Abstract
Purpose
This study proposes machine learning to analyze the risk factors of the collapse in patients with non-traumatic hip osteonecrosis of the femoral head.
Methods
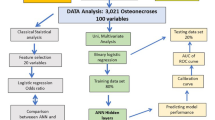
We collected data of 900 consecutive patients (634 males) with bilateral (428) or unilateral non-traumatic osteonecrosis diagnosed before collapse (at stage I or stage II). The follow-up was average five years (3 to 8 years). A total of 50 variables related to the osteonecrosis were included in the study. The osteonecroses were randomly divided into a training set (80%) and a validation set (20%) with a similar percentage of hips with collapse in the two groups. Machine learning (ML) algorithms were trained with the selected variables. Performance was evaluated and the different factors (variables) for collapse were ranked with Shapley values. The primary outcome was prediction of occurrence of collapse from automated inventory systems.
Results
In this series of patients, the accuracy with machine learning for predicting collapse within three years follow-up was 81.2%. Accuracies for predicting collapse within six to 12-24 months were 54.2%, 67.3%, and 71.2%, respectively, demonstrating that the accuracy is lower for a prevision in the short term than for the mid-term. Despite none of the risk-factors alone achieving statistical significance for prediction, the system allowed ranking the different variables for risk of collapse. The highest risk factors for collapse were sickle cell disease, liver, and cardiac transplantation treated with corticosteroids, osteonecrosis volume > 50% of the femoral head. Cancer (such as leukemia), alcohol abuse, lupus erythematosus, Crohn’s disease, pemphigus vulgaris treated with corticosteroids, and osteonecrosis volume between 40 and 50% were medium risk factors for collapse. Familial cluster of collapse, HIV infection, chronic renal failure, nephrotic syndrome, and renal transplantation, when treated with corticosteroids, stage II, osteonecrosis volume between 30 and 40%, chemotherapy, hip pain with VAS > 6, and collapse progression on the contralateral side, were also significant but lowest risk factors. A heat map is proposed to illustrate the ranking of the combinations of the different variables. The highest risk of collapse is obtained with association of various risks factors.
Conclusion
This study, for the first time, demonstrated prediction of collapse and ranking of factors for collapse with a machine learning system. This study also shows that collapse is due to a multifactorial risk factors.








Similar content being viewed by others
Data Availability
University of Paris.
Code availability
None.
References
Mont MA, Zywiel MG, Marker DR, McGrath MS, Delanois RE (2010) The natural history of untreated asymptomatic osteonecrosis of the femoral head: a systematic literature review. J Bone Joint Surg Am 92(12):2165–2170. https://doi.org/10.2106/JBJS.I.00575
Liu F, Wang W, Yang L, Wang B, Wang J, Chai W, Zhao D (2017) An epidemiological study of etiology and clinical characteristics in patients with nontraumatic osteonecrosis of the femoral head. J Res Med Sci. 22:15. https://doi.org/10.4103/1735-1995.200273
Hernigou P, Bachir D, Galacteros F (2003) The natural history of symptomatic osteonecrosis in adults with sickle-cell disease. J Bone Joint Surg Am 85(3):500–4. https://doi.org/10.2106/00004623-200303000-00016
Kuroda Y, Tanaka T, Miyagawa T, Kawai T, Goto K, Tanaka S et al (2019) Classification of osteonecrosis of the femoral head: who should have surgery? Bone Joint Res 8(10):451–458. https://doi.org/10.1302/2046-3758.810.BJR-2019-0022.R1
Steinberg ME, Bands RE, Parry S, Hoffman E, Chan T, Hartman KM (1999) Does lesion size affect the outcome in avascular necrosis? Clin Orthop Relat Res 367:262–271
Lieberman JR, Engstrom SM, Meneghini MR, SooHoo NF (2012) Which factors influence preservation of the osteonecrotic femoral head? Clin Orthop Relat Res 470(2):525–534. https://doi.org/10.1007/s11999-011-2050-4
Hernigou P, Poignard A, Nogier A, Manicom O (2004) Fate of very small asymptomatic stage-I osteonecrotic lesions of the hip. J Bone Joint Surg Am 86(12):2589–2593. https://doi.org/10.2106/00004623-200412000-00001
Nishii T, Sugano N, Ohzono K, Sakai T, Sato Y, Yoshikawa H (2002) Significance of lesion size and location in the prediction of collapse of osteonecrosis of the femoral head: a new three-dimensional quantification using magnetic resonance imaging. J Orthop Res 20(1):130–136. https://doi.org/10.1016/S0736-0266(01)00063-8
Vicaş RM, Bodog FD, Fugaru FO, Grosu F, Badea O, Lazăr L, Cevei ML, Nistor-Cseppento CD, Beiuşanu GC, Holt G, Voiţă-Mekereş F, Buzlea CD, Ţica O, Ciursaş AN, Dinescu SN (2020) Histopathological and immunohistochemical aspects of bone tissue in aseptic necrosis of the femoral head. Rom J Morphol Embryol Oct-Dec 61(4):1249–1258. https://doi.org/10.47162/RJME.61.4.26
Margolus N, Levitin LB (1998) The maximum speed of dynamical evolution. Physica D 120(1–2):188–195. https://doi.org/10.1016/S0167-2789(98)00054-2.S2CID468290
Molnar C (2020) Interpretable Machine Learning. A Guide for Making Black Box Models Explainable. Lulu.com, USA
