Abstract
Purpose
Meniscal tears or histological meniscal calcifications (in the absence of radiological chondrocalcinosis) are frequent in osteoarthritis. Whether lateral meniscal lesions influence clinical outcomes after medial unicompartmental knee arthroplasty (UKA) is unknown.
Methods
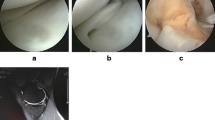
We analyzed 130 patients (130 knees) with medial unicompartmental knee arthroplasties between 2005 and 2015. These 130 knees had full articular cartilage thickness in the lateral compartment and no radiological chondrocalcinosis on preoperative radiographs. The lateral meniscus was analyzed with preoperative MRI and a biopsy of the anterior horn at the time of surgery. Synovial fluid was collected and analyzed for calcium pyrophosphate dihydrate crystal deposition (CPPD crystals). Lateral meniscal tears were untreated when detected on MRI or during surgery, with the hypothesis that these tears on the opposite compartment would remain asymptomatic in medial UKA. At average 10-year follow-up, patients were evaluated with clinical and radiographic outcome, with a focus on the risk of joint space narrowing of the lateral femorotibial compartment.
Results
CPPD crystals were present in the synovial fluid of 70 knees. Lateral meniscal tears were seen on MRI in 34 (49%) normal meniscuses of the 60 knees without CPPD crystals and in six other knees without histological meniscal calcification despite CPPD crystals. Histological calcification was present on 61 lateral meniscuses with 53 meniscal tears. The results showed no significant differences in the clinical outcomes between knees with lateral meniscal tears or lateral meniscal histological chondrocalcinosis or both lesions and those without these conditions. Additionally, radiographic progression of osteoarthritis in the opposite femorotibial compartment of the knee was not more frequent in patients with these meniscal issues. The ten year cumulative survival rates, measured by the need for total knee arthroplasty, were 91% for knees without meniscal lesions and 92% for knees with these lesions.
Conclusion
On this basis, treatment of meniscal tears of the lateral compartment and routine aspiration of the knee to assess for birefringent crystals in the planning of medial UKA do not appear necessary.




Similar content being viewed by others
Data availability
University of Paris on demand.
Code availability
None.
References
Andronic O, Helmy N, Kellner C, Graf DA (2023) A decreased tibial tuberosity-trochlear groove distance is associated with lateral patellofemoral joint degeneration after implantation of medial fixed-bearing unicompartmental knee arthroplasty - a minimum five year follow-up. Int Orthop. https://doi.org/10.1007/s00264-023-05812-y
Ge J, Liu C, Sun X, Zhang Q, Ji B, Guo W (2023) Gap balance difference of unicompartmental knee arthroplasty between hanging leg and supine leg position: a prospective cohort study. Int Orthop 47(3):745–753. https://doi.org/10.1007/s00264-022-05680-y
Foissey C, Batailler C, Vahabi A, Fontalis A, Servien E, Lustig S (2023) Better accuracy and implant survival in medial imageless robotic-assisted unicompartmental knee arthroplasty compared to conventional unicompartmental knee arthroplasty: two- to eleven-year follow-up of three hundred fifty-six consecutive knees. Int Orthop 47(2):533–541. https://doi.org/10.1007/s00264-022-05640-6
Favroul C, Batailler C, Canetti R, Shatrov J, Zambianchi F, Catani F, Servien E, Lustig S (2023) Image-based robotic unicompartmental knee arthroplasty allowed to match the rotation of the tibial implant with the native kinematic knee alignment. Int Orthop 47(2):519–526. https://doi.org/10.1007/s00264-022-05637-1
Stern SH, Becker MW, Insall JN (1993) Unicondylar knee arthroplasty: an evaluation of selection criteria. Clin Orthop Rel Res 286:143–148
Foissey C, Batailler C, Shatrov J, Servien E, Lustig S (2023) Is combined robotically assisted unicompartmental knee arthroplasty and anterior cruciate ligament reconstruction a good solution for the young arthritic knee? Int Orthop 47(4):963–971. https://doi.org/10.1007/s00264-022-05544-5
Hernigou P, Pascale W, Pascale V, Homma Y, Poignard A (2012) Does primary or secondary chondrocalcinosis influence long-term survivorship of unicompartmental arthroplasty? Clin Orthop Relat Res 470(7):1973–1979
Kumar V, Pandit HG, Liddle AD, Borror W, Jenkins C, Mellon SJ, Hamilton TW, Athanasou N, Dodd CAF, Murray DW (2017) Comparison of outcomes after UKA in patients with and without chondrocalcinosis: a matched cohort study. Knee Surg Sports Traumatol Arthrosc 25(1):319–324
Moret CS, Iordache E, D’Ambrosi R, Hirschmann MT (2022) Chondrocalcinosis does not affect functional outcome and prosthesis survival in patients after total or unicompartmental knee arthroplasty: a systematic review. Knee Surg Sports Traumatol Arthrosc 30(3):1039–1049
Kamatsuki Y, Furumatsu T, Hiranaka T, Okazaki Y, Kintaka K, Kodama Y, Miyazawa S, Ozaki T (2023) Epidemiological features of acute medial meniscus posterior root tears. Int Orthop. https://doi.org/10.1007/s00264-023-05848-0
Ghouri A, Muzumdar S, Barr AJ, Robinson E, Murdoch C, Kingsbury SR, Conaghan PG (2022) The relationship between meniscal pathologies, cartilage loss, joint replacement and pain in knee osteoarthritis: a systematic review. Osteoarthr Cartil 30(10):1287–1327. https://doi.org/10.1016/j.joca.2022.08.002
