Abstract
Purpose
Total hip arthroplasty (THA) is a successful treatment for hip osteoarthritis secondary to hip dysplasia. However, the reported rate of complications following THA in the settings of neuromuscular diseases is high. This systematic review aimed to analyze the indications, functional outcomes and surgical failures of primary THA in cerebral palsy (CP) patients.
Methods
MEDLINE, EMBASE and the Cochrane Database of Systematic Reviews were searched, and all clinical studies focusing on THA in patients with CP from inception through March 2020 were included. The methodological quality was assessed with Guo et al.’s quality appraisal checklist for case series and case–control studies, while cohort and prospective studies were evaluated with a modified version of the Downs and Black’s quality assessment checklist.
Results
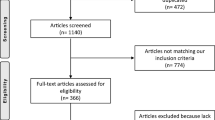
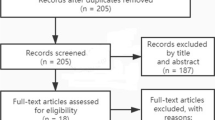
The initial search returned 69 studies out of which 15, including 2732 THAs, met the inclusion criteria. The most frequent indication for THA was dislocated painful hip for which previous non-operative treatment had failed. Complications presented in 10 to 45% of cases. The most frequently reported complication was dislocation (1–20%), followed by component loosening (0.74–20%). Aseptic component loosening was the most frequent cause of revision surgery, followed by dislocation and periprosthetic fracture. Mean implant survival at ten years was 84% (range 81–86%).
Conclusion
The available literature suggests that although THA is a beneficial procedure in CP patients, it has a higher rate of complications and worse implant survival than the general population.

Similar content being viewed by others
References
Flynn JM, Miller F (2002) Management of hip disorders in patients with cerebral palsy. J Am Acad Orthop Surg 10:198–209
Lonstein JE, Beck K (1986) Hip dislocation and subluxation in cerebral palsy. J Pediatr Orthop 6:521–526
Palisano R, Rosenbaum P, Walter S et al (2008) Development and reliability of a system to classify gross motor function in children with cerebral palsy. Dev Med Child Neurol 39:214–223
Castle ME, Schneider C (1978) Proximal femoral resection-interposition arthroplasty. J Bone Joint Surg 60:1051–1054
McCarthy RE, Simon S, Douglas B et al (1988) Proximal femoral resection to allow adults who have severe cerebral palsy to sit. J Bone Joint Surg Am 70:1011–1016
Kolman SE, Ruzbarsky JJ, Spiegel DA, Baldwin KD (2016) Salvage options in the cerebral palsy hip: a systematic review. J Pediatr Orthop 36:645–650
Boldingh EJ, Bouwhuis CB, van der Heijden-Maessen HCM et al (2014) Palliative hip surgery in severe cerebral palsy. J Pediatr Orthop B 23:86–92
Skoff HD, Keggi K (1986) Total hip replacement in the neuromuscularly impaired. Orthop Rev 15:154–159
Cabanela ME, Weber M (2000) Total hip arthroplasty in patients with neuromuscular disease. Instr Course Lect 49:163–168
Abu-Zidan FM, Abbas AK, Hefny AI (2013) Clinical “case series”: a concept analysis. Af Health Sci 12(4). https://doi.org/10.4314/ahs.v12i4.25
Voss PH, Rehfuess EA (2013) Quality appraisal in systematic reviews of public health interventions: an empirical study on the impact of choice of tool on meta-analysis. J Epidemiol Community Health 67:98–104
Guo B, Moga C, Harstall C, Schopflocher D (2016) A principal component analysis is conducted for a case series quality appraisal checklist. J Clin Epidemiol 69:199-207.e2
Hennequin-Hoenderdos NL, Slot DE, Van der Weijden GA (2016) The incidence of complications associated with lip and/or tongue piercings: a systematic review. Int J Dent Hyg 14:62–73
Downs SH, Black N (1998) The feasibility of creating a checklist for the assessment of the methodological quality both of randomised and non-randomised studies of health care interventions. J Epidemiol Community Health 52:377–384
Trac MH, McArthur E, Jandoc R et al (2016) Macrolide antibiotics and the risk of ventricular arrhythmia in older adults. CMAJ 188:E120–E129
Houdek MT, Watts CD, Wyles CC et al (2017) Total hip arthroplasty in patients with cerebral palsy: a cohort study matched to patients with osteoarthritis. J Bone Joint Surg Am 99:488–493
Moon AS, Pinto MC, Cichos KH et al (2020) Total joint arthroplasty in patients with cerebral palsy. J Am Acad Orthop Surg 28:171–177
King G, Hunt LP, Wilkinson JM et al (2016) Good outcome of total hip replacement in patients with cerebral palsy: a comparison of 389 patients and 425,813 controls from the National Joint Registry for England and Wales. Acta Orthop 87:93–99
Morin C, Ursu C, Delecourt C (2016) Total hip replacement in young non-ambulatory cerebral palsy patients. Orthop Traumatol Surg Res 102:845–849