Sultan AA, Mohamed N, Samuel LT, Chughtai M, Sodhi N, Krebs VE, Stearns KL, Molloy RM, Mont MA (2019) Classification systems of hip osteonecrosis: an updated review. Int Orthop 43(5):1089–1095. https://doi.org/10.1007/s00264-018-4018-4
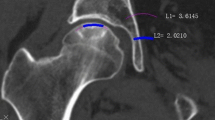
Hernigou P, Lambotte JC (2001) Volumetric analysis of osteonecrosis of the femur. Anatomical correlation using MRI. J Bone Joint Surg Br 83:672–5
Hernigou P, Lambotte JC (2000) Bilateral hip osteonecrosis: influence of hip size on outcome. Ann Rheum Dis 59(10):817–21
Hernigou P, Dubory A, Homma Y, Guissou I, FlouzatLachaniette CH, Chevallier N, Rouard H (2018) Cell therapy versus simultaneous contralateral decompression in symptomatic corticosteroid osteonecrosis: a thirty-year follow-up prospective randomized study of one hundred and twenty five adult patients. Int Orthop. 42(7):1639–1649. https://doi.org/10.1007/s00264-018-3941-8
Duval-Beaupère G, Schmidt C, Cosson P (1992) A barycentremetric study of the sagittal shape of spine and pelvis: the conditions required for an economic standing position. Ann Biomed Eng 20:451–462. https://doi.org/10.1007/BF02368136
Le Huec JC, Hasegawa K (2016) Normative values for the spine shape parameters using 3D standing analysis from a database of 268 asymptomatic Caucasian and Japanese subjects. Eur Spine J 25:3630–3637. https://doi.org/10.1007/s00586-016-4485-5
Vollmer S, Mateen BA, Bohner G, Király FJ, Ghani R, Jonsson P et al (2020) Machine learning and artificial intelligence research for patient benefit: 20 critical questions on transparency, replicability, ethics, and effectiveness. BMJ 368:l6927
Moons KG, Wolff RF, Riley RD, Whiting PF, Westwood M, Collins GS et al (2019) PROBAST: a tool to assess risk of bias and applicability of prediction model studies: explanation and elaboration. Ann Intern Med 170(W1):1–33. https://doi.org/10.7326/M18-1377
Breiman L, Friedman J, Stone CJ, Olshen RA (1984) Classification and regression trees. Taylor & Francis
Fernandez A, Garcia S, Herrera F, Chawla NV (2018) SMOTE for learning from imbalanced data: progress and challenges, marking the 15-year anniversary. J Art Intell Res 61(1):863–905. https://doi.org/10.1613/jair.1.11192]
Lundberg SM, Lee S-I. A (2017) unified approach to interpreting model predictions. NIPS; New York: Curran Associates; 4765–4774
Meng Y, Yang N, Qian Z, Zhang G (2020) What makes an online review more helpful: an interpretation framework using XGBoost and SHAP values. J Theor Appl Electron Res 16(3):466–490. https://doi.org/10.3390/jtaer16030029]
Rodriguez VL, Fischhoff B, Davis AL. (2022) Risk heatmaps as visual displays: opening movie studios after the COVID-19 shutdown. Risk Anal. https://doi.org/10.1111/risa.14017
Ha YC, Jung WH, Kim JR, Seong NH, Kim SY, Koo KH (2006) Prediction of collapse in femoral head osteonecrosis: a modified Kerboul method with use of magnetic resonance images. J Bone Joint Surg Am. 88(Suppl 3):35–40. https://doi.org/10.2106/JBJS.F.00535
Fan Y, Zhang J, Chen M, Pang F, Chen H, Wu Y, Liang Y, Wei Z, Cai K, Li W, Fang H, Hong G, Zhou C, Chen Z (2022) Diagnostic value of necrotic lesion boundary in bone collapse of femoral head osteonecrosis. Int Orthop. 46(3):423–431. https://doi.org/10.1007/s00264-021-05081-7
Kwon HM, Yang IH, Park KK, Cho BW, Kam JH, Kong Y, Yang JH, Lee WS (2020) High pelvic incidence is associated with disease progression in nontraumatic osteonecrosis of the femoral head. Clin Orthop Relat Res. 478(8):1870–1876. https://doi.org/10.1097/CORR.0000000000001155
Hiratsuka S, Takahata M, Hojo Y, Kajino T, Hisada Y, Iwata A, Yamada K, Iwasaki N (2018) Increased risk of symptomatic progression of instability following decompression for lumbar canal stenosis in patients receiving chronic glucocorticoids therapy. J Orthop Sci. https://doi.org/10.1016/j.jos.2018.08.002
Osawa Y, Takegami Y, Kato D, Okamoto M, Iida H, Imagama S. (2022) Hip function in patients undergoing conservative treatment for osteonecrosis of the femoral head. Int Orthop. https://doi.org/10.1007/s00264-022-05569-w. Online ahead of print
Osawa Y, Seki T, Takegami Y, Makida K, Ochiai S, Imagama S (2021) Collapse progression or cessation affects the natural history of contralateral osteonecrosis of the femoral head. J Arthroplasty 36(12):3839–3844. https://doi.org/10.1016/j.arth.2021.08.005
Bradway JK, Morrey BF (1993) The natural history of the silent hip in bilateral atraumatic osteonecrosis. J Arthroplast 8(4):383–387. https://doi.org/10.1016/S0883-5403(06)80036-7
Acknowledgements
The author thanks the Paris-Saclay University for reviewing mathematics data.
Funding
There is no funding source.
Author information
Authors and Affiliations
Contributions
One author PH.
Corresponding author
Ethics declarations
Ethics approval
All data are reported in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent for publication
The author agrees to publish the manuscript.
Competing interests
The author declares no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hernigou, P. Revisiting prediction of collapse in hip osteonecrosis with artificial intelligence and machine learning: a new approach for quantifying and ranking the contribution and association of factors for collapse. International Orthopaedics (SICOT) 47, 677–689 (2023). https://doi.org/10.1007/s00264-022-05631-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-022-05631-7