Abstract
Purpose
Discharge against medical advice (DAMA) is a worldwide phenomenon. It continues to challenge the healthcare system and has profound effects on outcomes of treatment. It is when a patient leaves the hospital against the treating physician’s recommendation. The objectives of this study are to identify the prevalence, associated factors, and proffer recommendations to mitigate the anomaly in our local/regional healthcare system.
Methods
This was a cross-sectional study with data collected from consecutive patients who sought DAMA at the accident and emergency department of the hospital from October 2020 to March 2022. Data were analyzed using SPSS version 26. Descriptive and inferential statistics were used for data presentation.
Results
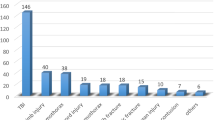
Ninety-nine cases of DAMA out of 4608 patients seen at the Emergency Department during the study period, giving a prevalence rate of 2.14%. 70.7% (70) of these patients were aged 16–44 years with male-to-female ratio of 2.5:1. An estimated half the number of the patients who DAMA were traders 44.4% (44), 14.1% (14) were in paid employment, 22.2% (22) were unskilled workers, and 3% (3) unemployed. Financial constraint was the leading cause in 73 (73.7%) cases. The majority of patients had limited or no formal education, and this was significantly associated with DAMA (P = 0.032). Ninety-two patients (92.6%) sought discharge within 72 h of admission and 89 (89.9%) admitted to leaving to seek alternative methods of care.
Conclusion
DAMA is still a problem in our environment. Comprehensive health insurance must be mandatory for all citizens with improved scope and coverage, especially for trauma victims.


Similar content being viewed by others
References
Machin LL, Goodwin D, Warriner D (2018) An alternative view of self-discharge against medical advice: an opportunity to demonstrate empathy, empowerment, and care. Qual Health Res 28(5):702–710. https://doi.org/10.1177/1049732318754514
Taqueti VR (2007) Leaving against medical advice. N Engl J Med 357(3):213–215
Beauchamp TL, Childress JF (2001) Principles of biomedical ethics, 5th edn. Oxford University Press, New York, p 451
Carrese JA (2006) Refusal of care: patient’s well-being and physicians ethical obligations; but doctor, I want to go home. JAMA 296(6):691–695. https://doi.org/10.1001/jama.296.6.691
Williams GC, Freedman ZR, Deci EL (1998) Supporting autonomy to motivate patients with diabetes for glucose control. Diabetes Care 21(10):1644–1651. https://doi.org/10.2337/diacare.21.10.1644
Alfandre DJ (2009) “I’m going home”: discharges against medical advice. Mayo Clin Proc 84(3):255–260. https://doi.org/10.4065/84.3.255
Hwang SW, Li J, Gupta R, Chien V, Martin RE (2003) What happens to patients who leave hospital against medical advice? CMAJ 168(4):417–420
Aliyu ZY (2002) Discharge against medical advice: sociodemographic, clinical and financial perspectives. Int J Clin Pract 56(5):325–327
Choi M, Kim H, Qian H, Palepu A (2011) Readmission rates of patients discharged against medical advice: a matched cohort study. PloS One 6(9):e24459. https://doi.org/10.1371/journal.pone.0024459
Udosen AM, Glen E, Ogbudu S, Nkposong E (2006) Incidence of leaving against medical advice (LAMA) among patients admitted at the accident and emergency unit of the Univeristy of Calabar Teaching Hospital, Calabar, Nigeria. Niger J Clin Pract 9(2):120–123
Yusuf MB, Ogunlusi JD, Popoola SO, Ogunlayi SO, Babalola WO, Oluwadiya KS (2017) Self-discharge against medical advice from tertiary health institution: a call for concern. Niger Postgrad Med J 24:174–177. https://doi.org/10.4103/npmj.npmj_88_17
Ibrahim SA, Kwoh CK, Krishnan E (2007) Factors associated with patients who leave acute-care hospitals against medical advice. Am J Public Health 97(12):2204–8. https://doi.org/10.2105/AJPH.2006.100164
Duñó R, Pousa E, Sans J, Tolosa C, Ruiz A (2003) Discharge against medical advice at a general hospital in Catalonia. Gen Hosp Psychiatry 25(1):46–50. https://doi.org/10.1016/s0163-8343(02)00253-0
Pages KP, Russo JE, Wingerson DK, Ries RK, Roy-Byrne PP, Cowley DS (1998) Predictors and outcome of discharge against medical advice from the psychiatric units of a general hospital. Psychiatr Serv 49(9):1187–92. https://doi.org/10.1176/ps.49.9.1187
Madubueze CC, Madubueze UC, Omoke NI, Una AF, Babalola OR, Alabi S, Dim EM (2022) National survey on discharge against medical advice among patients with musculoskeletal trauma in Nigeria. Niger J Med 31:13–19. https://doi.org/10.4103/NJM.NJM_186_21
Eze B, Agu K, Nwosu J (2010) Discharge against medical advice at a tertiary center in southeastern Nigeria: sociodemographic and clinical dimensions. Patient Intell 2(Default):27–31. https://doi.org/10.2147/PI.S11337
Feras HA, Farooq M, Elshehry AF, Hassan MA, Jawaid RF (2017) The rate and reasons for discharge against medical advice. Bahrain Med Bull 39(3):140–145
Saitz R, Ghali WA, Moskowitz MA (2000) The impact of leaving against medical advice on hospital resource utilization. J Gen Intern Med 15(2):103–107. https://doi.org/10.1046/j.1525-1497.2000.12068.x
Albert HD, Kornfeld DS (1973) The threat to sign out against medical advice. Ann Intern Med 79(6):888–91. https://doi.org/10.7326/0003-4819-79-6-888
Popoola SO, Onyemaechi NOC, Kortor JN, Oluwadiya KS (2013) Leave against medical advice (LAMA) from in-patient orthopaedic treatment. SA Orthop J 12(3):58–61
Matthews DA, Suchman AL, Branch WT Jr (1993) Making “connexions”: enhancing the therapeutic potential of patient-clinician relationships. Ann Intern Med 118(12):973–7. https://doi.org/10.7326/0003-4819-118-12-199306150-00010
Beckman HB, Markakis KM, Suchman AL, Frankel RM (1994) The doctor-patient relationship and malpractice Lessons from plaintiff depositions. Arch Intern Med 154(12):1365–70
Orimolade EA, Adegbehingbe OO, Oginni LM, Asuquo JE, Esan O (2013) Reasons why trauma patients request for discharge against medical advice in Wesley Guild Hospital Ilesha. East Cent Afri J Surg 18(3):71–75
Epstein RM, Hadee T, Carroll J, Meldrum SC, Lardner J, Shields CG (2007) Could this be something serious Reassurance, uncertainty, and empathy in response to patients’ expressions of worry. J Gen Intern Med 22(12):1731–9. https://doi.org/10.1007/s11606-007-0416-9
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Adetunji Mapaderun Toluse, Adebola Biala, and Adedamola Dele Onibonoje performed material preparation, data collection, and analysis. Adedamola Dele Onibonoje wrote the first draft of the manuscript, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. The Ethics Committee of the National Orthopaedic Hospital, Lagos, granted approval (Date- 11 August 2020 /S. 314/IV No. 970).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Toluse, A.M., Onibonoje, A.D., Biala, A. et al. Discharge against medical advice: cross-sectional survey from a regional orthopaedic hospital in sub-Saharan Africa. International Orthopaedics (SICOT) 47, 1671–1676 (2023). https://doi.org/10.1007/s00264-023-05836-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-023-05836-4