Schroeder K, Hauck C, Wiedenhöfer B et al (2010) Long-term results of hip arthroplasty in ambulatory patients with cerebral palsy. Int Orthop 34:335–339
Yoon B-H, Lee Y-K, Ha Y-C, Koo K-H (2015) Contemporary ceramic total hip arthroplasty in patients with cerebral palsy: does it work? Clin Orthop Surg 7:39–45
Sanders RJM, Swierstra BA, Goosen JHM (2013) The use of a dual-mobility concept in total hip arthroplasty patients with spastic disorders: no dislocations in a series of ten cases at midterm follow-up. Arch Orthop Trauma Surg 133:1011–1016
Weber M, Cabanela ME (1999) Total hip arthroplasty in patients with cerebral palsy. Orthopedics 22:425–427
Raphael BS, Dines JS, Akerman M, Root L (2010) Long-term followup of total hip arthroplasty in patients with cerebral palsy. Clin Orthop Relat Res 468:1845–1854
Buly RL, Huo M, Root L, Binzer T, Wilson Jr PD (1993) Total hip arthroplasty in cerebral palsy. Long-term follow-up results. Clin Orthop Relat Res (296):148–153
Molenaers B, Driesen R, Molenaers G, Corten K (2017) The direct anterior approach for complex primary total hip arthroplasty: the extensile acetabular approach on a regular operating room table. J Arthroplasty 32:1553–1559
Root L, Goss JR, Mendes J (1986) The treatment of the painful hip in cerebral palsy by total hip replacement or hip arthrodesis. J Bone Joint Surg Am 68:590–598
Prosser GH, Shears E, O’Hara JN (2012) Hip resurfacing with femoral osteotomy for painful subluxed or dislocated hips in patients with cerebral palsy. J Bone Joint Surg Br 94:483–487
Gabos PG, Miller F, Galban MA et al (1999) Prosthetic interposition arthroplasty for the palliative treatment of end-stage spastic hip disease in nonambulatory patients with cerebral palsy. J Pediatr Orthop 19:796–804
Alosh H, Kamath AF, Baldwin KD et al (2014) Outcomes of total hip arthroplasty in spastic patients. J Arthroplasty 29:1566–1570
Givon U (2017) Management of the spastic hip in cerebral palsy. Curr Opin Pediatr 29:65–69
Melbye SM, Haug SCD, Fenstad AM et al (2021) How does implant survivorship vary with different corail femoral stem variants? Results of 51,212 cases with up to 30 years of follow-up from the Norwegian Arthroplasty Register. Clin Orthop Relat Res 479:2169–2180
Streit MR, Lehner B, Peitgen DS et al (2020) What Is the long-term (27- to 32-year) survivorship of an uncemented tapered titanium femoral component and survival in patients younger than 50 years? Clin Orthop Relat Res 478:1283–1291
Inacio MC, Lorimer M, Davidson DC et al (2018) What is the risk of revision surgery in hydroxyapatite-coated femoral hip stems? Findings from a large national registry. Clin Orthop Relat Res 476:2353–2366
Buttaro MA, Slullitel PA, García Mansilla AM et al (2017) Long-term outcome of unconstrained primary total hip arthroplasty in ipsilateral residual poliomyelitis. Orthopedics 40:e255–e261
Kraay MJ, Bigach SD (2014) The neuromuscularly challenged patient: total hip replacement is now an option. Bone Joint J 96-B:27–31
Ryu H-G, Roh YJ, Oh K-J et al (2021) Dual mobility articulation total hip arthroplasty for displaced neck fracture in elderly with neuromuscular disorder. Injury 52:1480–1486
Adams CT, Lakra A (2020) Clinical and functional outcomes of total hip arthroplasty in patients with cerebral palsy: a systematic review. J Orthop 21:19–24
Author information
Authors and Affiliations
Contributions
CL: study selection, data abstraction, methodological quality assessment, wrote first draft of the manuscript. CF: data abstraction, wrote the final manuscript. DC: study selection, data abstraction, methodological quality assessment, wrote first draft of the manuscript. FC: methodological quality assessment, edited the manuscript. GZ: methodological quality assessment, edited the manuscript. PAS: co-designed the study, conducted data analysis, wrote the manuscript, edited the manuscript. MAB: co-designed the study, edited the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This work was performed at the Italian Hospital of Buenos Aires, Argentina. All authors have participated in research. The article is not submitted elsewhere. It is a new manuscript submission.
Catalina Larrague and Cecilia Fieiras are both primary authors.
Pablo A. Slullitel and Martin A. Buttaro are both Senior authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Larrague, C., Fieiras, C., Campelo, D. et al. Feasibility of total hip arthroplasty in cerebral palsy patients: a systematic review on clinical outcomes and complications. International Orthopaedics (SICOT) 46, 2493–2507 (2022). https://doi.org/10.1007/s00264-022-05528-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-022-05528-5