Abstract
Purpose
It has been suggested that low-grade infections could be the cause of arthrofibrosis. However, this hypothesis has not been conclusively proven. The aim of this study is to assess the incidence of unexpected positive cultures (UPC) in patients undergoing revision total joint arthroplasty for a diagnosis of arthrofibrosis.
Methods
A retrospective single-centre review was performed. All patients who underwent an aseptic revision due to histologically confirmed arthrofibrosis (based on the synovial-like interface membrane (SLIM) criteria) were included. The incidence of UPC was then calculated.
Results
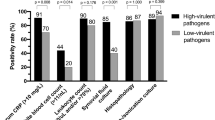
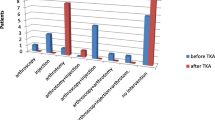
A total of 147 patients were included. Of these, 100 underwent a total knee arthroplasty (TKA) procedure and 46 a total hip arthroplasty (THA) surgery. One patient had a periprosthetic joint infection and was therefore excluded. Of the 146 included patients, 6 had confirmed UPC (4.08%). The following bacteria were identified: Anaerococcus octavius, Staphylococcus epidermidis, Enterobacter cloacae, Staphylococcus hominis, Streptococcus pluranimalium, Staphylococcus pettenkoferi.
Conclusions
Our results suggest that the incidence of UPC in patients with arthrofibrosis is low. It is lower than that of UPC in patients that undergo a revision for other causes. There is no proven relationship between histologically confirmed arthrofibrosis following total joint arthroplasty and prosthetic joint infection.

Similar content being viewed by others
Data availability
The authors have the database available in Microsoft Excel and SPSS formats, and we are disposed to send it if it is required.
Code availability
All statistical analysis were performed using IBM SPSS Statistics (version 24.0; New 103 York, NY, USA).
References
Ribau A, Ekhtiari S, Budin M, Zanna L, Fatih Dasci M, Gehrke T et al (2023) Unexpected positive cultures in patients who have a history of septic revision in the same joint. J Arthroplasty. https://doi.org/10.1016/j.arth.2023.02.078
A P, G P, Re MM, Ad T (2015) The epidemiology of revision total knee and hip arthroplasty in England and Wales: a comparative analysis with projections for the United States. A study using the National Joint Registry dataset. Bone Jt J. https://doi.org/10.1302/0301-620x.97b8.35170
Pabinger C, Lothaller H, Portner N, Geissler A (2018) Projections of hip arthroplasty in OECD countries up to 2050. Hip Int J Clin Exp Res Hip Pathol Ther 28(5):498–506
Klug A, Gramlich Y, Rudert M, Drees P, Hoffmann R, Weißenberger M et al (2021) The projected volume of primary and revision total knee arthroplasty will place an immense burden on future health care systems over the next 30 years. Knee Surg Sports Traumatol Arthrosc 29(10):3287–3298
Kalson NS, Borthwick LA, Mann DA, Deehan DJ, Lewis P, Mann C et al (2016) International consensus on the definition and classification of fibrosis of the knee joint. Bone Jt J 98-B(11):1479–88
Gehrke T, Althaus L, Linke P, Salber J, Krenn V, Citak M (2022) Arthrofibrosis following primary total hip arthroplasty: a distinct clinical entity. Arch Orthop Trauma Surg 142(3):511–515
Barrack RL, Aggarwal A, Burnett RSJ, Clohisy JC, Ghanem E, Sharkey P et al (2007) The fate of the unexpected positive intraoperative cultures after revision total knee arthroplasty. J Arthroplasty 22(6 Suppl 2):94–99
Rauzi MR, Foran JRH, Bade MJ (2022) Multimodal conservative management of arthrofibrosis after total knee arthroplasty compared to manipulation under anesthesia: a feasibility study with retrospective cohort comparison. Pilot Feasibility Stud 8(1):71
Cheuy VA, Foran JRH, Paxton RJ, Bade MJ, Zeni JA, Stevens-Lapsley JE (2017) Arthrofibrosis associated with total knee arthroplasty. J Arthroplasty 32(8):2604–2611
Brückner C, Straube E, Petersen I, Sachse S, Keller P, Layher F et al (2019) Low-grade infections as a possible cause of arthrofibrosis after total knee arthroplasty. Patient Saf Surg 13(1):1
Salib CG, Reina N, van Wijnen AJ, Hanssen AD, Berry DJ, Abdel MP (2021) Absence of signature inflammatory markers in synovial fluid for total knee arthroplasties revised for arthrofibrosis. Orthop Traumatol Surg Res 107(3):102870
Thompson R, Novikov D, Cizmic Z, Feng JE, Fideler K, Sayeed Z et al (2019) Arthrofibrosis after total knee arthroplasty: pathophysiology, diagnosis, and management. Orthop Clin 50(3):269–279
Linke P, Lausmann C, Gehrke T, Citak M (2022) Arthrofibrosis of the hip joint : diagnostic and therapeutic challenge. Unfallchirurgie Heidelb Ger 125(11):868–871
Chen X, Wang Z, Huang Y, Deng W, Zhou Y, Chu M (2021) Identification of novel biomarkers for arthrofibrosis after total knee arthroplasty in animal models and clinical patients. EBioMedicine 70:103486
Neufeld ME, Lanting BA, Shehata M, Howard JL, MacDonald SJ, Teeter MG et al (2021) Prevalence and outcomes of unexpected positive intraoperative cultures in presumed aseptic revision hip arthroplasty. J Bone Joint Surg Am 103(15):1392–1401
Purudappa PP, Sharma OP, Priyavadana S, Sambandam S, Villafuerte JA (2020) Unexpected positive intraoperative cultures (UPIC) in revision Hip and knee arthroplasty- a review of the literature. J Orthop 17:1–6
Kloos J, Vander Linden K, Vermote S, Berger P, Vandenneucker H (2022) Prevalence, interpretation, and management of unexpected positive cultures in revision TKA: a systematic review. Knee Surg Sports Traumatol Arthrosc Off J ESSKA 30(12):3998–4009
Goh GS, Tarabichi S, Clarkson SJ, Zanna L, Citak M, Parvizi J (2022) Positive cultures can be safely ignored in revision arthroplasty patients that do not meet the 2018 International Consensus Meeting Criteria. J Arthroplasty 37(11):2257–2261
Author information
Authors and Affiliations
Contributions
All persons who meet authorship criteria are listed as authors, and all authors certify that they have participated sufficiently in the work.
Corresponding author
Ethics declarations
Informed consent
Not applicable.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lara-Taranchenko, Y., Moreira, T., Sandiford, N.A. et al. Unexpected positive cultures in patients with arthrofibrosis following total hip and total knee arthroplasty. International Orthopaedics (SICOT) 48, 345–350 (2024). https://doi.org/10.1007/s00264-023-05990-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-023-05990-9