Derfus BA, Kurian JB, Butler JJ (2002) The high prevalence of pathologic calcium crystals in preoperative knees. J Rheumatol 29:570–574
Sokoloff L, Varma A (1988) Chondrocalcinosis in surgically resected joints. Arthritis Rheum 31:750–756
Ward RJ, Driban JB, MacKay JW, McAlindon TE, Lu B, Eaton CB, Lo GH, Barbe MF, Harkey MS (2023) Meniscal degeneration is prognostic of destabilzing meniscal tear and accelerated knee osteoarthritis: data from the Osteoarthritis Initiative. J Orthop Res. https://doi.org/10.1002/jor.25575
Molloy ES, McCarthy GM (2006) Basic calcium phosphate crystals: pathways to joint degeneration. Curr Opin Rheumatol 18:187–92
Wang W, Ding R, Zhang N, Hernigou P (2021) Subchondral bone cysts regress after correction of malalignment in knee osteoarthritis: comply with Wolff’s law. Int Orthop 45(2):445–451. https://doi.org/10.1007/s00264-020-04809-1
Abreu M, Johnson K, Chung CB et al (2004) Calcification in calcium pyrophosphate dihydrate (CPPD) crystalline deposits in the knee: anatomic, radiographic, MR imaging, and histologic study in cadavers. Skeletal Radiol 33:392–398
Hernigou P, Delambre J, Quiennec S, Poignard A (2021) Human bone marrow mesenchymal stem cell injection in subchondral lesions of knee osteoarthritis: a prospective randomized study versus contralateral arthroplasty at a mean fifteen year follow-up. Int Orthop 45(2):365–373. https://doi.org/10.1007/s00264-020-04571-4
Bellamy N, Buchanan WW, Goldsmith CH, Campbell J, Stitt LW (1988) Validation study of a health status instrument for measuring clinically important patient relevant outcomes to antirheumatic drug therapy in patients with osteoarthritis of the hip or knee. J Rheumatol 15:1833–1840
Gibilisco PA, Schumacher HR Jr, Hollander JL, Soper KA (1985) Synovial fluid crystals in osteoarthritis. Arthritis Rheum 28:511–515
Zhang W, Doherty M, Bardin T, Barskova V, Guerne P-A, Jansen TL, Leeb BF, Perez-Ruiz F, Pimentao J, Punzi L, Richette P, Sivera F, Uhlig T, Watt I, Pascual E (2011) European League Against Rheumatism recommendations for calcium pyrophosphate deposition. Part I: terminology and diagnosis. Ann Rheum Dis 70(4):563–570
Rosenthal AK, Ryan LM (2016) Calcium pyrophosphate deposition disease. N Engl J Med 374(26):2575–2584
Barskova VG, Kudaeva FM, Bozhieva LA, Smirnov AV, Volkov AV, Nasonov EL (2013) Comparison of three imaging techniques in diagnosis of chondrocalcinosis of the knees in calcium pyrophosphate deposition disease. Rheumatology (Oxford) 52:1090–1094
Felson DT, Anderson JJ, Naimark A, Kannel W, Meenan RF (1989) The prevalence of chondrocalcinosis in the elderly and its association with knee osteoarthritis: the Framingham Study. J Rheumatol 16:1241–1245
Mitsuyama H, Healey RM, Terkeltaub RA, Coutts RD, Amiel D (2007) Calcification of human articular knee cartilage is primarily an effect of aging rather than osteoarthritis. Osteoarthr Cartil 15(5):559–565
Severino FR, de Oliveira VM, de Paula LeiteCury R, Severino NR, de Moraes Barros Fucs PM (2022) Causes of knee pain evaluated by arthroscopy after knee arthroplasty: a case series. Int Orthop 46(4):697–703. https://doi.org/10.1007/s00264-021-05048-8
Malinowski K, Kim DW, Mostowy M, Pękala P, Kennedy NI, LaPrade RF (2023) Incomplete meniscal healing in early second-look arthroscopy does not indicate failure of repair: a case series. Int Orthop. https://doi.org/10.1007/s00264-023-05868-w
Kawada K, Furumatsu T, Tamura M, Xue H, Higashihara N, Kintaka K, Yokoyama Y, Ozaki T (2023) Medial joint space narrowing progresses after pullout repair of medial meniscus posterior root tear. Int Orthop. https://doi.org/10.1007/s00264-023-05701-4
Sun X, Hernigou P, Zhang Q, Zhang N, Wang W, Chen Y, Guo W (2021) Sensor and machine learning-based assessment of gap balancing in cadaveric unicompartmental knee arthroplasty surgical training. Int Orthop 45(11):2843–2849. https://doi.org/10.1007/s00264-021-05176-1
Sessa V, Celentano U (2021) Unicompartmental knee arthroplasty: all-poly versus metal-backed tibial component-a long-term follow-up study. Int Orthop 45(12):3063–3068. https://doi.org/10.1007/s00264-021-05031-3
Hernigou P, Deschamps G (2004) Alignment influences wear in the knee after medial unicompartmental arthroplasty. Clin Orthop Relat Res 423:161–165
Author information
Authors and Affiliations
Contributions
Data collection: PH, SK, and JH; redaction: PH; lecture and corrections: NZ, WG, JG, QZ, and JH.
Corresponding author
Ethics declarations
Ethical approval
All data are reported in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent to participate
Patients agree.
Consent for publication
The authors agree to publish the manuscript.
Competing interests
The authors have no conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hernigou, P., Karam, S., Zhang, N. et al. Lateral meniscus with tears or with histologic calcification does not increase the risk of lateral osteoarthritis after medial unicompartmental arthroplasty. International Orthopaedics (SICOT) 47, 2477–2485 (2023). https://doi.org/10.1007/s00264-023-05907-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-023-05907-6