bencini L et al (2014) TiLoop®Bra mesh used for immediate breast reconstruction: comparison of retropectoral and subcutaneous implant placement in a prospective single-institution series. Eur J Plast Surg 37:599–604
Rezai M, Strauß S, Kimmig R, Kern P (2016) Risk-reducing, conservative mastectomy—analysis of surgical outcome and quality of life in 272 implant-based reconstructions using TiLoop® Bra versus autologous corial flaps. Gland Surg 5(1):1–8
Petersen A, Eftekhari AL, Damsgaard TE (2012) Immediate breast reconstruction: a retrospective study with emphasis on complications and risk factors. J Plast Surg Hand Surg 46:344–348
Pinsolle V, Grinfeder C, Mathoulin-Pelissier S, Faucher A (2006) Complications analysis of 266 immediate breast reconstructions. J Plast Reconstr Aesthet Surg 59:1017–1024
Das DK, Choudhury UC (2013) “Thoraco-Abdominal Flap”—a simple flap for skin and soft tissue cover following radical surgery for locally advanced breast cancer—the Malaysian experience. Int J Collab Res Intern Med Public Health 5(6):398–406
Yang JD, Kim MC, Lee JW, Cho YK, Choi KY, Chung HY, Cho BC, Park HY (2012) Usefulness of oncoplastic volume replacement techniques after breast conserving surgery in small to moderate-sized breasts. APS 39(5):489–496
Lee S, Lee J, Lee S, Bae Y (2014) Oncoplastic breast surgery with latissimus dorsi myocutaneous flap for large defect in patients with ptotic breasts: is it feasible when combined with local flaps? World J Surg 12:65
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
The authors declare that they have no conflicts of interest to disclose.
Rights and permissions
About this article
Cite this article
De Riggi, M.A., Rocco, N., Gherardini, G. et al. Management of Implant Exposure in One-Stage Breast Reconstruction Using Titanium-Coated Polypropylene Mesh: Sub-Mammary Intercostal Perforator Flap. Aesth Plast Surg 40, 896–900 (2016). https://doi.org/10.1007/s00266-016-0720-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-016-0720-z